Abstract
Background
Anaplastic lymphoma kinase (ALK) is expressed in ~ 60% of glioblastomas and conveys tumorigenic functions. Therefore, ALK inhibitory strategies with alectinib are conceivable for patients with glioblastoma. The aims of this preclinical study were to investigate efficacy as well as to understand and potentially overcome primary and acquired resistance mechanisms of alectinib in glioblastoma.
Methods
Efficacy of alectinib was analyzed dependent on ALK expression in different glioblastoma initiating cells and after lentiviral knockdown of ALK. Alectinib resistant cells were generated by continuous treatment with increasing alectinib doses over 3 months. M-RNA, phospho-protein and protein regulation were analyzed to decipher relevant pathways associated to treatment or resistance and specifically inhibited to evaluate rational salvage therapies.
Results
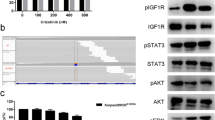
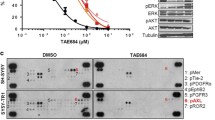
Alectinib reduced clonogenicity and proliferation and induced apoptosis in ALK expressing glioblastoma initiating cells, whereas cells without ALK expression or after ALK depletion via knockdown showed primary resistance against alectinib. High expression of cMyc and activation of the ERK1/2 pathway conferred resistance against alectinib in ALK expressing glioblastoma cells. Pharmacological inhibition of these pathways by cMyc inhibitor or MEK inhibitor, trametinib, overcame alectinib resistance and re-sensitized resistant cells to continued alectinib treatment. The combination of alectinib with radiotherapy demonstrated synergistic effects in inhibition of clonogenicity in non-resistant and alectinib resistant glioblastoma cells.
Conclusion
The data offer rationales for alectinib treatment in ALK expressing glioblastoma and for the use of ALK expression status as potential biomarker for alectinib treatment. In addition, the results propose MEK inhibition or radiotherapy as reasonable salvage treatments after acquired alectinib resistance.





Similar content being viewed by others
References
Kinoshita K, Asoh K, Furuichi N, Ito T, Kawada H, Hara S, Ohwada J, Miyagi T, Kobayashi T, Takanashi K, Tsukaguchi T, Sakamoto H, Tsukuda T, Oikawa N (2012) Design and synthesis of a highly selective, orally active and potent anaplastic lymphoma kinase inhibitor (CH5424802). Bioorg Med Chem 20(3):1271–1280. https://doi.org/10.1016/j.bmc.2011.12.021
Peters S, Camidge DR, Shaw AT, Gadgeel S, Ahn JS, Kim DW, Ou SI, Perol M, Dziadziuszko R, Rosell R, Zeaiter A, Mitry E, Golding S, Balas B, Noe J, Morcos PN, Mok T, Investigators AT (2017) Alectinib versus crizotinib in untreated ALK-positive non-small-cell lung cancer. N Engl J Med 377(9):829–838. https://doi.org/10.1056/NEJMoa1704795
Hida T, Nokihara H, Kondo M, Kim YH, Azuma K, Seto T, Takiguchi Y, Nishio M, Yoshioka H, Imamura F, Hotta K, Watanabe S, Goto K, Satouchi M, Kozuki T, Shukuya T, Nakagawa K, Mitsudomi T, Yamamoto N, Asakawa T, Asabe R, Tanaka T, Tamura T (2017) Alectinib versus crizotinib in patients with ALK-positive non-small-cell lung cancer (J-ALEX): an open-label, randomised phase 3 trial. Lancet 390(10089):29–39. https://doi.org/10.1016/S0140-6736(17)30565-2
Gadgeel S, Peters S, Mok T, Shaw AT, Kim DW, Ou SI, Perol M, Wrona A, Novello S, Rosell R, Zeaiter A, Liu T, Nuesch E, Balas B, Camidge DR (2018) Alectinib versus crizotinib in treatment-naive anaplastic lymphoma kinase-positive (ALK+) non-small-cell lung cancer: CNS efficacy results from the ALEX study. Ann Oncol. https://doi.org/10.1093/annonc/mdy405
Gourd E (2018) Alectinib shows CNS efficacy in ALK-positive NSCLC. Lancet Oncol 19(10):e520. https://doi.org/10.1016/S1470-2045(18)30707-1
