Abstract
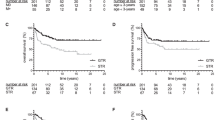
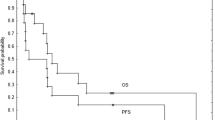
Embryonal tumors are an aggressive subtype of high-grade, pediatric central nervous system (CNS) tumors often with dismal survival rates. The 5-year survival for highest-risk embryonal tumors may be as low as 10 %. We report feasibility and efficacy from our experience using intravenous (IV) cyclophosphamide concurrently with craniospinal radiation (CSI) in high-risk embryonal CNS tumors of childhood. Ten consecutive children (aged: 3.5–15.5 years, median: 10.2 years, six male) with high-risk embryonal tumors, including: large cell/anaplastic medulloblastoma (6), atypical teratoid rhabdoid tumor (1), and leptomeningeal primitive neuroectodermal tumor (3), were treated with IV cyclophosphamide 1 g/M2 on days 1 and 2 of CSI. Following a median of 36 Gy CSI plus tumor boosts, adjuvant treatment consisted of 21 doses of oral etoposide (7) and alkylator based chemotherapy from five to eight cycles in all. Of the ten patients thus treated, six remain alive with no evidence of disease and four are deceased. Median survival was 3.3 years, with a 3-year progression-free survival of 50 % (5/10). Median follow-up was: 3.3 years (range: 5 months—12.9 years) in the five patients with progression, median time-to-progression was: 1.3 years (range: 1 month—3 years). Median follow-up in the patients without progression is 8.8 years (range: 3–12.9 years). Complications due to adjuvant chemotherapy were typical and included myelosupression (10), necessitating shortened duration of chemotherapy in three, and hemorrhagic cystitis (1). In high-risk embryonal CNS tumors, cyclophosphamide given concurrently with CSI is well tolerated. Early results suggest that a phase II trial is warranted.
Similar content being viewed by others
References
CBTRUS (2010) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the united states in 2004–2006. Central Brain Tumor Registry of the United States, Hinsdale. www.cbtrus.org. Accessed 23 May 2012
Ellison DW, Kocak M, Dalton J, Megahed H, Lusher ME, Ryan SL, Zhao W, Nicholson SL, Taylor RE, Bailey S, Clifford SC (2011) definition of disease-risk stratification groups in childhood medulloblastoma using combined clinical, pathologic, and molecular variables. J Clin Oncol 29(11):1400–1407
Gupta N, Banerjee A, Haas-Kogan D (eds) (2004) Pediatric CNS tumors. Embryonal Tumors. Springer, Berlin, pp 85–103
Albright AL, Wisoff JH, Zeltzer P, Boyett J, Rorke LB, Stanley P, Geyer JR, Milstein JM (1995) Prognostic factors in children with supratentorial (nonpineal) primitive neuroectodermal tumors. A neurosurgical perspective from the Children’s Cancer Group. Pediatr Neurosurg 22:1–7
Reddy AT, Janss AJ, Phillips PC, Weiss HL, Packer RJ (2000) Outcome for children with supratentorial primitive neuroectodermal tumors treated with surgery, radiation, and chemotherapy. Cancer 1:2189–2193
Pizer BL, Weston CL, Robinson KJ, Ellison DW, Ironside J, Saran F, Lashford LS, Tait D, Lucraft H, Walker DA, Bailey CC, Taylor RE (2006) Analysis of patients with supratentorial primitive neuro-ectodermal tumours entered into the SIOP/UKCCSG PNET 3 study. Eur J Cancer 42:1120–1128
