Abstract
Purpose
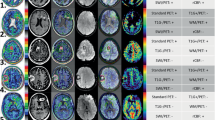
To identify qualitative MRI features of non-(contrast)-enhancing tumor (nCET) in glioblastoma’s T2-FLAIR hyperintense lesion.
Methods
Thirty-three histologically confirmed glioblastoma patients whose T1-, T2- and contrast-enhanced T1-weighted MRI and 11C-methionine positron emission tomography (Met-PET) were available were included in this study. Met-PET was utilized as a surrogate for tumor burden. Imaging features for identifying nCET were searched by qualitative examination of 156 targets. A new scoring system to identify nCET was established and validated by two independent observers.
Results
Three imaging features were found helpful for identifying nCET; “Bulky gray matter involvement”, “Around the rim of contrast-enhancement (Around-rim),” and “High-intensity on T1WI and low-intensity on T2WI (HighT1LowT2)” resulting in an nCET score = 2 × Bulky gray matter involvement – 2 × Around-rim + HighT1LowT2 + 2. The nCET score’s classification performances of two independent observers measured by AUC were 0.78 and 0.80, with sensitivities and specificities using a threshold of four being 0.443 and 0.771, and 0.916 and 0.768, respectively. The weighted kappa coefficient for the nCET score was 0.946.
Conclusion
The current investigation demonstrated that qualitative assessments of glioblastoma’s MRI might help identify nCET in T2/FLAIR high-intensity lesions. The novel nCET score is expected to aid in expanding treatment targets within the T2/FLAIR high-intensity lesions.
Graphical abstract






Similar content being viewed by others
Data availability
The data generated and analyzed during the current study are not publicly available for legal/ethical reasons but are available from the corresponding author upon reasonable request.
References
Sanai N, Polley MY, McDermott MW et al (2011) An extent of resection threshold for newly diagnosed glioblastomas: clinical article. J Neurosurg 115:3–8. https://doi.org/10.3171/2011.2.jns10998
Li YM, Suki D, Hess K, Sawaya R (2016) The influence of maximum safe resection of glioblastoma on survival in 1229 patients: can we do better than gross-total resection? J Neurosurg 124:977–988. https://doi.org/10.3171/2015.5.jns142087
Lacroix M, Abi-Said D, Fourney DR et al (2001) A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg 95:190–198. https://doi.org/10.3171/jns.2001.95.2.0190
Kinoshita M, Arita H, Okita Y et al (2016) Comparison of diffusion tensor imaging and 11 C-methionine positron emission tomography for reliable prediction of tumor cell density in gliomas. J Neurosurg 125:1136–1142. https://doi.org/10.3171/2015.11.jns151848
Molinaro AM, Hervey-Jumper S, Morshed RA et al (2020) Association of maximal extent of resection of contrast-enhanced and non–contrast-enhanced tumor with survival within molecular subgroups of patients with newly diagnosed glioblastoma. Jama Oncol 6:495–503. https://doi.org/10.1001/jamaoncol.2019.6143
Sengupta A, Agarwal S, Gupta PK et al (2018) On differentiation between vasogenic edema and non-enhancing tumor in high-grade glioma patients using a support vector machine classifier based upon pre and post-surgery MRI images. Eur J Radiol 106:199–208. https://doi.org/10.1016/j.ejrad.2018.07.018
Takahashi S, Takahashi M, Kinoshita M et al (2021) Fine-tuning approach for segmentation of gliomas in brain magnetic resonance images with a machine learning method to normalize image differences among facilities. Cancers 13:1415. https://doi.org/10.3390/cancers13061415
Pope WB, Sayre J, Perlina A et al (2005) MR imaging correlates of survival in patients with high-grade gliomas. AJNR Am J Neuroradiol 26:2466–2474
Lasocki A, Gaillard F, Tacey M et al (2015) Incidence and prognostic significance of non-enhancing cortical signal abnormality in glioblastoma. J Méd Imaging Radiat Oncol 60:66–73. https://doi.org/10.1111/1754-9485.12421
Lasocki A, Gaillard F (2019) Non-contrast-enhancing tumor: a new frontier in glioblastoma research. Am J Neuroradiol 40:758–765. https://doi.org/10.3174/ajnr.a6025
Kracht LW, Miletic H, Busch S et al (2004) Delineation of brain tumor extent with [11C]l-methionine positron emission tomography. Clin Cancer Res 10:7163–7170. https://doi.org/10.1158/1078-0432.ccr-04-0262
Okita Y, Kinoshita M, Goto T et al (2010) 11C-methionine uptake correlates with tumor cell density rather than with microvessel density in glioma: a stereotactic image-histology comparison. Neuroimage 49:2977–2982. https://doi.org/10.1016/j.neuroimage.2009.11.024
