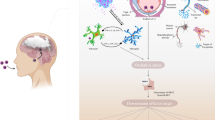
We present here an analysis of non-Russian publications illustrating changes in concepts relating to the etiology, pathogenesis, main pathophysiological syndromes, and clinical manifestations of nervous system damage in COVID-19 over 2.5 years of the pandemic. The current view of COVID-19 is that it is a pathology with a tendency to multiple organ damage, in which the symptoms of nervous system damage not only determine the severity of the disease, but also indirectly affect the development of somatic manifestations, such as distress syndrome. Particular attention is paid to analysis of publications summarizing available information on the incidence of cognitive deficit in the acute and post-COVID periods and their risk factors and prospects for recovery. The mechanisms probably underlying cognitive deficit are considered. Despite a significant number of observations and publications, some of the mechanisms of nervous system damage in COVID-19 and the selectivity of the cognitive deficit pattern remain unclear. Contemporary publications lack information on long term prognostication of the state of the cognitive domain, which is an important argument for research to continue.
Similar content being viewed by others
References
Mao, L., Jin, H., Wang, M., et al., “Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China,” JAMA Neurol., 77, No. 6, 683–690 (2020), https://doi.org/10.1001/jamaneurol.2020.1127.
Hamming, I., Timens, W., Bulthuis, M. L., et al., “Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis,” J. Pathol., 203, 631–637 (2004), https://doi.org/10.1002/path.1570.
Daly, J. L., Simonetti, B., Klein, K., et al., “Neuropilin-1 is a host factor for SARS-CoV-2 infection,” Science, 370, 861–865 (2020), https://doi.org/10.1126/science.abd3072.
Qi, J., Zhou, Y., Hua, J., et al., “The scRNA-seq expression profiling of the receptor ACE2 and the cellular protease TMPRSS2 reveals human organs susceptible to COVID-19 infection,” BioRxiv (2020), 2004.2016.045690, https://doi.org/10.3390/ijerph18010284.
Matschke, J., Lütgehetmann, M., Hagel, C., et al., “Neuropathology of patients with covid-19 in Germany: a post-mortem case series,” Lancet Neurol., 19, No. 11, 919–929 (2020), https://doi.org/10.1016/S1474-4422(20)30308-2.
Ehrengruber, M. U., Ehler, E., Billeter, M. A., and Naim, H. Y., “Measles virus spreads in rat hippocampal neurons by cell-to-cell contact and in a polarized fashion,” J. Virol., 76, 5720–5728 (2002), https://doi.org/10.1128/jvi.76.11.5720-5728.2002.
Brann, D. H., Tsukahara, T., Weinreb, C., et al., “Non-neuronal expression of SARS-CoV-2 entry genes in the olfactory system suggests mechanisms underlying COVID-19-associated anosmia,” Sci. Adv., 6, eabc5801 (2020), https://doi.org/10.1126/sciadv.abc5801.
Chen, R., Yu, J., Wang, K., et al., “The spatial and cell-type distribution of SARS-CoV-2 receptor ACE2 in human and mouse brain,” BioRxiv (2020), 2004.2007.030650, https://doi.org/10.3389/fneur.2020.573095.
Xia, S., Liu, M., Wang, C., et al., “Inhibition of SARS-CoV-2 (previously 2019-nCoV) infection by a highly potent pan-coronavirus fusion inhibitor targeting its spike protein that harbors a high capacity to mediate membrane fusion,” Cell Res., 30, 343–355 (2020), https://doi.org/10.1038/s41422-020-0305-x.
Puelles, V. G., Lütgehetmann, M., Lindenmeyer, M. T., et al., “Multiorgan and renal tropism of sars-cov-2,” N. Engl. J. Med., 383, No. 6, 590–592 (2020), https://doi.org/10.1056/NEJMc2011400.
Dubé, M., Le Coupanec, A., Wong, A. H. M., et al., “Axonal transport enables neuron-to-neuron propagation of human coronavirus oc43,” J. Virol., 92, e00404–e418 (2018), https://doi.org/10.1128/JVI.00404-18.
Jin, Y., Ji, W., Yang, H., et al., “Endothelial activation and dysfunction in COVID-19: From basic mechanisms to potential therapeutic approaches,” Signal Transduct. Target Ther., 5, 293 (2020), https://doi.org/10.1038/s41392-020-00454-7.
Stefano, G. B., Ptacek, R., Ptackova, H., et al., “Selective neuronal mitochondrial targeting in SARS-CoV-2 infection affects cognitive processes to induce ‘brain fog’ and results in behavioral changes that favor viral survival,” Med. Sci. Monit., 27, e930886 (2021), https://doi.org/10.12659/MSM.930886.
Huang, C., Wang, Y., Li, X., et al., “Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China,” Lancet, 395, 497–506 (2020), https://doi.org/10.1016/S0140-6736(20)30183-5.
The Great British Intelligence Test, https://www.bbc.co.uk/programmes/articles/5tFHwWMgg9VbrHT9kvGlFqd/the-great-britishintelligence-test.
Hampshirea, A., Trendera, W., Chamberlainb, S. R., et al., “Cognitive deficits in people who have recovered from COVID-19,” EClinical-Medicine, 39, 101044 (2021), https://doi.org/10.1016/j.eclinm.2021.101044.
Tabacof, L., Tosto-Mancuso, J., Wood, J., et al., “Post-acute COVID-19 syndrome negatively impacts physical function, cognitive function, health-related quality of life, and participation,” Am. J. Phys. Med. Rehabil., 101, No. 1, 48–52 (2022), https://doi.org/10.1097/PHM.0000000000001910.
