Abstract
Objectives
Skin lesions, uncommon in US cases (<10%), occur in 38–85% of cases reported from Latin America. Although these differences may reflect reporting bias, delayed diagnosis, or differences in host immune response among different ethnic groups, they also could result from genetic differences changing the pathobiology of the organism. It is possible that genetic differences among strains of H. capsulatum may influence the pathogenesis and clinical manifestations of histoplasmosis.
Methods
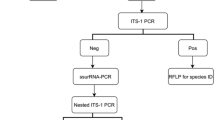
We examined the clinical features of patients with mucocutaneous manifestations of histoplasmosis and performed genetic analysis based on nucleotide sequence variations in the internal transcribed spacer regions of rRNA genes of H. capsulatum isolates of patients. Two pairs of PCR primers were designed to develop and amplify the ITS regions of H. capsulatum, 5′-TACCCGGCCACCCTTGTCTA-3′ and 5′-AGCGGGTGGCAAAGCCC-3′. These primers were based on the ITS sequence of Ajellomyces capsulatus, the ascomycetous teleomorph form of H. capsulatum, deposited in the GenBank (accession number U18363). Eight patients attending a tertiary-care hospital in southern Brazil were enrolled into the study. All case patients had skin cultures growing H. capsulatum at the mycology laboratory.
Results
Six of eight (75%) patients were HIV-positive and presented involvement of multiples organs by H. capsulatum. Two HIV-negative patients did not present evidence of involvement of other organs besides mucosa and skin. ITS sequencing of a DNA H. capsulatum fragment of 485-bp from isolates of 8 patients revealed two distinct strains. The 2 distinct fragments (Hc1, Hc2) differed from each other at 7 positions in the ITS regions. They were identical to strains of H. capsulatum isolated in patients from Colombia and Argentina, but different from strains isolated in US. Hc1 and Hc2 were isolated in 5 patients and 3 patients, respectively, with mucocutaneous manifestations of histoplasmosis. Both Hc1 and Hc2 strains were isolated in HIV-infected and non-HIV-infected patients.
Conclusions
Mucocutaneous manifestations of histoplasmosis, which are frequently seen in Brazilian patients were caused by 2 specific strains in our institution. Those strains have been isolated in patients with these particular clinical features of histoplasmosis in Latin America. Our study suggests that unique pathogenic characteristics among the Latin American species of H. capsulatum might explain its increased dermatotropism.


Similar content being viewed by others
References
Wheat LJ, Kauffman CA. Histoplasmosis. Infect Dis Clin North Am. 2003;17:1–19. doi:10.1016/S0891-5520(02)00039-9.
Murillo J, Castro KG. HIV infection and AIDS in Latin America. Infect Dis Clin North Am. 1994;8:1–11.
Wheat LJ, Connolly-Stringfield PA, Baker RL, et al. Disseminated histoplasmosis in the acquired immune deficiency syndrome: clinical findings, diagnosis and treatment, and review of the literature. Medicine (Baltimore). 1990;69:361–74.
Wheat L. Histoplasmosis in the acquired immunodeficiency syndrome. Curr Top Med Mycol. 1996;7:7–18.
Machado AA, Coelho IC, Roselino AMF, et al. Histoplasmosis in individuals with acquired immunodeficiency syndrome (AIDS): report of six cases with cutaneous-mucosal involvement. Mycopathologia. 1991;115:13–8. doi:10.1007/BF00436416.
Corti ME, Cendoya CA, Soto I, et al. Disseminated histoplasmosis and AIDS: clinical aspects and diagnostic methods for early detection. AIDS Patient Care STDS. 2000;14:149–54.
Karimi K, Wheat JL, Connoly P, et al. Differences in Histoplasmosis in patients with acquired immunodeficiency syndrome in the United States and Brazil. J Infect Dis. 2002;186:1655–60. doi:10.1086/345724.
Couppié P, Clyti E, Nacher M, et al. Acquired immunodeficiency syndrome-related oral and/or cutaneous histoplasmosis: a descriptive and comparative study of 21 cases in French Guiana. Int J Dermatol. 2002;41:571–6. doi:10.1046/j.1365-4362.2002.01590.x.
Ramdial PK, Mosam A, Diova NC, et al. Disseminated histoplasmosis in patients infected with human immunodeficiency virus. J Cutan Pathol. 2002;29:215–25. doi:10.1034/j.1600-0560.2002.290404.x.
Thompson GR, La Valle CE, Everett ED. Unusual manifestations of histoplasmosis. Diagn Microbiol Infect Dis. 2004;50:33–41. doi:10.1016/j.diagmicrobio.2004.04.020.
