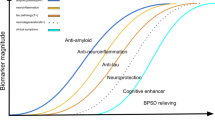
Multiple sclerosis (MS) is chronic autoimmune disease with a high level of heterogeneity in its course and prognosis. More than half of patients with MS do not discuss their long-term prognosis with the treating doctor. Most patients regard personalized information on the course of MS as extremely important in relation to taking decisions on family planning, choice of profession, and treatment. Determination of prognosis in routine clinical practice uses clinical markers, though these are nominally divided into favorable and unfavorable factors, which allows general conclusions regarding the prognosis of MS to be made. Neuroimaging and biological markers are mainly used for research purposes, though they are now actively employed in clinical studies to assess the effects of treatment on the organic causes of persistent disability. This review describes studies of the prognostic value of various clinical, neuroimaging, and biological markers.
Similar content being viewed by others
References
All-Russian Society of Neurologists, Clinical Guidelines for Multiple Sclerosis (2019), https://www.ructrims.org/files/%D0%9A%D0%BB%D0%B8%D0%BD%20%D1%80%D0%B5%D0%BA%D0%A0%D0%A1_2019_3.docx, acc. Feb. 15, 2021.
N. Ghasemi, S. Razavi, and E. Nikzad, “Multiple sclerosis: Pathogenesis, symptoms, diagnoses and cell-based therapy,” Cell J., 19, No. 1, 1–10 (2017), https://doi.org/10.22074/cellj.2016.4867.
Q. Wu, E. A. Mills, Q. Wang, et al., “Siponimod enriches regulatory T and B lymphocytes in secondary progressive multiple sclerosis,” JCI Insight, 5, No. 3 (2020), https://doi.org/10.1172/jci.insight.134251.
T. Ziemssen, K. Akgün, and W. Brück, “Molecular biomarkers in multiple sclerosis,” J. Neuroinflamm., 16, No. 1, 272 (2019), https://doi.org/10.1186/s12974-019-1674-2.
R. Bergamaschi, C. Berzuini, A. Romani, and V. Cosi, “Predicting secondary progression in relapsing-remitting multiple sclerosis: a Bayesian analysis,” J. Neurol. Sci., 189, No. 1–2, 13–21 (2001), https://doi.org/10.1016/S0022-510X(01)00572-X.
A. Fambiatos, V. Jokubaitis, D. Horakova, et al., “Risk of secondary progressive multiple sclerosis: A longitudinal study,” Mult. Scler., 26, No. 1, 79–90 (2020), https://doi.org/10.1177/1352458519868990.
F. B. S. Briggs, J. C. Yu, M. F. Davis, et al., “Multiple sclerosis risk factors contribute to onset heterogeneity,” Mult. Scler. Relat. Disord., 28, 11–16 (2019), https://doi.org/10.1016/j.msard.2018.12.007.
A. N. Boiko, B. T. Mugutdinova, and T. M. Mugutdinov, “Prognostic significance of neuropsychological tests in patients with typical remitting multiple sclerosis,” Med. Alfavit, 2, No. 17(354) (2018), https://elibrary.ru/item.asp?id=36574676.
K. Tilling, M. Lawton, N. Robertson, et al., “Modelling disease progression in relapsing-remitting onset multiple sclerosis using multilevel models applied to longitudinal data from two natural history cohorts and one treated cohort,” Health Technol. Assess., 20, No. 81, 1–48 (2016), https://doi.org/10.3310/hta20810.
Proceedings of the Third All-Russian Congress with International Participation, “Multiple Sclerosis and Other Demyelinating Diseases (ROKIRS/RUCTRIMS Congress), Ekaterinburg, Sept. 13–16, 2018, Zh. Nevrol. Psikhiat., 118, No. 8, Spec. Iss., 128–171 (2018), https://doi.org/10.17116/jnevro2018118082128.
A. I. Volkov and E. V. Popova, “New tools for early detection of the progression of multiple sclerosis,” Zh. Nevrol. Psikhiatr., 120, No. 7–2 (2020), https://doi.org/10.17116/jnevro202012007243.
S. S. Jordy, A. Starzewski, Jr., F. A. Macedo, et al., “Olfactory alterations in patients with multiple sclerosis,” Arq. Neuropsiquiatr., 74, No. 9, 697–700 (2016), https://doi.org/10.1590/0004-282X20160128.
L. Tonetti, F. Camilli, S. Giovagnoli, et al., “Circadian activity rhythm in early relapsing-remitting multiple sclerosis,” J. Clin. Med., 8, No. 12 (2019), https://doi.org/10.3390/jcm8122216.
