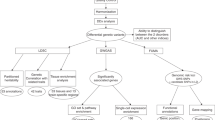
Studies of the genomic architecture of complex phenotypes, which include common somatic and mental diseases, have shown them to be characterized by high levels of polygenicity, i.e., there are large numbers of genes associated with the risk of developing these diseases. There is interest in establishing the genetic similarity of these two groups of diseases. The purpose of the present review is to analyze genetic studies of the comorbidity of somatic and mental diseases from the point of view of the universality and specificity of mental disorders in somatic diseases, the reciprocal relationships of these types of pathologies, and the modulating influence of external environmental factors on comorbidity. The analysis results point to the existence of a common genetic predisposition to mental and somatic diseases. The existence of genes common to both does not exclude specificity of the development of mental disorders in relation to specific somatic pathologies. We can suggest the existence of genes unique to a particular somatic and comorbid mental illness, as well as genes common to these diseases. Common genes may have varying degrees of specificity, i.e., they are universal in nature, this being apparent, for example, in the development of major depressive disorder in a variety of somatic diseases; common genes can also be specific for only a couple of individual diseases (schizophrenia and breast cancer). Moreover, common genes can have multidirectional effects, which also contributes to the specificity of comorbidity. In addition, the search for common genes for somatic and mental diseases needs account to be taken of the modulating influences of confounding factors (treatment, unhealthy lifestyle, behavioral characteristics), which may also differ in specificity depending on the diseases in question.
Similar content being viewed by others
References
Neznanov, N. G., Mazo, G. E., Rukavishnikov, G. V., and Kibitov, A. O., “Depression as a predictor of somatic diseases: pathophysiological prerequisites and genetic risk,” Usp. Fiziol. Nauk., 48, No. 4, 29–39 (2017).
Watanabe, K., Stringer, S., Frei, et al., “A global overview of pleiotropy and genetic architecture in complex traits,” Nat. Genet., 51, No. 9, 1339–1348 (2019).
Bennett, J. M., Reeves, G., Billman, G. E., et al., “Inflammation – nature’s way to efficiently respond to all types of challenges: Implications for understanding and managing ‘the epidemic’ of chronic diseases,” Front. Med (Lausanne), 5, 316 (2018).
Liang, C. S., Gałecki, P., and Su, K. P., “Unresolved systemic inflammation, long COVID, and the common pathomechanisms of somatic and psychiatric comorbidity,” J. Clin. Med., 11, No. 17, 5114 (2022).
Ji, H. F., Zhuang, Q. S., and Shen, L., “Genetic overlap between type 2 diabetes and major depressive disorder identified by bioinformatics analysis,” Oncotarget, 7, No. 14, 17410–17414 (2016).
Lu, D., Song, J., Lu, Y., et al., “A shared genetic contribution to breast cancer and schizophrenia,” Nat. Commun., 11, No. 1, 4637 (2020).
Lin, H., Lin, W. H., Lin, F., et al., “Potential pleiotropic genes and shared biological pathways in epilepsy and depression based on GWAS summary statistics,” Comput. Intell. Neurosci., 2022, 6799285 (2022).
Torgersen, K., Rahman, Z., Bahrami, S., et al., “Shared genetic loci between depression and cardiometabolic traits,” PLoS Genetics, 18, No. 5, e1010161 (2022).
Cao, H., Li, S., Baranova, A., et al., “Shared genetic liability between major depressive disorder and atopic diseases,” Front. Immunol., 12, 665160 (2021).
Pouget, J., Schizophrenia Working Group of the Psychiatric Genomics Consortium, Han, B., et al., “Cross-disorder analysis of schizophrenia and 19 immune-mediated diseases identifies shared genetic risk,” Hum. Mol. Genet., 28, No. 20, 3498–3513 (2019).
Fanelli, G., Franke, B., De Witte, W., et al., “Insulinopathies of the brain? Genetic overlap between somatic insulin-related and neuropsychiatric disorders,” Transl. Psychiatry, 12, No. 1, 59 (2022).
Amare, A. T., Schubert, K. O., Klingler-Hoffmann, M., et al., “The genetic overlap between mood disorders and cardiometabolic diseases: a systematic review of genome wide and candidate gene studies,” Transl. Psychiatry, 7, No. 1, e1007 (2017).
