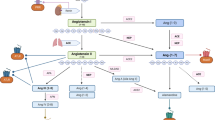
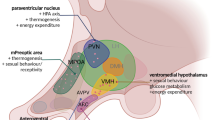
In male rats, repeated but not single exposures to stress increased the conversion of corticosterone (CS) to 11-dehydrocorticosterone (11-DHCS), particularly on the background of administration of dehydroepiandrosterone sulfate (DHEAS). Naltrexone given 20 min before DHEAS at a dose of 0.1 mg/kg, at which it selectively blocks μ opioid receptors, prevented this effect of DHEAS, which is evidence that it is mediated by μ opioid receptors. This action of DHEAS involved endogenous ACTH and was thus mediated by central regulatory mechanisms. Our results, along with published data, lead to the first proposed scheme for the physiological regulation of the interconversion of CS and 11-DHCS in conditions of repeated stress with the involvement of DHEAS and μ opioid receptors.
Similar content being viewed by others
References
T. A. Obut, M. V. Ovsyukova, and O. P. Cherkasova, “Effects of dehydroepiandrosterone sulfate on stress reactivity: a μ opiate mechanism,” Ros. Fiziol. Zh. im. I. M. Sechenova, 88, No. 12, 1578–1584 (2002).
T. A. Obut, M. V. Ovsyukova, and O. P. Cherkasova, “The stress reactivity-limiting effect of dehydroepiandrosterone sulfate and its mechanism,” Byull. Éksperim. Biol. Med., 135, No. 3, 269–271 (2003).
P. O. Cover and J. C. Buckingham, “Effects of selective opioidreceptor blockade on the hypothalamo-pituitary-adrenocortical responses to surgical trauma in the rat,” J. Endocrinol., 121, 213–220 (1989).
M. Homma, T. Onodera, M. Hirabatake, K. Oka, M. Kanazawa, T. Miwa, and T. Hayashi, “Activation of 11 beta-hydroxysteroid dehydrogenase by dehydroepiandrosterone sulfate as an anti-hypertensive agent in spontaneously hypertensive rats,” J. Pharm. Pharmacol., 50, 1139–1145 (1998).
S. Kapas, A. Purbrick, and J. P. Hinson, “Action of opioid peptides on the rat adrenal cortex: stimulation of steroid secretion through a specific mu opioid receptor,” J. Endocrinol., 144, 503–510 (1995).
K. Leung and A. Munck, “Peripheral actions of glucocorticoids,” Ann. Rev. Physiol., 37, 245–272 (1975).
C. Monder and V. Lakshmi, “Corticosteroid 11 beta-dehydrogenase of rat tissues: immunological studies,” Endocrinology, 126, 2435–2443 (1990).
D. J. Morris, A. S. Brem, R. Ge, P. H. Jellinck, R. R. Sasai, and M. P. Hardy, “The functional roles of 11 beta-HSDl: vascular tissue, testis and brain,” Mol. Cell. Endocrinol., 203, 1–12 (2003).
K. H. Nwe, A. W. Norhazlina, A. Hamid, P. B. Morat, and B. A. Khalid, “In vivo effects of stress, ACTH and corticosterone on testicular 11 beta-hydroxysteroid dehydrogenase oxidative activity in rats and the possible mechanism of actions,” Exp. Clin. Endocrinol. Diabetes, 108, 369–377 (2000).
J. R. Seckl, “11Beta-hydroxysteroid dehydrogenase in the brain: a novel regulator of glucocorticoid action?” Front. Neuroendocrinol., 18, 49–99 (1997).
M. Shimojo, J. Conodon, C. B. Whorwood, and P. M. Stewart, “Adrenal 11 beta-hydroxysteroid dehydrogenase,” Endocr. Res., 22, 771–780 (1996).
B. R. Walker, J. C. Campbell, B. C. Williams, and C. R. Edwards, “Tissue-specific distribution of the NAD(+)-dependent isoform of 11 beta-hydroxysteroid dehydrogenase,” Endocrinology, 131, 970–972 (1992).
P. C. White, T. Mure, and A. K. Agarwal, “11β-Hydroxysteroid dehydrogenase and the syndrome of apparent mineralocorticoid excess,” Endocr. Rev., 18, 135–156 (1997).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Rossiiskii Fiziologicheskii Zhurnal imeni I. M. Sechenova, Vol. 94, No. 8, pp. 945–951, August, 2008.
Rights and permissions
About this article
Cite this article
Obut, T.A., Ovsyukova, M.V., Dement’eva, T.Y. et al. Effects of Dehydroepiandrosterone Sulfate on the Conversion of Corticosterone into 11-Dehydrocorticosterone in Stress: A Regulatory Scheme. Neurosci Behav Physi 39, 695–699 (2009). https://doi.org/10.1007/s11055-009-9179-6
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-009-9179-6