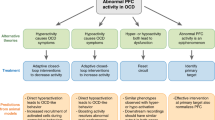
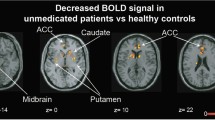
Impairment of the cerebral error detection mechanism is believed to be one of the causes of obsessive-compulsive disorder (OCD) and the anterior cingulate cortex (ACC) is the key element supporting this mechanism. However, neuroimaging data on the functional activity of the ACC in patients with OCD in the state of operational rest* and during activity are extremely diverse. An earlier explanation of this fact was the hypothesis that changes in ACC activity depend on the nature of the OCD present. With the aim of testing this hypothesis experimentally, the present studies performed combined PET-fMRI studies of the functional activity of the ACC in patients with OCD in the state of operational rest and on performance of activity presumptively involving the error detection mechanism. This activity was modeled using a Go/NoGo test with two tasks with different levels of difficulty. The ACC in patients in the state of operational rest showed glucose hypermetabolism, which decreased with increases in disease duration. The functional activity of the ACC during performance of actions was decreased in patients with OCD as compared with a group of healthy subjects. In addition, ACC activity on performance of the simpler task was found to increase with the course of illness; conversely, performance of the more difficult task decreased activity. Thus, the data obtained here support the hypothesis. Glucose hypermetabolism in the state of operational rest at the initial stages of illness was replaced by hypometabolism, probably because the ACC stopped carrying out its normal functions, which were compensated for by redistribution of the function among other relatively intact structures. This may lead to distortion of the functional specialization of the ACC, where the functional activity of the ACC in conditions of enhanced cognitive load decreased with increases in the duration of illness, while activity increased in conditions of relatively simple cognitive loading.
Similar content being viewed by others
References
Bechtereva, N. P. and Gretchin, V. B., “Physiological foundations of mental activity,” Int. Rev. Neurobiol., 11, 329–352 (1968).
Bechtereva, N. P., Neurophysiological Aspects of Human Mental Activity, Meditsina, Leningrad (1971).
Bechtereva, N. P., Shemyakina, N. V., Starchenko, M. G., et al., “Error detectors mechanisms of the brain: background and prospects,” Int. J. Psychophysiol., 58, No. 2–3, 227–234 (2005).
Brown, L. T., Mikell, C. B., Youngerman, B. E., et al., “Dorsal anterior cingulotomy and anterior capsulotomy for severe, refractory obsessive-compulsive disorder: a systematic review of observational studies,” J. Neurosurg., 124, 77–89 (2016).
Busatto, G. F., Buchpiguel, C. A., Zamignani, D. R., et al., “Regional cerebral blood flow abnormalities in early-onset obsessive-compulsive disorder: An exploratory SPECT study,” J. Am. Acad. Child. Adolesc. Psychiatry, 40, No. 3, 347–54 (2001).
Carter, C. S., Braver, T. S., Barch, D. M., et al., “Anterior cingulate cortex, error detection, and the online monitoring of performance,” Science, 280, No. 5364, 747–749 (1998).
Dehaene, S., Posner, M. I., and Tucker, D. M., “Localization of a neural system for error detection and compensation,” Psychol. Sci., 5, No. 5, 303–305 (1994).
Dougherty, D. D., Baer, L., Cosgrove, G. R., et al., “Prospective long-term follow-up of 44 patients who received cingulotomy for treatment-refractory obsessive-compulsive disorder,” Am. J. Psychiatry, 159, No. 2, 269–75 (2002).
Endrass, T., Klawohn, J., Schuster, F., and Kathmann, N., “Overactive performance monitoring in obsessive-compulsive disorder: ERP evidence from correct and erroneous reactions,” Neuropsychologia, 46, No. 7, 1877–1887 (2008).
Evdokimov, S. A., Pronina, M. V., Polyakova, G. Yu., et al., “Independent components analysis of event-related potentials in patients with diagnoses of schizophrenia, obsessive-compulsive disorder, and depressive disorder,” Fiz. Vyssh. Nerv. Deyat., 64, No. 5, 500–509 (2014).
Fitzgerald, K. D., Stern, E. R., Angstadt, M., et al., “Altered function and connectivity of the medial frontal cortex in pediatric obsessive-compulsive disorder,” Biol. Psychol., 68, No. 11, 1039–1047 (2010).
Fitzgerald, K. D., Welsh, R. C., Gehring, W. J., et al., “Error-related hyperactivity of the anterior cingulate cortex in obsessive-compulsive disorder,” Biol. Psychiatry, 57, No. 3, 287–294 (2005).
Friston, K. J., Ashburner, J. T., Kiebel, S. J., et al., Statistical Parametric Mapping: The Analysis of Functional Brain Images, Academic Press, London (2006), p. 656.
