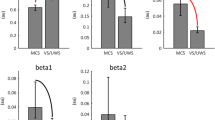
Objective. To assess impairments to cognitive functions and study the organization of brain bioelectrical activity in the sleep–waking cycle in patients with frontal lobe tumors. Materials and methods. Twenty patients of both sexes aged 48.6 ± 6.4 years and 10 healthy subjects (controls) were investigated. Group 1 included patients without neurological impairments with tumors of mean volume 8.9 ± 5.1 cm3 and group 2 included patients with signs of frontal dysfunction and mean tumor volume 40.7 ± 2.1 cm3. Impairments to cognitive functions were assessed using a battery of tests. The EEG was recorded in waking and during nocturnal sleep. Results. Degradation of cognitive functions in patients with frontal lobe tumors was accompanied by increases in power in the δ and θ ranges and cortical areactivity during waking, along with increased power in the δ, θ, and α frequency ranges and decreased activation in the REM sleep phase. Conclusions. The data obtained here may be of value in seeking markers for early signs of deterioration of cognitive functions in patients with frontal lobe tumors for prompt correction of patients’ functional status.
Similar content being viewed by others
References
K. Teffer and K. Semendeferi, “Human prefrontal cortex: evolution, development, and pathology,” Progr. Brain Res., 195, 191–218 (2012), https://doi.org/https://doi.org/10.1016/B978-0-444-53860-4.00009-X.
J. Hiser and M. Koenigs, “The multifaceted role of ventromedial prefrontal cortex in emotion, decision-making, social cognition, and psychopathology,” Biol. Psychiatry, 83, No. 8, 638–647 (2018), https://doi.org/https://doi.org/10.1016/j.biopsych.2017.10.030.
J. S. Fang, Y. Wang, and T. Jiang, “The influence of frontal lobe tumors and surgical treatment on advanced cognitive functions,” World Neurosurg., 91, 340–346 (2016), https://doi.org/https://doi.org/10.1016/j.wneu.2016.04.006.
Sh. Funahashi, “Principles of frontal lobe function,” Clin. Neurophysiol., 115, No. 1, 242–242 (2004), https://doi.org/https://doi.org/10.1016/S1388-2457(03)00300-6.
A. Del Arco and F. Mora, “Neurotransmitters and prefrontal cortex- limbic system interactions: Implications for plasticity and psychiatric disorders,” J. Neural Transm. (Vienna), 116, No. 8, 941–952 (2009), https://doi.org/https://doi.org/10.1007/s00702-009-0243-8.
S. M. Szczepanski and R. T. Knight, “Insights into human behavior from lesions to the prefrontal cortex,” Neuron, 83, No. 5, 1002–1018 (2014), https://doi.org/https://doi.org/10.1016/j.neuron.2014.08.011.
M. K. Scullin and Ch. Gao, “Dynamic contributions of slow wave sleep and REM sleep to cognitive longevity,” Curr. Sleep Med. Rep., 4, No. 4, 284–293 (2018), https://doi.org/https://doi.org/10.1007/s40675-018-0131-6.
M. C. Della, S. Johnsen, G. Atzori, et al., “Rapid eye movement sleep, sleep continuity and slow wave sleep as predictors of cognition, mood, and subjective sleep quality in healthy men and women, aged 20–84 years,” Front. Psychiatry, 9, 255–272 (2018), https://doi.org/https://doi.org/10.3389/fpsyt.2018.00255.
J. Haba-Rubio, H. Marti-Soler, N. Tobback, et al., “Characteristics and cognitive impairment in the general population. The HypnoLaus Study,” Neurology, 88, 463–469 (2017), https://doi.org/https://doi.org/10.1212/WNL.0000000000003557.
M. G. Poluektov and I. S. Preobrazhenskaya, “Impairments to sleep and cognitive functions, approaches to therapy,” Nevrol. Neiropsikh. Psikhosom., No. 1, 68–73 (2014), https://doi.org/10.14412/2074-2711-2014-1-68-73.
M. Hu, P. Zhang, C. Li, et al., “Sleep disturbance in mild cognitive impairment: a systematic review of objective measures,” Neurol. Sci., 38, No. 8, 1363–1371 (2017), https://doi.org/https://doi.org/10.1007/s10072-017-2975-9.