Gainor JF, Sherman CA, Willoughby K, Logan J, Kennedy E, Brastianos PK, Chi AS, Shaw AT (2015) Alectinib salvages CNS relapses in ALK-positive lung cancer patients previously treated with crizotinib and ceritinib. J Thorac Oncol 10(2):232–236. https://doi.org/10.1097/JTO.0000000000000455
Soda M, Choi YL, Enomoto M, Takada S, Yamashita Y, Ishikawa S, Fujiwara S, Watanabe H, Kurashina K, Hatanaka H, Bando M, Ohno S, Ishikawa Y, Aburatani H, Niki T, Sohara Y, Sugiyama Y, Mano H (2007) Identification of the transforming EML4-ALK fusion gene in non-small-cell lung cancer. Nature 448(7153):561–566. https://doi.org/10.1038/nature05945
Morris SW, Kirstein MN, Valentine MB, Dittmer K, Shapiro DN, Look AT, Saltman DL (1995) Fusion of a kinase gene, ALK, to a nucleolar protein gene, NPM, in non-Hodgkin's lymphoma. Science 267(5196):316–317
Chen Y, Takita J, Choi YL, Kato M, Ohira M, Sanada M, Wang L, Soda M, Kikuchi A, Igarashi T, Nakagawara A, Hayashi Y, Mano H, Ogawa S (2008) Oncogenic mutations of ALK kinase in neuroblastoma. Nature 455(7215):971–974. https://doi.org/10.1038/nature07399
George RE, Sanda T, Hanna M, Frohling S, Luther W 2nd, Zhang J, Ahn Y, Zhou W, London WB, McGrady P, Xue L, Zozulya S, Gregor VE, Webb TR, Gray NS, Gilliland DG, Diller L, Greulich H, Morris SW, Meyerson M, Look AT (2008) Activating mutations in ALK provide a therapeutic target in neuroblastoma. Nature 455(7215):975–978. https://doi.org/10.1038/nature07397
Osajima-Hakomori Y, Miyake I, Ohira M, Nakagawara A, Nakagawa A, Sakai R (2005) Biological role of anaplastic lymphoma kinase in neuroblastoma. Am J Pathol 167(1):213–222. https://doi.org/10.1016/S0002-9440(10)62966-5
Hallberg B, Palmer RH (2013) Mechanistic insight into ALK receptor tyrosine kinase in human cancer biology. Nat Rev Cancer 13(10):685–700. https://doi.org/10.1038/nrc3580
Pulford K, Morris SW, Turturro F (2004) Anaplastic lymphoma kinase proteins in growth control and cancer. J Cell Physiol 199(3):330–358. https://doi.org/10.1002/jcp.10472
Parsons DW, Jones S, Zhang X, Lin JC, Leary RJ, Angenendt P, Mankoo P, Carter H, Siu IM, Gallia GL, Olivi A, McLendon R, Rasheed BA, Keir S, Nikolskaya T, Nikolsky Y, Busam DA, Tekleab H, Diaz LA Jr, Hartigan J, Smith DR, Strausberg RL, Marie SK, Shinjo SM, Yan H, Riggins GJ, Bigner DD, Karchin R, Papadopoulos N, Parmigiani G, Vogelstein B, Velculescu VE, Kinzler KW (2008) An integrated genomic analysis of human glioblastoma multiforme. Science 321(5897):1807–1812. https://doi.org/10.1126/science.1164382
Cancer Genome Atlas Research N (2008) Comprehensive genomic characterization defines human glioblastoma genes and core pathways. Nature 455(7216):1061–1068. https://doi.org/10.1038/nature07385
Karagkounis G, Stranjalis G, Argyrakos T, Pantelaion V, Mastoris K, Rontogianni D, Komaitis S, Kalamatianos T, Sakas D, Tiniakos D (2017) Anaplastic lymphoma kinase expression and gene alterations in glioblastoma: correlations with clinical outcome. J Clin Pathol 70(7):593–599. https://doi.org/10.1136/jclinpath-2016-204102
Ferguson SD, Xiu J, Weathers SP, Zhou S, Kesari S, Weiss SE, Verhaak RG, Hohl RJ, Barger GR, Reddy SK, Heimberger AB (2016) GBM-associated mutations and altered protein expression are more common in young patients. Oncotarget 7(43):69466–69478. https://doi.org/10.18632/oncotarget.11617
Wellstein A (2012) ALK receptor activation, ligands and therapeutic targeting in glioblastoma and in other cancers. Front Oncol 2:192. https://doi.org/10.3389/fonc.2012.00192
Chiba R, Akiya M, Hashimura M, Oguri Y, Inukai M, Hara A, Saegusa M (2017) ALK signaling cascade confers multiple advantages to glioblastoma cells through neovascularization and cell proliferation. PLoS ONE 12(8):e0183516. https://doi.org/10.1371/journal.pone.0183516
