Abstract
Purpose
The purpose of this review is to assess the recent evidence regarding the management of squamous cell carcinoma of the skull-base and to discuss the implications of these findings on clinical practice.
Method
Free text Medline and MeSH term search of publications relating to Squamous Cell Carcinoma & Skull-base and Skull base, Neoplasm respectively. Multidisciplinary clinical guidelines were also reviewed.
Results
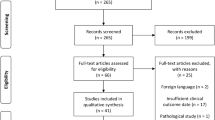
The primary search yielded a total of 271 papers which following initial review was reduced to 28. Secondary search yielded 56 papers. There were no randomised controlled trials relating to squamous cell carcinoma of the skull-base and as such this review is based on cohort studies, case series and expert opinion.
Conclusion
Squamous cell carcinoma (SCC) is the most common cancer occurring in the Head and Neck. Squamous cell carcinoma is also the most common cancer arising within the nose and sinuses of which skull-base squamous cell carcinoma is a rare subgroup.
Evidence relating to the management and survival of skull-base SCC is based on expert opinion and. retrospective analyses Clinical examination and biopsy, imaging and a broad multidisciplinary team are key to the management of skull-base SCC. The information gathered should be used to guide informed discussion by suitably trained experts with patients regarding surgical approach, post-operative recovery and adjuvant or neoadjuvant treatments. The standard of care is currently to perform skull base resection with or without additional craniotomy, pedicled or free flap reconstruction in multiple layers and post-operative radiation (usually photons or protons). Open approaches have traditionally been the mainstay, however in certain cases endoscopic approaches can yield equivalent results and offer many advantages. Despite advances in care survival remains poor with a nearly one in five risk of nodal recurrence within two years.
Similar content being viewed by others
References
Lund VJ, Stammberger H, Nicolai P et al (2010) European position paper on endoscopic management of tumours of the nose, paranasal sinuses and skull base. Rhinol Suppl 22:1–143
von Buchwald C, Bradley PJ (2007) Risks of malignancy in inverted papilloma of the nose and paranasal sinuses. Curr Opin Otolaryngol Head Neck Surg 15(2):95–98. https://doi.org/10.1097/MOO.0b013e3280803d9b
Tanvetyanon T, Qin D, Padhya T, Kapoor R, McCaffrey J, Trotti A (2009) Survival outcomes of squamous cell carcinoma arising from sinonasal inverted papilloma: report of 6 cases with systematic review and pooled analysis. Am J Otolaryngol 30(1):38–43. https://doi.org/10.1016/j.amjoto.2008.02.005
Bhattacharyya N (2002) Cancer of the nasal cavity: survival and factors influencing prognosis. Arch Otolaryngol Head Neck Surg 128(9):1079–1083. https://doi.org/10.1001/archotol.128.9.1079
Feiz-Erfan I, Suki D, Hanna E, DeMonte F (2007) Prognostic significance of transdural invasion of cranial base malignancies in patients undergoing craniofacial resection. Neurosurgery 61(6):1178–1185. https://doi.org/10.1227/01.neu.0000306095.53388.f1
Wang EW, Gardner PA, Zanation AM (2019) International consensus statement on endoscopic skull-base surgery: executive summary. Int Forum Allergy Rhinol 9(S3):S127–S144. https://doi.org/10.1002/alr.22327
Gardner PA, Kassam AB, Rothfus WE, Snyderman CH, Carrau RL (2008) Preoperative and intraoperative imaging for endoscopic endonasal approaches to the skull base. Otolaryngol Clin North Am 41(1):215–230. https://doi.org/10.1016/j.otc.2007.10.010
Paleri V, Urbano TG, Mehanna H et al (2016) Management of neck metastases in head and neck cancer: United Kingdom National Multidisciplinary Guidelines. J Laryngol Otol 130(S2):S161–S169. https://doi.org/10.1017/S002221511600058X
Ganly I, Patel SG, Singh B et al (2011) Craniofacial resection for malignant tumors involving the skull base in the elderly: an international collaborative study. Cancer 117(3):563–571. https://doi.org/10.1002/cncr.25390
