Abstract
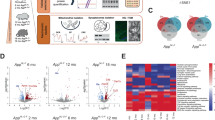
Alzheimer’s disease (AD) is the most common neurodegenerative disorder, and is caused by multiple pathological factors, such as the overproduction of β-amyloid (Aβ) and the hyperphosphorylation of tau. However, there is limited knowledge of the mechanisms underlying AD pathogenesis and no effective biomarker for the early diagnosis of this disorder. Thus in this study, a quantitative phosphoproteomics analysis was performed to evaluate global protein phosphorylation in the hippocampus of Aβ overexpressing APP/PS1 transgenic mice and tau overexpressing MAPT×P301S transgenic mice, two in vivo AD model systems. These animals, up to ten weeks old, do not exhibit cognitive dysfunctions and are widely used to simulate early-stage AD patients. The number of differentially phosphorylated proteins (DPPs) was greater for APP/PS1 transgenic mice than for MAPT×P301S transgenic mice. The function of the DPPs in APP/PS1 transgenic mice was mainly related to synapses, while the function of the DPPs in MAPT×P301S transgenic mice was mainly related to microtubules. In addition, an AD core network was established including seven phosphoproteins differentially expressed in both animal models, and the function of this core network was related to synapses and oxidative stress. The results of this study suggest that Aβ and tau induce different protein phosphorylation profiles in the early stage of AD, leading to the dysfunctions in synapses and microtubule, respectively. And the detection of same DPPs in these animal models might be used for early AD diagnosis.









Similar content being viewed by others
Data availability
The raw LC-MS data and supplemental information are available via the integrated Proteome Resources (https://www.iprox.cn//page/project.html?id=IPX0005949000).
Abbreviations
- AAK1:
-
ap2 associated protein kinase 1
- Aβ:
-
β-amyloid
- ADAM22:
-
disintegrin and metalloproteinase domain containing protein 22
- AD:
-
Alzheimer’s disease
- ADD2:
-
β-adducin 2
- ANK2:
-
ankyrin-2
- APBA1:
-
amyloid beta A4 precursor protein binding family a member 1
- BCA:
-
bicinchoninic acid
- BCR:
-
breakpoint cluster region protein
- BP:
-
biological process
- BSN:
-
bassoon
- CANX:
-
calnexin
- CAP2:
-
adenylyl cyclase-associated protein
- CC:
-
cellular components
- CDK5:
-
cyclin dependent kinase 5
- CFL1:
-
cofilin 1
- cGMP-PKG:
-
cyclic guanosine monophosphate- protein kinase G
- CSF:
-
cerebrospinal fluid
- CTNND2:
-
catenina δ-2
- DBN1:
-
drebrin 1
- DNM1:
-
dynamin-1
- DPPs:
-
differentially phosphorylated proteins
- DPYSL2:
-
dihydropyrimidinase-related protein 2
- ERK1/2:
-
extracellular regulated protein kinase 1/2
- FC:
-
fold change
- FDRs:
-
false discovery rates
- GIT1:
-
ARF GTPase-activating protein
- GO:
-
Gene Ontology
- GPM6A:
-
neuronal membrane glycoprotein M6-a
- GSK3β:
-
glycogen synthase kinase-3β
- HIST1H1B:
-
histone H1.5
- HSP90AA1:
-
heat shock protein 90-α
- INA:
-
α-internexin
- KCNA2:
-
potassium voltage-gated channel subfamily A member 2
- KEGG:
-
Kyoto Encyclopedia of Genes and Genomes
- MAP1A:
-
microtubule-associated protein 1 A
- MAP1B:
-
microtubule-associated protein 1B
- MAPK3:
-
mitogen-activated protein kinase 3
- MAP2:
-
microtubule-associated protein 2
- MAP7D1:
-
MAP7 domain-containing protein 1
- MAPT:
-
microtubule-associated protein tau
- MF:
-
molecular function
- nano-LC-MS/MS:
-
nanoscale liquid chromatography with tandem mass spectrometry
- NEFH:
-
neurofilament heavy polypeptide
- NF1:
-
neurofibromin
- NFTs:
-
neurofibrillary tangles
- NIH:
-
national Institutes of Health
- NLRP3:
-
Nucleotide-binding oligomerization domain, leucine- rich repeat and pyrin domain- containing 3
- NMDAR:
-
N-methyl-d-aspartic acid receptor
- OXR1:
-
oxidation resistance protein 1
- PACS1:
-
phosphofurin acidic cluster sorting protein 1
- PCA:
-
principal component analysis
- PLCB1:
-
1-phosphatidylinositol 4,5-bisphosphate phosphodiesterase β-1
- PLXNC1:
-
plexin-C1
- PP1:
-
(phosphatase-1)
- PP2A:
-
protein phosphatase-2 A
- PP5:
-
