Abstract
Purpose
Spinal ependymomas represent the most common primary intramedullary tumors for which optimal management remains undefined. When possible, gross total resection (GTR) is often the mainstay of treatment, with consideration of radiotherapy (RT) in cases of residual or recurrent tumor. The impact of extent of resection and radiotherapy remain understudied.
Objective
Report on a large institutional cohort with lengthy follow-up to provide information on long-term outcomes and to contribute to limited data assessing the value of extent of resection and RT.
Methods
Patients with pathologically proven primary spinal ependymoma between 1990 and 2018 were identified. Kaplan-Meier estimates were used to calculate progression-free survival (PFS); local-control (LC) and overall survival (OS). Logistic regression was used to analyze variables’ association with receipt of RT.
Results
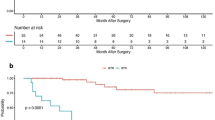
We identified 69 patients with ependymoma of which 4 had leptomeningeal dissemination at diagnosis and were excluded. Of the remaining cohort (n = 65), 42 patients (65%) had Grade II spinal ependymoma, 20 (31%) had Grade I myxopapillary ependymoma and 3 (5%) had Grade III anaplastic ependymoma; 54% underwent GTR and 39% underwent RT. With a median follow-up of 5.7 years, GTR was associated with improved PFS. For grade II lesions, STR+RT yielded better outcomes than STR alone (10y PFS 77.1% vs 68.2%, LC 85.7% vs 50%). Degree of resection was the only significant predictor of adjuvant radiotherapy (p < 0.0001).
Conclusion
Our findings confirm the importance of GTR in spinal ependymomas. Adjuvant RT should be utilized in the setting of a subtotal resection with expectation of improved disease-related outcomes.





Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Ryu SM, Lee SH, Kim ES, Eoh W (2018) Predicting survival of patients with spinal ependymoma using machine learning algorithms with the SEER database. World Neurosurg. https://doi.org/10.1016/j.wneu.2018.12.091
Lee SH, Chung CK, Kim CH, Yoon SH, Hyun SJ, Kim KJ, Kim ES, Eoh W, Kim HJ (2013) Long-term outcomes of surgical resection with or without adjuvant radiation therapy for treatment of spinal ependymoma: a retrospective multicenter study by the Korea Spinal Oncology Research Group. Neuro Oncol 15(7):921–929. https://doi.org/10.1093/neuonc/not038
Neumann JE, Spohn M, Obrecht D, Mynarek M, Thomas C, Hasselblatt M, Dorostkar MM, Wefers AK, Frank S, Monoranu CM, Koch A, Witt H, Kool M, Pajtler KW, Rutkowski S, Glatzel M, Schuller U (2020) Molecular characterization of histopathological ependymoma variants. Acta Neuropathol 139(2):305–318. https://doi.org/10.1007/s00401-019-02090-0
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P, Ellison DW (2016) The 2016 world health organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131(6):803–820. https://doi.org/10.1007/s00401-016-1545-1
Harrop JS, Ganju A, Groff M, Bilsky M. (2009). Primary intramedullary tumors of the spinal cord. Spine (Phila Pa 1976) 34 (22 Suppl):S69-77. doi:https://doi.org/10.1097/BRS.0b013e3181b95c6f
Samuel N, Tetreault L, Santaguida C, Nater A, Moayeri N, Massicotte EM, Fehlings MG (2016) Clinical and pathological outcomes after resection of intramedullary spinal cord tumors: a single-institution case series. Neurosurg Focus 41(2):E8. https://doi.org/10.3171/2016.5.FOCUS16147
Ruda R, Reifenberger G, Frappaz D, Pfister SM, Laprie A, Santarius T, Roth P, Tonn JC, Soffietti R, Weller M, Moyal EC (2018) EANO guidelines for the diagnosis and treatment of ependymal tumors. Neuro Oncol 20(4):445–456. https://doi.org/10.1093/neuonc/nox166