Stylianou DC, Auf der Maur A, Kodack DP, Henke RT, Hohn S, Toretsky JA, Riegel AT, Wellstein A (2009) Effect of single-chain antibody targeting of the ligand-binding domain in the anaplastic lymphoma kinase receptor. Oncogene 28(37):3296–3306. https://doi.org/10.1038/onc.2009.184
Powers C, Aigner A, Stoica GE, McDonnell K, Wellstein A (2002) Pleiotrophin signaling through anaplastic lymphoma kinase is rate-limiting for glioblastoma growth. J Biol Chem 277(16):14153–14158. https://doi.org/10.1074/jbc.M112354200
Grzelinski M, Steinberg F, Martens T, Czubayko F, Lamszus K, Aigner A (2009) Enhanced antitumorigenic effects in glioblastoma on double targeting of pleiotrophin and its receptor ALK. Neoplasia 11(2):145–156
Koyama-Nasu R, Haruta R, Nasu-Nishimura Y, Taniue K, Katou Y, Shirahige K, Todo T, Ino Y, Mukasa A, Saito N, Matsui M, Takahashi R, Hoshino-Okubo A, Sugano H, Manabe E, Funato K, Akiyama T (2014) The pleiotrophin-ALK axis is required for tumorigenicity of glioblastoma stem cells. Oncogene 33(17):2236–2244. https://doi.org/10.1038/onc.2013.168
Le Rhun E, Chamberlain MC, Zairi F, Delmaire C, Idbaih A, Renaud F, Maurage CA, Gregoire V (2015) Patterns of response to crizotinib in recurrent glioblastoma according to ALK and MET molecular profile in two patients. CNS Oncol 4(6):381–386. https://doi.org/10.2217/cns.15.30
Wick W, Dettmer S, Berberich A, Kessler T, Karapanagiotou-Schenkel I, Wick A, Winkler F, Pfaff E, Brors B, Debus J, Unterberg A, Bendszus M, Herold-Mende C, Eisenmenger A, von Deimling A, Jones DTW, Pfister SM, Sahm F, Platten M (2018) N2M2 (NOA20) phase I/II trial of molecularly matched targeted therapies plus radiotherapy in patients with newly diagnosed non-MGMT hypermethylated glioblastoma. Neuro Oncol. https://doi.org/10.1093/neuonc/noy161
Pfaff E, Kessler T, Balasubramanian GP, Berberich A, Schrimpf D, Wick A, Debus J, Unterberg A, Bendszus M, Herold-Mende C, Capper D, Schenkel I, Eisenmenger A, Dettmer S, Brors B, Platten M, Pfister SM, von Deimling A, Jones DTW, Wick W, Sahm F (2018) Feasibility of real-time molecular profiling for patients with newly diagnosed glioblastoma without MGMT promoter hypermethylation-the NCT Neuro Master Match (N2M2) pilot study. Neuro Oncol 20(6):826–837. https://doi.org/10.1093/neuonc/nox216
Lemke D, Weiler M, Blaes J, Wiestler B, Jestaedt L, Klein AC, Low S, Eisele G, Radlwimmer B, Capper D, Schmieder K, Mittelbronn M, Combs SE, Bendszus M, Weller M, Platten M, Wick W (2014) Primary glioblastoma cultures: can profiling of stem cell markers predict radiotherapy sensitivity? J Neurochem 131(2):251–264. https://doi.org/10.1111/jnc.12802
Campeau E, Ruhl VE, Rodier F, Smith CL, Rahmberg BL, Fuss JO, Campisi J, Yaswen P, Cooper PK, Kaufman PD (2009) A versatile viral system for expression and depletion of proteins in mammalian cells. PLoS ONE 4(8):e6529. https://doi.org/10.1371/journal.pone.0006529
Berberich A, Kessler T, Thome CM, Pusch S, Hielscher T, Sahm F, Oezen I, Schmitt LM, Ciprut S, Hucke N, Rubmann P, Fischer M, Lemke D, Breckwoldt MO, von Deimling A, Bendszus M, Platten M, Wick W (2018) Targeting resistance against the MDM2 inhibitor RG7388 in glioblastoma cells by the MEK inhibitor trametinib. Clin Cancer Res. https://doi.org/10.1158/1078-0432.CCR-18-1580
Hu Y, Smyth GK (2009) ELDA: extreme limiting dilution analysis for comparing depleted and enriched populations in stem cell and other assays. J Immunol Methods 347(1–2):70–78. https://doi.org/10.1016/j.jim.2009.06.008
Hertenstein A, Schumacher T, Litzenburger U, Opitz CA, Falk CS, Serafini T, Wick W, Platten M (2011) Suppression of human CD4+ T cell activation by 3,4-dimethoxycinnamonyl-anthranilic acid (tranilast) is mediated by CXCL9 and CXCL10. Biochem Pharmacol 82(6):632–641. https://doi.org/10.1016/j.bcp.2011.06.013