Gehring, W. J., Himle, J., and Nisenson, L. G., “Action-monitoring dysfunction in obsessive-compulsive disorder,” Psychol. Sci., 11, No. 1, 1–6 (2000).
Hajcak, G. and Simons, R. F., “Error-related brain activity in obsessivecompulsive undergraduates,” Psychiatry Res., 110, No. 1, 63–72 (2002).
Holte, S., Eriksson, L., and Dahlbom, M., “A preliminary evaluation of the Scanditronix PC2048-15B brain scanner,” Eur. J. Nucl. Med., 15, No. 11, 719–721 (1989).
Huey, E. D., Zahn, R., Krueger, F., et al., “A psychological and neuroanatomical model of obsessive-compulsive disorder,” J. Neuropsych. Clin. Neurosci., 20, No. 4, 390–408 (2008).
Jenike, M., Baer, L., Ballantine, H. T., et al., “Cingulotomy for refractory obsessive-compulsive disorder: A long-term follow-up of 33 patients,” Arch. Gen. Psychiatry, 48, 548–555 (1991).
Johnstone, T., Ores Walsh, K. S., Greischar, L. L., et al., “Motion correction and the use of motion covariates in multiple-subject fMRI analysis,” Hum. Brain Mapp., 27, No. 10, 779–788 (2006).
Jung, H. H., Kim, C. H., Chang, J. H., et al., “Bilateral anterior cingulotomy for refractory obsessive-compulsive disorder: Long-term follow- up results,” Stereotact. Funct. Neurosurg., 84, 184–189 (2006).
Kang, D. H., Jang, J. H., Han, J. Y., et al., “Neural correlates of altered response inhibition and dysfunctional connectivity at rest in obsessive- compulsive disorder,” Prog. Neuropsychopharmacol. Biol. Psychiatry, 40, 340–346 (2012).
Kireev, M. V., Korotkov, A. D., Polyakov, Yu. I., et al., “PET studies of the functional state of the brain in intrusive states,” Profi lakt. Klin. Med., 40, No. 3, 245–248 (2011a).
Kireev, M. V., Korotkov, A. D., Polyakov, Yu. I., et al., “The cerebral error detection mechanism – a PET study,” Ros. Fiziol. Zh., 97, No. 10, 1060–1065 (2011b).
Kireev, M. V., Medvedeva, N. S., Korotkov, A. D., et al., “Pathology of the anterior cingulate gyrus in obsessive-compulsive disorders,” Fiziol. Cheloveka, 39, No. 1, 54–57 (2013).
Kireev, M. V., Medvedeva, N. S., Masharipov, R. S., et al., “Spatial differentiation of sensory discrimination and comparison in working memory in GoNogo task: An fMRI study,” Int. J. Psychophysiol., 108, 101 (2016).
Kireev, M. V., Systematic Organization of the Brain in Supporting Targeted Behavior: Doct. Dissert. in Biol. Sci., 03.00.13, St. Petersburg (2017).
Maltby, N., Tolin, D. F., Worhunsky, et al., “Dysfunctional action monitoring hyperactivates frontal-striatal circuits in obsessive-compulsive disorder: An event-related fMRI study,” NeuroImage, 24, No. 2, 495–503 (2005).
McGovern, R. A. and Sheth, S. A., “Role of the dorsal anterior cingulate cortex in obsessive-compulsive disorder: Converging evidence from cognitive neuroscience and psychiatric neurosurgery,” J. Neurosurg., 126, No. 1, 132–147 (2017).
Medvedev, S. V., Anichkov, A. D., and Polyakov, Yu. I., “Physiological mechanisms of the effectiveness of stereotaxic bilateral cingulotomy in the treatment of refractory mental dependence in drug addiction,” Fiziol. Cheloveka, 29, No. 4, 117–123 (2003).
Medvedev, S. V., Kireev, M. V., and Korotkov, A. D., “Functional MRI and PET in clinical practice – General principles and limitations in mapping brain functions,” Luch. Diag. Ter., 3, No. 3, 20–26 (2012).
Millet, B., Dondaine, T., Reymann, J. M., et al., “Obsessive compulsive- disorder networks: Positron emission tomography and neuropsychology provide new insights,” PLoS One, 8, 1, e53241 (2013).
Nabeyama, M., Nakagawa, A., Yoshiura, T., et al., “Functional MRI study of brain activation alterations in patients with obsessive-compulsive disorder after symptom improvement,” Psychiatry Res., 163, No. 3, 236–247 (2008).
