Abstract
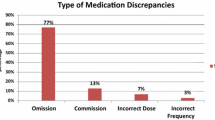
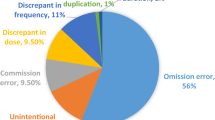
Objective To determine the frequency and clinical significance of medication errors when (a) pharmacists elicit medication histories in the Emergency Department after medications have been prescribed by doctors and (b) pharmacists obtain and chart medication histories prior to doctors’ approval. Setting The Queen Elizabeth Hospital, a 350 bed South Australian teaching hospital, serving the local adult community. Method Emergency Department patients at risk of medication misadventure were recruited in two phases with a ‘usual practice’ arm (6 weeks) and a ‘pharmacist medication charting’ arm (5 weeks) reflecting an alternative intervention. In the ‘usual care’ arm, medication histories were compiled by a pharmacy researcher after a doctor had completed the medication chart. The researcher-elicited medication histories were compared with the doctors’ medication charts and unintentional discrepancies were recorded. In the ‘pharmacist medication charting’ arm, the same process was followed except the researcher compiled the patients’ medication histories at triage, prior to patients seeing a doctor. The medication history was then transcribed onto a medication chart for authorisation by a doctor. In addition, whether resolution of unintentional discrepancies for patients in the ‘usual care’ arm had occurred by discharge was determined by examining patients’ medical records. Main outcome measure Frequency of unintentional discrepancies and medication errors. Results The study included 45 and 29 patients in the ‘usual care’ and intervention arms, respectively. In the ‘usual care’ arm, 75.6% of patients had one or more unintentional discrepancies compared with 3.3% in the ‘pharmacist medication charting’ arm. This resulted in an average of 2.35 missed doses per patient in the ‘usual care’ arm and 0.24 in the intervention arm. In addition, an average of 1.04 incorrect doses per patient were administered in the ‘usual care’ arm and none in the ‘pharmacist medication charting’ arm. The differences observed between the arms were statistically significant (P < 0.05) and deemed clinically significant by a multidisciplinary panel. Conclusion This study provides evidence for pharmacists eliciting medication histories to prepare medication charts at the earliest possible opportunity following a patient’s presentation to the Emergency Department

Similar content being viewed by others
References
ASHP Continuity of Care Task Force. Continuity of care in medication management: review of issues and considerations for pharmacy. Am J Health Syst Pharm. 2005;62:1714–20. doi:10.2146/ajhp050257.
Australian Pharmaceutical Advisory Committee. Guiding principles to achieve continuity of medication management. Canberra (Australia): Commonwealth Department of Health and Aged Care; 2005.
Stowasser DA, McGuire TM, Petrie GM, Lauchlan RL, Collins DM. Information quality: a major consideration in the development of medication liaison services. Aust J Pharm. 1997;27(5):362–6.
Lum E, Muscillo N, McLeod S, Coombes I. Medication reconciliation—the Queensland Health experience. J Pharm Prac Res. 2007;37(1):7–10.
Manno MS, Hayes DD. How medication reconciliation saves lives. Nursing 2006. 2006;36(3):63–4.
Dutton K, Hedger N, Wills S, Brown D, Davies P. Prevent medication errors on admission. Clin Gov Int J. 2003;8(2):128–37. doi:10.1108/14777270310471612.
Peth HA. Medication errors in the emergency department: a systems approach to minimizing risk. Emerg Med Clin North Am. 2003;21:141–58. doi:10.1016/S0733-8627(02)00085-8.
Dean B, Schachter M, Vincent C, Barber N. Causes of prescribing errors in hospital inpatients: a prospective study. Lancet. 2002;259:1373–8. doi:10.1016/S0140-6736(02)08350-2.
Fertleman M, Barnett N, Patel T. Improving medication management for patients: the effect of a pharmacist on post-admission ward rounds. Qual Saf Health Care. 2005;14:207–11. doi:10.1136/qshc.2004.011759.
Binyon D. Pharmaceutical care: its impact on patient care and the hospital-community interface. Pharm J. 1994;253:344–9.