Kinoshita M, Arita H, Goto T et al (2012) A novel PET index, 18F-FDG–11C-methionine uptake decoupling score, reflects glioma cell infiltration. J Nucl Med 53:1701–1708. https://doi.org/10.2967/jnumed.112.104992
Verburg N, Hoefnagels FWA, Barkhof F et al (2017) Diagnostic accuracy of neuroimaging to delineate diffuse gliomas within the brain: a meta-analysis. Am J Neuroradiol 38:1884–1891. https://doi.org/10.3174/ajnr.a5368
Arita H, Kinoshita M, Kagawa N et al (2011) 11C-methionine uptake and intraoperative 5‐aminolevulinic acid‐induced fluorescence as separate index markers of cell density in glioma. Cancer 118:1619–1627. https://doi.org/10.1002/cncr.26445
Galldiks N, Ullrich R, Schroeter M et al (2010) Volumetry of [11C]-methionine PET uptake and MRI contrast enhancement in patients with recurrent glioblastoma multiforme. Eur J Nucl Med Mol I 37:84–92. https://doi.org/10.1007/s00259-009-1219-5
Nariai T, Tanaka Y, Wakimoto H et al (2005) Usefulness of l -[methyl-11C] methionine—positron emission tomography as a biological monitoring tool in the treatment of glioma. J Neurosurg 103:498–507. https://doi.org/10.3171/jns.2005.103.3.0498
Hatakeyama T, Kawai N, Nishiyama Y et al (2008) 11C-methionine (MET) and 18F-fluorothymidine (FLT) PET in patients with newly diagnosed glioma. Eur J Nucl Med Mol I 35:2009–2017. https://doi.org/10.1007/s00259-008-0847-5
Čížek J, Herholz K, Vollmar S et al (2004) Fast and robust registration of PET and MR images of human brain. Neuroimage 22:434–442. https://doi.org/10.1016/j.neuroimage.2004.01.016
D’Alessio A, Proietti G, Sica G, Scicchitano BM (2019) Pathological and molecular features of glioblastoma and its peritumoral tissue. Cancers 11:469. https://doi.org/10.3390/cancers11040469
de Leeuw CN, Vogelbaum MA (2018) Supratotal resection in glioma: a systematic review. Neuro-Oncol 21:179–188. https://doi.org/10.1093/neuonc/noy166
Verburg N, Koopman T, Yaqub MM et al (2019) Improved detection of diffuse glioma infiltration with imaging combinations: a diagnostic accuracy study. Neurooncology 22:412–422. https://doi.org/10.1093/neuonc/noz180
Yan JL, Li C, van der Hoorn A et al (2020) A neural network approach to identify the peritumoral invasive areas in glioblastoma patients by using MR radiomics. Sci Rep 10:9748. https://doi.org/10.1038/s41598-020-66691-6
Chang PD, Malone HR, Bowden SG et al (2017) A multiparametric model for mapping cellularity in glioblastoma using radiographically localized biopsies. Am J Neuroradiol 38:890–898. https://doi.org/10.3174/ajnr.a5112
Lasocki A, Gaillard F, Tacey M et al (2018) Morphologic patterns of noncontrast-enhancing tumor in glioblastoma correlate with IDH1 mutation status and patient survival. J Clin Neurosci 47:168–173. https://doi.org/10.1016/j.jocn.2017.09.007
Muccio CF, Tarantino A, Esposito G, Cerase A (2011) Differential diagnosis by unenhanced FLAIR T2-weighted magnetic resonance images between solitary high grade gliomas and cerebral metastases appearing as contrast-enhancing cortico-subcortical lesions. J Neuro-Oncol 103:713–717. https://doi.org/10.1007/s11060-010-0454-8
Kinoshita M, Uchikoshi M, Tateishi S et al (2021) Magnetic resonance relaxometry for tumor cell density imaging for glioma: an exploratory study via 11C-methionine PET and its validation via stereotactic tissue sampling. Cancers 13:4067. https://doi.org/10.3390/cancers13164067
Yamamoto S, Sanada T, Sakai M et al (2022) Prediction and visualization of non-enhancing tumor in glioblastoma via T1w/T2w-ratio map. Brain Sci 12:99. https://doi.org/10.3390/brainsci12010099
Hirata T, Kinoshita M, Tamari K et al (2018) 11C-methionine-18F-FDG dual-PET-tracer–based target delineation of malignant glioma: evaluation of its geometrical and clinical features for planning radiation therapy. J Neurosurg 131:676–686. https://doi.org/10.3171/2018.4.jns1859
Author information
Authors and Affiliations
Contributions
M.S., A.A., N.K., E.S., and K.N. acquired data. S.Y., Y.O., H.A., T.S., and M.K. analyzed the data. H.K. supervised the research project. M.K conceptualized the research. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamamoto, S., Okita, Y., Arita, H. et al. Qualitative MR features to identify non-enhancing tumors within glioblastoma’s T2-FLAIR hyperintense lesions. J Neurooncol 165, 251–259 (2023). https://doi.org/10.1007/s11060-023-04454-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04454-9