ABSTRACT
Purpose
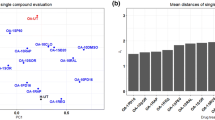
In the treatment of osteoarthritis (OA), some of the therapeutic approaches require delivery of drug(s) to the diseased cartilage. Presence of adequate drug levels in the cartilage is one of the important criteria in selection and ranking of lead compounds. The purpose of this study was to investigate the correlation in cartilage compound levels between in vitro experiments and in vivo animal studies.
Materials and Methods
Bovine cartilage samples were incubated with test compounds of various concentrations in a culture medium, in the absence or presence of 25 mg/ml of serum albumin which served as an artificial synovial fluid (SF). The test compounds were also dosed to rabbits, the animal model used for efficacy studies, over a six-week treatment period. Test article concentrations in plasma, SF, and cartilage were determined by LC/MS/MS analysis.
Results and Conclusions
A correlation in cartilage drug concentration was observed between in vitro and in vivo studies. Plasma protein binding and the test article’s affinity to cartilage were the major determining factors for drug delivery to cartilage in vivo.


Similar content being viewed by others
Abbreviations
- \({\text{AUC}}_{{\text{cartilage}}}^{} \) :
-
area under the compound concentration-time curve in cartilage
- \({\text{AUC}}_{{\text{diseased\_SF}}}^{{\text{unbound}}} \) or \({\text{AUC}}_{{\text{diseased\_SF}}}^{{\text{total}}} \) :
-
area under the unbound or total compound concentration-time curve in diseased SF
- \({\text{AUC}}_{{\text{plasma}}}^{{\text{unbound}}} \) or \({\text{AUC}}_{{\text{serum}}}^{{\text{unbound}}} \) :
-
area under the unbound compound concentration-time curve in plasma or serum
- \({\text{AUC}}_{{\text{SF}}}^{{\text{unbound}}} \)or \({\text{AUC}}_{{\text{SF}}}^{{\text{total}}} \) :
-
area under the unbound or total compound concentration-time curve in SF
- \({\text{AUC}}_{{\text{plasma}}}^{{\text{total}}} \) or \({\text{AUC}}_{{\text{serum}}}^{{\text{total}}} \) :
-
area under the total compound concentration-time curve in plasma or serum
- \(C_{cartilage}^{} \) :
-
compound concentration in cartilage
- \(C_{{\text{plasma}}}^{} \) or \(C_{{\text{plasma}}}^{{\text{total}}} \) or \({}^{{\text{drug}}}C_{{\text{plasma}}}^{{\text{total}}} \) or \(C_{{\text{serum}}}^{} \) or \(C_{{\text{serum}}}^{{\text{total}}} \) :
-
total compound concentration in plasma or serum
- \(C_{{\text{plasma}}}^{{\text{protein}}} \) or \(C_{{\text{serum}}}^{{\text{protein}}} \) :
-
total protein concentration in plasma or serum
- \(C_{{\text{SF}}}^{} \) or \(C_{{\text{SF}}}^{{\text{total}}} \) or \({}^{{\text{drug}}}C_{{\text{SF}}}^{{\text{total}}} \) or \(C_{{\text{healthy\_SF}}}^{{\text{total}}} \) :
-
total compound concentration in SF
- \(C_{{\text{diseased\_SF}}}^{{\text{unbound}}} \) or \(C_{{\text{diseased\_SF}}}^{{\text{total}}} \) :
-
unbound or total compound concentration in diseased SF
- \(C_{{\text{plasma}}}^{{\text{unbound}}} \) or \([C_{{\text{plasma}}} \times \% _{{\text{free}} - {\text{fraction}}} ]\) or \(C_{{\text{serum}}}^{{\text{unbound}}} \) :
-
unbound compound concentration in plasma or serum
- \(C_{{\text{SF}}}^{{\text{unbound}}} \) or \({}^{{\text{drug}}}C_{{\text{SF}}}^{{\text{unbound}}} \) or \(C_{{\text{healthy\_SF}}}^{{\text{unbound}}} \) :
-
unbound compound concentration in synovial fluid (SF)
- \({}^{{\text{drug}}}C_{{\text{SF}}}^{{\text{bound\_to\_proteins}}} \) or \({}^{{\text{drug}}}C_{{\text{plasma}}}^{{\text{bound\_to\_proteins}}} \) :
-
SF or plasma compound concentrations that associated with SF or plasma proteins
- %free-fraction :
-
percentage of unbound compound in plasma
- SF:
-
synovial fluid
References
J.M. Milner, and T.E. Cawston. Matrix metalloproteinase knockout studies and the potential use of matrix metalloproteinase inhibitors in the rheumatic diseases. Curr. Drug Targets Inflamm. Allergy. 4(3):363–375 (2005).
