Abstract
Background
Cholangiocarcinoma is a malignant tumor originating from bile duct epithelial cells. Since tumor metastasis is associated with poor prognosis and short-term survival of patients, there is an urgent need for alternative therapeutic approaches for CCA. Because of that reason, we aimed to investigate effect of SAHA which is known as HDAC inhibitor on extrahepatic cholangiocarcinoma cell line (TFK-1).
Methods
Cell cycle was measured by Muse Cell Analyzer. YAP, TAZ, TGF-β protein levels were determined by western-blotting method. TEAD (1–3), TIMP2 and TIMP3 genes level were determined by real-time PCR analysis.
Results
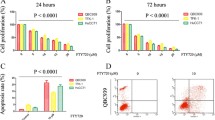
We have seen the positive effects of SAHA on the TFK-1 cell line as it reduces cell viability and arresting cells in the G0/G1 phase. We also observed the negative effects of SAHA, as it increases the expression levels of YAP, TAZ, TGF-β protein and TEAD (1–3) gene. We also found that SAHA reduced the expression levels of TIMP2 and TIMP3 in TFK-1 cells, but was not statistically significant.
Conclusions
Although observing its antiproliferative effects, these negative effects may be related to the cells being resistant to the drug or the remaining cells having a more aggressive phenotype. Therefore, we think that caution should be exercised in the use of this drug for CCA treatment.




Similar content being viewed by others
References
Esposito I, Schirmacher P (2008) Pathological aspects of cholangiocarcinoma. HPB (Oxford) 10:83–86
Trinh SX, Nguyen HT, Saimuang K, Prachayasittikul V, Chan W (2017) Metformin inhibits migration and invasion of cholangiocarcinoma. Cells Asian Pac J Cancer 18:473–477
Kanwala R, Gupta S (2012) Epigenetic modifications in cancer. Clin Genet 81:303–311
Gallinari P, Marco SD, Jones P, Pallaoro M, Steinkühler C (2007) HDACs, histone deacetylation and gene transcription: from molecular biology to cancer therapeutics. Cell Res 17:195–211
Ropero S, Esteller M (2007) The role of histone deacetylases (HDACs) in human cancer. Mol Oncol 1:19–25
Marks P, Rifkind RA, Richon VM, Breslow R, Miller T, Kelly WK (2001) Histone deacetylases and cancer: causes and therapies. Nat Rev Cancer 1:194–202
Li G, Tian Y, Zhu WG (2020) The roles of histone deacetylases and their ınhibitors in cancer therapy. Front Cell Dev Biol 8:576946
Ropero S, Esteller M (2007) The role of histone deacetylases (HDACs) in human cancer. Mol Oncol 1(1):19–25
Pant K, Peixoto E, Richard S, Gradilone SA (2020) Role of histone deacetylases in carcinogenesis: potential role in cholangiocarcinoma. Cells 9(3):780
Fouladi M (2006) Histone deacetylase inhibitors in cancer therapy. Cancer Invest 24:521–527
Suraweera A, Byrne KJO, Richard DJ (2018) Combination therapy with histone deacetylase inhibitors (HDACi) for the treatment of cancer: achieving the full therapeutic potential of HDACi. Front Oncol 8:92
Mann BS, Johnson JR, Cohen MH, Justice R, Pazdur R (2007) FDA approval summary: vorinostat for treatment of advanced primary cutaneous T-cell lymphoma. Oncologist 13:2318–2322
Kong D, Ahmad A, Bao B, Li Y, Banerjee S, Sarkar FH (2012) Histone deacetylase ınhibitors ınduce epithelial-to-mesenchymal transition in prostate cancer cells. PLoS One 7:e45045
Pan DJ (2010) The hippo signaling pathway in development and cancer. Dev Cell 19:491–505
Zhang L, Ren F, Zhang Q, Chen Y, Wang B, Jiang J (2008) The TEAD/TEF family of transcription factor Scalloped mediates Hippo signaling in organ size control. Dev Cell 14:377–387