Lamontagne, S. J., Winters, M. F., Pizzagalli, D. A., and Olmstead, M. C., “Post-acute sequelae of COVID-19: Evidence of mood and cognitive impairment,” Brain Behav. Immun. Health, 17, 100347 (2021), https://doi.org/10.1016/j.bbih.2021.100347.
Evans, R. A., McAuley, H., Harrison, E. M., et al., “Physical, cognitive, and mental health impacts of COVID-19 after hospitalisation (PHOSP-COVID, a UK multicentre, prospective cohort study,” Lancet Respir. Med., 9, No. 11, 1275–1287 (2021), https://doi.org/10.1016/S2213-2600(21)00383-0.
Liu, Y.-H., Wang, Y.-R., Wang, Q.-H., et al., “Post-infection cognitive impairments in a cohort of elderly patients with COVID-19,” Mol. Neurodegener., 16, No. 1, 48 (2021), https://doi.org/10.1186/s13024-021-00469-w.
Ferrucci, R., Dini, M., Rosci, C., et al., “One-year cognitive follow-up of COVID-19 hospitalized patients,” Eur. J. Neurol., 29, No. 7, 2006–2014 (2022), https://doi.org/10.1111/ene.15324.
Cristillo, V., Pilotto, A., Piccinelli, S. C., et al., “Premorbid vulnerability and disease severity impact on Long-COVID cognitive impairment,” Aging Clin. Exp. Res., 34, No. 1, 257–260 (2022), https://doi.org/10.1007/s40520-021-02042-3.
Duca, A., Pivo, S., Focà, E., et al., “Calculated decisions: Brescia-COVID Respiratory Severity Scale (BCRSS). Algorithm,” Emerg. Med. Pract., 22, No. 5, Supplement, CD1–CD2 (2020).
Hollocks, M. J., Brookes, R. L., Morris, R. G., and Markus, H. S., “The Brief Memory and Executive Test (BMET): A cognitive screening tool to detect and differentiate vascular cognitive impairment and Alzheimer’s disease,” Int. J. Geriatr. Psychiatry, 33, No. 2, 273–279 (2018), https://doi.org/10.1002/gps.4787.
Cecchetti, G., Agosta, F., Canu, E., et al., “Cognitive, EEG, and MRI features of COVID 19 survivors: a 10 month study,” J. Neurol., 34, No. 8, 1–13 (2022), https://doi.org/10.1007/s00415-022-11047-5.
Crivelli, L., Calandri, I., Corvalan, N., et al., “Cognitive consequences of COVID-19: results of a cohort study from South America,” Arq. Neuropsiquiatr., 80, No. 3, 240–247 (2022), https://doi.org/10.1590/0004-282X-ANP-2021-0320.
Jaywant, A., Vanderlind, W. M., Alexopoulos, G. S., et al., “Frequency and profile of objective cognitive deficits in hospitalized patients recovering from COVID-19,” Neuropsychopharmacology, 46, No. 13, 2235–2240 (2021), https://doi.org/10.1038/s41386-021-00978-8.
Alemanno, F., Houdayer, E., Parma, A., et al., “COVID-19 cognitive deficits after respiratory assistance in the subacute phase: A COVID rehabilitation unit experience,” PLoS One, 16, No. 2, e0246590 (2021), https://doi.org/10.1371/journal.pone.0246590.
Miskowiak, K. W., Johnsen, S., Sattler, S. M., et al., “Cognitive impairments four months after COVID-19 hospital discharge: Pattern, severity and association with illness variables,” Eur. Neuropsychopharmacol., 46, 39–48 (2021), https://doi.org/10.1016/j.euroneuro.2021.03.019.
Chen, C., Haupert, S. R., Zimmermann, L., et al., “Global prevalence of post COVID-19 condition or long COVID: A meta-analysis and systematic review,” J. Infect. Dis., 226, No. 9, 1593–2607 (2022), https://doi.org/10.1093/infdis/jiac136.
Ceban, F., Ling, S., Lui, L. M. W., et al., “Fatigue and cognitive impairment in Post-COVID-19 Syndrome: A systematic review and meta-analysis,” Brain Behav. Immun., 101, 93–135 (2022), https://doi.org/10.1016/j.bbi.2021.12.020.
Badenoch, J. B., Rengasamy, E. R., Watson, C., et al., “Persistent neuropsychiatric symptoms after COVID-19: a systematic review and meta-analysis,” Brain Commun., 4, No. 1, fcab297 (2021), https://doi.org/10.1093/braincomms/fcab297.
Mattioli, F., Stampatori, C., Righetti, F., et al., “Neurological and cognitive sequelae of Covid 19: a four month follow up,” J. Neurol., 268, No. 12, 4422–4428 (2021), https://doi.org/10.1007/s00415-021-10579-6.
Del Brutto, O. H., Rumbea, D. A., Recalde, B. Y., and Mera, R. M., “Cognitive sequelae of long COVID may not be permanent: A prospective study,” Eur. J. Neurol., 29, No. 4, 1218–1221 (2022), https://doi.org/10.1111/ene.15215.
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Nevrologii i Psikhiatrii imeni S. S. Korsakova, Vol. 122, No. 11, pp. 7–10, November, 2022.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kicherova, O.A., Reikhert, L.I., Akhmetyanov, M.A. et al. Cognitive Dysfunction in COVID-19. Neurosci Behav Physi 53, 818–821 (2023). https://doi.org/10.1007/s11055-023-01474-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-023-01474-w