O. Mirmosayyeb, S. Brand, M. Barzegar, et al., “Clinical characteristics and disability progression of early- and late-onset multiple sclerosis compared to adult-onset multiple sclerosis,” J. Clin. Med., 9, No. 5 (2020), https://doi.org/10.3390/jcm9051326.
A. V. Genovese, J. Hagemeier, N. Bergsland, et al., “Atrophied brain T2 lesion volume at MRI is associated with disability progression and conversion to secondary progressive multiple sclerosis,” Radiology, 293, No. 2, 424–433 (2019), https://doi.org/10.1148/radiol.2019190306.
E. Fisher, J. C. Lee, K. Nakamura, and R. A. Rudick, “Gray matter atrophy in multiple sclerosis: a longitudinal study,” Ann. Neurol., 64, No. 3, 255–265 (2008), https://doi.org/10.1002/ana.21436.
L. K. Fisniku, P. A. Brex, D. R. Altmann, et al., “Disability and T2 MRI lesions: a 20-year follow-up of patients with relapse onset of multiple sclerosis,” Brain, 131, No. 3, 808–817 (2008), https://doi.org/10.1093/brain/awm329.
R. Cortese, S. Collorone, O. Ciccarelli, and A. T. Toosy, “Advances in brain imaging in multiple sclerosis,” Ther. Adv. Neurol. Disord., 12 (2019), https://doi.org/10.1177/1756286419859722.
A. Eshaghi, R. V. Marinescu, A. L. Young, et al., “Progression of regional grey matter atrophy in multiple sclerosis,” Brain, 141, No. 6, 1665–1677 (2018), https://doi.org/10.1093/brain/awy088.
A. Eshaghi, F. Prados, W. J. Brownlee, et al., and the MAGNIMS study group., “Deep gray matter volume loss drives disability worsening in multiple sclerosis,” Ann. Neurol., 83, No. 2, 210–222 (2018), https://doi.org/10.1002/ana.25145.
M. Bross, M. Hackett, and E. Bernitsas, “Approved and emerging disease modifying therapies on neurodegeneration in multiple sclerosis,” Int. J. Mol. Sci., 21, No. 12, 4312 (2020), https://doi.org/10.3390/ijms21124312.
A. Gajofatto, M. Calabrese, M. D. Benedetti, and S. Monaco, “Clinical, MRI, and CSF markers of disability progression in multiple sclerosis,” Dis. Markers, 35, 484959 (2013), https://doi.org/10.1155/2013/484959.
B. Audoin, G. R. Davies, L. Finisku, et al., “Localization of grey matter atrophy in early RRMS,” J. Neurol., 253, No. 11, 1495–1501 (2006), https://doi.org/10.1007/s00415-006-0264-2.
M. A. Rocca, S. Mesaros, E. Pagani, et al., “Thalamic damage and long-term progression of disability in multiple sclerosis,” Radiology, 257, No. 2, 463–469 (2010), https://doi.org/10.1148/radiol.10100326.
P. Preziosa, M. A. Rocca, S. Mesaros, et al., “Intrinsic damage to the major white matter tracts in patients with different clinical phenotypes of multiple sclerosis: a voxelwise diffusion-tensor MR study,” Radiology, 260, No. 2, 541–550 (2011), https://doi.org/10.1148/radiol.11110315.
R. J. Fox, T. Cronin, J. Lin, et al., “Measuring myelin repair and axonal loss with diffusion tensor imaging,” AJNR Am. J. Neuroradiol., 32, No. 1, 85–91 (2011), https://doi.org/10.3174/ajnr.A2238.
R. T. Naismith, J. Xu, N. T. Tutlam, et al., “Increased diffusivity in acute multiple sclerosis lesions predicts risk of black hole,” Neurology, 74, No. 21, 1694–1701 (2010), https://doi.org/10.1212/WNL.0b013e3181e042c4.
D. Ontaneda and R. J. Fox, “Imaging as an outcome measure in multiple sclerosis,” Neurotherapeutics, 14, No. 1, 24–34 (2017), https://doi.org/10.1007/s13311-016-0479-6.
M. Absinta, P. Sati, and D. S. Reich, “Advanced MRI and staging of multiple sclerosis lesions,” Nat. Rev. Neurol., 12, No. 6, 358–368 (2016), https://doi.org/10.1038/nrneurol.2016.59.
