Abstract
Introduction
The optimal treatment paradigm for brain metastasis that recurs locally after initial radiosurgery remains an area of active investigation. Here, we report outcomes for patients with BMRS treated with stereotactic laser ablation (SLA, also known as laser interstitial thermal therapy, LITT) followed by consolidation radiosurgery.
Methods
Clinical outcomes of 20 patients with 21 histologically confirmed BMRS treated with SLA followed by consolidation SRS and > 6 months follow-up were collected retrospectively across three participating institutions.
Results
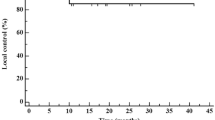
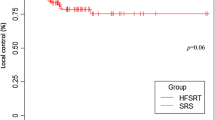
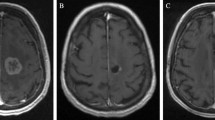
Consolidation SRS (5 Gy × 5 or 6 Gy × 5) was carried out 16–73 days (median of 26 days) post-SLA in patients with BMRS. There were no new neurological deficits after SLA/cSRS. While 3/21 (14.3%) patients suffered temporary Karnofsky Performance Score (KPS) decline after SLA, no KPS decline was observed after cSRS. There were no 30-day mortalities or wound complications. Two patients required re-admission within 30 days of cSRS (severe headache that resolved with steroid therapy (n = 1) and new onset seizure (n = 1)). With a median follow-up of 228 days (range: 178–1367 days), the local control rate at 6 and 12 months (LC6, LC12) was 100%. All showed diminished FLAIR volume surrounding the SLA/cSRS treated BMRS at the six-month follow-up; none of the patients required steroid for symptoms attributable to these BMRS. These results compare favorably to the available literature for repeat SRS or SLA-only treatment of BMRS.
Conclusions
This multi-institutional experience supports further investigations of SLA/cSRS as a treatment strategy for BMRS.




Similar content being viewed by others
Data availability
Data will be made available upon request as deemed appropriate by the corresponding author.
Code availability
Not applicable.
References
Roberge D, Brown PD, Whitton A et al (2018) The future is now-prospective study of radiosurgery for more than 4 brain metastases to start in 2018! Front Oncol 8:380
Douglas JG, Margolin K (2002) The treatment of brain metastases from malignant melanoma. Semin Oncol 29:518–524
Christ SM, Mahadevan A, Floyd SR et al (2015) Stereotactic radiosurgery for brain metastases from malignant melanoma. Surg Neurol Int 6:S355–S365
Kao WH, Riker AI, Kushwaha DS et al (2011) Upregulation of Fanconi anemia DNA repair genes in melanoma compared with non-melanoma skin cancer. J Invest Dermatol 131:2139–2142
Zohrabian VM, Nandu H, Gulati N et al (2007) Gene expression profiling of metastatic brain cancer. Oncol Rep 18:321–328
Lamb R, Fiorillo M, Chadwick A et al (2015) Doxycycline down-regulates DNA-PK and radiosensitizes tumor initiating cells: Implications for more effective radiation therapy. Oncotarget 6:14005–14025
Koffer P, Chan J, Rava P et al (2017) Repeat stereotactic radiosurgery for locally recurrent brain metastases. World Neurosurg 104:589–593
Iorio-Morin C, Mercure-Cyr R, Figueiredo G et al (2019) Repeat stereotactic radiosurgery for the management of locally recurrent brain metastases. J Neurooncol 145:551–559
Koiso T, Yamamoto M, Kawabe T et al (2016) Follow-up results of brain metastasis patients undergoing repeat Gamma Knife radiosurgery. J Neurosurg 125:2–10
Minniti G, Scaringi C, Paolini S et al (2016) Repeated stereotactic radiosurgery for patients with progressive brain metastases. J Neurooncol 126:91–97
Franzini A, Moosa S, Servello D et al (2019) Ablative brain surgery: an overview. Int J Hyperthermia 36:64–80
Carpentier A, McNichols RJ, Stafford RJ et al (2011) Laser thermal therapy: real-time MRI-guided and computer-controlled procedures for metastatic brain tumors. Lasers Surg Med 43:943–950
