Abstract
Background
Currently, no recognized evidence is known about the bacterial communities found within seminal vesicles (SV) of men presenting with refractory hematospermia.
Methods and results
Fifteen male patients with refractory hematospermia or anejaculation were enrolled, and 15 SV-Infection (SV-In) samples from SV with hemorrhage and/or stones, 11 SV-Control (SV-C) samples from SV with non-infection, and 14 Urine (Urine) samples from posterior urethra were obtained via transurethral seminal vesiculoscopy. Then the high-throughput 16 S rRNA gene sequencing method was performed to characterize the microbiota profile. Finally, a total of 1535 operational taxonomic units (OTUs) were found, 1295 OTUs were shared across three groups, 7 OTUs, 45 OTUs, and 48 OTUs were unique to SV-C group, SV-In group, and Urine group, respectively. The 5 top bacterial phyla (mean relative abundance) in all samples were Firmicutes (52.08%), Bacteroidetes (21.69%), Proteobacteria (12.72%), Actinobacteria (9.64%), and Fusobacteria (1.62%), the 5 top bacterial genera in all samples were Bacteroides (9.13%), Lactobacillus (5.38%), Bifidobacterium (5.35%), Faecalibacterium (5.10%), and Allobaculum (3.34%), of which Bifidobacterium had the highest level in SV-C samples and had a significant difference (P < 0.05) across all groups. Differential analysis showed genera Leuconostoc and LachnospiraceaeFCS020group were identified as biomarkers in the SV-In microbiota.
Conclusion
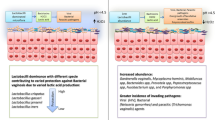
Altered microbiota composition in seminal vesicles is related to refractory hematospermia in men, and the distribution of genus Leuconostoc or LachnospiraceaeFCS020group within seminal vesicles may interact with hematospermia. This study provides clues for the diagnosis and treatment of this urologic disorder.




Similar content being viewed by others
Data availability
16 S rRNA gene sequence data for each sample have been deposited at NCBI’s Sequence Read Archive (SRA; BioProject ID: PRJNA892056).
References
Modgil V, Rai S, Ralph DJ, Muneer A (2016) An update on the diagnosis and management of ejaculatory duct obstruction. Nat Rev Urol 13(1):13–20. https://doi.org/10.1038/nrurol.2015.276
Avellino GJ, Lipshultz LI, Sigman M, Hwang K (2019) Transurethral resection of the ejaculatory ducts: etiology of obstruction and surgical treatment options. Fertil Steril 111(3):427–443. https://doi.org/10.1016/j.fertnstert.2019.01.001
Liao LG, Li YF, Zhang Y, Li K, Zhu T, Li BJ, Wang Q, Liu XD, Luo Y, Zhou B, Jiang J (2019) Etiology of 305 cases of refractory hematospermia and therapeutic options by emerging endoscopic technology. Sci Rep 9(1):5018. https://doi.org/10.1038/s41598-019-41123-2
Chen WK, Yu DD, Chen ZX, Li PF, Cai J, Liu YP, Wu ZG (2021) Transurethral seminal vesiculoscopy for intractable hematospermia: experience from 144 patients. BMC Urol 21(1):48. https://doi.org/10.1186/s12894-021-00817-4
Wang XS, Li M, Shao GF, Sun WD, Zhang XL, Xiao ZY, Ma Z, Yuan MZ, Guo LQ (2020) Real-time transrectal ultrasound-guided seminal vesiculoscopy for the treatment of patients with persistent hematospermia: a single-center, prospective, observational study. Asian J Androl 22(5):507–512. https://doi.org/10.4103/aja.aja_134_19
Ren ZJ, Yang B, Lu DL, Liu SZ, Yang LC, Wang LC, Peng ZF, Liu LR, Dong Q (2020) Transurethral resection of ejaculatory duct combined with seminal vesiculoscopy for management of persistent or recurrent hemospermia in men with ejaculatory duct obstruction. BMC Urol 20(1):34. https://doi.org/10.1186/s12894-020-00589-3
Chen R, Wang L, Sheng X, Piao SG, Nian XW, Cheng X, Zhou T, Li HZ, Liu YW, Chen GH, Zhang CL, Kong DP, Xiao GA, Lu X, Jia ZY, Liu ZY, Sun YH (2018) Transurethral seminal vesiculoscopy for recurrent hemospermia: experience from 419 cases. Asian J Androl 20(5):438–441. https://doi.org/10.4103/aja.aja_76_17
