Abstract
Purpose
Monocarboxylate transporter (MCT) inhibition represents a potential treatment strategy for γ-hydroxybutyric acid (GHB) overdose by blocking its renal reabsorption in the kidney. This study further evaluated the effects of a novel, highly potent MCT inhibitor, AR-C155858, on GHB toxicokinetics/toxicodynamics (TK/TD).
Methods
Rats were administered GHB (200, 600 or 1500 mg/kg i.v. or 1500 mg/kg po) with and without AR-C155858. Breathing frequency was continuously monitored using whole-body plethysmography. Plasma and urine samples were collected up to 8 h. The effect of AR-C155858 on GHB brain/plasma partitioning was also assessed.
Results
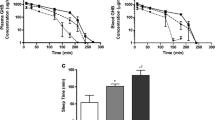
AR-C155858 treatment significantly increased GHB renal and total clearance after intravenous GHB administration at all the GHB doses used in this study. GHB-induced respiratory depression was significantly improved by AR-C155858 as demonstrated by an improvement in the respiratory rate. AR-C155858 treatment also resulted in a significant reduction in brain/plasma partitioning of GHB (0.1 ± 0.03) when compared to GHB alone (0.25 ± 0.02). GHB CLR and CLoral (CL/F) following oral administration were also significantly increased following AR-C155858 treatment (from 1.82 ± 0.63 to 5.74 ± 0.86 and 6.52 ± 0.88 to 10.2 ± 0.75 ml/min/kg, respectively).
Conclusion
The novel and highly potent MCT inhibitor represents a potential treatment option for GHB overdose.






Similar content being viewed by others
Abbreviations
- AUEC:
-
Area under the effect curve
- AUC:
-
Area under the plasma concentration-time curve
- Cl:
-
Clearance
- ClM :
-
Metabolic clearance
- ClR :
-
Renal clearance
- Emax :
-
Maximum pharmacodynamic effect
- GABA:
-
γ-aminobutyric acid
- GHB:
-
γ-hydroxybutyrate
- MCT:
-
Monocarboxylate transporter
- Td :
-
Duration of effect
- TK/TD:
-
Toxicokinetics/toxicodynamics
References
Maitre M. The gamma-hydroxybutyrate signalling system in brain: organization and functional implications. Prog Neurobiol. 1997;51(3):337–61.
Wong CG, Chan KF, Gibson KM, Snead OC. Gamma-hydroxybutyric acid: neurobiology and toxicology of a recreational drug. Toxicol Rev. 2004;23(1):3–20.
Li J, Stokes SA, Woeckener A. A tale of novel intoxication: a review of the effects of gamma-hydroxybutyric acid with recommendations for management. Ann Emerg Med. 1998;31(6):729–36.
Mason PE, Kerns 2nd WP. Gamma hydroxybutyric acid (GHB) intoxication. Acad Emerg Med. 2002;9(7):730–9.
Zvosec DL, Smith SW, Porrata T, Strobl AQ, Dyer JE. Case series of 226 gamma-hydroxybutyrate-associated deaths: lethal toxicity and trauma. Am J Emerg Med. 2011;29(3):319–32.
Palatini P, Tedeschi L, Frison G, Padrini R, Zordan R, Orlando R, et al. Dose-dependent absorption and elimination of gamma-hydroxybutyric acid in healthy volunteers. Eur J Clin Pharmacol. 1993;45(4):353–6.
Lettieri JT, Fung HL. Dose-dependent pharmacokinetics and hypnotic effects of sodium gamma-hydroxybutyrate in the rat. J Pharmacol Exp Ther. 1979;208(1):7–11.
Arena C, Fung HL. Absorption of sodium gamma-hydroxybutyrate and its prodrug gamma-butyrolactone: relationship between in vitro transport and in vivo absorption. J Pharm Sci. 1980;69(3):356–8.
Morris ME, Hu K, Wang Q. Renal clearance of gamma-hydroxybutyric acid in rats: increasing renal elimination as a detoxification strategy. J Pharmacol Exp Ther. 2005;313(3):1194–202.
Lettieri J, Fung HL. Absorption and first-pass metabolism of 14C-gamma-hydroxybutyric acid. Res Commun Chem Pathol Pharmacol. 1976;13(3):425–37.
