Abstract
Purpose
In this study we report our 30-year experience in stereotactic radiosurgery (SRS) treatment of lung squamous cell carcinoma (LUSC) brain metastases (BMs). It will serve to provide detailed longitudinal outcomes and predictors of efficacy in treating LUSC-BMs with SRS.
Method
We retrospectively reviewed 51 patients and 109 tumors treated with SRS at our center between 1993 and 2022. Patient demographics, PDL1 genotype, immunotherapy use and mortality cause were recorded. Radiological and clinical outcomes were followed at 1-3-month intervals post-SRS. Cox-regression analysis and Kaplan-Meier survival curves were performed in statistical analysis.
Results
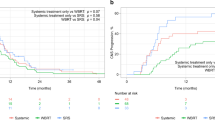
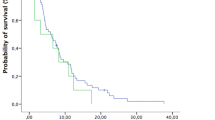
We included 37 male and 14 female patients (median age 62.7 years at BM diagnosis). Median overall survival (OS) time was 6.9 months, 6-month OS rate was 62.1%, and Karnofsky performance scale (KPS) was the only independent predictor. Median time for local control maintenance was 7.6 months, 6-month local control rate was 69.1%, with TKI as the only independent predictor. Median time to distant failure was 5.13 months, 6-month distant failure rate was 51.1%, and factors with significant impact included gender (p = 0.002), presence of extracranial metastases (p < 0.001), use of immunotherapy(p < 0.001), PDL1 genotype (p = 0.034), and total intracranial metastases number (p = 0.008). However, no definitive benefits of immunotherapy were identified in patients with higher PDL1 mutational tumors.
Conclusion
In this study we defined the natural history of disease progression and outcomes in SRS-treated LUSC-BM patients. We also identified predictors of OS and tumor control among these patients. The findings of this study will serve as a guide when counseling these patients for SRS.



Similar content being viewed by others
Data Availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- AC:
-
adenocarcinoma
- ARE:
-
adverse radiation effects
- BM:
-
brain metastasis
- KPS:
-
Karnofsky performance scale
- LUSC-BM:
-
lung squamous cell carcinoma with brain metastases
- OS:
-
overall survival
- QoL:
-
quality of life
- SRS:
-
stereotactic radiosurgery
- SqCC:
-
squamous cell carcinoma
- TKIs:
-
tyrosine kinase inhibitors
References
Graf AH, Buchberger W, Langmayr H, Schmid KW (1988) Site preference of metastatic tumours of the brain. Virchows Arch A Pathol Anat Histopathol 412(5):493–498. https://doi.org/10.1007/BF00750584
Ramotar M, Barnes S, Moraes F, Dasgupta A, Laperriere N, Millar BA, Berlin A, Conrad T, van Prooijen M, Damyanovich A, Heaton R, Cho YB, Coolens C, Liu G, Shepherd FA, Bradbury P, Leighl N, Bernstein M, Zadeh G, Kongkham P, Doherty M, Shultz DB (2019) Neurological Death is Common in Patients With EGFR Mutant Non-Small Cell Lung Cancer Diagnosed With Brain Metastases. Adv Radiat Oncol 5(3):350–357. https://doi.org/10.1016/j.adro.2019.11.002
Pérez-Larraya JG, Hildebrand J (2014) Handbook of Clinical Neurology (ed): Brain metastases. Elsevier, pp 1143–1157. https://doi.org/10.1016/B978-0-7020-4088-7.00077-8
Brown PD, Jaeckle K, Ballman KV, Farace E, Cerhan JH, Anderson SK, Carrero XW, Barker FG 2, Deming R, Burri SH, Ménard C, Chung C, Stieber VW, Pollock BE, Galanis E, Buckner JC, Asher AL (2016) Effect of Radiosurgery Alone vs Radiosurgery With Whole Brain Radiation Therapy on Cognitive Function in Patients With 1 to 3 Brain Metastases: A Randomized Clinical Trial. JAMA 316(4):401–409. https://doi.org/10.1001/jama.2016.9839
