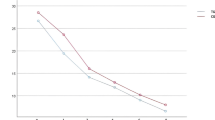
Valdoxan at a dose of 25 mg per day for three months was used in 40 patients aged 55–85 years with post-stroke depression. Patients’ status was assessed clinically and in terms of a series of scales (Hamilton, MMSE, Tinnetti, etc.). High antidepressant efficacy and good tolerance were demonstrated. On the background of stabilization of the emotional background, patients showed improvements in motor and cognitive functions.
Similar content being viewed by others
References
B. A. Volel, “Valdoxan (agomelatine): an innovatory mechanism of action,” Psikhiatr. Psikhofarmakoter., 3, 35–39 (2008).
E. I. Gusev, A. B. Gekht, A. N. Bogolepova, and I. B. Sorokina, “Characteristics of depressive syndrome in patients with ischemic stroke,” Zh. Nevrol. Psikhiat., Stroke Suppl., 3, 28–31 (2001).
E. I. Gusev and A. N. Bogolepova, “Depressive disorders in stroke patients,” Zh. Nevrol. Psikhiat., Stroke Suppl., 22, 10–16 (2008).
S. V. Ivanov, “Valdoxan (agomelatine) in the treatment of moderate and severe nonpsychotic depression in out-patient and hospital practice (results of the Russian Multicenter Study CHRONOS),” Psikhiatr. Psikhofarmakoter., 6, 14–17 (2009).
“A set of measures for the prophylaxis, diagnosis, and treatment of patients with cardiovascular diseases in the Russian Federation. Federal Program [in Russian],” in: Proc. 2nd Russ. Int. Congr. Cerebrovascular Pathology and Stroke, Vol. 7, p. 20 (2007).
V. E. Medvedev, “Perspectives in the use of melatoninergic agents in the treatment of depression in patients with cardiovascular diseases,” Psikhiatr. Psikhofarmakoter., 3, 17–22 (2010).
V. E. Medvedev and A. V. Epifanov, “An innovatory method for the treatment of depression in patients with ischemic heart disease,” Oboz. Psikhiatr. Med. Psikhol. im. Bekhtereva, 3, 31–36 (2010).
V. I. Skvortsova, “Decreases in the morbidity, lethality, and disability due to stroke in the Russian Federation,” Zh. Nevrol. Psikhiat., Stroke Suppl., Spec. Iss., Proc. 2nd Russ. Int. Congr. Cerebrovascular Pathology and Stroke, 25–27 (2007).
A. B. Smulevich and S. V. Ivanov, “Depression and biological rhythms: the CIRCADIAN-1 questionnaire study,” Psikhiatr. Psikhofarmakoter., 6, 4–8 (2008).
L. I. Syromyatnikova, T. A. Spigina, and V. V. Shestakov, “Circadian rhythm and depression in cardiological patients,” Psikhich. Rasstr. Obshch. Med., 1, 19–24 (2010).
A. Berg, H. Palomäki, M. Lehtihalmes, et al., “Poststroke depression: an 18-month follow-up,” Stroke, 34, 138–143 (2003).
A. Berg, J. Lonnqvist, H. Palomaki, and M. Kaste, “Assessment of depression after stroke. A comparison of different screening instruments,” Stroke, 40, 523–529 (2009).
M. Bourin, E. Mocaër, and R. Porsholt, “Antidepressant-like activity of S20098 (agomelatine) in the forced swimming test in rodents: involvement of melatonin and serotonin receptors,” J. Psych. Neurosci., 29, No. 2, 126–133 (2004).
D. Eser, T. C. Baghai, and H.-J. Möller, “Agomelatine: the evidence for its place in the treatment of depression,” Core Evidence, 3, 171–179 (2009).
G. M. Goodwin, F. Rouillon, and R. Emsley, “Long-term treatment with agomelatine: prevention of relapse in patients with major depressive disorder over 10 months (abstract),” 21st European College of Neuropsychopharmacology Congress, Aug. 30 – Sept. 3, 2008, Barcelona, Spain, Eur. Neuropsychopharmacol., 18, 338–339 (2008).
C. Haacke, A. Althous, A. Spottke, et al., “Long-term outcome after stroke evaluating health-related quality of life using utility measurements,” Stroke, 37, 193–198 (2006).
M. J. Joliat, M. E. Schmidt, M. Fava, et al., “Long-term treatment outcomes of depression with associated anxiety – efficacy of continuation treatment with fluoxetine,” J. Clin. Psychiatry, 65, 373–378 (2004).
B. S. Jonas and J. F. Lando, “Negative affect as a prospective risk factor for hypertension,” Psychosom. Med., 62, 188–196 (2000).
M. Lader, “Pharmacotherapy of mood disorders and treatment discontinuation,” Drugs, 67, 1657–1663 (2007).
T. Lindén, C. Blomstrand, and I. Skoog, “Depressive disorders after 20 months in elderly stroke patients: a case-controlled study,” Stroke, 38, 1860–1863 (2007).