Liu JK, Decker D, Schaefer SD et al (2003) Zones of approach for craniofacial resection: minimizing facial incisions for resection of anterior cranial base and paranasal sinus tumors. Neurosurgery 53(5):1126–1135. https://doi.org/10.1227/01.neu.0000088802.58956.5a
Carrau RL, Snyderman CH, Kassam AB, Jungreis CA (2001) Endoscopic and endoscopic-assisted surgery for juvenile angiofibroma. Laryngoscope 111(3):483–487. https://doi.org/10.1097/00005537-200103000-00019
Wagenmann M, Schipper J (2011) The transnasal approach to the skull base From sinus surgery to skull base surgery. GMS Curr Top Otorhinolaryngol Head Neck Surg. https://doi.org/10.3205/cto000081
Rawal RB, Gore MR, Harvey RJ, Zanation AM (2012) Evidence-based practice: endoscopic skull base resection for malignancy. Otolaryngol Clin North Am 45(5):1127–1142. https://doi.org/10.1016/j.otc.2012.06.013
Wellman BJ, Traynelis VC, McCulloch TM, Funk GF, Menezes AH, Hoffman HT (1999) Midline anterior craniofacial approach for malignancy: results of en bloc versus piecemeal resections. Skull Base Surg 9(1):41–46. https://doi.org/10.1055/s-2008-1058171
Poetker DM, Mendolia-Loffredo S, Smith TL (2007) Outcomes of endoscopic sinus surgery for chronic rhinosinusitis associated with sinonasal polyposis. Am J Rhinol 21(1):84–88. https://doi.org/10.2500/ajr.2007.21.2978
Lund V, Howard DJ, Wei WI (2007) Endoscopic resection of malignant tumors of the nose and sinuses. Am J Rhinol 21(1):89–94. https://doi.org/10.2500/ajr.2007.21.2957
Abdelmeguid AS, Raza SM, Su SY et al (2019) Endoscopic resection of sinonasal malignancies. Head Neck. https://doi.org/10.1002/hed.26047
Wood JW, Eloy JA, Vivero RJ et al (2012) Efficacy of transnasal endoscopic resection for malignant anterior skull-base tumors. Int Forum Allergy Rhinol 2(6):487–495. https://doi.org/10.1002/alr.21062
Abergel A, Cavel O, Margalit N, Fliss DM, Gil Z (2012) Comparison of quality of life after transnasal endoscopic vs open skull base tumor resection. Arch Otolaryngol Head Neck Surg 138(2):142–147. https://doi.org/10.1001/archoto.2011.1146
Castelnuovo P, Lepera D, Turri-Zanoni M et al (2013) Quality of life following endoscopic endonasal resection of anterior skull base cancers. J Neurosurg 119(6):1401–1409. https://doi.org/10.3171/2013.8.JNS13296
Larjani S, Monteiro E, Witterick I et al (2016) Preliminary cross-sectional reliability and validity of the Skull Base Inventory (SBI) quality of life questionnaire. J Otolaryngol Head Neck Surg 45(1):45. https://doi.org/10.1186/s40463-016-0158-y
Hanna E, DeMonte F, Ibrahim S, Roberts D, Levine N, Kupferman M (2009) Endoscopic resection of sinonasal cancers with and without craniotomy: oncologic results. Arch Otolaryngol Head Neck Surg 135(12):1219–1224. https://doi.org/10.1001/archoto.2009.173
Castelnuovo P, Battaglia P, Turri-Zanoni M et al (2014) Endoscopic endonasal surgery for malignancies of the anterior cranial base. World Neurosurg 82(6 Suppl):S22–31. https://doi.org/10.1016/j.wneu.2014.07.021
Nicolai P, Battaglia P, Bignami M et al (2008) Endoscopic surgery for malignant tumors of the sinonasal tract and adjacent skull base: a 10-year experience. Am J Rhinol 22(3):308–316. https://doi.org/10.2500/ajr.2008.22.3170
Su SY, Kupferman ME, DeMonte F, Levine NB, Raza SM, Hanna EY (2014) Endoscopic resection of sinonasal cancers. Curr Oncol Rep 16(2):369. https://doi.org/10.1007/s11912-013-0369-6
Ziai H, Yu E, Fu T et al (2018) Impact of Dural Resection on Sinonasal Malignancies with Skull Base Encroachment or Erosion. Journal of neurological surgery. 79(5):419–426. https://doi.org/10.1055/s-0037-1612617
Hadad G, Bassagasteguy L, Carrau RL et al (2006) A novel reconstructive technique after endoscopic expanded endonasal approaches: vascular pedicle nasoseptal flap. Laryngoscope 116(10):1882–1886. https://doi.org/10.1097/01.mlg.0000234933.37779.e4
Price JC, Loury M, Carson B, Johns ME (1988) The pericranial flap for reconstruction of anterior skull base defects. Laryngoscope 98(11):1159–1164. https://doi.org/10.1288/00005537-198811000-00002