Soliman H, Das S, Larson DA, Sahgal A (2016) Stereotactic radiosurgery (SRS) in the modern management of patients with brain metastases. Oncotarget 7(11):12318–12330. https://doi.org/10.18632/oncotarget.7131
Aoyama H, Shirato H, Tago M, Nakagawa K, Toyoda T, Hatano K, Kenjyo M, Oya N, Hirota S, Shioura H, Kunieda E, Inomata T, Hayakawa K, Katoh N, Kobashi G (2006) Stereotactic radiosurgery plus whole-brain radiation therapy vs stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA 295(21):2483–2491. https://doi.org/10.1001/jama.295.21.2483
Singh R, Lehrer EJ, Ko S, Peterson J, Lou Y, Porter AB, Kotecha R, Brown PD, Zaorsky NG, Trifiletti DM (2020) Brain metastases from non-small cell lung cancer with EGFR or ALK mutations: A systematic review and meta-analysis of multidisciplinary approaches. Radiother Oncol 144:165–179. https://doi.org/10.1016/j.radonc.2019.11.010
Shaw AT, Ou SH, Bang YJ, Camidge DR, Solomon BJ, Salgia R, Riely GJ, Varella-Garcia M, Shapiro GI, Costa DB, Doebele RC, Le LP, Zheng Z, Tan W, Stephenson P, Shreeve SM, Tye LM, Christensen JG, Wilner KD, Clark JW, Iafrate AJ (2014) Crizotinib in ROS1-Rearranged Non-Small-Cell Lung Cancer. N Engl J Med 371:1963–1971. https://doi.org/10.1056/NEJMoa1406766
Chiou G, Chiang C, Yang H, Shen C, Wu H, Chen YW, Chen CJ, Luo YH, Hu YS, Lin CJ, Chung WY, Shiau CY, Guo WY, Pan DH, Lee CC (2022) Combined stereotactic radiosurgery and tyrosine kinase inhibitor therapy versus tyrosine kinase inhibitor therapy alone for the treatment of non–small cell lung cancer patients with brain metastases. J Neurosurg 137(2):563–570. https://doi.org/10.3171/2021.9.JNS211373
Jiang T, Su C, Li X, Zhao C, Zhou F, Ren S, Zhou C, Zhang J (2016) EGFR TKIs plus WBRT Demonstrated No Survival Benefit Other Than That of TKIs Alone in Patients with NSCLC and EGFR Mutation and Brain Metastases. J Thorac Oncol 11(10):1718–1728. https://doi.org/10.1016/j.jtho.2016.05.013
Langer CJ, Besse B, Gualberto A, Brambilla E, Soria JC (2010) The evolving role of histology in the management of advanced non-small-cell lung cancer. J Clin Oncol 28(36):5311–5320. https://doi.org/10.1200/JCO.2010.28.8126
Kuremsky JG, Urbanic JJ, Petty WJ, Lovato JF, Bourland JD, Tatter SB, Ellis TL, McMullen KP, Shaw EG, Chan MD (2013) Tumor histology predicts patterns of failure and survival in patients with brain metastases from lung cancer treated with gamma knife radiosurgery. Neurosurgery 73(4):641–647 discussion 647. https://doi.org/10.1227/NEU.0000000000000072
Ellis PM, Vella ET, Ung YC (2017) Immune Checkpoint Inhibitors for Patients With Advanced Non–Small-Cell Lung Cancer: A Systematic Review. Clin Lung Cancer 18(5):444–459. https://doi.org/10.1016/j.cllc.2017.02.001
Enright TL, Witt JS, Burr AR, Yadav P, Leal T, Baschnagel AM (2021) Combined Immunotherapy and Stereotactic Radiotherapy Improves Neurologic Outcomes in Patients with Non–small-cell Lung Cancer Brain Metastases. Clin Lung Cancer 22(2):110–119. https://doi.org/10.1016/j.cllc.2020.10.014
Brahmer J, Reckamp KL, Baas P, Crinò L, Eberhardt WE, Poddubskaya E, Antonia S, Pluzanski A, Vokes EE, Holgado E, Waterhouse D, Ready N, Gainor J, Arén Frontera O, Havel L, Steins M, Garassino MC, Aerts JG, Domine M, Paz-Ares L, Reck M, Baudelet C, Harbison CT, Lestini B, Spigel DR (2015) Nivolumab versus Docetaxel in Advanced Squamous-Cell Non-Small-Cell Lung Cancer. N Engl J Med 373(2):123–135. https://doi.org/10.1056/NEJMoa1504627