Chintagumpala M, Hassall T, Palmer S, Ashley D, Wallace D, Kasow K, Merchant TE, Krasin MJ, Dauser R, Boop F, Krance R, Woo S, Cheuk R, Lau C, Gilbertson R, Gajjar A (2009) A pilot study of risk-adapted radiotherapy and chemotherapy in patients with supratentorial PNET. Neuro Oncol. 11:33–40
Athale UH, Duckworth J, Odame I, Barr R (2009) Childhood atypical teratoid rhabdoid tumor of the central nervous system: a meta-analysis of observational studies. J Pediatr Hematol Oncol 31(9):651–663
Tekautz TM, Fuller CE, Blaney S, Fouladi M, Broniscer A, Merchant TE, Krasin M, Dalton J, Hale G, Kune LE, Wallace D, Gilbertson RJ, Gajjar A (2005) Atypical Teratoid/Rhabdoid Tumors (ATRT): improved survival in children 3 years of age and older with radiation therapy and high-dose alkylator-based chemotherapy. J Clin Oncol 23:1491–1499
Chi SN, Zimmerman MA, Yao X, Cohen KJ, Berger P, Biegel JA, Rorke-Adams LB, Fisher MJ, Janss A, Mazewski C, Goldman S, Manley PE, Bowers DC, Bendel A, Rubin J, Turner CD, Marcus KJ, Goumnerova L, Ullrich NJ, Kieran MW (2009) Intensive multimodality treatment for children with newly diagnosed CNS atypical teratoid rhabdoid tumor. J Clin Oncol 27:385–389
Bailey CC, Gnekow A, Wellek S, Jones M, Round C, Brown J, Phillips A, Neidhardt MK (1999) Prospective randomized trial of chemotherapy given before radiotherapy in childhood medulloblastoma in children: conclusions from the Children’s Cancer Group 921 randomized phase II study. J Clin Oncol 17:832–845
Kortmann RD, Kühl J, Timmermann B, Mittler U, Urban C, Budach V, Richter E, Willich N, Flentje M, Berthold F, Slavc I, Wolff J, Meisner C, Wiestler O, Sörensen N, Warmuth-Metz M, Bamberg M (2000) Postoperative neoadjuvant chemotherapy before radiotherapy as compared to immediate radiotherapy followed by maintenance chemotherapy in the treatment of medulloblastoma in childhood: results of the German prospective randomized trial HIT’91. Int J Radiat Oncol Biol Phys 46:269–279
Bouffet E, Doz F, Demaille MC, Tron P, Roche H, Plantaz D, Thyss A, Stephan JL, Lejars O, Sariban E, Buclon M, Zücker JM, Brunat-Mentigny M, Bernard JL, Gentet JC (1995) Preirradiation chemotherapy including “eight drugs in 1 day” regimen and high-dose methotrexate in childhood medulloblastoma: results of the M7 French cooperative study. J Neurosurg 82:608–614
Mosijczuk AD, Nigro MA, Thomas PRM, Burger PC, Krischer JP, Morantz RA, Kurdunowicz B, Mulne AF, Towbin RB, Freeman AI, Nigro ED, Friedman HS, Kun LE (1993) Preradiation chemotherapy in advanced medulloblastoma a pediatric oncology group pilot study. Cancer 72:2755–2762
Duffner PK, Cohen ME, Sanford RA, Horowitz ME, Krischer JP, Burger PC, Friedman HS, Kun LE (1995) Lack of efficacy of postoperative chemotherapy and delayed radiation in very young children with pineoblastoma. Pediatr Oncol Group Med Pediatr Oncol 25:38–44
Hartsell WF, Gajjar A, Heideman RL, Langston JA, Sanford RA, Walter A, Jones D, Chen G, Kun LE (1997) Patterns of failure in children with medulloblastoma: effects of preirradiation chemotherapy. Int J Radiat Oncol Biol Phys 39:15–24
Packer R, Sutton LN, Elterman R, Lange B, Goldwein J, Nicholson HS, Mulne L, Boyett J, D’Angio G, Wechsler-Jentzsch K, Reaman G, Cohen BH, Bruce DA, Rorke LB, Molloy P, Ryan J, LaFond D, Evans AE, Schut L (1994) Outcome for children with medulloblastoma treated with radiation and cisplatin, CCNU, and vincristine chemotherapy. J Neurosurg 81:690–698