Nakao, T., Nakagawa, A., Yoshiura, T., et al., “A functional MRI comparison of patients with obsessive-compulsive disorder and normal controls during a Chinese character Stroop task,” Psychiatry Res., 139, No. 2, 101–114 (2005).
Oldfield, R. C., “The assessment and analysis of handedness: The Edinburgh inventory,” Neuropsychologia, 9, 97–113 (1971).
Page, L., Rubia, K., Deeley, Q., et al., “A functional magnetic resonance imaging study of inhibitory control in obsessive-compulsive disorder,” Psychiatry Res., 174, No. 3, 202–209 (2009).
Perani, D., Colombo, C., Bressi, S., et al., “[18F]-FDG PET study in obsessive-compulsive disorder. A clinical/metabolic correlation study after treatment,” Br. J. Psychiatr., 166, 244–250 (1995).
Pitman, R. K., “A cybernetic model of obsessive-compulsive psychopathology,” Compr. Psychiatry., 28, No. 4, 334–343 (1987).
Rubia, K., Cubillo, A., Smith, A. B., et al., “Disorder-specifi c dysfunction in right inferior prefrontal cortex during two inhibition tasks in boys with attention-defi cit hyperactivity disorder compared to boys with obsessive-compulsive disorder,” Hum. Brain Mapp., 31, No. 2, 287–299 (2010).
Rubia, K., Cubillo, A., Woolley, J., et al., “Disorder-specifi c dysfunctions in patients with attention-defi cit/hyperactivity disorder compared to patients with obsessive-compulsive disorder during interference inhibition and attention allocation,” Hum. Brain Mapp., 32, No. 4, 601–611 (2011).
Schlosser, R. G., Wagner, G., Schachtzabel, C., et al., “Fronto-cingulate effective connectivity in obsessive-compulsive disorder: A study with fMRI and dynamic causal modeling,” Hum. Brain Mapp., 31, No. 12, 1834–1850 (2010).
Schwartz, J. M., “A role for volition and attention in the generation of new brain circuitry,” J. Consc. Stud., 6, No. 8–9, 115–142 (1999).
Sheth, A. S., Neal, J., Tangherlini, F., et al., “Limbic system surgery for treatment-refractory obsessive-compulsive disorder: A prospective long-term follow-up of 64 patients,” J. Neurosurg., 118, 491–497 (2013).
Swedo, S. E., Schapiro, M. B., Grady, C. L., et al., “Cerebral glucose metabolism in childhood-onset obsessive-compulsive disorder,” Arch. Gen. Psych., 46, 518–523 (1989).
Ukhtomskii, A. A., “Physiological rest and lability as biological factors,” Uchen. Zap. Leningrad. Gos. Univ., 17, No. 3, 213–226 (1937).
Ursu, S., Stenger, V. A., Shear, M. K., et al., “Overactive action monitoring in obsessive-compulsive disorder: evidence from functional magnetic resonance imaging,” Psychol. Sci., 14, No. 4, 347–353 (2003).
van Laere, K., Nuttin, B., Gabriels, L., et al., “Metabolic imaging of anterior capsular stimulation in refractory obsessive-compulsive disorder: A key role for the subgenual anterior cingulate and ventral striatum,” J. Nucl. Med., 47, 740–747 (2006).
van Veen, V. and Carter, C. S., “The anterior cingulate as a conflict monitor: fMRI and ERP studies,” Physiol. Behav., 77, No. 4–5, 477–482 (2002).
Yeung, N., “Conflict monitoring and cognitive control,” in: The Oxford Handbook of Cognitive Neuroscience, Vol. 2, The Cutting Edges,
Ochsner, K. N. and Kosslyn, S. (eds), Oxford Univ. Press, (2013), pp. 275–299.
Yucel, M., Harrison, B. J., Wood, S. J., et al., “Functional and biochemical alterations of the medial frontal cortex in obsessive-compulsive disorder,” Arch. Gen. Psych., 64, No. 8, 946–955 (2007).
Zuo, C., Ma, Y., Sun, B., et al., “Metabolic imaging of bilateral anterior capsulotomy in refractory obsessive-compulsive disorder: An FDG PET study,” J. Cereb. Blood Flow Metab., 33, No. 6, 880–887 (2013).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Vysshei Nervnoi Deyatel’nosti imeni I. P. Pavlova, Vol., 69, No. 2, pp. 164–174,March–April, 2019.
Rights and permissions
About this article
Cite this article
Medvedeva, N.S., Masharipov, R.S., Korotkov, A.D. et al. Dynamics of Activity in the Anterior Cingulate Cortex on Development of Obsessive-Compulsive Disorder: a Combined PET and FMRI Study. Neurosci Behav Physi 50, 298–305 (2020). https://doi.org/10.1007/s11055-020-00901-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-020-00901-6