J. Martel-Pelletier, D.J. Welsch, and J-P. Pelletier. Metalloproteases and inhibitors in arthritic diseases. Best Pract. Res. Clin. Rheumatol. 15(5):805–829 (2001).
S.S. Glasson, R. Askew, B. Sheppard, B. Carito, T. Blanchet, H-L. Ma, C.R. Flannery, D. Peluso, K. Kanki, Z. Yang, M.K. Majumdar, and E.A. Morris. Deletion of active ADAMTS5 prevents cartilage degradation in a murine model of osteoarthritis. Nature. 434:644–648 (2005).
H. Nagase, and M. Kashiwagi. Aggrecanases and cartilage matrix degradation. Arthritis Res. Ther. 5(2):94–103 (2003).
J.W. Skiles, N.C. Gonnella, and A.Y. Jeng. The design, structure, and clinical update of small molecular weight matrix metalloproteinase inhibitors. Curr Med Chem. 11(22):2911–2977 (2004).
M. Sabatini, C. Lesur, M. Thomas, A. Chomel, P. Anract, G. de Nanteuil, and P. Pastoureau. Effect of inhibition of matrix metalloproteinases on cartilage loss in vitro and in a guinea pig model of osteoarthritis. Arthritis Rheum. 52(1):171–180 (2005).
T.G. Benedek. A history of the understanding of cartilage. OsteoArthr. Cartil. 14:203–209 (2006).
H. Imhof, M. Breitnseher, F. Kainberger, and S. Trattnig. Degenerative joint disease: cartilage or vascular disease? Skelet. Radiol. 26:398–403 (1997).
J.E. Shea, and S.C. Miller. Skeletal function and structure: implication of tissue-targeted therapeutics. Adv. Drug Deliv. Rev. 57:945–957 (2005).
J. Li, T.S. Rush III, W. Li, D. DeVincentis, X. Du, Y. Hu, J.R. Thomason, J.S. Xiang, J.S. Skotnicki, and S. Tam. Synthesis and SAR of highly selective MMP-13 inhibitors. Bioorg. Med. Chem. Lett. 15:4961–4966 (2005).
Y. Hu, J. Xiang, M. DiGrandi, X. Du, M. Ipek, L. Laakso, J. Li, W. Li, T. Rush, J. Schmid, J. Skotnicki, S. Tam, J. Thomason, Q. Wang, and J. Levin. Potent, selective and orally bioavailable matrix metalloproteinase-13 inhibitors for the treatment of osteoarthritis. Bioorg. Med. Chem. 13:6629–6644 (2005).
R.A. Gatter, and H.R. Schumacher. A practical handbook of joint fluid analysis, 2nd edition. Lea & Febiger, Philadelphia, 1991, pp. 70–77.
D.J. McCarty. The physiology of normal synovium. In L. Sokoloff (ed.), The Joints and Synovial Fluid, Vol. II, Chapter 7, Academic, New York, 1980, pp. 294–315.
P.S. MacWilliams, and K.R. Friedrichs. Laboratory evaluation and interpretation of synovial fluid. Vet. Clin. Small. Anim. 33:153–178 (2003).
B. Davis, and T. Morris. Physiological parameters in laboratory animals and humans. Pharm. Res. 10:1093–1096 (1993).
P.A. Simkin, M.P. Wu, and D.M. Foster. Articular pharmacokinetics of protein-bound anti-rheumatic agents. Clin. Pharmacokinet. 25:342–50 (1993).