Ali MA, Carroll KT, Rennert RC et al (2016) Stereotactic laser ablation as treatment for brain metastases that recur after stereotactic radiosurgery: a multiinstitutional experience. Neurosurg Focus 41:E11
Ahluwalia M, Barnett GH, Deng D et al (2018) Laser ablation after stereotactic radiosurgery: a multicenter prospective study in patients with metastatic brain tumors and radiation necrosis. J Neurosurg 130:804–811
Bastos DC de A, Rao G, Oliva ICG et al (2020) Predictors of local control of brain metastasis treated with laser interstitial thermal therapy. Neurosurgery 87:112–122
Rezaie P, Khoei S, Khoee S et al (2018) Evaluation of combined effect of hyperthermia and ionizing radiation on cytotoxic damages induced by IUdR-loaded PCL-PEG-coated magnetic nanoparticles in spheroid culture of U87MG glioblastoma cell line. Int J Radiat Biol 94:1027–1037
Overgaard J (1989) The current and potential role of hyperthermia in radiotherapy. Int J Radiat Oncol Biol Phys 16:535–549
Dewey WC (2009) Arrhenius relationships from the molecule and cell to the clinic. Int J Hyperthermia 25:3–20
Datta NR, Ordóñez SG, Gaipl US et al (2015) Local hyperthermia combined with radiotherapy and-/or chemotherapy: recent advances and promises for the future. Cancer Treat Rev 41:742–753
Grauer O, Jaber M, Hess K et al (2019) Combined intracavitary thermotherapy with iron oxide nanoparticles and radiotherapy as local treatment modality in recurrent glioblastoma patients. J Neurooncol 141:83–94
Hong CS, Beckta JM, Kundishora AJ et al (2020) Laser interstitial thermal therapy for treatment of cerebral radiation necrosis. Int J Hyperthermia 37:68–76
Chen C, Lee I, Tatsui C et al (2021) Laser interstitial thermotherapy (LITT) for the treatment of tumors of the brain and spine: a brief review. J Neurooncol 151:429–442
Munier S, Ginalis EE, Patel NV, et al (2020) Radiation Necrosis in Intracranial Lesions. Cureus 12:e7603
Lin NU, Lee EQ, Aoyama H et al (2015) Response assessment criteria for brain metastases: proposal from the RANO group. Lancet Oncol 16:e270–e278
Beechar VB, Prabhu SS, Bastos D et al (2018) Volumetric response of progressing post-SRS lesions treated with laser interstitial thermal therapy. J Neurooncol 137:57–65
Wen PY, Chang SM, Van den Bent MJ et al (2017) Response assessment in neuro-oncology clinical trials. J Clin Oncol 35:2439–2449
Sloan AE, Ahluwalia MS, Valerio-Pascua J et al (2013) Results of the NeuroBlate System first-in-humans Phase I clinical trial for recurrent glioblastoma: clinical article. J Neurosurg 118:1202–1219
Loi M, Caini S, Scoccianti S, et al (2020) Stereotactic reirradiation for local failure of brain metastases following previous radiosurgery: Systematic review and meta-analysis. Crit Rev Oncol Hematol 153:103043
Kim AH, Tatter S, Rao G et al (2020) Laser Ablation of Abnormal Neurological Tissue Using Robotic NeuroBlate System (LAANTERN): 12-Month Outcomes and Quality of Life After Brain Tumor Ablation. Neurosurgery 87:E338–E346
Holt DE, Gill BS, Clump DA et al (2015) Tumor bed radiosurgery following resection and prior stereotactic radiosurgery for locally persistent brain metastasis. Front Oncol 5:84
Rana N, Pendyala P, Cleary RK et al (2017) Long-term Outcomes after Salvage Stereotactic Radiosurgery (SRS) following In-Field Failure of Initial SRS for Brain Metastases. Front Oncol 7:279
Dincoglan F, Sager O, Demiral S et al (2019) Fractionated stereotactic radiosurgery for locally recurrent brain metastases after failed stereotactic radiosurgery. Indian J Cancer 56:151–156
Terakedis BE, Jensen RL, Boucher K, Shrieve DC (2014) Tumor control and incidence of radiation necrosis after reirradiation with stereotactic radiosurgery for brain metastases. J Radiosurg SBRT 3(1):21–28
Bates JE, Usuki YP, KY, et al (2016) Repeat courses of SRS in patients initially treated with SRS alone for brain-metastasis melanoma. Melanoma Manag 3(2):97–104