Carbone DP, Reck M, Paz-Ares L, Creelan B, Horn L, Steins M, Felip E, van den Heuvel MM, Ciuleanu TE, Badin F, Ready N, Hiltermann TJN, Nair S, Juergens R, Peters S, Minenza E, Wrangle JM, Rodriguez-Abreu D, Borghaei H, Blumenschein GR Jr, Villaruz LC, Havel L, Krejci J, Corral Jaime J, Chang H, Geese WJ, Bhagavatheeswaran P, Chen AC, Socinski MA, CheckMate 026 Investigators (2017) First-line nivolumab in stage IV or recurrent non-small-cell lung cancer. N Engl J Med 376:2415–2426. https://doi.org/10.1056/NEJMoa1613493
Govindan R, Szczesna A, Ahn MJ, Schneider CP, Gonzalez Mella PF, Barlesi F, Han B, Ganea DE, Von Pawel J, Vladimirov V, Fadeeva N, Lee KH, Kurata T, Zhang L, Tamura T, Postmus PE, Jassem J, O’Byrne K, Kopit J, Li M, Tschaika M, Reck M (2017) Phase III Trial of Ipilimumab Combined With Paclitaxel and Carboplatin in Advanced Squamous Non-Small-Cell Lung Cancer. J Clin Oncol 35(30):3449–3457. https://doi.org/10.1200/JCO.2016.71.7629
Herbst RS, Baas P, Kim DW, Felip E, Pérez-Gracia JL, Han JY, Molina J, Kim JH, Arvis CD, Ahn MJ, Majem M, Fidler MJ, de Castro G Jr, Garrido M, Lubiniecki GM, Shentu Y, Im E, Dolled-Filhart M, Garon EB (2016) Pembrolizumab versus docetaxel for previously treated, PD-L1-positive, advanced non-small-cell lung cancer (KEYNOTE-010): a randomised controlled trial. The Lancet 387:1540–1550. https://doi.org/10.1016/S0140-6736(15)01281-7
Referenced with permission from the NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®) for Guideline Non-Small Cell Lung Cancer V.3 (2022) © National Comprehensive Cancer Network, Inc. 2022. All rights reserved. Accessed [Aug 10, 2022]. To view the most recent and complete version of the guideline, go online to NCCN.org
Lee CC, Chou CL, Chen CJ, Yang HC, Wu HM, Shiau CY, Pan DH, Chung WY (2018) Stereotactic radiosurgery for hypervascular intracranial tumors. J Neurooncol 140:547–558. https://doi.org/10.1007/s11060-018-2980-8
Lee CC, Pan DH, Chung WY, Liu KD, Yang HC, Wu HM, Guo WY, Shih YH (2012) Brainstem cavernous malformations: the role of Gamma Knife surgery. J Neurosurg 117(Suppl):164–169. https://doi.org/10.3171/2012.8.GKS121066
Lee CC, Wintermark M, Xu Z, Yen CP, Schlesinger D, Sheehan JP (2014) Application of diffusion-weighted magnetic resonance imaging to predict the intracranial metastatic tu- mor response to gamma knife radiosurgery. J Neurooncol 118:351–361. https://doi.org/10.1007/s11060-014-1439-9
Lee CC, Yen CP, Xu Z, Schlesinger D, Sheehan J (2014) Large intracranial metastatic tumors treated by Gamma Knife surgery: outcomes and prognostic factors. J Neurosurg 120:52–59. https://doi.org/10.3171/2013.9.JNS131163
Andrews DW, Scott CB, Sperduto PW, Flanders AE, Gaspar LE, Schell MC, Werner-Wasik M, Demas W, Ryu J, Bahary JP, Souhami L, Rotman M, Mehta MP, Curran WJ Jr (2004) Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet 363:1665–1672. https://doi.org/10.1016/S0140-6736(04)16250-8
Shaw E, Scott C, Souhami L, Dinapoli R, Kline R, Loeffler J, Farnan N (2000) Single dose radiosurgical treatment of recurrent previously irradiated primary brain tumors and brain metastases: final report of RTOG protocol 90 – 05. Int J Radiat Oncol Biol Phys 47(2):291–298. https://doi.org/10.1016/s0360-3016(99)00507-6
Farris M, McTyre ER, Cramer CK, Hughes R, Randolph DM 2nd, Ayala-Peacock DN, Bourland JD, Ruiz J, Watabe K, Laxton AW, Tatter SB, Zhou X, Chan MD (2017) Brain Metastasis Velocity: A Novel Prognostic Metric Predictive of Overall Survival and Freedom From Whole-Brain Radiation Therapy After Distant Brain Failure Following Upfront Radiosurgery Alone. Int J Radiat Oncol Biol Phys 98(1):131–141. https://doi.org/10.1016/j.ijrobp.2017.01.201