A. Dal-Bianco, G. Grabner, C. Kronnerwetter, et al., “Slow expansion of multiple sclerosis iron rim lesions: pathology and 7 T magnetic resonance imaging,” Acta Neuropathol., 133, No. 1, 25–42 (2017), https://doi.org/10.1007/s00401-016-1636-z.
C. Elliott, J. S. Wolinsky, S. L. Hauser, et al., “Slowly expanding/evolving lesions as a magnetic resonance imaging marker of chronic active multiple sclerosis lesions,” Mult. Scler., 25, No. 14, 1915–1925 (2019), https://doi.org/10.1177/1352458518814117.
A. A. Bogdan, Changes in the Functional State of Brain Matter in Multiple Sclerosis Based on Proton Magnetic Resonance Spectroscopy Data (2020), publ. online, https://cutt.ly/cjFwnIN, acc. Jan. 18, 2021.
V. I. Golovkin, A. V. Pozdnyakov, Yu. F. Kamynin, and I. S. Martens, “New techniques for predicting therapy in multiple sclerosis,” Byull. Sib. Med., 9, No. 4, 138–144 (2010), https://doi.org/10.20538/1682-0363-2010-4-138-144.
R. Srinivasan, N. Sailasuta, R. Hurd, et al., “Evidence of elevated glutamate in multiple sclerosis using magnetic resonance spectroscopy at 3 T,” Brain, 128, No. 5, 1016–1025 (2005), https://doi.org/10.1093/brain/awh467.
T. A. Kobys’, “Neuroimaging predictors of the progression of disability in multiple sclerosis,” Vestn. Sovrem. Klin. Med., 9, No. 4 (2016), https://cyberleninka.ru/article/n/neyrovizualizatsionnye-prediktory-progressirovaniya-invalidizatsii-pri-rasseyannom-skleroze, acc. Dec. 3, 2020.
C. Tur, A. Eshaghi, D. R. Altmann, et al., “Structural cortical network reorganization associated with early conversion to multiple sclerosis,” Sci. Rep., 8, No. 1, 10715 (2018), https://doi.org/10.1038/s41598-018-29017-1.
T. Charalambous, C. Tur, F. Prados, et al., “Structural network disruption markers explain disability in multiple sclerosis,” J Neurol. Neurosurg. Psychiatry, 90, No. 2, 219–226 (2019), https://doi.org/10.1136/jnnp-2018-318440.
B. Nourbakhsh and E. M. Mowry, “Multiple sclerosis risk factors and pathogenesis,” Continuum (Minneap. Minn.), 25, No. 3, 596–610 (2019), https://doi.org/10.1212/CON.0000000000000725.
C. E. Teunissen, H. Tumani, S. Engelborghs, and B. Mollenhauer, “Biobanking of CSF: international standardization to optimize biomarker development,” Clin. Biochem., 47, No. 4–5, 288–292 (2014), https://doi.org/10.1016/j.clinbiochem.2013.12.024.
M. Tintore, À. Rovira, J. Río, et al., “Defining, high, medium and low impact prognostic factors for developing multiple sclerosis,” Brain, 138, No. 7, 1863–1874 (2015), https://doi.org/10.1093/brain/awv105.
J. Kuhle, G. Disanto, R. Dobson, et al., “Conversion from clinically isolated syndrome to multiple sclerosis: A large multicentre study,” Mult. Scler., 21, No. 8, 1013–1024 (2015), https://doi.org/10.1177/1352458514568827.
G. Hinsinger, N. Galéotti, N. Nabholz, et al., “Chitinase 3-like proteins as diagnostic and prognostic biomarkers of multiple sclerosis,” Mult. Scler., 21, No. 10, 1251–1261 (2015), https://doi.org/10.1177/1352458514561906.
M. S. Boesen, P. E. H. Jensen, M. Magyari, et al., “Increased cerebrospinal fluid chitinase 3-like 1 and neurofilament light chain in pediatric acquired demyelinating syndromes,” Mult. Scler. Relat. Disord., 24, 175–183 (2018), https://doi.org/10.1016/j.msard.2018.05.017.
E. Thouvenot, G. Hinsinger, C. Demattei, et al., “Cerebrospinal fluid chitinase-3-like protein 1 level is not an independent predictive factor for the risk of clinical conversion in radiologically isolated syndrome,” Mult. Scler., 25, No. 5, 669–677 (2019), https://doi.org/10.1177/1352458518767043.
P. Kušnierová, D. Zeman, P. Hradílek, et al., “Determination of chitinase 3-like 1 in cerebrospinal fluid in multiple sclerosis and other neurological diseases,” PLoS One, 15, No. 5, e0233519 (2020), https://doi.org/10.1371/journal.pone.0233519.