protein phosphatase-5
- PPI:
-
protein-protein interaction
- PRKCE:
-
protein kinase C epsilon type
- PRKCG:
-
protein kinase C gamma type
- PSEN1:
-
presenilin 1
- RIMS1:
-
regulating synaptic membrane exocytosis protein 1
- RTN4:
-
reticulon 4
- SORT1:
-
sortilin 1
- SPNB2:
-
β-spectrin
- SRRM2:
-
serine/arginine repetitive matrix protein 2
- SYN2:
-
synapsin-2
- SYNJ1:
-
synaptojanin 1
- SV2A:
-
synaptic vesicle glycoprotein 2a
- TTBK1:
-
tau tubulin kinase 1
- UNC13A:
-
protein unc-13 homolog A
- VMAP2:
-
vesicle-associated membrane protein 2
- WT:
-
wild-type
References
Ahmad F, Mein H, Jing Y, Zhang H, Liu P (2021) Behavioural functions and cerebral blood Flow in a P301S Tauopathy Mouse Model: a time-course study. Int J Mol Sci 22. https://doi.org/10.3390/ijms22189727
Al Zaabi N, Al Menhali N, Al-Jasmi F (2018) SYNJ1 gene associated with neonatal onset of neurodegenerative disorder and intractable seizure. Mol Genet Genomic Med 6:109–113. https://doi.org/10.1002/mgg3.341
Alonso AD, Cohen LS, Corbo C, Morozova V, ElIdrissi A, Phillips G, Kleiman FE (2018) Hyperphosphorylation of Tau Associates with changes in its function beyond Microtubule Stability. Front Cell Neurosci 12:338. https://doi.org/10.3389/fncel.2018.00338
Bednarek E, Caroni P (2011) β-Adducin is required for stable assembly of new synapses and improved memory upon environmental enrichment. Neuron 69:1132–1146. https://doi.org/10.1016/j.neuron.2011.02.034
Brocco MA, Fernández ME, Frasch AC (2010) Filopodial protrusions induced by glycoprotein M6a exhibit high motility and aids synapse formation. Eur J Neurosci 31:195–202. https://doi.org/10.1111/j.1460-9568.2009.07064.x
Chen C, Jiang X, Li Y, Yu H, Li S, Zhang Z, Xu H, Yang Y, Liu G, Zhu F, Ren X, Zou L, Xu B, Liu J, Spencer PS, Yang X (2019a) Low-dose oral copper treatment changes the hippocampal phosphoproteomic profile and perturbs mitochondrial function in a mouse model of Alzheimer’s disease. Free Radic Biol Med 135:144–156. https://doi.org/10.1016/j.freeradbiomed.2019.03.002
Chen Y, Xu J, Zhou X, Liu S, Zhang Y, Ma S, Fu AKY, Ip NY, Chen Y (2019b) Changes of protein phosphorylation are Associated with synaptic functions during the early stage of Alzheimer’s Disease. ACS Chem Neurosci 10:3986–3996. https://doi.org/10.1021/acschemneuro.9b00190
Chung SH (2009) Aberrant phosphorylation in the pathogenesis of Alzheimer’s disease. BMB Rep 42 467 – 74 https//. https://doi.org/10.5483/bmbrep.2009.42.8.467
de Wilde MC, Overk CR, Sijben JW, Masliah E (2016) Meta-analysis of synaptic pathology in Alzheimer’s disease reveals selective molecular vesicular machinery vulnerability. Alzheimers Dement 12:633–644. https://doi.org/10.1016/j.jalz.2015.12.005
Ferrari A, Hoerndli F, Baechi T, Nitsch RM, Götz J (2003) beta-amyloid induces paired helical filament-like tau filaments in tissue culture. J Biol Chem 278:40162–40168. https://doi.org/10.1074/jbc.M308243200
Ferreira S, Pitman KA, Summers BS, Wang S, Young KM, Cullen CL (2021) Oligodendrogenesis increases in hippocampal grey and white matter prior to locomotor or memory impairment in an adult mouse model of tauopathy. Eur J Neurosci 54:5762–5784. https://doi.org/10.1111/ejn.14726
Goodwin LO, Splinter E, Davis TL, Urban R, He H, Braun RE, Chesler EJ, Kumar V, van Min M, Ndukum J, Philip VM, Reinholdt LG, Svenson K, White JK, Sasner M, Lutz C, Murray SA (2019) Large-scale discovery of mouse transgenic integration sites reveals frequent structural variation and insertional mutagenesis. Genome Res 29:494–505. https://doi.org/10.1101/gr.233866.117
Guo Q, Li H, Cole AL, Hur JY, Li Y, Zheng H (2013) Modeling Alzheimer’s disease in mouse without mutant protein overexpression: cooperative and independent effects of Aβ and tau. PLoS ONE 8:e80706. https://doi.org/10.1371/journal.pone.0080706
Guo T, Zhang D, Zeng Y, Huang TY, Xu H, Zhao Y (2020) Molecular and cellular mechanisms underlying the pathogenesis of Alzheimer’s disease. Mol Neurodegener 15:40. https://doi.org/10.1186/s13024-020-00391-7
