Abstract
Purpose
Primary central nervous system lymphoma (PCNSL) involving the hypothalamic–pituitary axis (H–P axis) is a rare intracranial neoplasm. We aimed to determine the unique characteristics and treatment outcomes of patients with PCNSL at the H–P axis and review the literature.
Methods
We retrospectively reviewed the electronic medical records of patients with PCNSL in our institute from 2000 to 2017. We analyzed patient characteristics, clinicopathologic features, imaging results, and treatment outcomes. Furthermore, we searched the PubMed database and gathered more cases from published studies to analyze patient treatment outcomes.
Results
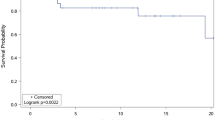
A total of 488 patients were diagnosed with central nervous system lymphoma at our institute. Seven (1.4%) patients had H–P axis involvement, five had diffuse large B-cell lymphoma, and two had mucosa-associated lymphoid tissue lymphoma. All patients had anterior pituitary lobe dysfunction, and two had posterior lobe dysfunction. The median progression-free survival (PFS) for seven patients was 29.0 (range: 0.9–48.1) months, and the 3-year survival rate was 42.9%. Pooled analysis included 45 patients. The median PFS for these patients was 7.0 months (0.9–52.0), and the 2-year survival rate was 20%. Univariate and multivariate analyses revealed that the patients with visual field defects had better prognosis (p = 0.0153 and 0.043, respectively).
Conclusion
PCNSL at the H–P axis is associated with a higher rate of pituitary dysfunction than other parasellar pathologies. PCNSL at the H–P axis has a worse treatment outcome than PCNSL at other sites. However, visual field defect is related to a favorable prognosis in these patients.



Similar content being viewed by others
References
Terada T, Kovacs K, Stefaneanu L, Horvath E (1995) Incidence, pathology, and recurrence of pituitary adenomas: study of 647 unselected surgical cases. Endocr Pathol 6(4):301–310. https://doi.org/10.1007/bf02738730
Famini P, Maya MM, Melmed S (2011) Pituitary magnetic resonance imaging for sellar and parasellar masses: ten-year experience in 2598 patients. J Clin Endocrinol Metab 96(6):1633–1641. https://doi.org/10.1210/jc.2011-0168
Huang BY, Castillo M (2005) Nonadenomatous tumors of the pituitary and sella turcica. Topics in magnetic resonance imaging: TMRI 16(4):289–299. https://doi.org/10.1097/01.rmr.0000224685.83629.18
Koiso T, Akutsu H, Takano S, Yamamoto T, Ishikawa E, Okoshi Y, Matsumura A (2014) Malignant lymphoma in the parasellar region. Case Rep Med 2014:747280. https://doi.org/10.1155/2014/747280
Yang J, Zhao N, Zhang G, Zheng W (2013) Clinical features of patients with non-Hodgkin's lymphoma metastasizing to the pituitary glands. Oncol Lett 5(5):1643–1648. https://doi.org/10.3892/ol.2013.1266
Rizek P, Seitelbach M, Alturkustani M, Leung A, Fraser JA (2012) Sellar and parasellar intravascular lymphoma mimicking pituitary apoplexy. J Neuroophthalmol 32(1):33–37. https://doi.org/10.1097/WNO.0b013e31823f457e
Giustina A, Gola M, Doga M, Rosei EA (2001) Clinical review 136: primary lymphoma of the pituitary: an emerging clinical entity. J Clin Endocrinol Metab 86(10):4567–4575. https://doi.org/10.1210/jcem.86.10.7909
Komninos J, Vlassopoulou V, Protopapa D, Korfias S, Kontogeorgos G, Sakas DE, Thalassinos NC (2004) Tumors metastatic to the pituitary gland: case report and literature review. J Clin Endocrinol Metab 89(2):574–580. https://doi.org/10.1210/jc.2003-030395
