Abstract
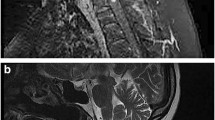
Intramedullary spinal cord metastases of solid neoplasms are associated with poor long-term survival. As the characteristics of secondary intramedullary spinal cord non-Hodgkin’s lymphoma (NHL) are not well understood, we sought to describe its clinical features and outcome. We retrospectively reviewed the Mayo Clinic patient database, lymphoma database, and pathology records from 1996 to 2010 and identified patients with clinical myelopathy and neuroimaging evidence of secondary intramedullary spinal cord involvement from pathologically confirmed systemic NHL. Seven patients were included in this study. The median age was 61 years (range, 41–81). Symptom onset was subacute (≤8 weeks) in six. Four patients were wheelchair-dependent at diagnosis. Spinal cord NHL was diagnosed by cerebrospinal fluid cytology in four; Positron emission tomography hypermetabolism in two; or MRI features alone. Myelopathy developed in five patients at a median 8 months (range, 1–58) following systemic NHL diagnosis, while myelopathy was the heralding symptom of NHL in two patients. Spinal cord MRI lesions were characteristically gadolinium enhancing and expansile. Four patients had co-existing MRI brain lesions. Six patients had B-cell NHL and one patient T-cell NHL. Six of the seven were treated (high dose intravenous methotrexate in three; radiation therapy in two; and R-CHOP in one). Median survival was 11.5 months (range, 1–28) with a 33% 2-year survival compared to historical median survival estimates of spinal cord metastases due to solid tumors of 3 months. In secondary intramedullary spinal cord involvement of NHL early neurological morbidity is common, but overall survival compares favorably to previously reported survival in spinal cord metastases from solid tumors.


Similar content being viewed by others
References
Grier J, Batchelor T (2005) Metastatic neurologic complications of non-Hodgkin’s lymphoma. Curr Oncol Rep 7:55–60
Schiff D, O’Neill BP (1996) Intramedullary spinal cord metastases: clinical features and treatment outcome. Neurology 47:906–912
Costigan DA, Winkelman MD (1985) Intramedullary spinal cord metastasis. A clinicopathological study of 13 cases. J Neurosurg 62:227–233
Batson OV (1995) The function of the vertebral veins and their role in the spread of metastases: 1940. Clin Orthop Relat Res 312:4–9
Mathur S, Law AJ, Hung N (2000) Late intramedullary spinal cord metastasis in a patient with lymphoblastic lymphoma: case report. J Clin Neurosci 7:264–268
Fisher RG (1979) Intramedullary lymphoma of the spinal cord. Neurosurgery 5:270–272
Wong Chung ME, van Heesewijk JP, Ramos LM (1991) Intramedullary non-Hodgkin’s lymphoma of the spinal cord; a case report. Eur J Radiol 12:226–227
Edelson RN, Deck MD, Posner JB (1972) Intramedullary spinal cord metastases. Clinical and radiographic findings in nine cases. Neurology 22:1222–1231
Sze G, Krol G, Zimmerman RD, Deck MD (1988) Intramedullary disease of the spine: diagnosis using gadolinium-DTPA-enhanced MR imaging. AJR Am J Roentgenol 151:1193–1204
Grem JL, Burgess J, Trump DL (1985) Clinical features and natural history of intramedullary spinal cord metastasis. Cancer 56:2305–2314
Flanagan EP, O’Neill BP, Porter AB, Lanzino G, Habermann TM, Keegan BM (2011) Primary intramedullary spinal cord lymphoma. Neurology 77(8):784–791
Pittock SJ, Lennon VA (2008) Aquaporin-4 autoantibodies in a paraneoplastic context. Arch Neurol 65:629–632
Flanagan EP, McKeon A, Lennon VA, Kearns J, Weinshenker BG, Krecke KN, Matiello M, Keegan BM, Mokri B, Aksamit AJ, Pittock SJ (2011) Paraneoplastic isolated myelopathy: clinical course and neuroimaging clues. Neurology 76(24):2089–2095
Keegan BM, Pittock SJ, Lennon VA (2008) Autoimmune myelopathy associated with collapsin response-mediator protein-5 immunoglobulin G. Ann Neurol 63:531–534
Chamroonrat W, Posteraro A, El-Haddad G, Zhuang H, Alavi A (2005) Radiation myelopathy visualized as increased FDG uptake on positron emission tomography. Clin Nucl Med 30:560
Cheshire WP, Santos CC, Massey EW, Howard JF Jr (1996) Spinal cord infarction: etiology and outcome. Neurology 47:321–330
Clarke JL, Perez HR, Jacks LM, Panageas KS, Deangelis LM (2010) Leptomeningeal metastases in the MRI era. Neurology 74:1449–1454
Hollender A, Kvaloy S, Lote K, Nome O, Holte H (2000) Prognostic factors in 140 adult patients with non-Hodgkin’s lymphoma with systemic central nervous system (CNS) involvement. A single centre analysis. Eur J Cancer 36:1762–1768
van Besien K, Ha CS, Murphy S, McLaughlin P, Rodriguez A, Amin K, Forman A, Romaguera J, Hagemeister F, Younes A, Bachier C, Sarris A, Sobocinski KS, Cox JD, Cabanillas F (1998) Risk factors, treatment, and outcome of central nervous system recurrence in adults with intermediate-grade and immunoblastic lymphoma. Blood 91:1178–1184
Conflict of interest
Drs. Flanagan, O’Neill, Porter and Habermann have no disclosures.Dr Keegan serves as Clinical Pathological Conference Section Co-Editor for Neurology, neurology podcast Panel and Chief Editor for eMedicine and has served as a consultant to Novartis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flanagan, E.P., O’Neill, B.P., Habermann, T.M. et al. Secondary intramedullary spinal cord non-Hodgkin’s lymphoma. J Neurooncol 107, 575–580 (2012). https://doi.org/10.1007/s11060-011-0781-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-011-0781-4