Wostrack M, Ringel F, Eicker SO, Jagersberg M, Schaller K, Kerschbaumer J, Thome C, Shiban E, Stoffel M, Friedrich B, Kehl V, Vajkoczy P, Meyer B, Onken J (2018) Spinal ependymoma in adults: a multicenter investigation of surgical outcome and progression-free survival. J Neurosurg Spine 28(6):654–662. https://doi.org/10.3171/2017.9.SPINE17494
Byun HK, Yi S, Yoon HI, Kim SH, Cho J, Suh CO (2018) Clinical outcomes of radiotherapy for spinal cord ependymoma with adverse prognostic features: a single-center study. J Neurooncol 140(3):649–657. https://doi.org/10.1007/s11060-018-2995-1
Wahab SH, Simpson JR, Michalski JM, Mansur DB (2007) Long term outcome with post-operative radiation therapy for spinal canal ependymoma. J Neurooncol 83(1):85–89. https://doi.org/10.1007/s11060-006-9310-2
Kobayashi K, Ando K, Kato F, Kanemura T, Sato K, Kamiya M, Nishida Y, Ishiguro N, Imagama S (2018) Surgical outcomes of spinal cord and cauda equina ependymoma: postoperative motor status and recurrence for each WHO grade in a multicenter study. J Orthop Sci 23(4):614–621. https://doi.org/10.1016/j.jos.2018.03.004
Brown DA, Goyal A, Takami H, Graffeo CS, Mahajan A, Krauss WE, Bydon M (2020) Radiotherapy in addition to surgical resection may not improve overall survival in WHO grade II spinal ependymomas. Clin Neurol Neurosurg 189:105632. https://doi.org/10.1016/j.clineuro.2019.105632
Oh MC, Kim JM, Kaur G, Safaee M, Sun MZ, Singh A, Aranda D, Molinaro AM, Parsa AT (2013) Prognosis by tumor location in adults with spinal ependymomas. J Neurosurg Spine 18(3):226–235. https://doi.org/10.3171/2012.12.spine12591
Cachia D, Johnson DR, Kaufmann TJ, Lowe S, Andersen S, Olar A, Cooper SL, Frankel BM, Gilbert MR (2018) Case-based review: ependymomas in adults. Neurooncol Pract 5(3):142–153. https://doi.org/10.1093/nop/npy026
Klekamp J (2015) Spinal ependymomas Part 1: intramedullary ependymomas. Neurosurg Focus 39(2):6. https://doi.org/10.3171/2015.5.focus15161
Gilbert MR, Ruda R, Soffietti R (2010) Ependymomas in adults. Curr Neurol Neurosci Rep 10(3):240–247. https://doi.org/10.1007/s11910-010-0109-3
Weber DC, Wang Y, Miller R, Villa S, Zaucha R, Pica A, Poortmans P, Anacak Y, Ozygit G, Baumert B, Haller G, Preusser M, Li J (2015) Long-term outcome of patients with spinal myxopapillary ependymoma: treatment results from the MD Anderson Cancer Center and institutions from the Rare Cancer Network. Neuro Oncol 17(4):588–595. https://doi.org/10.1093/neuonc/nou293
Volpp PB, Han K, Kagan AR, Tome M (2007) Outcomes in treatment for intradural spinal cord ependymomas. Int J Radiat Oncol Biol Phys 69(4):1199–1204. https://doi.org/10.1016/j.ijrobp.2007.04.058
Chang UK, Choe WJ, Chung SK, Chung CK, Kim HJ (2002) Surgical outcome and prognostic factors of spinal intramedullary ependymomas in adults. J Neurooncol 57(2):133–139
Nakamura M, Ishii K, Watanabe K, Tsuji T, Takaishi H, Matsumoto M, Toyama Y, Chiba K (2008) Surgical treatment of intramedullary spinal cord tumors: prognosis and complications. Spinal Cord 46(4):282–286. https://doi.org/10.1038/sj.sc.3102130
Celano E, Salehani A, Malcolm JG, Reinertsen E, Hadjipanayis CG (2016) Spinal cord ependymoma: a review of the literature and case series of ten patients. J Neurooncol 128(3):377–386. https://doi.org/10.1007/s11060-016-2135-8
Figueiredo N, Brooks N, Resnick DK (2013) Evidence-based review and guidelines for the management of myxopapillary and intramedullary ependymoma. J Neurosurg Sci 57(4):327–341. https://doi.org/10.4172/2155-9562-C5-073
Oh MC, Ivan ME, Sun MZ, Kaur G, Safaee M, Kim JM, Sayegh ET, Aranda D, Parsa AT (2013) Adjuvant radiotherapy delays recurrence following subtotal resection of spinal cord ependymomas. Neuro Oncol 15(2):208–215. https://doi.org/10.1093/neuonc/nos286
