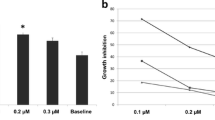
The persistence of human papillomavirus affects the processes of proliferation and differentiation of the stratified squamous epithelium of the cervix with the development of cervical intraepithelial neoplasia and cervical cancer. Hormonal factors have an impact on the process of neoplastic transformation. The aim of this study was an evaluation of the effect of glycyrrhizic acid on the viability of HeLa cervical adenocarcinoma cells at different concentrations of sex steroid hormones. The half-maximal inhibitory concentration (IC50) of glycyrrhizic acid against HeLa cervical adenocarcinoma cells was 72.2 μM. The IC50 of glycyrrhizic acid increased by 13.4% and 17% for testosterone, decreased by 1.8% and 11.8% for estradiol, and increased by 8.7% and 8.6% for progesterone, respectively, in the presence of the hormones at concentrations of 10 μM and 1 μM. Thus, testosterone and progesterone at concentrations of 10 and 1 μM diminished the antiproliferative effect of glycyrrhizic acid, while estradiol at a low concentration (1 μM) enhanced it.

Similar content being viewed by others
References
R. L. Siegel, K. D. Miller, N. S. Wagle, and A. Jemal, Ca-Cancer J. Clin., 73(1), 17 – 48 (2023).
S. I. Rogovskaya, I. V. Mikheeva, O. Yu. Shipulina, et al., Epidemiol. Vaktsinoprofilakt., 62(1), 25 – 33 (2012).
Russian Society of Obstetricians and Gynecologists. Russian Society of Specialists on Prevention and Treatment of Reproductive System Tumors. Clinical Recommendations (2020).
V. F. Levshin and A. Ya. Zavel’skaya, Vopr. Onkol., 63(3), 506 – 516 (2017).
M. L. Bristol, C. D. James, X. Wang, et al., mSphere, 5(2), e00049 – 20 (2020).
A. Gadducci, S. Cosio, and F. Fruzzetti, Anticancer Res., 40(11), 5995 – 6002 (2020).
J.-Q. Ma, X.-H. Wang, L.-P. Tang, et al., Int. J. Clin. Exp. Med., 8(4), 5571 – 5575 (2015).
M. Ruutu, J. Rautava, A. Turunen, et al., Cytotechnology, 70(1), 235 – 244 (2018).
L. Hefler, C. Grimm, C. Tempfer, and A. Reinthaller, Anticancer Res., 30(4), 1257 – 1261 (2010).
K. Baskaran, P. K. Kumar, K. Santha, and I. Sivakamasundari, J. Med. Sci. Res., 6(3), 74 – 79 (2018).
E. Roura, N. Travier, T. Waterboer, et al., PLoS One, 11(3), e0151427 (2016).
H. Xu, S. Egger, L. S. Velentzis, et al., Cancer Epidemiol., 55, 162 – 169 (2018).
S. Mitra, M. S. Lami, A. Ghosh, et al., Cancers, 12(3), 759 – 785 (2022).
G. Garcia-Salazar, Z. Urban-Morlan, S. Mendoza-Elvira, et al., Intervirology, 66(1), 41 – 53 (2022).
A. Farooqui, F. Khan, I. Khan, et al., Biomed. Pharmacother., 97, 752 – 764 (2018).
M. Saeed, J. Pharm. Res. Int., 32(25), 52 – 66 (2020).
Y. B. Ko, B. R. Kim, S. L. Nam, et al., Cell. Signalling, 26(4), 777 – 783 (2014).
R. Smolarczyk, T. Cichon, S. Matuszczak, et al., Arch. Immunol. Ther. Exp., 60(5), 391 – 399 (2012).
G. Vergoten and C. Bailly, Med. Drug Discovery, 7, 100058 (2020).
Instructions on Medical Use of Epigen Intim (2016).
A. Wdowiak, N. Farahmandlou, A. Tajik, et al., J. Biol. Stud., 4(3), 106 – 119 (2021).
P. Kumar, A. Nagarajan, and P. D. Uchil, Cold Spring Harbor Protoc., No. 6, 095505 (2018).
J. L. Sebaugh, Pharm. Stat., 10(2), 128 – 134 (2011).
I. A. Kirilyuk, V. A. Svyatchenko, D. A. Morozov, et al., Antibiot. Khimioter., 57(1), 3 – 12 (2012).
H. Hosseinzadeh and M. Nassiri-Asl, Phytother. Res., 29(12), 1868 – 1886 (2015).
R. Jain, M. A. Hussein, S. Pierce, et al., Pharmacol. Res., 178, 106138 (2022).
Y. Satomi, H. Nishino, and S. Shibata, Anticancer Res., 25(6B), 4043 – 4047 (2005).
G. Sharma, S. Kar, S. Palit, and P. K. Das, J. Cell Physiol., 227(5), 1923 – 1931 (2012).
D. Wang, H. K. Wong, Y. B. Feng, and Z. J. Zhang, J. Neurooncol., 116(2), 221 – 230 (2014).
J. E. Klaunig and Z. Wang, Curr. Opin. Toxicol., 7, 116 – 121 (2018).
M. H. Nascimento and D. R. de Araujo, Future Pharmacol., 2, 1 – 15 (2022).
D. Njus, P. M. Kelley, Y. J. Tu, and H. B. Schlegel, Free Radical Biol. Med., 159, 37 – 43 (2020).
N. T. T. Nga, V. T. An, and D. D. Quang, Vietnam J. Sci. Technol., 57(4), 485 – 490 (2019).
A. R. Shahverdi, F. Shahverdi, E. Faghfuri, et al., Arch. Med. Res., 49(1), 10 – 17 (2018).
J. Ji, P. Zuo, and Y. L. Wang, Nanoscale Res. Lett., 10(1), 453 – 461 (2015).
T. E. Belokrinitskaya, Yu. N. Ponomareva, G. M. Lomneva, et al., Acta Biomed. Sci., No. 1, 143 – 147 (2005).
M. Hong, J. Wang, C. Su, et al., Int. J. Gynecol. Cancer, 27(6), 1247 – 1255 (2017).
F. Garrido, C. M. Wild, U. Jeschke, et al., Int. J. Mol. Sci., 24(3), 2815 – 2828 (2023).
E. Zhang, Y. Zhang, Z. Fan, et al., Molecules, 25(8), 1960 – 1974 (2020).
R. Lopez-Romero, M. Rodriguez-Esquivel, P. Romero-Morelos, et al., Int. J. Clin. Exp. Pathol., 12(9), 3208 – 3221 (2019).
S. Scholl, M. Popovic, A. De la Rochefordiere, et al., EBioMedicine, 43, 253 – 260 (2019).
T. Matsumoto, T. Suzuki, M. Nakamura, et al., Cancer Med., 12(9), 10816 – 10828 (2023).
J. Wei, Y. Wang, K. Shi, and Y. Wang, BioMed Res. Int., 2020, 8959210 (2020).
Q. Fan, T. Huang, X. Sun, et al., Exp. Ther. Med., 21(5), 414 – 424 (2021).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Khimiko-Farmatsevticheskii Zhurnal, Vol. 58, No. 1, pp. 3 – 9, January, 2024.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Filimonova, M.S., Shimanovskiy, N.L. Effect of Glycyrrhizic Acid on the Viability of Hela Cervical Adenocarcinoma Cell Line at Different Concentrations of Sex Steroid Hormones. Pharm Chem J (2024). https://doi.org/10.1007/s11094-024-03112-2
Received:
Published:
DOI: https://doi.org/10.1007/s11094-024-03112-2