Abstract
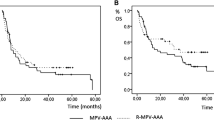
Treatment of recurrent primary CNS lymphoma (PCNSL) though not standardized most often utilizes whole brain radiotherapy, re-challenge with high-dose methotrexate, or administration of an alkylating chemotherapy. High-dose cytarabine (HD-araC) has been advocated as an active agent in PCNSL but limited information exists regarding single agent activity in the recurrent setting. A retrospective review of 14 patients (10 males, 4 females: median age 60 years) with recurrent PCNSL treated at second recurrence with single agent HD-araC. HD-araC was administered at 3gm/m2 over a 3-h infusion every 12 h for a total of 4 doses (defined as a cycle of therapy). GM-CSF was administered at conclusion of HD-araC. Patients were clinically and radiographically evaluated every 4-weeks. Common toxicity criteria Grade 3 or 4 toxicity included thrombocytopenia (11 patients; 79 %), anemia (10; 71 %), fatigue (8; 57 %), mucositis (8; 57 %), neutropenia (8; 57 %) and neutropenic fever (5; 36 %). No patient discontinued therapy due to toxicity nor were there any treatment-related deaths. Best response to HD-araC was stable disease in 6 patients (43 %), partial response in 5 (36 %) and progressive disease in 3 (21 %). Median progression free survival 3 months (range 2–5 months; 95 % CI 2–4 months) and progression free survival was 0 % at 6-months. Median survival after onset of HD-araC was 12 months (range 3–18+ months; 95 % CI 3–15 months). Single agent HD-araC has limited activity in recurrent PCNSL and is associated with significant toxicity in this small retrospective study.


Similar content being viewed by others
References
Rubenstein JL, Hsi ED, Johnson JL et al (2013) Intensive chemotherapy and immunotherapy in patients with newly diagnosed primary CNS lymphoma: CALGB 50202 (Alliance 50202). J Clin Oncol 31:3061–3068
Wang CC, Carnevale J, Rubenstein JL (2014) Progress in central nervous system lymphomas. Br J Haematol 166:311–325
Ponzoni M, Issa S, Batchelor TT, Rubenstein JL (2014) Beyond high-dose methotrexate and brain radiotherapy: novel targets and agents for primary CNS lymphoma. Ann Oncol 25:316–322
Rubenstein JL, Gupta NK, Mannis GN, Lamarre AK, Treseler P (2013) How I treat CNS lymphomas. Blood 122:2318–2330
Morris P, Correa DD, Yahalom J et al (2013) Rituximab, methotrexate, procarbazine and vincristine followed by consolidation reduced-dose whole brain radiotherapy and cytarabine in newly diagnosed primary CNS lymphoma: final results and long-term outcome. J Clin Oncol 31:3971–3979
Ferreri AJ, Ciceri F, Brandes AA et al (2014) MATILDE chemotherapy regimen for primary CNS lymphoma: results at a median follow-up of 12 years. Neurology 82:1370–1373
Chamberlain MC, Johnston SK (2010) High-dose methotrexate and rituximab with deferred radiotherapy for newly diagnosed primary B-cell CNS lymphoma. Neuro-Oncology 12:736–744
Ferreri AJM, Reni M, Foppoli M, International Extranodal Lymphoma Study Group (IELSG) et al (2009) High-dose cytarabine plus high-dose methotrexate versus high-dose methotrexate alone in patients with primary CNS lymphoma: a randomised phase 2 trial. Lancet 374:1512–1520
Thiel E, Korfel A, Martus P et al (2010) High-dose methotrexate with or without whole brain radiotherapy for primary CNS lymphoma (G-PCNSL-SG-1): a phase 3, randomised, non-inferiority trial. Lancet Oncol 11:1036–1047
Wieduwilt MJ, Valles F, Issa S et al (2012) Immunochemotherapy with intensive consolidation for primary CNS lymphoma: a pilot study and prognostic assessment by diffusion-weighted MRI. Clin Cancer Res 18:1146–1155
DeAngelis LM, Yahalom J, Thaler HT et al (1992) Combined modality therapy for primary CNS lymphoma. J Clin Oncol 10:635–643
Pentsova E, DeAngelis L, Omuro A (2014) Methotrexate re-challenge for recurrent primary central nervous system lymphoma. J Neuooncol 117:161–165
Reni M, Zaja F, Mason W et al (2007) Temozolomide as salvage treatment in primary brain lymphomas. Br J Cancer 96:864–867
Herrlinger U, Brugger W, Bamberg M et al (2000) PCV salvage chemotherapy for recurrent primary CNS lymphoma. Neurology 54:1707–1708
Reni M, Ferreri AJ (2001) Therapeutic management of refractory or relapsed primary central nervous system lymphomas. Ann Hematol 80(suppl 3):B113–B117
Frei E, Bickers JN, Hewlett JS et al (1979) Dose schedule and antitumor studies of arabinosyl cytosine. Cancer Res 29:1325–1332
Ho DHW, Frei E (1971) Clinical pharmacology of 1-B-D-arabinofuranosylcytosine. Clin Pharmacol Ther 12:944–954
Slevin ML, Piall EM, Aherne GW, Harvey VJ, Johnstoin HA, Lister TA (1983) Effect of dose and schedule on pharmacokinetics of high-dose cytosine arabinoside in plasma and cerebrospinal fluid. J Clin Oncol 1:546–551
Macdonald DR, Cascino TL, Schold SC et al (1990) Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 8:1277–1280
Nguyen PL, Chakravarti A, Finkelstein DM et al (2005) Results of whole-brain radiation as salvage of methotrexate failure for immunocompetent patients with primary CNS lymphoma. J Clin Oncol 23:1507–1513
Raizer JJ, Rademaker A, Evens AM et al (2012) Pemetrexed in the treatment of relapsed/refractory primary central nervous system lymphoma. Cancer 118:3743–3748
Fischer L, Thiel E, Klasen HA et al (2006) Prospective trial on topotecan salvage therapy in primary CNS lymphoma. Ann Oncol 17:1141–1145
Soussain C, Suzan F, Hoang-Xuan K et al (2001) Results of intensive chemotherapy followed by hematopoietic stem-cell rescue in 22 patients with refractory or recurrent primary CNS lymphoma or intraocular lymphoma. J Clin Oncol 19:742–749
Chamberlain MC (2014) Salvage therapy with bendamustine for methotrexate refractory recurrent primary CNS lymphoma: a retrospective case series. J Neurooncol 18:155–162
Acknowledgments
I would like to express my appreciation to Dr. Bernardo Goulart for statistical assistance and for the expert administrative assistance provided by Alisa Clein.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chamberlain, M.C. High-dose cytarabine salvage therapy for recurrent primary CNS lymphoma. J Neurooncol 126, 545–550 (2016). https://doi.org/10.1007/s11060-015-1994-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-015-1994-8