Carter MK, Allin DM, Scott LA, Grauer D. Pharmacist acquired medication histories in a university hospital emergency department. Am J Health Syst Pharm. 2006;63:2500–3. doi:10.2146/ajhp060028.
Elliott RA. Problems with medication use in the elderly: an Australian perspective. J Pharm Prac Res. 2006;36(1):58–66.
Gleason K, Groszek J, Sullivan C, Rooney D, Barnard C, Noskin G. Reconciliation of discrepancies in medication histories and admission orders of newly hospitalised patients. Am J Health Syst Pharm. 2004;61:1689–95.
Nester TM, Hale LS. Effectiveness of a pharmacist-acquired medication history in promoting patient safety. Am J Health Syst Pharm. 2002;59:2221–5.
Chan M, Nicklason F, Vial JH. Adverse drug events as a cause of hospital admission in the elderly. Intern Med. 2001;31:199–205. doi:10.1046/j.1445-5994.2001.00044.x.
Simonson W, Feinberg JL. Medication-related problems in the elderly: defining the issues and identifying solutions. Drugs Aging. 2005;22(7):559–69. doi:10.2165/00002512-200522070-00002.
Crook M, Ajdukovic M, Angley C, Soulsby N, Doecke C, Stupans I, et al. Eliciting comprehensive medication histories in the emergency department: the role of the pharmacist. Pharm Pract. 2007;5(2):78–84.
Pickrell L, Duggan C, Dhillon S. From hospital admission to discharge: an exploratory study to evaluate seamless care. Pharm J. 2001;267(7172):650–3.
Emmerton L, Marriott J, Bessell T, Nissen L, Dean L. Pharmacists and prescribing rights: review of international developments. J Pharm Pharm Sci. 2005;8(2):217–25.
Bond CA, Raehl CL, Franke T. Clinical pharmacy services, pharmacy staffing, and the total cost of care in United States hospitals. Pharmacotherapy. 2000;20(6):609–21. doi:10.1592/phco.20.7.609.35169.
Bond CA, Raehl CL, Franke T. Clinical pharmacy services and hospital mortality rates. Pharmacotherapy. 1999;19(5):556–64. doi:10.1592/phco.19.8.556.31531.
Lada P, Delgado G. Documentation of pharmacists’ interventions in an emergency department and associated cost avoidance. Am J Health Syst Pharm. 2007;64:63–8. doi:10.2146/ajhp050213.
Rossi S, editor. Australian medicines handbook. Adelaide (Australia): Australian Medicines Handbook; 2008. ISBN: 978-0-9757919-9-8.
Bolas H, Brookes K, Scott M, McElnay J. Evaluation of a hospital-based community liason pharmacy service in Northern Ireland. Pharm World Sci. 2004;26:114–20. doi:10.1023/B:PHAR.0000018601.11248.89.
Cornish PL, Knowles SR, Marchesano R, Tam VC, Shadowitz S, Juurlink DN, et al. Unintended medication discrepancies at the time of hospital admission. Arch Intern Med. 2005;165:424–9. doi:10.1001/archinte.165.4.424.
Vira T, Colquhoun M, Etchells E. Reconcilable differences: correcting medication errors at hospital admission and discharge. Qual Saf Health Care. 2006;15:122–6. doi:10.1136/qshc.2005.015347.
von Laue NC, Schwappach DL, Koeck CM. The epidemiology of preventable adverse drug events: a review of the literature. Mid Eur J Med. 2003;115(12):407–15.
Acknowledgements
We would like to acknowledge Dr Ken Ooi, Dr Mark Hoby, Dr Vinay Raniga, Dr Rick Catterwell, Dr Lynne Giles and Ms Cathy Caird for their involvement.
Funding
This study was supported by the Sansom Institute, School of Pharmacy and Medical Sciences.
Conflict of interest
None declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vasileff, H.M., Whitten, L.E., Pink, J.A. et al. The effect on medication errors of pharmacists charting medication in an emergency department. Pharm World Sci 31, 373–379 (2009). https://doi.org/10.1007/s11096-008-9271-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-008-9271-y