Villano JL, Koshy M, Shaikh H, Dolecek TA, McCarthy BJ (2011) Age, gender, and racial differences in incidence and survival in primary CNS lymphoma. Br J Cancer 105(9):1414–1418. https://doi.org/10.1038/bjc.2011.357
O'Neill BP, Decker PA, Tieu C, Cerhan JR (2013) The changing incidence of primary central nervous system lymphoma is driven primarily by the changing incidence in young and middle-aged men and differs from time trends in systemic diffuse large B-cell non-Hodgkin's lymphoma. Am J Hematol 88(12):997–1000. https://doi.org/10.1002/ajh.23551
Samaratunga H, Perry-Keene D, Apel RL (1997) Primary lymphoma of pituitary gland: a neoplasm of acquired malt? Endocr Pathol 8(4):335–341. https://doi.org/10.1007/bf02739936
Shaw JA, Strachan FM, Sawers HA, Bevan JS (1997) Non-Hodgkin lymphoma with panhypopituitarism, hyperprolactinaemia and sixth nerve palsy. J R Soc Med 90(5):274–275. https://doi.org/10.1177/014107689709000512
Freda PU, Post KD (1999) Differential diagnosis of sellar masses. Endocrinol Metabol Clin N Am 28(1):81–117. https://doi.org/10.1016/s0889-8529(05)70058-x
Kuhn D, Buchfelder M, Brabletz T, Paulus W (1999) Intrasellar malignant lymphoma developing within pituitary adenoma. Acta Neuropathol 97(3):311–316. https://doi.org/10.1007/s004010050990
Au WY, Kwong YL, Shek TW, Leung G, Ooi C (2000) Diffuse large-cell B-cell lymphoma in a pituitary adenoma: an unusual cause of pituitary apoplexy. Am J Hematol 63(4):231–232. https://doi.org/10.1002/(sici)1096-8652(200004)63:4%3c231:aid-ajh14%3e3.0.co;2-z
Mathiasen RA, Jarrahy R, Cha ST, Kovacs K, Herman VS, Ginsberg E, Shahinian HK (2000) Pituitary lymphoma: a case report and literature review. Pituitary 2(4):283–287. https://doi.org/10.1023/a:1009969417380
Landman RE, Wardlaw SL, McConnell RJ, Khandji AG, Bruce JN, Freda PU (2001) Pituitary lymphoma presenting as fever of unknown origin. J Clin Endocrinol Metab 86(4):1470–1476. https://doi.org/10.1210/jcem.86.4.7389
Kaufmann TJ, Lopes MB, Laws ER Jr, Lipper MH (2002) Primary sellar lymphoma: radiologic and pathologic findings in two patients. AJNR Am J Neuroradiol 23(3):364–367
Pascual JM, González-Llanos F, Roda JM (2002) Primary hypothalamic-third ventricle lymphoma. Case report and review of the literature. Neurocirugía 13(4):305–310. https://doi.org/10.1016/s1130-1473(02)70605-2
Katz BJ, Jones RE, Digre KB, Warner JE, Moore KR (2003) Panhypopituitarism as an initial manifestation of primary central nervous system non-Hodgkin's lymphoma. Endocr Pract 9(4):296–300. https://doi.org/10.4158/ep.9.4.296
Lee MT, Lee TI, Won JG, Chau WK, Yang HJ, Li JC, Lin HD, Tang KT (2004) Primary hypothalamic lymphoma with panhypopituitarism presenting as stiff-man syndrome. Am J Med Sci 328(2):124–128. https://doi.org/10.1097/00000441-200408000-00010
Rudnik A, Larysz D, Blamek S, Larysz P, Bierzynska-Macyszyn G, Wlaszczuk P, Bazowski P (2007) Primary pituitary lymphoma. Folia neuropathol 45(3):144–148
Liu JK, Sayama C, Chin SS, Couldwell WT (2007) Extranodal NK/T-cell lymphoma presenting as a pituitary mass. Case report and review of the literature. J Neurosurg 107(3):660–665. https://doi.org/10.3171/JNS-07/09/0660
Romeike BF, Joellenbeck B, Stein H, Loddenkemper C, Hummel M, Firsching R, Mawrin C (2008) Precursor T-lymphoblastic lymphoma within a recurrent pituitary adenoma. Acta Neurochir 150(8):833–836. https://doi.org/10.1007/s00701-008-1585-y
Tamer G, Kartal I, Aral F (2009) Pituitary infiltration by non-Hodgkin's lymphoma: a case report. J Med Case Rep 3:9293. https://doi.org/10.1186/1752-1947-3-9293