McKay WH, McTyre ER, Okoukoni C et al (2017) Repeat stereotactic radiosurgery as salvage therapy for locally recurrent brain metastases previously treated with radiosurgery. J Neurosurg 127(1):148–156
Moreau J, Khalil T, Dupic G, et al (2018) Second course of stereotactic radiosurgery for locally recurrent brain metastases: Safety and efficacy. PLoS One 13(4): e0195608
Balermpas P, Stera S, Muller von der Grun J, et al (2018) Repeated in-field radiosurgery for locally recurrent brain metastases: Feasibility, results and survival in a heavily treated patient cohort. PLoS One 13(6): e0198692
Jiang X, Wang H, Song Y et al (2019) A second course of stereotactic image-guided robotic radiosurgery for patients with cerebral metastasis. World Neurosurg 123:e6121–e6628
Jablonska PA, Serrano Tejero D, Calvo Gonzalez A, et al (2020) Repeated stereotactic radiosurgery for recurrent brain metastases: An effective strategy to control intracranial oligometastatic disease. Crit Rev Oncol Hematol 153: 103028
Niranjan A, Monaco E, Flickinger J, Lunsford LD (2019) Guidelines for Multiple Brain Metastases Radiosurgery. Prog Neurol Surg 34:100–109
Achrol AS, Rennert RC, Anders C et al (2019) Brain metastases. Nat Rev Dis Primers 5:5
Alattar AA, Bartek J Jr, Chiang VL et al (2019) Stereotactic laser ablation as treatment of brain metastases recurring after stereotactic radiosurgery: a systematic literature review. World Neurosurg 128:134–142
Verma N, Cowperthwaite MC, Burnett MG, Markey MK (2013) Differentiating tumor recurrence from treatment necrosis: a review of neuro-oncologic imaging strategies. Neuro Oncol 15:515–534
Alomari A, Rauch PJ, Orsaria M et al (2014) Radiologic and histologic consequences of radiosurgery for brain tumors. J Neurooncol 117:33–42
Dixit KS, Kumthekar PU (2020) Optimal management of corticosteroids in patients with intracranial malignancies. Curr Treat Options Oncol 21:77
Ramakrishna R, Formenti S (2019) Radiosurgery and Immunotherapy in the Treatment of Brain Metastases. World Neurosurg 130:615–622
Kroeze SGC, Fritz C, Hoyer M et al (2017) Toxicity of concurrent stereotactic radiotherapy and targeted therapy or immunotherapy: a systematic review. Cancer Treat Rev 53:25–37
Schwabe B, Kahn T, Harth T et al (1997) Laser-induced thermal lesions in the human brain: short- and long-term appearance on MRI. J Comput Assist Tomogr 21:818–825
Camidge DR, Lee EQ, Lin NU et al (2018) Clinical trial design for systemic agents in patients with brain metastases from solid tumours: a guideline by the Response Assessment in Neuro-Oncology Brain Metastases working group. Lancet Oncol 19:e20–e32
Funding
No funding was provided for this study.
Author information
Authors and Affiliations
Contributions
JM, YH, EF, KD, MR, CW, JY, ES, MG, PF, EDM, NF, GHB, VC and AM collected data. IPP drafted the manuscript. CCC conceived the study, performed procedures reported, drafted the manuscript. All authors edited the final draft of the manuscript and provided critical review.
Corresponding author
Ethics declarations
Conflict of interest
The authors do not have any conflicts of interest to report.
Ethical approval
This study was approved by the local IRB at each participating institution.
Consent to participate
Consent for data collection was waived as this was a retrospective study.
Consent for publication
Not applicable, no private health information is published in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Peña Pino, I., Ma, J., Hori, Y.S. et al. Stereotactic Laser Ablation (SLA) followed by consolidation stereotactic radiosurgery (cSRS) as treatment for brain metastasis that recurred locally after initial radiosurgery (BMRS): a multi-institutional experience. J Neurooncol 156, 295–306 (2022). https://doi.org/10.1007/s11060-021-03893-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-021-03893-6