Wang Q, Darling IM, Morris ME. Transport of gamma-hydroxybutyrate in rat kidney membrane vesicles: role of monocarboxylate transporters. J Pharmacol Exp Ther. 2006;318(2):751–61.
Halestrap AP, Price NT. The proton-linked monocarboxylate transporter (MCT) family: structure, function and regulation. Biochem J. 1999;343(Pt 2):281–99.
Ganapathy V, Thangaraju M, Gopal E, Martin PM, Itagaki S, Miyauchi S, et al. Sodium-coupled monocarboxylate transporters in normal tissues and in cancer. AAPS J. 2008;10(1):193–9.
Gopal E, Fei YJ, Sugawara M, Miyauchi S, Zhuang L, Martin P, et al. Expression of slc5a8 in kidney and its role in Na(+)-coupled transport of lactate. J Biol Chem. 2004;279(43):44522–32.
Wang Q, Lu Y, Morris ME. Monocarboxylate transporter (MCT) mediates the transport of gamma-hydroxybutyrate in human kidney HK-2 cells. Pharm Res. 2007;24(6):1067–78.
Cui D, Morris ME. The drug of abuse gamma-hydroxybutyrate is a substrate for sodium-coupled monocarboxylate transporter (SMCT) 1 (SLC5A8): characterization of SMCT-mediated uptake and inhibition. Drug Metab Dispos. 2009;37(7):1404–10.
Wang Q, Morris ME. Flavonoids modulate monocarboxylate transporter-1-mediated transport of gamma-hydroxybutyrate in vitro and in vivo. Drug Metab Dispos. 2007;35(2):201–8.
Wang Q, Wang X, Morris ME. Effects of L-lactate and D-mannitol on gamma-hydroxybutyrate toxicokinetics and toxicodynamics in rats. Drug Metab Dispos. 2008;36(11):2244–51.
Morris ME, Morse BL, Baciewicz GJ, Tessena MM, Acquisto NM, Hutchinson DJ, DiCenzo R. Monocarboxylate transporter inhibition with osmotic diuresis increases γ-hydroxybutyrate renal elimination in humans: a proof-of-concept study. J Clinic Toxicol. 2011;1(2):1000105.
Carai MA, Colombo G, Brunetti G, Melis S, Serra S, Vacca G, et al. Role of GABA(B) receptors in the sedative/hypnotic effect of gamma-hydroxybutyric acid. Eur J Pharmacol. 2001;428(3):315–21.
Kaupmann K, Cryan JF, Wellendorph P, Mombereau C, Sansig G, Klebs K, et al. Specific gamma-hydroxybutyrate-binding sites but loss of pharmacological effects of gamma-hydroxybutyrate in GABA(B)(1)-deficient mice. Eur J Neurosci. 2003;18(10):2722–30.
Morse BL, Vijay N, Morris ME. gamma-Hydroxybutyrate (GHB)-induced respiratory depression: combined receptor-transporter inhibition therapy for treatment in GHB overdose. Mol Pharmacol. 2012;82(2):226–35.
Bhattacharya I, Boje KM. GHB (gamma-hydroxybutyrate) carrier-mediated transport across the blood–brain barrier. J Pharmacol Exp Ther. 2004;311(1):92–8.
Roiko SA, Felmlee MA, Morris ME. Brain uptake of the drug of abuse gamma-hydroxybutyric acid in rats. Drug Metab Dispos. 2012;40(1):212–8.
Vijay N, Morris ME. Role of monocarboxylate transporters in drug delivery to the brain. Curr Pharm Des. 2014;20(10):1487–98.
Roiko SA, Vijay N, Felmlee MA, Morris ME. Brain extracellular gamma-hydroxybutyrate concentrations are decreased by L-lactate in rats: role in the treatment of overdoses. Pharm Res. 2013;30(5):1338–48.
Pahlman C, Qi Z, Murray CM, Ferguson D, Bundick RV, Donald DK, et al. Immunosuppressive properties of a series of novel inhibitors of the monocarboxylate transporter MCT-1. Transpl Int. 2013;26(1):22–9.
