Abstract
Purpose
Menkes disease is a rare hereditary disease in which systemic deficiency of copper due to mutation of the ATP7A gene causes severe neurodegenerative disorders. The present parenteral drugs have limited efficacy, so there is a need for an efficacious drug that can be administered orally. This study focused on glyoxal-bis (N(4)-methylthiosemicarbazonato)-copper(II (CuGTSM), which has shown efficacy in macular mice, a murine model of Menkes disease, and examined its pharmacokinetics. In addition, nanosized CuGTSM (nCuGTSM) was prepared, and the effects of nanosizing on CuGTSM pharmacokinetics were investigated.
Methods
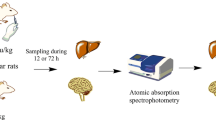
CuGTSM or nCuGTSM (10 mg/kg) was administered orally to male macular mice or C3H/HeNCrl mice (control), and plasma was obtained by serial blood sampling. Plasma concentrations of CuGTSM and GTSM were measured by LC-MS/MS and pharmacokinetic parameters were calculated.
Results
When CuGTSM was administered orally, CuGTSM and GTSM were both detected in the plasma of both mouse strains. When nCuGTSM was administered, the Cmax was markedly higher, and the mean residence time was longer than when CuGTSM was administered for both CuGTSM and GTSM in both mouse strains. With macular mice, the AUC ratio (GTSM/CuGTSM) was markedly higher and the plasma CuGTSM concentration was lower than with C3H/HeNCrl mice when either CuGTSM or nCuGTSM was administered.
Conclusion
Absorption of orally administered CuGTSM was confirmed in macular mice, and the nano-formulation improved the absorption and retention of CuGTSM in the body. However, the plasma concentration of CuGTSM was lower in macular mice than in control mice, suggesting easier dissociation of CuGTSM.






Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the concentration-time curve
- AUMC:
-
Area under the first moment curve
- BBB:
-
Blood-brain barrier
- Cmax :
-
Maximum plasma concentration
- Cu:
-
Copper
- CuATSM:
-
Diacetyl-bis(N(4)-methylthiosemicarbazonato)-copper(II)
- CuBTSCs:
-
Copper(II) bis(thiosemicarbazones)
- CuGTSM:
-
Glyoxal-bis (N(4)-methylthiosemicarbazonato)-copper(II)
- Cu(OAc)2 :
-
Copper(II) acetate monohydrate
- CuPTSM:
-
Pyruvaldehyde bis(N(4)-methylthiosemicarbazonato)-copper(II)
- DEDTC:
-
Diethyldithiocarbamate
- DMDTC:
-
Dimethyldithiocarbamate
- IS:
-
Internal standard
- MRT:
-
Mean residence time
- MW:
-
Molecular weight
- nCuGTSM:
-
Nanosized CuGTSM
- QOL:
-
Quality of life
- SDS:
-
Sodium dodecyl sulfate
- SSV:
-
Standard suspension vehicle
- T1/2 :
-
Elimination half-life
- Tmax :
-
Time to maximum plasma concentration
References
Tümer Z, Møller LB. Menkes disease. Eur J Hum Genet. 2010;18:511–8.
Vulpe C, Levinson B, Whitney S, Packman S, Gitschier J. Isolation of a candidate gene for Menkes disease and evidence that it encodes a copper-transporting ATPase. Nat Genet. 1993;3:7–13.
Kodama H, Murata Y. Molecular genetics and pathophysiology of Menkes disease. Pediatr Int. 1999;41:430–35.
Chelly J, Tümer Z, Tønnesen T, Petterson A, Ishikawa-Brush Y, Tommerup N, Horn N, Monaco AP. Isolation of a candidate gene for Menkes disease that encodes a potential heavy metal binding protein. Nat Genet. 1993;3:14–9.
Mercer JF, Livingston J, Hall B, Paynter JA, Begy C, Chandrasekharappa S, et al. Isolation of a partial candidate gene for Menkes disease by positional cloning. Nat Genet. 1993;3:20–5.
Kaler SG, Gallo LK, Proud VK, Percy AK, Mark Y, Segal NA, Goldstein DS, Holmes CS, Gahl WA. Occipital horn syndrome and a mild Menkes phenotype associated with splice site mutations at the MNK locus. Nat Genet. 1994;8:195–202.