Liu B, Li J, Li P, Zhang J, Song N, Wang Z, Yin C (2014) Transurethral seminal vesiculoscopy in the diagnosis and treatment of intractable seminal vesiculitis. J Int Med Res 42(1):236–242. https://doi.org/10.1177/0300060513509472
Drury RH, King B, Herzog B, Hellstrom WJG (2021) Hematospermia Etiology, Diagnosis, Treatment, and Sexual Ramifications: A Narrative Review. Sexual medicine reviews https://doi.org/10.1016/j.sxmr.2021.07.004
Saracoglu M, Ozturk H, Duran A, Atalay S (2015) Effect of microorganisms on etiology of hematospermia. Arch Ital Urol Androl 87(1):80–82. https://doi.org/10.4081/aiua.2015.1.80
Davidson RM, Epperson LE (2018) Microbiome sequencing methods for studying Human Diseases. Methods in molecular biology. (Clifton NJ) 1706:77–90. https://doi.org/10.1007/978-1-4939-7471-9_5
Suh Y, Gandhi J, Joshi G, Lee MY, Weissbart SJ, Smith NL, Joshi G, Khan SA (2017) Etiologic classification, evaluation, and management of hematospermia. Transl Androl Urol 6(5):959–972. https://doi.org/10.21037/tau.2017.06.01
Furuya S, Masumori N, Takayanagi A (2016) Natural history of hematospermia in 189 japanese men. Int J urology: official J Japanese Urol Association 23(11):934–940. https://doi.org/10.1111/iju.13176
Shoemaker R, Kim J (2021) Urobiome: an outlook on the metagenome of urological diseases. Investig Clin Urol 62(6):611–622. https://doi.org/10.4111/icu.20210312
Ruan W, Engevik MA, Spinler JK, Versalovic J (2020) Healthy human gastrointestinal microbiome: composition and function after a Decade of Exploration. Dig Dis Sci 65(3):695–705. https://doi.org/10.1007/s10620-020-06118-4
Onywera H, Williamson AL, Cozzuto L, Bonnin S, Mbulawa ZZA, Coetzee D, Ponomarenko J, Meiring TL (2020) The penile microbiota of Black South african men: relationship with human papillomavirus and HIV infection. BMC Microbiol 20(1):78. https://doi.org/10.1186/s12866-020-01759-x
Weng SL, Chiu CM, Lin FM, Huang WC, Liang C, Yang T, Yang TL, Liu CY, Wu WY, Chang YA, Chang TH, Huang HD (2014) Bacterial communities in semen from men of infertile couples: metagenomic sequencing reveals relationships of seminal microbiota to semen quality. PLoS ONE 9(10):e110152. https://doi.org/10.1371/journal.pone.0110152
Sanders ME, Merenstein DJ, Reid G, Gibson GR, Rastall RA (2019) Probiotics and prebiotics in intestinal health and disease: from biology to the clinic. Nat Rev Gastroenterol Hepatol 16(10):605–616. https://doi.org/10.1038/s41575-019-0173-3
Tomaiuolo R, Veneruso I, Cariati F, D’Argenio V (2020) Microbiota and Human Reproduction: the case of male infertility. High Throughput 9(2). https://doi.org/10.3390/ht9020010
Ogier JC, Casalta E, Farrokh C, Saihi A (2008) Safety assessment of dairy microorganisms: the Leuconostoc genus. Int J Food Microbiol 126(3):286–290. https://doi.org/10.1016/j.ijfoodmicro.2007.08.012
Vojinovic D, Radjabzadeh D, Kurilshikov A, Amin N, Wijmenga C, Franke L, Ikram MA, Uitterlinden AG, Zhernakova A, Fu J, Kraaij R, van Duijn CM (2019) Relationship between gut microbiota and circulating metabolites in population-based cohorts. Nat Commun 10(1):5813. https://doi.org/10.1038/s41467-019-13721-1
Acknowledgements
None.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization, H.L. and L.T.; Methodology, H.L., H.H., and Y.F.; Formal Analysis, H.L., H.H., and Y.F.; Investigation, H.L.; Writing - Original Draft, H.L.; Writing - Review & Editing, X.Z., Z.X., and L.T.; Visualization, X.Z. and Z.X.; Supervision, L.T.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Beijing Chao-Yang Hospital, Capital Medical University (No. 2021-KE-482).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lei, H., Han, H., Feng, Y. et al. Altered microbiota profile in seminal vesicles of men presenting with refractory hematospermia. Mol Biol Rep 50, 2381–2389 (2023). https://doi.org/10.1007/s11033-022-08139-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-08139-w