Ekberg H, Qi Z, Pahlman C, Veress B, Bundick RV, Craggs RI, et al. The specific monocarboxylate transporter-1 (MCT-1) inhibitor, AR-C117977, induces donor-specific suppression, reducing acute and chronic allograft rejection in the rat. Transplantation. 2007;84(9):1191–9.
Ovens MJ, Davies AJ, Wilson MC, Murray CM, Halestrap AP. AR-C155858 is a potent inhibitor of monocarboxylate transporters MCT1 and MCT2 that binds to an intracellular site involving transmembrane helices 7–10. Biochem J. 2010;425(3):523–30.
Felmlee MA, Roiko SA, Morse BL, Morris ME. Concentration-effect relationships for the drug of abuse gamma-hydroxybutyric acid. J Pharmacol Exp Ther. 2010;333(3):764–71.
Drasbek KR, Christensen J, Jensen K. Gamma-hydroxybutyrate–a drug of abuse. Acta Neurol Scand. 2006;114(3):145–56.
Shitara Y, Nagamatsu Y, Wada S, Sugiyama Y, Horie T. Long-lasting inhibition of the transporter-mediated hepatic uptake of sulfobromophthalein by cyclosporin a in rats. Drug Metab Dispos. 2009;37(6):1172–8.
Morse BL, Morris ME. Effects of monocarboxylate transporter inhibition on the oral toxicokinetics/toxicodynamics of gamma-hydroxybutyrate and gamma-butyrolactone. J Pharmacol Exp Ther. 2013;345(1):102–10.
Kaufman EE, Nelson T. An overview of gamma-hydroxybutyrate catabolism: the role of the cytosolic NADP(+)-dependent oxidoreductase EC 1.1.1.19 and of a mitochondrial hydroxyacid-oxoacid transhydrogenase in the initial, rate-limiting step in this pathway. Neurochem Res. 1991;16(9):965–74.
Gerhart DZ, Enerson BE, Zhdankina OY, Leino RL, Drewes LR. Expression of monocarboxylate transporter MCT1 by brain endothelium and glia in adult and suckling rats. Am J Physiol. 1997;273(1 Pt 1):E207–13.
Morse BL, Felmlee MA, Morris ME. gamma-Hydroxybutyrate blood/plasma partitioning: effect of physiologic pH on transport by monocarboxylate transporters. Drug Metab Dispos. 2012;40(1):64–9.
Galicia M, Nogue S, Miro O. Liquid ecstasy intoxication: clinical features of 505 consecutive emergency department patients. Emerg Med J. 2011;28(6):462–6.
Morse BL, Morris ME. Toxicokinetics/toxicodynamics of gamma-hydroxybutyrate-ethanol intoxication: evaluation of potential treatment strategies. J Pharmacol Exp Ther. 2013;346(3):504–13.
Lam WK, Felmlee MA, Morris ME. Monocarboxylate transporter-mediated transport of gamma-hydroxybutyric acid in human intestinal Caco-2 cells. Drug Metab Dispos. 2010;38(3):441–7.
Morse BA, Vijay N, Morris ME. Mechanistic modeling of Monocarboxylate transporter-mediated toxicokinetic/toxicodynamic interactions between γ-hydroxybutyrate and L-lactate. AAPS J. 2014;16(4):756–70.
ACKNOWLEDGMENTS AND DISCLOSURES
The authors thank Donna Ruszaj for her assistance in developing the current LC-MS/MS method. This work was supported by the National Institutes of Health National Institute on Drug Abuse [grant DA023223]. NV was funded in part by a fellowship from Pfizer Global Inc.
Authorship Contributions
Participated in research design: Morris, Vijay and Morse
Conducted experiments: Vijay and Morse
Contributed new reagents or analytic tools: Morris and Vijay
Performed data analysis: Vijay, Morris
Wrote or contributed to the writing of the manuscript: Morris and Vijay
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vijay, N., Morse, B.L. & Morris, M.E. A Novel Monocarboxylate Transporter Inhibitor as a Potential Treatment Strategy for γ-Hydroxybutyric Acid Overdose. Pharm Res 32, 1894–1906 (2015). https://doi.org/10.1007/s11095-014-1583-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-014-1583-0