Tümer Z, Horn N. Menkes disease: recent advances and new aspects. J Med Genet. 1997;34:265–74.
Lutsenko S, Barnes NL, Bartee MY, Dmitriev OY. Function and regulation of human copper-transporting ATPases. Physiol Rev. 2007;87:1011–46.
Choi BS, Zheng W. Copper transport to the brain by the blood-brain barrier and blood-CSF barrier. Brain Res. 2009;1248:14–21.
Sarkar B, Lingertat-Walsh K, Clarke JT. Copper-histidine therapy for Menkes disease. J Pediatr. 1993;123:828–30.
Kodama H, Fujisawa C, Bhadhprasit W. Pathology, clinical features and treatments of congenital copper metabolic disorders-focus on neurologic aspects. Brain and Development. 2011;33:243–51.
Tanaka K, Kobayashi K, Fujita Y, Fukuhara C, Onosaka S, Min K. Effects of chelators on copper therapy of macular mouse, a model animal of Menkes’ kinky disease. Res Commun Chem Pathol Pharmacol. 1990;69:217–27.
Lenartowicz M, Krzeptowski W, Koteja P, Chrzascik K, Møller LB. Prenatal treatment of mosaic mice (Atp7a mo-ms) mouse model for Menkes disease, with copper combined by dimethyldithiocarbamate (DMDTC). PLoS ONE. 2012;7:e40400.
Kodama H, Sato E, Gu YH, Shiga K, Fujisawa C, Kozuma T. Effect of copper and diethyldithiocarbamate combination therapy on the macular mouse, an animal model of Menkes disease. J Inherit Metab Dis. 2005;28:971–8.
Bhadhprasit W, Kodama H, Fujisawa C, Hiroki T, Ogawa E. Effect of copper and disulfiram combination therapy on the macular mouse, a model of Menkes disease. J Trace Elem Med Biol. 2012;26:105–8.
Ogawa E, Kodama H. Effects of disulfiram treatment in patients with Menkes disease and occipital horn syndrome. J Trace Elem Med Biol. 2012;26:102–4.
Paterson BM, Donnelly PS. Copper complexes of bis(thiosemicarbazones): from chemotherapeutics to diagnostic and therapeutic radiopharmaceuticals. Chem Soc Rev. 2011;40:3005–18.
Yoshii Y, Matsumoto H, Yoshimoto M, Furukawa T, Morokoshi Y, Sogawa C, et al. Controlled administration of penicillamine reduces radiation exposure in critical organs during 64Cu-ATSM internal radiotherapy: a novel strategy for liver protection. PLoS One. 2014;9:e86996.
Matsumoto H, Yoshii Y, Baden A, Kaneko E, Hashimoto H, Suzuki H, et al. Preclinical pharmacokinetic and safety studies of copper-diacetyl-Bis(N4-Methylthiosemicarbazone) (Cu-ATSM): Translational studies for internal radiotherapy. Transl Oncol. 2019;12:1206–12.
Crouch PJ, Hung LW, Adlard PA, Cortes M, Lal V, Filiz G, Perez KA, Nurjono M, Caragounis A, du T, Laughton K, Volitakis I, Bush AI, Li QX, Masters CL, Cappai R, Cherny RA, Donnelly PS, White AR, Barnham KJ. Increasing cu bioavailability inhibits Aβ oligomers and tau phosphorylation. Proc Natl Acad Sci U S A. 2009;106:381–6.
Speer A, Shrestha TB, Bossmann SH, Basaraba RJ, Harber GJ, Michalek SM, Niederweis M, Kutsch O, Wolschendorf F. Copper-boosting compounds: a novel concept for antimycobacterial drug discovery. Antimicrob Agents Chemother. 2013;57:1089–91.
Dehdashti F, Grigsby PW, Lewis JS, Laforest R, Siegel BA, Welch MJ. Assessing tumor hypoxia in cervical cancer by PET with 60Cu-labeled diacetylbis(N4-methylthiosemicarbazone). J Nucl Med. 2008;49:201–5.