J.-A. Bertrand, D. G. Marchand, R. B. Postuma, and J.-F. Gagnon, “Cognitive dysfunction in rapid eye movement sleep behavior disorder,” Sleep and Biological Rhythms, 11, 21–26 (2013), https://doi.org/https://doi.org/10.1111/j.1479-8425.2012.00547.x.
O. I. Kit, A. I. Shikhliarova, G. V. Zhukova, et al., “Activation Therapy: Theoretical and applied aspects,” Cardiometry, 7, 22–29 (2015), https://doi.org/https://doi.org/10.12710/cardiometry.2015.7.2229.
M. K. Folstein, S. E. Folstein, and P. R. McHugh, “Mini-Mental State. A practical method for grading the cognitive state of patients for the clinician,” J. Psychiatr. Res., 12, No. 3, 189–198 (1975).
B. Dubois and I. Litvan, “The FAB: A Frontal Assessment Battery at bedside,” Neurology, 55, No. 11, 1621–1626 (2000), https://doi.org/https://doi.org/10.1212/wnl.55.11.1621.
D. Maust, M. Cristancho, L. Gray, et al., “Psychiatric rating scales,” in: Handbook of Clinical Neurology, M. J. Aminoff et al., (eds.), Elsevier, New York, NY (2012).
The AASM Manual for the Scoring of Sleep and Associated Events: Rules, Terminology, and Technical Specifications. Scoring Manual, Vers. 2016-v.2.3.0, https://rtsleepworld.com, acc. June 1, 2019.
I. N. Deryabina, “Characteristics of brain bioelectrical activity in elderly women with different levels of cognitive impairment,” Ekol. Cheloveka, 10, 51–56 (2016).
N. Fauzan and A. Nur Hurunain, “Early detection of mild cognitive impairment, dementia and Alzheimer’s using qEEG,” Eur. J. Interdiscip. Stud., No. 3, 152–159 (2015), https://doi.org/10.26417/ejis.v3i1.p149-153.
E. Hita-Yañez, M. Atienza, and J. L. Cantero, “Polysomnographic and subjective sleep markers of mild cognitive impairment,” Sleep, 36, No. 9, 1327–1334 (2013), https://doi.org/https://doi.org/10.5665/sleep.2956.
C. E. Westerberg, B. A. Mander, S. M. Florczak, et al., “Concurrent impairments in sleep and memory in amnestic mild cognitive impairment,” J. Int. Neuropsychol. Sol., 18, 490–500 (2012), https://doi.org/https://doi.org/10.1017/S135561771200001X.
J. Taillard, P. Sagaspe, C. Berthomier, et al., “Non-REM sleep characteristics predict early cognitive impairment in an aging population,” Front. Neurol., 10, 197 (2019), https://doi.org/https://doi.org/10.3389/fneur.2019.00197.
R. J. Brazète, J. Montplaisir, D. Petit, et al., “Electroencephalogram slowing in rapid eye movement sleep behavior disorder is associated with mild cognitive impairment,” Sleep Med., 14, No. 11, 1059–1063 (2013), https://doi.org/https://doi.org/10.1016/j.sleep.2013.06.013.
B. Guarnieri and S. Sorbi, “Sleep and cognitive decline: A strong bidirectional relationship. It is time for specific recommendations on routine assessment and the management of sleep disorders in patients with mild cognitive impairment and dementia,” Eur. J. Neurol., 74, No. 1–2, 43–48 (2015), https://doi.org/https://doi.org/10.1159/000434629.
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Nevrologii i Psikhiatrii imeni S. S. Korsakova, Vol. 122, No. 3, Iss. 1, pp. 106–111, March, 2022.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arapova, Y.Y., Popov, I.A., Shikhliarova, A.I. et al. Studies of Cognitive Functions and the Organization of Brain Bioelectrical Activity during Waking and Sleep in Patients with Frontal Lobe Tumors. Neurosci Behav Physi 52, 994–998 (2022). https://doi.org/10.1007/s11055-022-01328-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-022-01328-x