Bliss CI (1939) The toxicity of poisons applied jointly. Ann Appl Biol 26:585–615
Gainor JF, Dardaei L, Yoda S, Friboulet L, Leshchiner I, Katayama R, Dagogo-Jack I, Gadgeel S, Schultz K, Singh M, Chin E, Parks M, Lee D, DiCecca RH, Lockerman E, Huynh T, Logan J, Ritterhouse LL, Le LP, Muniappan A, Digumarthy S, Channick C, Keyes C, Getz G, Dias-Santagata D, Heist RS, Lennerz J, Sequist LV, Benes CH, Iafrate AJ, Mino-Kenudson M, Engelman JA, Shaw AT (2016) Molecular mechanisms of resistance to first- and second-generation ALK inhibitors in ALK-rearranged lung cancer. Cancer Discov 6(10):1118–1133. https://doi.org/10.1158/2159-8290.CD-16-0596
Golding B, Luu A, Jones R, Viloria-Petit AM (2018) The function and therapeutic targeting of anaplastic lymphoma kinase (ALK) in non-small cell lung cancer (NSCLC). Mol Cancer 17(1):52. https://doi.org/10.1186/s12943-018-0810-4
Gadgeel SM, Gandhi L, Riely GJ, Chiappori AA, West HL, Azada MC, Morcos PN, Lee RM, Garcia L, Yu L, Boisserie F, Di Laurenzio L, Golding S, Sato J, Yokoyama S, Tanaka T, Ou SH (2014) Safety and activity of alectinib against systemic disease and brain metastases in patients with crizotinib-resistant ALK-rearranged non-small-cell lung cancer (AF-002JG): results from the dose-finding portion of a phase 1/2 study. Lancet Oncol 15(10):1119–1128. https://doi.org/10.1016/S1470-2045(14)70362-6
Kodama T, Hasegawa M, Takanashi K, Sakurai Y, Kondoh O, Sakamoto H (2014) Antitumor activity of the selective ALK inhibitor alectinib in models of intracranial metastases. Cancer Chemother Pharmacol 74(5):1023–1028. https://doi.org/10.1007/s00280-014-2578-6
Iwahara T, Fujimoto J, Wen D, Cupples R, Bucay N, Arakawa T, Mori S, Ratzkin B, Yamamoto T (1997) Molecular characterization of ALK, a receptor tyrosine kinase expressed specifically in the nervous system. Oncogene 14(4):439–449. https://doi.org/10.1038/sj.onc.1200849
Rihawi K, Alfieri R, Fiorentino M, Fontana F, Capizzi E, Cavazzoni A, Terracciano M, La Monica S, Ferrarini A, Buson G, Petronini PG, Ardizzoni A (2018) MYC amplification as a potential mechanism of primary resistance to crizotinib in ALK-rearranged non-small cell lung cancer: a brief report. Transl Oncol 12(1):116–121. https://doi.org/10.1016/j.tranon.2018.09.013
Pilling AB, Kim J, Estrada-Bernal A, Zhou Q, Le AT, Singleton KR, Heasley LE, Tan AC, DeGregori J, Doebele RC (2018) ALK is a critical regulator of the MYC-signaling axis in ALK positive lung cancer. Oncotarget 9(10):8823–8835. https://doi.org/10.18632/oncotarget.24260
Chiarle R, Voena C, Ambrogio C, Piva R, Inghirami G (2008) The anaplastic lymphoma kinase in the pathogenesis of cancer. Nat Rev Cancer 8(1):11–23. https://doi.org/10.1038/nrc2291
Shaw AT, Friboulet L, Leshchiner I, Gainor JF, Bergqvist S, Brooun A, Burke BJ, Deng YL, Liu W, Dardaei L, Frias RL, Schultz KR, Logan J, James LP, Smeal T, Timofeevski S, Katayama R, Iafrate AJ, Le L, McTigue M, Getz G, Johnson TW, Engelman JA (2016) Resensitization to crizotinib by the lorlatinib ALK resistance mutation L1198F. N Engl J Med 374(1):54–61. https://doi.org/10.1056/NEJMoa1508887
Funding
L.S. was funded by the German Cancer Aid while performing this study (Funding No. 70112464). N2M2 is funded by the German Cancer Aid (7011980) and the resistance studies by DFG SFB 1389 TP A03 to W.W. and T.K.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no potential conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Berberich, A., Schmitt, LM., Pusch, S. et al. cMyc and ERK activity are associated with resistance to ALK inhibitory treatment in glioblastoma. J Neurooncol 146, 9–23 (2020). https://doi.org/10.1007/s11060-019-03348-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-019-03348-z