Clevers H (2006) Wnt/beta-catenin signaling in development and disease. Cell 127:469–480
Imajo M, Miyatake K, Iimura A, Miyamoto A, Nishida E (2012) A molecular mechanism that links Hippo signalling to the inhibition of Wnt/β-catenin signalling. EMBO J 31:1109–1122
Saab S, Chang OSS, Nagaoka K, Hung MC, Yamaguchi H (2019) The potential role of YAP in Axl-mediated resistance to EGFR tyrosine kinase inhibitors. Am J Cancer Res 9:2719–2729
Hiemer SE, Szymaniak AD, Varelas X (2014) The transcriptional regulators TAZ and YAP direct transforming growth factor β-induced tumorigenic phenotypes in breast cancer cells. J Biol Chem 289:13461–13474
Massagué J (2008) TGFβ in cancer. Cell 134:215–230
Leivonen SK, Lazaridis K, Decock J, Chantry A, Edwards DR, Kähäri VM (2013) TGF-β-elicited ınduction of tissue ınhibitor of metalloproteinases (TIMP)-3 expression in fibroblasts ınvolves complex ınterplay between smad3, p38α, and ERK1/2. PLoS One 8:e57474
Barillari G (2020) The impact of matrix metalloproteinase-9 on the sequential steps of the metastatic process. Int J Mol Sci 21:4526
Başkol G, Özel M, Uçar Ç, Doğru BN, Yüksek EH, Güneş F, Başkol M (2019) SAHA modulates cell proliferation, colony forming and epithelial-mesenchymal transition in CCA cells. Turk J Biochem 44:70–77
Natarajan U, Venkatesan T, Radhakrishnan V, Samuel S, Rasappan P, Rathinavelu A (2019) Cell Cycle Arrest and Cytotoxic Effects of SAHA and RG7388 Mediated through p21WAF1/CIP1 and p27KIP1 in Cancer Cells. Medicina (Kaunas) 55:30
Sugihara T, Isomoto H, Gores G, Smoot R (2019) YAP and the Hippo pathway in cholangiocarcinoma. J Gastroenterol 54:485–491
Zanconato F, Cordenonsi M, Piccolo S (2016) YAP/TAZ at the roots of cancer. Cancer Cell 29:783–803
Kessenbrock K, Plaks V, Werb Z (2010) Matrix metalloproteinases: regulators of the tumor microenvironment. Cell 141:52–67
Li Y, Seto E (2016) HDACs and HDAC ınhibitors in cancer development and therapy. Cold Spring Harb Perspect Med 6:026831
Mottamal M, Zheng S, Huang TL, Wang G (2015) Histone deacetylase inhibitors in clinical studies as templates for new anticancer agents. Molecules 20:3898–3941
Stimson L, Wood V, Khan O, Fotheringham S, La Thangue NB (2009) HDAC inhibitor-based therapies and haematological malignancy. Ann Oncol 20:1293–1302
He J, Yao W, Wang J, Schemmer P, Yang Y, Liu Y, Qian Y, Qi W, Zhang J, Shen Q, Yang T (2016) TACC3 overexpression in cholangiocarcinoma correlates with poor prognosis and is a potential anti-cancer molecular drug target for HDAC inhibitors. Oncotarget 7:75441–75456
Fröhlich LF, Mrakovcic M, Smole C, Zatloukal K (2016) Molecular mechanism leading to SAHA-induced autophagy in tumor cells: evidence for a p53-dependent pathway. Cancer Cell Int 16:68
Shi XY, Ding W, Li TQ, Zhang YX, Zhao SC (2017) Histone deacetylase (HDAC) inhibitor, Suberoylanilide Hydroxamic Acid (SAHA), induces apoptosis in prostate cancer cell lines via the Akt/FOXO3a signaling pathway. Med Sci Monit 23:5793–5802
Wang YC, Yang X, Xing LH, Kong WZ (2013) Effects of SAHA on proliferation and apoptosis of hepatocellular carcinoma cells and hepatitis B virus replication. World J Gastroenterol 19:5159–5164
Pobbati AV, Hong W (2020) A combat with the YAP/TAZ-TEAD oncoproteins for cancer therapy. Theranostics 10:3622–3635
Marti P, Stein C, Blumer T, Abraham Y, Dill MT, Pikiolek M, Orsini V, Jurisic G, Megel P, Makowska Z, Agarinis C, Tornillo L, Bouwmeester T, Ruffner H, Bauer A, Parker CN, Schmelzle T, Terracciano LM, Heim MH, Tchorz JS (2015) YAP promotes proliferation, chemoresistance, and angiogenesis in human cholangiocarcinoma through TEAD transcription factors. Hepatology 62:1497–1510