Singh C, Qian JM, Yu JB, Chiang VL (2019) Local tumor response and survival outcomes after combined stereotactic radiosurgery and immunotherapy in non–small cell lung cancer with brain metastases. J Neurosurg JNS 132(2):512–517. https://doi.org/10.3171/2018.10.JNS181371
Breindel JL, Haskins JW, Cowell EP, Zhao M, Nguyen DX, Stern DF (2013) EGF receptor activates MET through MAPK to enhance non-small cell lung carcinoma invasion and brain metastasis. Cancer Res 73(16):5053–5065. https://doi.org/10.1158/0008-5472.CAN-12-3775
Shi AA, Digumarthy SR, Temel JS, Halpern EF, Kuester LB, Aquino SL (2006) Does initial staging or tumor histology better identify asymptomatic brain metastases in patients with non-small cell lung cancer? J Thorac Oncol 1(3):205–210. https://doi.org/10.1016/s1556-0864(15)31569-0
Mujoomdar A, Austin J, Malhotra R, Powell C, Pearson G, Shiau M, Raftopoulos H (2007) Clinical predictors of metastatic disease to the brain from non-small cell lung carcinoma: primary tumor size, cell type, and lymph node metastases. Radiology 242 3:882–888. https://doi.org/10.1148/RADIOL.2423051707
Guo S, Reddy CA, Chao ST, Suh JH, Barnett GH, Vogelbaum MA, Videtic GM (2012) Impact of non-small cell lung cancer histology on survival predicted from the graded prognostic assessment for patients with brain metastases. Lung Cancer 77(2):389–393. https://doi.org/10.1016/j.lungcan.2012.03.028
Janssen-Heijnen MLG, Schipper RM, Razenberg PPA, Crommelin MA, Coebergh JWW (1998) Prevalence of co-morbidity in lung cancer patients and its relationship with treatment: A population-based study. Lung Cancer 21(2):105–113. https://doi.org/10.1016/s0169-5002(98)00039-7
Chiang CL, Tsai CM, Chou TY, Chen YM, Lai SL, Shih JF, Chiu CH, Lee YC (2013) Erlotinib in patients with advanced lung squamous cell carcinoma. Cancer Chemother Pharmacol 71:203–208. https://doi.org/10.1007/s00280-012-1997-5
Tseng JS, Yang TY, Chen KC, Hsu KH, Chen HY, Chang GC (2012) Retrospective study of erlotinib in patients with advanced squamous lung cancer. Lung Cancer 77(1):128–133. https://doi.org/10.1016/j.lungcan.2012.02.012
Hata A, Katakami N, Kunimasa K, Yoshioka H, Fujita S, Kaji R, Tachikawa R, Tomii K, Imai Y, Iwasaku M, Ishida T (2011) Erlotinib for Pretreated Squamous Cell Carcinoma of the Lung in Japanese Patients. Jpn J Clin Oncol 41(12):1366–1372. https://doi.org/10.1093/jjco/hyr159
Lanier CM, McTyre E, LeCompte M, Cramer CK, Hughes R, Watabe K, Lo HW, O’Neill S, Munley MT, Laxton AW, Tatter SB, Ruiz J, Chan MD (2018) The number of prior lines of systemic therapy as a prognostic factor for patients with brain metastases treated with stereotactic radiosurgery: Results of a large single institution retrospective analysis. Clin Neurol Neurosurg 165:24–28. https://doi.org/10.1016/j.clineuro.2017.12.021
Lee CC, Hsu SPC, Lin CJ, Wu HM, Chen YW, Luo YH, Chiang CL, Hu YS, Chung WY, Shiau CY, Guo WY, Hung-Chi Pan D, Yang HC (2019) Epidermal growth factor receptor mutations: association with favorable local tumor control following Gamma Knife radiosurgery in patients with non–small cell lung cancer and brain metastases. J Neurosurg JNS 133(2):313–320. https://doi.org/10.3171/2019.4.JNS19446
Garon EB, Hellmann MD, Rizvi NA, Carcereny E, Leighl NB, Ahn MJ, Eder JP, Balmanoukian AS, Aggarwal C, Horn L, Patnaik A, Gubens M, Ramalingam SS, Felip E, Goldman JW, Scalzo C, Jensen E, Kush DA, Hui R (2019) Five-Year Overall Survival for Patients With Advanced Non–Small-Cell Lung Cancer Treated With Pembrolizumab: Results From the Phase I KEYNOTE-001 Study. J Clin Oncol 37(28):2518–2527. https://doi.org/10.1200/JCO.19.00934