R. S. K. Lo, J. O. Y. Cheng, E. M. C. Wong, et al., “Handicap and its determinants of change in stroke survivors: one-year follow-up study,” Stroke, 39, 148–153 (2008).
H. Loo, A. Hale, and H. D’haenen, “Determination of the Valdoxan dose, a melatoninergic agonist and selective 5-HT2c antagonist, in the treatment of major depressive disorder: a double-blind, placebocontrolled study with dose ranging (abstract),” Psikhiatr. Psikhofarmakoter., 2, 52–58 (2009).
S. D. Mendelson, “The current status of the platelet 5-HT receptor in depression,” J. Affect. Disord., 57, 13–24 (2002).
M. J. Millan, A. Gobert, F. Lejeune, et al., “The novel melatonin agonist agomelatine (S20098) is an antagonist at 5-hydroxytryptamine 2C receptors, blockade of which enhances the activity of frontocortical dopaminergic and adrenergic pathways,” J. Pharmacol. Exp. Ther., 306, 954–964 (2003).
S. A. Montgomery, S. H. Kennedy, G. D. Burrows, et al., “Absence of discontinuation symptoms with agomelatine and occurrence of discontinuation symptoms with paroxetine: a randomized, doubleblind, placebo-controlled discontinuation study,” Int. Clin. Psychopharmacol., 19, 271–280 (2004).
S. A. Montgomery, J.-P. Oli, and S. H. Kennedy, “Antidepressant efficacy of agomelatine in major depressive disorder: meta-analysis of three pivotal studies,” Eur. Neuropsychopharmacol., 16, Suppl. 4, 321 (2006).
V. Murray, M. Von Arbin, A. Bartfai, et al., “Double-blind comparison of sertraline and placebo in stroke patients with minor depression and less severe major depression,” J. Clin. Psychiatry, 66, 708–716 (2005).
D. L. Musselman, E. Betan, H. Larsen, and L. S. Phillips, “Relationship of depression to diabetes mellitus types 1 and 2: epidemiology, biology, and treatment,” Biol. Psychiatry, 54, 317–329 (2003).
K. Narushima, J. T. Kosier, and R. G. Robinson, “A reappraisal of poststroke depression, intra- and inter-hemispheric lesion location using meta-analysis,” J. Neuropsych. Clin. Neurosci., 15, 422–430 (2003).
J. H. Pan, X. Y. Song, S. Y. Lee, et al., “Longitudinal analysis of quality of life for stroke survivors using latent curve models,” Stroke, 39, 2795–2802 (2008).
S. L. Paul, H. M. Dewey, J. W. Sturm, et al., “Prevalence of depression and use of antidepressant medication at 5 years poststroke in the North East Melbourne Stroke Incidence Study,” Stroke, 37, 2854–2855 (2006).
M. A. Quera Salva, B. Vanier, J. Laredo, et al., “Major depressive disorder, sleep EEG and agomelatine: an open-label study,” Int. J. Neuropsychopharmacol., 10, 691–696 (2007).
R. G. Ronbins, G. Spalleta, R. E. Jorge, et al., “Decreased heart rate variability is associated with poststroke depression,” Am. J. Geriatr. Psychiatry, 16, No. 11, 867–873 (2008).
M. Santos, G. Gold, E. Kowari, et al., “Differential impact of lacunes and microvascular lesions on poststroke depression,” Stroke, 40, 3557–3562 (2009).
J. W. Sturm, G. A. Donnan, H. M. Dewey, et al., “Determinants of handicap after stroke: the North East Melbourne Stroke Incidence Study (NEMESIS),” Stroke, 35, 715–720 (2004).
R. Vataja, A.Leppävuori, T. Pohjasvaara, et al., “Poststroke depression and lesion location revisited,” J. Neuropsych. Clin. Neurosci., 16, 156–162 (2004).
S. Wassertheil-Smoller, W. B. Applegate, K. Berge, et al., “Change in depression as a precursor of cardiovascular events. SHEP Cooperative Research Group (Systolic Hypertension in the Elderly),” Arch. Int. Med., 5, 553–561 (1996).
E. M. Whyte, B. H. Mulsant, J. Vanderbilt, et al., “Depression after stroke: a prospective epidemiology study,” J. Am. Geriatr. Soc., 52, 774–778 (2004).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Nevrologii i Psikhiatrii imeni S. S. Korsakova, Vol. 111, No. 4, pp. 42–46, April, 2011.
Rights and permissions
About this article
Cite this article
Bogolepova, A.N., Chukanova, E.I., Smirnova, M.Y. et al. Experience in the Use of Valdoxan in the Treatment of Post-Stroke Depression. Neurosci Behav Physi 42, 556–560 (2012). https://doi.org/10.1007/s11055-012-9600-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-012-9600-4