Hao Y, Baker D, Dijke P (2019) TGF-β-mediated epithelial-mesenchymal transition and cancer metastasis. Int J Mol Sci 20:2767
Ling HH, Kuo CC, Lin BX, Huang YH, Lin CW (2017) Elevation of YAP promotes the epithelial-mesenchymal transition and tumor aggressiveness in colorectal cancer. Exp Cell Res 350:218–225
Jiang GM, Wang HS, Zhang F, Zhang KS, Liu ZC, Fang R, Wang H, Cai SH, Du J (2013) Histone deacetylase inhibitor induction of epithelial-mesenchymal transitions via up-regulation of Snail facilitates cancer progression. Biochim Biophys Acta 1833:663–671
Basu D, Reyes-Múgica M, Rebbaa A (2013) Histone acetylation-mediated regulation of the hippo pathway. PLoS One 8:e62478
Willis BC, Borok Z (2007) TGF-beta-induced EMT: mechanisms and implications for fibrotic lung disease. Am J Physiol Lung Cell Mol Physiol 293:L525–L534
Wang J, Xu MX, Jiang XL, Mei XY, Liu XG (2018) Histone deacetylase inhibitor SAHA-induced epithelial-mesenchymal transition by upregulating Slug in lung cancer cells. Anticancer Drugs 29:80–88
Papoutsoglou P, Louis C, Coulouarn C (2019) Transforming growth factor-beta (TGFβ) signaling pathway in cholangiocarcinoma. Cells 8:960
İnce AT, Yıldız K, Gangarapu V, Kayar Y, Baysal B, Karatepe O, Sarbay Kemik A, Şentürk H (2015) Serum and biliary MMP-9 and TIMP-1 concentrations in the diagnosis of cholangiocarcinoma. Int J Clin Exp Med 8:2734–2740
Bourboulia D, Han HY, Jensen-Taubman S, Gavil N, Isaac B, Wei B, Neckers L, Stetler-Stevenson WG (2013) TIMP-2 modulates cancer cell transcriptional profile and enhances E-cadherin/beta-catenin complex expression in A549 lung cancer cells. Oncotarget 4:166–176
Scheau C, Badarau IA, Costache R, Caruntu C, Mihai GL, Didilescu AC, Constantin C, Neagu M (2019) The role of matrix metalloproteinases in the epithelial-mesenchymal transition of hepatocellular carcinoma. Anal Cell Pathol (Amst) 2019:9423907
Selaru FM, Olaru AV, Kan T, David S, Cheng Y, Mori Y, Yang J, Paun B, Jin Z, Agarwal R, Hamilton JP, Abraham J (2009) MicroRNA-21 is overexpressed in human cholangiocarcinoma and regulates programmed cell death 4 and tissue inhibitor of metalloproteinase 3. Hepatology 49:1595–1601
Shen Z, Liao X, Shao Z, Feng M, Yuan J, Wang S, Gan S, Ha Y, He Z, Jie W (2019) Short-term stimulation with histone deacetylase inhibitor trichostatin a induces epithelial-mesenchymal transition in nasopharyngeal carcinoma cells without increasing cell invasion ability. BMC Cancer 19:262
Author information
Authors and Affiliations
Contributions
Concept – GB; Design – GB, MB, MÖ; Supervision – GB; Resource – GB; Materials – GB, MÖ, HA, FG, ÇU, BND; Data Collection and/or Processing – GB, MÖ, HA; Analysis and/or Interpretation – GB, HA, MÖ, FG, ÇU, BND; Literature Search – GB, MB, MÖ; Writing – GB, MÖ; Critical Reviews – GB, MB.
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest was declared by the authors. The authors declared that this study had received no financial support.
Ethical approval
Ethics committee approval is not needed since it is a cell culture study.
Informed consent
No informed consent is needed since it is a cell culture study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Özel, M., Başkol, G., Başkol, M. et al. SAHA induce hippo pathway in CCA cells without increasing cell proliferation. Mol Biol Rep 49, 3649–3656 (2022). https://doi.org/10.1007/s11033-022-07204-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-07204-8