Rittmeyer A, Barlesi F, Waterkamp D, Park K, Ciardiello F, von Pawel J, Gadgeel SM, Hida T, Kowalski DM, Dols MC, Cortinovis DL, Leach J, Polikoff J, Barrios C, Kabbinavar F, Frontera OA, De Marinis F, Turna H, Lee JS, Ballinger M, Kowanetz M, He P, Chen DS, Sandler A, Gandara DR, OAK Study Group (2017) Atezolizumab versus docetaxel in patients with previously treated non-small-cell lung cancer (OAK): a phase 3, open-label, multicentre randomised controlled trial. Lancet 389(10066):255–265. https://doi.org/10.1016/S0140-6736(16)32517-X
Paz-Ares L, Luft A, Vicente D, Tafreshi A, Gümüş M, Mazières J, Hermes B, Çay Şenler F, Csőszi T, Fülöp A, Rodríguez-Cid J, Wilson J, Sugawara S, Kato T, Lee KH, Cheng Y, Novello S, Halmos B, Li X, Lubiniecki GM, Piperdi B, Kowalski DM, KEYNOTE-407 Investigators (2018) Pembrolizumab plus Chemotherapy for Squamous Non-Small-Cell Lung Cancer. N Engl J Med 379(21):2040–2051. https://doi.org/10.1056/NEJMoa1810865
Gettinger SN, Redman MW, Bazhenova L, Hirsch FR, Mack PC, Schwartz LH, Bradley JD, Stinchcombe TE, Leighl NB, Ramalingam SS, Tavernier SS, Yu H, Unger JM, Minichiello K, Highleyman L, Papadimitrakopoulou VA, Kelly K, Gandara DR, Herbst RS (2021) Nivolumab Plus Ipilimumab vs Nivolumab for Previously Treated Patients With Stage IV Squamous Cell Lung Cancer: The Lung-MAP S1400I Phase 3 Randomized Clinical Trial. JAMA Oncol 7(9):1368–1377. https://doi.org/10.1001/jamaoncol.2021.2209
Yang M, Lin C, Wang Y, Chen K, Zhang H, Li W (2022) Identification of a cytokine-dominated immunosuppressive class in squamous cell lung carcinoma with implications for immunotherapy resistance. Genome Med 14(1):72. https://doi.org/10.1186/s13073-022-01079-x
Pan F, Cui S, Wang W, Gu A, Jiang L (2018) Survival analysis for lung adenosquamous carcinoma patients with brain metastasis. J Cancer 9(20):3707–3712. https://doi.org/10.7150/jca.27441
Maeda H, Matsumura A, Kawabata T, Suito T, Kawashima O, Watanabe T, Okabayashi K, Kubota I, for the Japan National Hospital Organization Study Group for Lung Cancer (2012) Adenosquamous carcinoma of the lung: surgical results as compared with squamous cell and adenocarcinoma cases. Eur J Cardiothorac Surg 41(2):357–361. https://doi.org/10.1016/j.ejcts.2011.05.050
Funding
This work was financially supported by the Ministry of Science and Technology, Taiwan, under the project MOST 110-2314-B-075-038 -MY2 and MOST 111-2314-b-075-066.
Author information
Authors and Affiliations
Contributions
The first draft of this manuscript was written by Yu-Chi Chen and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Disclosure Statement
The authors have no relevant disclosures to make.
Conflict of Interest
None of the authors have any conflicts of interest to declare.
Ethics Approval
This study is restrospective in nature and the patients’ data are analysed anonymously, therefore the Institutional Review Board states that no ethics approval is required.
Consent to Participate
Written informed consent to participate was provided by all patients.
Consent to Publish
Written informed consent to publish was provided by all patients.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, YC., Yang, HC., Chiang, CL. et al. Natural history of lung squamous cell brain metastases in patients treated with radiosurgery: a thirty-year experience at a tertiary medical center. J Neurooncol 161, 135–146 (2023). https://doi.org/10.1007/s11060-022-04153-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-022-04153-x