Massie, M. J., “Prevalence of depression in patients with cancer,” J. Natl. Cancer Inst. Monogr., 2004, 57–71 (2004).
Charles, E. F., Lambert, C. G., and Kerner, B., “Bipolar disorder and diabetes mellitus: evidence for disease-modifying effects and treatment implications,” Int. J. Bipolar. Disord., 4, No. 1, 13 (2016).
Jiang, X., Finucane, H. K., Schumacher, F. R., et al., “Shared heritability and functional enrichment across six solid cancers,” Nat. Commun., 10, No. 1, 431 (2019).
Wu, E., Ni, J. T., Xie, T., et al., “Noncausal effects of genetic predicted depression and colorectal cancer risk: A Mendelian randomization study,” Medicine (Baltimore), 101, No. 34, e30177 (2022).
Yuan, K., Song, W., Liu, Z., et al., “Mendelian randomization and GWAS meta analysis revealed the risk-increasing effect of schizophrenia on cancers,” Biology (Basel), 11, 1345 (2022).
Ge, F., Huo, Z., Liu, Y., et al., “Association between schizophrenia and prostate cancer risk: Results from a pool of cohort studies and Mendelian randomization analysis,” Compr. Psychiatry, 115, 152308 (2022).
Zhu, G. L., Xu, C., Yang, K. B., et al., “Causal relationship between genetically predicted depression and cancer risk: a two-sample bi-directional mendelian randomization,” BMC Cancer, 22, No. 1, 353 (2022).
Perry, B. I., Bowker, N., Burgess, S., et al., “Evidence for shared genetic aetiology between schizophrenia, cardiometabolic, and inflammation-related traits: Genetic correlation and colocalization analyses,” Schizophr. Bull. Open, 3, No. 1, sgac001 (2022), eCollection 2022.
Zhang, F., Cao, H., and Baranova, A., “Shared genetic liability and causal associations between major depressive disorder and cardiovascular diseases,” Front. Cardiovasc. Med., 11, No. 8, 735136 (2021).
Shi, J., Wu, L., Zheng, W., et al., “Genetic evidence for the association between schizophrenia and breast cancer,” J. Psychiatr. Brain Sci., 3, No. 4, 7 (2018).
Kim, S., Kim, K., Myung, W., et al., “Two-sample Mendelian randomization study for schizophrenia and breast cancer,” Precis. Future Med., 4, 21–30 (2020).
Lu, Y., Wang, Z., Georgakis, M. K., et al., “Genetic liability to depression and risk of coronary artery disease, myocardial infarction, and other cardiovascular outcomes,” J. Am. Heart Assoc., 10, No. 1, e017986-e (2021).
Zhuo, C. and Triplett, P. T., “Association of schizophrenia with the risk of breast cancer incidence: a meta-analysis,” JAMA Psychiatry, 75, 363–369 (2018).
Golimbet, V. E., Volel’, B. A., Korovaitseva, G. I., et al., “Depression comorbid with ischemic heart disease: a psychometric and molecular-genetic study,” Zh. Nevrol. Psikhiatr., 115, No. 2, 42–47 (2015).
Torgersen, K., Bahrami, S., Frei, O., et al., “Shared genetic architecture between neuroticism, coronary artery disease and cardiovascular risk factors,” Transl. Psychiatry, 11, No. 1, 368 (2021).
Frank, P., Ajnakina, O., Steptoe, A., et al., “Genetic susceptibility, inflammation and specific types of depressive symptoms: evidence from the English Longitudinal Study of Ageing,” Transl. Psychiatry, 10, No. 1, 140 (2020).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Nevrologii i Psikhiatrii imeni S. S. Korsakova, Vol. 123, No. 4, Iss. 2, pp. 60–64, April, 2023.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Golimbet, V.E., Klyushnik, T.P. Genome-Wide Studies of the Comorbidity of Somatic and Mental Diseases. Neurosci Behav Physi 53, 1386–1390 (2023). https://doi.org/10.1007/s11055-023-01531-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-023-01531-4