Chen SM, Chang CN, Wei KC, Jung SM, Chuang CC (2008) Sellar lymphoma mimicking sphenoid infection presenting with cavernous sinus syndrome. J Clin Neurosci 15(10):1148–1151. https://doi.org/10.1016/j.jocn.2007.08.021
Quintero Wolfe S, Hood B, Barker J, Benveniste RJ (2009) Primary central nervous system lymphoma mimicking pituitary apoplexy: case report. Pituitary 12(1):76–79. https://doi.org/10.1007/s11102-008-0084-8
Bayraktar S, Bassini W, Goodman M (2010) Primary pituitary lymphoma: idiopathic anasarca with relapse in bone marrow only. Acta Haematol 123(2):121–125. https://doi.org/10.1159/000272920
Fadoukhair Z, Amzerin M, Ismaili N, Belbaraka R, Latib R, Sbitti Y, M'Rabti H, Boutayeb S, Ichou M, Errihani H (2010) Symptomatic hypopituitarism revealing primary suprasellar lymphoma. BMC Endocr Disord 10:19. https://doi.org/10.1186/1472-6823-10-19
Yasuda M, Akiyama N, Miyamoto S, Warabi M, Takahama Y, Kitamura M, Yakushiji F, Kinoshita H (2010) Primary sellar lymphoma: intravascular large B-cell lymphoma diagnosed as a double cancer and improved with chemotherapy, and literature review of primary parasellar lymphoma. Pituitary 13(1):39–47. https://doi.org/10.1007/s11102-009-0196-9
Layden BT, Dubner S, Toft DJ, Kopp P, Grimm S, Molitch ME (2011) Primary CNS lymphoma with bilateral symmetric hypothalamic lesions presenting with panhypopituitarism and diabetes insipidus. Pituitary 14(2):194–197. https://doi.org/10.1007/s11102-008-0166-7
Hayasaka K, Koyama M, Yamashita T (2010) Primary pituitary lymphoma diagnosis by FDG-PET/CT. Clin Nucl Med 35(3):205. https://doi.org/10.1097/RLU.0b013e3181cc64a2
Martinez JH, Davila Martinez M, Mercado de Gorgola M, Montalvo LF, Tome JE (2011) The coexistence of an intrasellar adenoma, lymphocytic hypophysitis, and primary pituitary lymphoma in a patient with acromegaly. Case Rep Endocrinol 2011:941738. https://doi.org/10.1155/2011/941738
Anila KR, Nair RA, Koshy SM, Jacob PM (2012) Primary intravascular large B-cell lymphoma of pituitary. Indian J Pathol Microbiol 55(4):549–551. https://doi.org/10.4103/0377-4929.107811
Malaise O, Frusch N, Beck E, Servais S, Caers J, Caers J, de Prijck B, Betea D, Beguin Y (2012) Panhypopituitarism and diabetes insipidus in a patient with primary central nervous system lymphoma. Leuk Lymphoma 53(12):2515–2516. https://doi.org/10.3109/10428194.2012.682312
Li Y, Zhang Y, Xu J, Chen N (2011) Primary pituitary lymphoma in an immunocompetent patient: a rare clinical entity. J Neurol 259(2):297–305. https://doi.org/10.1007/s00415-011-6179-6
Carrasco CA, Rojas ZD, Chiorino R, Gonzalez G (2012) Primary pituitary lymphoma in immunocompetent patient: diagnostic problems and prolonged follow-up. Pituitary 15(1):93–96. https://doi.org/10.1007/s11102-010-0219-6
Rainsbury P, Mitchell-Innes A, Clifton N, Khalil H (2012) Primary lymphoma of the pituitary gland: an unusual cause of hemianopia in an immunocompetent patient. JRSM Short Rep 3(8):55. https://doi.org/10.1258/shorts.2012.012067
Wiens AL, Hagen MC, Bonnin JM, Rizzo KA (2012) T-cell lymphoblastic lymphoma/leukemia presenting as a pituitary mass lesion: a case report and review of the literature. Neuropathology 32(6):668–674. https://doi.org/10.1111/j.1440-1789.2012.01314.x
Papanastasiou L, Pappa T, Dasou A, Kyrodimou E, Kontogeorgos G, Samara C, Bacaracos P, Galanopoulos A, Piaditis G (2012) Case report: primary pituitary non-Hodgkin's lymphoma developed following surgery and radiation of a pituitary macroadenoma. Hormones (Athens, Greece) 11(4):488–494. https://doi.org/10.14310/horm.2002.1382