W.F. Elmquist, K.K.H. Chan, and R.J. Sawchuck. Transsynovial drug distribution: synovial mean transit time of diclofenac and other nonsteroidal anti-inflammatory drugs. Pharm. Res. 11:1689–1697 (1994).
S.G. Owen, H.W. Francis, and M.S. Roberts. Disappearance kinetics of solutes from synovial fluid after intra-articular injection. Br. J. Clin. Pharmacol. 38:349–355 (1994).
P. Netter, B. Bannwarth, and M-J. Rojer-Morrot. Recent finding on the pharmacokinetics of non-steriodal anti-inflammatory drugs in synovial fluid. Clin. Pharmacokinet. 17(3):145–162 (1989).
R.O. Day, A.J. McLachlan, G.G. Graham, and K.M. Williams. Pharmacokinetics of nonsteroidal anti-inflammatory drugs in synovial fluid. Clin Pharmacokinet. 36(3):191–210 (1999).
F. Lapicque, P. Vergne, J.Y. Jouzeau, D. Loeuille, P. Gillet, E. Vignon, P. Thomas, P. Velicitat, D. Turck, C. Guillaume, A. Gaucher, P. Bertin, and P. Netter. Articular diffusion of meloxicam after a single oral dose: relationship to cyclo-oxygenase inhibition in synovial cells. Clin. Pharmacokinet. 39(5):369–82 (2000).
O.G. Nilsen. Clinical pharmacokinetics of tenoxicam. Clin. Pharmacokinet. 24:16–43 (1994).
S.X. Peng, E.C. von Bargen, D.M. Bornes, and S. Pikul. Permeability of articular cartilage to matrix metalloprotease inhibitors. Pharm. Res. 15:1414–1418 (1998).
R.C. Evens, and T.M. Quinn. Solute diffusivity correlates with mechanical properties and matrix density of compressed articular cartilage. Arch. Biochem. biophys. 442:1–10 (2005).
J.H. Kimura. The role of water, proteoglycan, and collagen in solute transport in cartilage. In K.E. Kuettner (ed.), Articular Cartilage and Osteoarthritis, Raven, New York, 1991, pp. 355–372.
A.M. Garcia, E.H. Frank, P.E. Grimshaw, and A.J. Grodzinsky. Contributions of fluid convection and electrical migration to transport in cartilage: relevance to loading. Arch. Biochem. Biophys. 333:317–325 (1996).
F. Eckstein, M. Tieschky, S.C. Faber, M. Haubner, H. Kolem, K-H. Endlmeier, and M. Reiser. Effect of physical exercise on cartilage volume and thickness in vivo: MR imaging study. Radiology. 207:243–248 (1998).
U.G. Kersting, J.J. Stubendorff, M.C. Schmidt, and G-P. Bruggemann. Changes in knee cartilage volume and serum COMP concentration after running exercise. Osteoarthr. Cartil. 13:925–934 (2005).
M. Kurowski, and A. Dunky. Transsynovial kinetics of piroxicam in patients with rheumatoid arthritis. Eur. J. Clin. Pharmacol. 34:401–406 (1998).
J.B. Whitiam, K.F. Brown, M.J. Crooks, and G.F.W. Room. Transsynovial distribution of ibuprofen in arthritis patients. Clin. Pharmacol. Ther. 29:487–492 (1981).
R.O. Day, H. Francis, J. Vial, G. Geisslinger, and K.M. Williams. Naproxen concentrations in plasma and synovial fluid and effects on prostanoid concentrations. J. Rheumatol. 22(12):2295–30 (1995).
Acknowledgements
We thank Jessica Doherty, Cindy Clark, Amy Ignatowicz, Terrie Cunliffe-Beamer, and Glen Pedneault for performing in vivo studies.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, Q., Glasson, S., Raut, U. et al. In Vitro–In Vivo Correlation on Delivery of Drug Candidates to Articular Cartilage. Pharm Res 25, 1641–1646 (2008). https://doi.org/10.1007/s11095-008-9557-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-008-9557-8