Halvorsen CM, Kolstad F, Hald J, Johannesen TB, Krossnes BK, Langmoen IA, Lied B, Ronning P, Skaar S, Spetalen S, Helseth E. (2010). Long-term outcome after resection of intraspinal ependymomas: report of 86 consecutive cases. Neurosurgery 67 (6):1622-1631; discussion 1631. doi:https://doi.org/10.1227/NEU.0b013e3181f96d41
Kirkpatrick JP, van der Kogel AJ, Schultheiss TE (2010) Radiation dose-volume effects in the spinal cord. Int J Radiat Oncol Biol Phys 76(3 Suppl):S42-49. https://doi.org/10.1016/j.ijrobp.2009.04.095
Amsbaugh MJ, Grosshans DR, McAleer MF, Zhu R, Wages C, Crawford CN, Palmer M, De Gracia B, Woo S, Mahajan A (2012) Proton therapy for spinal ependymomas: planning, acute toxicities, and preliminary outcomes. Int J Radiat Oncol Biol Phys 83(5):1419–1424. https://doi.org/10.1016/j.ijrobp.2011.10.034
Clover LL, Hazuka MB, Kinzie JJ (1993) Spinal cord ependymomas treated with surgery and radiation therapy. A review of 11 cases. Am J Clin Oncol 16(4):350–353
Gomez DR, Missett BT, Wara WM, Lamborn KR, Prados MD, Chang S, Berger MS, Haas-Kogan DA (2005) High failure rate in spinal ependymomas with long-term follow-up. Neuro Oncol 7(3):254–259. https://doi.org/10.1215/S1152851704001231
Tsai CJ, Wang Y, Allen PK, Mahajan A, McCutcheon IE, Rao G, Rhines LD, Tatsui CE, Armstrong TS, Maor MH, Chang EL, Brown PD, Li J. (2014). Outcomes after surgery and radiotherapy for spinal myxopapillary ependymoma: update of the MD Anderson Cancer Center experience. Neurosurgery 75 (3):205-214; discussion 213-204. doi:https://doi.org/10.1227/NEU.0000000000000408
Rezai AR, Woo HH, Lee M, Cohen H, Zagzag D, Epstein FJ (1996) Disseminated ependymomas of the central nervous system. J Neurosurg 85(4):618–624. https://doi.org/10.3171/jns.1996.85.4.0618
Oh MC, Tarapore PE, Kim JM, Sun MZ, Safaee M, Kaur G, Aranda DM, Parsa AT (2013) Spinal ependymomas: benefits of extent of resection for different histological grades. J Clin Neurosci 20(10):1390–1397. https://doi.org/10.1016/j.jocn.2012.12.010
Bostrom A, von Lehe M, Hartmann W, Pietsch T, Feuss M, Bostrom JP, Schramm J, Simon M. (2011). Surgery for spinal cord ependymomas: outcome and prognostic factors. Neurosurgery 68(2):302-308, discussion 309. doi:https://doi.org/10.1227/NEU.0b013e3182004c1e
Abdel-Wahab M, Etuk B, Palermo J, Shirato H, Kresl J, Yapicier O, Walker G, Scheithauer BW, Shaw E, Lee C, Curran W, Thomas T, Markoe A (2006) Spinal cord gliomas: a multi-institutional retrospective analysis. Int J Radiat Oncol Biol Phys 64(4):1060–1071. https://doi.org/10.1016/j.ijrobp.2005.09.038
Nagasawa DT, Smith ZA, Cremer N, Fong C, Lu DC, Yang I (2011) Complications associated with the treatment for spinal ependymomas. Neurosurg Focus 31(4):E13. https://doi.org/10.3171/2011.7.focus11158
Lin Y, Smith ZA, Wong AP, Melkonian S, Harris DA, Lam S (2015) Predictors of survival in patients with spinal ependymoma. Neurol Res 37(7):650–655. https://doi.org/10.1179/1743132815Y.0000000041
McCormick PC, Torres R, Post KD, Stein BM (1990) Intramedullary ependymoma of the spinal cord. J Neurosurg 72(4):523–532. https://doi.org/10.3171/jns.1990.72.4.0523
Funding
We have no funding sources to report.
Author information
Authors and Affiliations
Contributions
All authors participated in the writing and editing of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest.
Ethics approval
Northwestern University IRB: STU00209605.
Consent to participate
No consent needed due to retrospective nature of study and use of patient records.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Savoor, R., Sita, T.L., Dahdaleh, N.S. et al. Long-term outcomes of spinal ependymomas: an institutional experience of more than 60 cases. J Neurooncol 151, 241–247 (2021). https://doi.org/10.1007/s11060-020-03658-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03658-7