Johns ME, Winn HR, McLean WC, Cantrell RW (1981) Pericranial flap for the closure of defects of craniofacial resection. Laryngoscope 91(6):952–959. https://doi.org/10.1288/00005537-198106000-00013
Neligan PC, Mulholland S, Irish J et al (1996) Flap selection in cranial base reconstruction. Plast Reconstr Surg 98(7):1159–1166. https://doi.org/10.1097/00006534-199612000-00005
Germani RM, Vivero R, Herzallah IR, Casiano RR (2007) Endoscopic reconstruction of large anterior skull base defects using acellular dermal allograft. Am J Rhinol 21(5):615–618. https://doi.org/10.2500/ajr.2007.21.3080
Eloy JA, Shukla PA, Choudhry OJ, Singh R, Liu JK (2012) Assessment of frontal lobe sagging after endoscopic endonasal transcribriform resection of anterior skull base tumors: is rigid structural reconstruction of the cranial base defect necessary? Laryngoscope 122(12):2652–2657. https://doi.org/10.1002/lary.23539
Casiano RR, Numa WA, Falquez AM (2001) Endoscopic resection of esthesioneuroblastoma. Am J Rhinol 15(4):271–279
Zanation AM, Snyderman CH, Carrau RL, Kassam AB, Gardner PA, Prevedello DM (2009) Minimally invasive endoscopic pericranial flap: a new method for endonasal skull base reconstruction. Laryngoscope 119(1):13–18. https://doi.org/10.1002/lary.20022
Bresler AY, Mir G, Grube J et al (2019) Endoscopic Paramedian Forehead Flap Reconstruction of the Anterior Skull Base for Recalcitrant Cerebrospinal Fluid Leaks: Minimally Invasive Adaptation of Ancient Flap. World Neurosurg 130:37–41. https://doi.org/10.1016/j.wneu.2019.06.162
Tabano A, Restelli F, Pozzi F et al (2019) The Helmet-Visor Pericranial Flap as a Viable Option for Anterior Cranial Base Reconstruction in Complex Oncologic Cases. World Neurosurg 128:506–513. https://doi.org/10.1016/j.wneu.2019.05.136
Klatt-Cromwell CN, Thorp BD, Del Signore AG, Ebert CS, Ewend MG, Zanation AM (2016) Reconstruction of Skull Base Defects. Otolaryngol Clin North Am 49(1):107–117. https://doi.org/10.1016/j.otc.2015.09.006
de Almeida JR, Su SY, Koutourousiou M et al (2015) Endonasal endoscopic surgery for squamous cell carcinoma of the sinonasal cavities and skull base: Oncologic outcomes based on treatment strategy and tumor etiology. Head Neck 37(8):1163–1169. https://doi.org/10.1002/hed.23731
Lund VJ, Clarke PM, Swift AC, McGarry GW, Kerawala C, Carnell D (2016) Nose and paranasal sinus tumours: United Kingdom National Multidisciplinary Guidelines. J Laryngol Otol 130(S2):S111–S118. https://doi.org/10.1017/S0022215116000530
Scangas GA, Eloy JA, Lin DT (2017) The Role of Chemotherapy in the Management of Sinonasal and Ventral Skull Base Malignancies. Otolaryngol Clin North Am 50(2):433–441. https://doi.org/10.1016/j.otc.2016.12.015
Dirix P, Nuyts S, Geussens Y et al (2007) Malignancies of the nasal cavity and paranasal sinuses: long-term outcome with conventional or three-dimensional conformal radiotherapy. Int J Radiat Oncol Biol Phys 69(4):1042–1050. https://doi.org/10.1016/j.ijrobp.2007.04.044
Al-Mamgani A, Monserez D, Rooij P, Verduijn GM, Hardillo JA, Levendag PC (2012) Highly-conformal intensity-modulated radiotherapy reduced toxicity without jeopardizing outcome in patients with paranasal sinus cancer treated by surgery and radiotherapy or (chemo)radiation. Oral Oncol 48(9):905–911. https://doi.org/10.1016/j.oraloncology.2012.03.024
Michel J, Fakhry N, Mancini J et al (2014) Sinonasal squamous cell carcinomas: clinical outcomes and predictive factors. Int J Oral Maxillofac Surg 43(1):1–6. https://doi.org/10.1016/j.ijom.2013.07.741
Huang D, Xia P, Akazawa P et al (2003) Comparison of treatment plans using intensity-modulated radiotherapy and three-dimensional conformal radiotherapy for paranasal sinus carcinoma. Int J Radiat Oncol Biol Phys 56(1):158–168. https://doi.org/10.1016/s0360-3016(03)00080-4
Mock U, Georg D, Bogner J, Auberger T, Potter R (2004) Treatment planning comparison of conventional, 3D conformal, and intensity-modulated photon (IMRT) and proton therapy for paranasal sinus carcinoma. Int J Radiat Oncol Biol Phys 58(1):147–154. https://doi.org/10.1016/s0360-3016(03)01452-4