S. Modvig, M. Degn, H. Roed, et al., “Cerebrospinal fluid levels of chitinase 3-like 1 and neurofilament light chain predict multiple sclerosis development and disability after optic neuritis,” Mult. Scler., 21, No. 14, 1761–1770 (2015), https://doi.org/10.1177/1352458515574148.
F. Baldacci, S. Lista, G. Palermo, et al., “The neuroinflammatory biomarker YKL-40 for neurodegenerative diseases: advances in development,” Expert Rev. Proteomics, 16, No. 7, 593–600 (2019), https://doi.org/10.1080/14789450.2019.1628643.
M. Khalil and J. Salzer, “CSF neurofilament light,” Neurology, 87, No. 11, 1068 (2016), https://doi.org/10.1212/WNL.0000000000003107.
D. L. Dong, Z. S. Xu, M. R. Chevrier, et al., “Glycosylation of mammalian neurofilaments. Localization of multiple O-linked N-acetylglucosamine moieties on neurofilament polypeptides L and M,” J. Biol. Chem., 268, No. 22, 16,679–16,687 (1993).
M. Khalil, C. E. Teunissen, M. Otto, et al., “Neurofilaments as biomarkers in neurological disorders,” Nat. Rev. Neurol., 14, No. 10, 577–589 (2018), https://doi.org/10.1038/s41582-018-0058-z.
C. Barro, P. Benkert, G. Disanto, et al., “Serum neurofilament as a predictor of disease worsening and Brain and spinal cord atrophy in multiple sclerosis,” Brain, 141, No. 8, 2382–2391 (2018), https://doi.org/10.1093/brain/awy154.
O. Ciccarelli, “Multiple sclerosis in 2018: new therapies and biomarkers,” Lancet Neurol., 18, No. 1, 10–12 (2019), https://doi.org/10.1016/S1474-4422(18)30455-1.
J. Kuhle, G. Disanto, J. Lorscheider, et al., “Fingolimod and CSF neurofilament light chain levels in relapsing-remitting multiple sclerosis,” Neurology, 84, No. 16, 1639–1643 (2015), https://doi.org/10.1212/WNL.0000000000001491.
L. Gaetani, F. Boscaro, G. Pieraccini, et al., “Host and microbial tryptophan metabolic profiling in multiple sclerosis,” Front. Immunol., 11 (2020), https://doi.org/10.3389/fimmu.2020.00157.
C. K. Lim, A. Bilgin, D. B. Lovejoy, et al., “Kynurenine pathway metabolomics predicts and provides mechanistic insight into multiple sclerosis progression,” Sci. Rep., 7, 41473 (2017), https://doi.org/10.1038/srep41473.
P. Ak and B. Se, “The role of the gut microbiome in multiple sclerosis risk and progression: Towards characterization of the ‘MS microbiome’,” Neurotherapeutics, 15 (2018), https://doi.org/10.1007/s13311-017-0587-y.
L. Dennison, M. Brown, S. Kirby, and I. Galea, “Do people with multiple sclerosis want to know their prognosis? A UK nationwide study,” PLoS One, 13, No. 2 (2018), https://doi.org/10.1371/journal.pone.0193407.
R. Magliozzi, O. W. Howell, R. Nicholas, et al., “Inflammatory intrathecal profiles and cortical damage in multiple sclerosis,” Ann. Neurol., 83, No. 4, 739–755 (2018), https://doi.org/10.1002/ana.25197.
D. A. Häring, H. Kropshofer, L. Kappos, et al., “Long-term prognostic value of longitudinal measurements of blood neurofilament levels,” Neurol. Neuroimmunol. Neuroinflamm., 7, No. 5, e856 (2020), https://doi.org/10.1212/NXI.0000000000000856.
Challenges in Design, Analysis and Reporting of Prognostic and Predictive Marker Research – from Single Studies to an EBM Based Assessment, Accessed March 3, 2021, https://methods.cochrane.org/sites/methods.cochrane.org.prognosis/files/public/uploads/program+abstracts.pdf.
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Nevrologii i Psikhiatrii imeni S. S. Korsakova, Vol. 122, No. 2, pp. 22–27, February, 2022.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alifirova, V.M., Kamenskikh, E.M., Koroleva, E.S. et al. Prognostic Markers in Multiple Sclerosis. Neurosci Behav Physi 52, 865–870 (2022). https://doi.org/10.1007/s11055-022-01310-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-022-01310-7