Wilkie MD, Al-Mahfoudh R, Javadpour M (2012) A rare case of primary sellar lymphoma presenting a diagnostic challenge. Br J Neurosurg 26(5):782–783. https://doi.org/10.3109/02688697.2012.674578
Cellina M, Fetoni V, Baron P, Orsi M, Oliva G (2015) Unusual primary central nervous system lymphoma location involving the fourth ventricle and hypothalamus. Neuroradiol J 28(2):120–125. https://doi.org/10.1177/1971400915576671
Ban VS, Chaudhary BR, Allinson K, Santarius T, Kirollos RW (2017) Concomitant primary CNS lymphoma and FSH-pituitary adenoma arising within the Sella: entirely coincidental? Neurosurgery 80(1):E170–E175. https://doi.org/10.1093/neuros/nyw003
Ravindra VM, Raheja A, Corn H, Driscoll M, Welt C, Simmons DL, Couldwell WT (2017) Primary pituitary diffuse large B-cell lymphoma with somatotroph hyperplasia and acromegaly: case report. J Neurosurg 126(5):1725–1730. https://doi.org/10.3171/2016.5.JNS16828
Tanki HN, Malik KN, Makhdoomi R, Feroz S, Ramzan AU (2018) Primary hypothalamic lymphoma in an adult male: a case report and literature review. Oman Med J 33(4):346–351. https://doi.org/10.5001/omj.2018.63
Tarabay A, Cossu G, Berhouma M, Levivier M, Daniel RT, Messerer M (2016) Primary pituitary lymphoma: an update of the literature. J Neurooncol 130(3):383–395. https://doi.org/10.1007/s11060-016-2249-z
Prabhakar VK, Shalet SM (2006) Aetiology, diagnosis, and management of hypopituitarism in adult life. Postgrad Med J 82(966):259–266. https://doi.org/10.1136/pgmj.2005.039768
Ferreri AJ, Blay JY, Reni M, Pasini F, Spina M, Ambrosetti A, Calderoni A, Rossi A, Vavassori V, Conconi A, Devizzi L, Berger F, Ponzoni M, Borisch B, Tinguely M, Cerati M, Milani M, Orvieto E, Sanchez J, Chevreau C, Dell'Oro S, Zucca E, Cavalli F (2003) Prognostic scoring system for primary CNS lymphomas: the International Extranodal Lymphoma Study Group experience. J Clin Oncol: Off J Am Soc Clin Oncol 21(2):266–272. https://doi.org/10.1200/jco.2003.09.139
Slone HW, Blake JJ, Shah R, Guttikonda S, Bourekas EC (2005) CT and MRI findings of intracranial lymphoma. AJR American J Roentgenol 184(5):1679–1685. https://doi.org/10.2214/ajr.184.5.01841679
Haldorsen IS, Espeland A, Larsson EM (2011) Central nervous system lymphoma: characteristic findings on traditional and advanced imaging. AJNR Am J Neuroradiol 32(6):984–992. https://doi.org/10.3174/ajnr.A2171
Zhang D, Hu LB, Henning TD, Ravarani EM, Zou LG, Feng XY, Wang WX, Wen L (2010) MRI findings of primary CNS lymphoma in 26 immunocompetent patients. Korean J Radiol 11(3):269–277. https://doi.org/10.3348/kjr.2010.11.3.269
Pisaneschi M, Kapoor G (2005) Imaging the sella and parasellar region. Neuroimaging Clin N Am 15(1):203–219. https://doi.org/10.1016/j.nic.2005.02.007
Grommes C, DeAngelis LM (2017) Primary CNS lymphoma. J Clin Oncol: Off J Am Soc Clin Oncol 35(21):2410–2418. https://doi.org/10.1200/jco.2017.72.7602
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Asan Medical Center, reference No. 2019-1067) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shin, DW., Kim, J.H., Kim, YH. et al. Primary central nervous system lymphoma involving the hypothalamic–pituitary axis: a case series and pooled analysis. J Neurooncol 147, 339–349 (2020). https://doi.org/10.1007/s11060-020-03422-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03422-x