Dietz DW, Dehdashti F, Grigsby PW, Malyapa RS, Myerson RJ, Picus J, Ritter J, Lewis JS, Welch MJ, Siegel BA. Tumor hypoxia detected by positron emission tomography with 60Cu-ATSM as a predictor of response and survival in patients undergoing neoadjuvant chemoradiotherapy for rectal carcinoma: a pilot study. Dis Colon Rectum. 2008;51:1641–8.
Lewis JS, Laforest R, Dehdashti F, Grigsby PW, Welch MJ, Siegel BA. An imaging comparison of 64Cu-ATSM and 60Cu-ATSM in cancer of the uterine cervix. J Nucl Med. 2008;49:1177–82.
Munakata M, Kodama H, Fujisawa C, Hiroki T, Kimura K, Watanabe M, Nishikawa M, Tsuchiya S. Copper-trafficking efficacy of copper-pyruvaldehyde bis(N4-methylthiosemicarbazone) on the macular mouse, an animal model of Menkes disease. Pediatr Res. 2012;72:270–6.
Munakata M, Kodama H, Tani N, Kimura K, Takahashi H, Maruyama K, Sakamoto Y, Kure S. Menkes disease: Oral administration of glyoxal-bis(N(4)-methylthiosemicarbazonato)-copper(II) rescues the macular mouse. Pediatr Res. 2018;84:770–7.
Andres SA, Bajaj K, Vishnosky NS, Peterson MA, Mashuta MS, Buchanan RM, Bates PJ, Grapperhaus CA. Synthesis, characterization, and biological activity of hybrid thiosemicarbazone-alkylthiocarbamate metal complexes. Inorg Chem. 2020;59:4924–35.
Torchilin VP. Multifunctional Nanocarriers. Adv Drug Deliv Rev. 2006;58:1532–55.
Taghipour YD, Hajialyani M, Naseri R, Hesari M, Mohammadi P, Stefanucci A, et al. Nanoformulations of natural products for management of metabolic syndrome. Int J Nanomedicine. 2019;14:5303–21.
Gingras BA, Suprunchuk T, Bayley CH. The preparation of some thiosemicarbazones and their copper complexes part III. Can J Chem. 1902;40:1053–9.
Betts HM, Barnard PJ, Bayly SR, Dilworth JR, Gee AD, Holland JP. Controlled axial coordination: solid-phase synthesis and purification of metallo-radiopharmaceuticals. Angew Chem Int Ed. 2008;47:8416–9.
Bhattacharjee A, Yang H, Duffy M, Robinson E, Conrad-Antoville A, Lu YW, Capps T, Braiterman L, Wolfgang M, Murphy MP, Yi L, Kaler SG, Lutsenko S, Ralle M. The activity of Menkes disease protein ATP7A is essential for redox balance in mitochondria. J Biol Chem. 2016;291:16644–58.
Acknowledgments and Disclosures
We thank Dr. Yoshimasa Sakamoto, Dr. Yukari Takase and Ms. Yuko Hino for breeding C3H/HeNCrl mice and macular mice. The authors declare that they have no conflict of interest.
Funding
This work was supported by JSPS KAKENHI Grant Number JP18K06762.
Author information
Authors and Affiliations
Contributions
Yoshiaki Yamagishi and Toshiyuki Kudo contributed equally to this work. Yoshiaki Yamagishi, Toshiyuki Kudo, Toshiro Fukami and Kiyomi Ito contributed to the study conception and design. Material preparation, data collection and analysis were performed by Yoshiaki Yamagishi, Toshiyuki Kudo, Masafumi Oyumi, Yusuke Sakamoto, Kazuki Takahashi, Taiki Akashi, Shohei Kobayashi, Takeaki Kawakami, Hitomi Goda, Hiroko Kodama, Yasuhiro Sato, Mitsutoshi Munakata, Kosho Makino and Hideyo Takahashi. The first draft of the manuscript was written by Yoshiaki Yamagishi, Toshiyuki Kudo, Taiki Akashi, Hideyo Takahashi, Toshiro Fukami and Kiyomi Ito. All authors read and approved the final manuscript.
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yamagishi, Y., Kudo, T., Oyumi, M. et al. Pharmacokinetics of CuGTSM, a Novel Drug Candidate, in a Mouse Model of Menkes Disease. Pharm Res 38, 1335–1344 (2021). https://doi.org/10.1007/s11095-021-03090-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-021-03090-0