Chera BS, Malyapa R, Louis D et al (2009) Proton therapy for maxillary sinus carcinoma. Am J Clin Oncol 32(3):296–303. https://doi.org/10.1097/COC.0b013e318187132a
Jensen AD, Poulakis M, Nikoghosyan AV et al (2016) High-LET radiotherapy for adenoid cystic carcinoma of the head and neck: 15 year’s experience with raster-scanned carbon ion therapy. Radiother Oncol 118(2):272–280. https://doi.org/10.1016/j.radonc.2015.05.010
Zenda S, Kohno R, Kawashima M et al (2011) Proton beam therapy for unresectable malignancies of the nasal cavity and paranasal sinuses. Int J Radiat Oncol Biol Phys 81(5):1473–1478. https://doi.org/10.1016/j.ijrobp.2010.08.009
Hoffmann TK (2012) (2012) Systemic therapy strategies for head-neck carcinomas: Current status. GMS Curr Top Otorhinolaryngol Head Neck Surg 11:03. https://doi.org/10.3205/cto000085
Hanna EY, Cardenas AD, DeMonte F et al (2011) Induction chemotherapy for advanced squamous cell carcinoma of the paranasal sinuses. Arch Otolaryngol Head Neck Surg 137(1):78–81. https://doi.org/10.1001/archoto.2010.231
Licitra L, Locati LD, Cavina R et al (2003) Primary chemotherapy followed by anterior craniofacial resection and radiotherapy for paranasal cancer. Ann Oncol 14(3):367–372. https://doi.org/10.1093/annonc/mdg113
Homma A, Oridate N, Suzuki F et al (2009) Superselective high-dose cisplatin infusion with concomitant radiotherapy in patients with advanced cancer of the nasal cavity and paranasal sinuses: a single institution experience. Cancer 115(20):4705–4714. https://doi.org/10.1002/cncr.24515
Hoppe BS, Nelson CJ, Gomez DR et al (2008) Unresectable carcinoma of the paranasal sinuses: outcomes and toxicities. Int J Radiat Oncol Biol Phys 72(3):763–769. https://doi.org/10.1016/j.ijrobp.2008.01.038
Ferris RL, Blumenschein G Jr, Fayette J et al (2016) Nivolumab for Recurrent Squamous-Cell Carcinoma of the Head and Neck. N Engl J Med 375(19):1856–1867. https://doi.org/10.1056/NEJMoa1602252
Abdul-Aziz D, Kozin ED, Lin BM et al (2017) Temporal bone computed tomography findings associated with feasibility of endoscopic ear surgery. Am J Otolaryngol 38(6):698–703. https://doi.org/10.1016/j.amjoto.2017.06.007
Reeves TD, Hill EG, Armeson KE, Gillespie MB (2011) Cetuximab therapy for head and neck squamous cell carcinoma: a systematic review of the data. Otolaryngol Head Neck Surg 144(5):676–684. https://doi.org/10.1177/0194599811399559
Udager AM, Rolland DCM, McHugh JB et al (2015) High-Frequency Targetable EGFR Mutations in Sinonasal Squamous Cell Carcinomas Arising from Inverted Sinonasal Papilloma. Cancer Res 75(13):2600–2606. https://doi.org/10.1158/0008-5472.CAN-15-0340
Bauml JM, Aggarwal C, Cohen RB (2019) Immunotherapy for head and neck cancer: where are we now and where are we going? Ann Transl Med 7(3):S75. https://doi.org/10.21037/atm.2019.03.58
Dulguerov P, Jacobsen MS, Allal AS, Lehmann W, Calcaterra T. Nasal and paranasal sinus carcinoma: are we making progress? A series of 220 patients and a systematic review. Cancer 2001;92(12):3012–29 doi: 10.1002/1097–0142(20011215)92:12<3012::aid-cncr10131>3.0.co
Kilic S, Kilic SS, Baredes S et al (2018) Comparison of endoscopic and open resection of sinonasal squamous cell carcinoma: a propensity score-matched analysis of 652 patients. Int Forum Allergy Rhinol 8(3):421–434. https://doi.org/10.1002/alr.22040
Cantu G, Bimbi G, Miceli R et al (2008) Lymph node metastases in malignant tumors of the paranasal sinuses: prognostic value and treatment. Arch Otolaryngol Head Neck Surg 134(2):170–177. https://doi.org/10.1001/archoto.2007.30
Funding
There was no funding granted for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Leonard, C.G., Padhye, V. & Witterick, I.J. Management of squamous cell carcinomas of the skull-base. J Neurooncol 150, 377–386 (2020). https://doi.org/10.1007/s11060-020-03545-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03545-1