Durkin MM, Connolly PA, Karimi K, Wheat E, Schnizlein-Bick C, Allen SD, et al. Pathogenic differences between North American and Latin American strains of Histoplasma capsulatum var. capsulatum in experimentally infected mice. J Clin Microbiol. 2004;42:4370–3. doi:10.1128/JCM.42.9.4370-4373.2004.
Jiang B, Bartlett MS, Allen SD, Smith JW, Wheat LJ, Connolly PA, et al. Typing of Histoplasma capsulatum isolates based on nucleotide sequence variation in the internal transcribed spacer regions of rRNA genes. J Clin Microbiol. 2000;38:241–5.
Cunha VS, Zampese MS, Aquino VR, Cestari TF, Goldani LZ. Mucocutaneous manifestations of disseminated histoplasmosis in patients with acquired immunodeficiency syndrome: particular aspects in a Latin-American population. Clin Exp Dermatol. 2007;32:250–5. doi:10.1111/j.1365-2230.2007.02392.x.
Kostman JR, Edlind TD, LiPuma JJ, Stull TL. Molecular epidemiology of Pseudomonas cepacia determined by polymerase chain reaction ribotyping. J Clin Microbiol. 1992;30:2084–7.
Johnson PC, Wheat LJ, Cloud GA, et al. Safety and efficacy of liposomal amphotericin B compared with conventional amphotericin B for induction therapy of histoplasmosis in patients with AIDS. Ann Intern Med. 2002;137:105–9.
Hajjeh RA, Pappas PG, Henderson H, et al. Multicenter case–control study of risk factors for histoplasmosis in Human Immunodeficiency Virus-infected persons. Clin Inf Dis. 2001;32:1215–20. doi:10.1086/319756.
Wheat LJ, Chetchotisakd P, Williams B, et al. Factors associated with severe manifestations of histoplasmosis in AIDS. Clin Inf Dis. 2000;30:877–81. doi:10.1086/313824.
Cohen PR, Grossman ME, Silvers DN. Disseminated histoplasmosis and human immunodeficiency virus infection. Int J Dermatol. 1991;30:614–22. doi:10.1111/j.1365-4362.1991.tb03484.x.
Borges AS, Ferreira MS, Silvestre MTA, et al. Histoplasmose em pacientes imunodeprimidos: estudo de 18 casos observados em Uberlândia, MG. Rev Soc Bras Med Trop. 1997;30:119–24.
Eidbo J, Sanchez RL, Tschen JA, et al. Cutaneous manifestations of histoplasmosis in the acquired immune deficiency syndrome. Am J Surg Pathol. 1993;17:110–6. doi:10.1097/00000478-199302000-00002.
Barton EN, Roberts L, Ince WE, et al. Cutaneous histoplasmosis in the acquired immune deficiency syndrome: a report of three cases from Trinidad. Trop Geogr Med. 1988;40:153–7.
Couppié P, Sobeski M, Aznar C, et al. Histoplasmosis and Acquired Immunodeficiency Syndrome: a study of prognostic factors. Clin Inf Dis. 2004;38:134–8. doi:10.1086/379770.
Gutierrez ME, Canton A, Sosa N, et al. Disseminated histoplasmosis in patients with AIDS in Panama: a review of 104 cases. Clin Inf Dis. 2005;40:1199–202. doi:10.1086/428842.
Negroni R, Helou SH, Daneri GL, et al. Interrupción de la profilaxis secundaria antifúngica en la histoplasmosis asociada al sida. Rev Iberoam Micol. 2004;21:75–8.
Severo LC, Oliveira FM, Irion K, et al. Histoplasmosis in Rio Grande do Sul, Brazil: a 21-year experience. Rev Inst Med Trop S Paulo. 2001;43:183–7. doi:10.1590/S0036-46652001000400001.
Unis G, Oliveira FM, Severo LC. Histoplasmose disseminada no Rio Grande do Sul. Rev Soc Bras Med Trop. 2004;37:463–8.
Acknowledgments
This study was supported in part by CNPq and FIPE (Hospital de Clínicas de Porto Alegre).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goldani, L.Z., Aquino, V.R., Lunardi, L.W. et al. Two Specific Strains of Histoplasma capsulatum causing Mucocutaneous Manifestations of Histoplasmosis: Preliminary Analysis of a Frequent Manifestation of Histoplasmosis in Southern Brazil. Mycopathologia 167, 181–186 (2009). https://doi.org/10.1007/s11046-008-9171-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-008-9171-7