Douglas JG, Barker JL, Ellenbogen RG, Geyer JR (2004) Concurrent chemotherapy and reduced-dose cranial spinal irradiation followed by conformal posterior fossa tumor bed boost for average-risk medulloblastoma: efficacy and patterns of failure. Int J Radiat Oncol Biol Phys 58(4):1161–1164
Urban C, Benesch M, Pakisch B, Lackner H, Kerbl R, Schwinger W, Oberbauer R (1988) Synchronous radiochemotherapy in unfavorable brain tumors of children and young adults. J Neuro Oncol 39:71–80
Littman P, Rosenstock JG, Bailey C (1978) Radiation myelitis following craniospinal irradiation with concurrent actinomycin-D therapy. Med Pediatr Oncol 5:145–151
Jakacki RI, Burger PC, Zhou T, Holmes EJ, Kocak M, Onar A, Goldwein J, Mehta M, Packer RJ, Tarbell N, Fitz C, Vezina G, Hilden J, Pollack IF (2012) Outcome of children with metastatic medulloblastoma treated with Carboplatin during craniospinal radiotherapy: a Children’s Oncology Group phase I/II study. J Clin Oncol 30:2648–2653
Yamaguchi M, Tobinai K, Oguchi M, Ishizuka N, Kobayashi Y, Isobe Y, Ishizawa K, Maseki N, Itoh K, Usui N, Wasada I, Kinoshita T, Ohshima K, Matsuno Y, Terauchi T, Nawano S, Ishikura S, Kagami Y, Hotta T, Oshimi K (2009) Phase I/II study of concurrent chemoradiotherapy for localized nasal natural killer/t-cell lymphoma: Japan Clinical Oncology Group Study JCOG0211. J Clin Oncol 27:5594–5600
MacDermed DM, Miller LL, Peabody TD, Simon MA, Luu HH, Haydon RC, Montag AG, Undevia SD, Connell PP (2010) Primary tumor necrosis predicts distant control in locally advanced soft-tissue sarcomas after preoperative concurrent chemoradiotherapy. Int J Radiat Oncology 76:1147–1153
Common Terminology Criteria for Adverse Events (CTCAE) Version 4.0. US Department of Health and Human Services. NIH NCI. http://evs.nci.nih.gov/ftp1/CTCAE/About.html.Accessed May 28, 2009 (v4.03:June 14, 2010)
Yasuda K, Taguchi H, Sawamura Y, Ikeda J, Aoyama H, Fujieda K, Ishii N, Kashiwamura M, Iwasaki Y, Shirato H (2008) Low-dose craniospinal irradiation and ifosfamide, cisplatin and etoposide for non-metastatic embryonal tumors in the central nervous system. Jpn J Clin Oncol 38:486–492
Tait DM, Thornton-Jones H, Bloom HJ, Lemerle J, Morris-Jones P (1990) Adjuvant chemotherapy for medulloblastoma: the first multi-center control trial of the International Society of Paediatric Oncology (SIOPI). Eur J Cancer 26:464–469
Yule SM, Foreman NK, Mitchell C, Gouldon N, May P, McDowell HP (1997) High-dose cyclophosphamide for poor-prognosis and recurrent pediatric brain tumors: a dose-escalation study. J Clin Oncol 15:3258–3265
Allen JC, Helson L (1981) High-dose cyclophosphamide chemotherapy for recurrent CNS tumors in children. J Neurosurg 55:749–756
Conflict of interest
None.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Campen, C.J., Dearlove, J., Partap, S. et al. Concurrent cyclophosphamide and craniospinal radiotherapy for pediatric high-risk embryonal brain tumors. J Neurooncol 110, 287–291 (2012). https://doi.org/10.1007/s11060-012-0969-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-012-0969-2