Hall AM, Roberson ED (2012) Mouse models of Alzheimer’s disease. Brain Res Bull 88:3–12. https://doi.org/10.1016/j.brainresbull.2011.11.017
Hoffman JL, Faccidomo S, Kim M, Taylor SM, Agoglia AE, May AM, Smith EN, Wong LC, Hodge CW (2019) Alcohol drinking exacerbates neural and behavioral pathology in the 3xTg-AD mouse model of Alzheimer’s disease. Int Rev Neurobiol 148:169–230. https://doi.org/10.1016/bs.irn.2019.10.017
Hurtado DE, Molina-Porcel L, Iba M, Aboagye AK, Paul SM, Trojanowski JQ, Lee VM (2010) A{beta} accelerates the spatiotemporal progression of tau pathology and augments tau amyloidosis in an Alzheimer mouse model. Am J Pathol 177:1977–1988. https://doi.org/10.2353/ajpath.2010.100346
Ju Y, Tam KY (2022) Pathological mechanisms and therapeutic strategies for Alzheimer’s disease. Neural Regen Res 17:543–549. https://doi.org/10.4103/1673-5374.320970
Julca DM, Diaz J, Berger S, Leon E (2019) MAP1B related syndrome: case presentation and review of literature. Am J Med Genet A 179:1703–1708. https://doi.org/10.1002/ajmg.a.61280
Kimura T, Ishiguro K, Hisanaga S (2014) Physiological and pathological phosphorylation of tau by Cdk5. Front Mol Neurosci 7:65. https://doi.org/10.3389/fnmol.2014.00065
Kohansal-Nodehi M, Chua JJ, Urlaub H, Jahn R, Czernik D (2016) Analysis of protein phosphorylation in nerve terminal reveals extensive changes in active zone proteins upon exocytosis. Elife 5. https://doi.org/10.7554/eLife.14530
Kosel F, Pelley JMS, Franklin TB (2020) Behavioural and psychological symptoms of dementia in mouse models of Alzheimer’s disease-related pathology. Neurosci Biobehav Rev 112:634–647. https://doi.org/10.1016/j.neubiorev.2020.02.012
Kurt MA, Davies DC, Kidd M, Duff K, Rolph SC, Jennings KH, Howlett DR (2001) Neurodegenerative changes associated with beta-amyloid deposition in the brains of mice carrying mutant amyloid precursor protein and mutant presenilin-1 transgenes. Exp Neurol 171:59–71. https://doi.org/10.1006/exnr.2001.7717
León A, Aparicio GI, Scorticati C (2021) Neuronal glycoprotein M6a: an emerging molecule in Chemical synapse formation and dysfunction. Front Synaptic Neurosci 13:661681. https://doi.org/10.3389/fnsyn.2021.661681
Leveille E, Ross OA, Gan-Or Z (2021) Tau and MAPT genetics in tauopathies and synucleinopathies. Parkinsonism Relat Disord 90:142–154. https://doi.org/10.1016/j.parkreldis.2021.09.008
Li H, Ruberu K, Muñoz SS, Jenner AM, Spiro A, Zhao H, Rassart E, Sanchez D, Ganfornina MD, Karl T, Garner B (2015) Apolipoprotein D modulates amyloid pathology in APP/PS1 Alzheimer’s disease mice. Neurobiol Aging 36:1820–1833. https://doi.org/10.1016/j.neurobiolaging.2015.02.010
Liu F, Grundke-Iqbal I, Iqbal K, Gong CX (2005) Contributions of protein phosphatases PP1, PP2A, PP2B and PP5 to the regulation of tau phosphorylation. Eur J Neurosci 22:1942–1950. https://doi.org/10.1111/j.1460-9568.2005.04391.x
Liu P, Zou LB, Wang LH, Jiao Q, Chi TY, Ji XF, Jin G (2014) Xanthoceraside attenuates tau hyperphosphorylation and cognitive deficits in intracerebroventricular-streptozotocin injected rats. Psychopharmacology 231:345–356. https://doi.org/10.1007/s00213-013-3240-4
Montenegro-Venegas C, Guhathakurta D, Pina-Fernandez E, Andres-Alonso M, Plattner F, Gundelfinger ED, Fejtova A (2022) Bassoon controls synaptic vesicle release via regulation of presynaptic phosphorylation and cAMP. EMBO Rep 23:e53659. https://doi.org/10.15252/embr.202153659
Nie L, He K, Xie F, Xiao S, Li S, Xu J, Zhang K, Yang C, Zhou L, Liu J, Zou L, Yang X (2021) Loganin substantially ameliorates molecular deficits, pathologies and cognitive impairment in a mouse model of Alzheimer’s disease. Aging 13:23739–23756. https://doi.org/10.18632/aging.203646
Nunomura A, Perry G (2020) RNA and Oxidative Stress in Alzheimer’s Disease: Focus on microRNAs. Oxid Med Cell Longev 2020, 2638130 https://doi.org/10.1155/2020/2638130
Pavon MV, Navakkode S, Wong LW, Sajikumar S (2023) Inhibition of Nogo-A rescues synaptic plasticity and associativity in APP/PS1 animal model of Alzheimer’s disease. Semin Cell Dev Biol 139:111–120. https://doi.org/10.1016/j.semcdb.2022.04.005
Peng L, Bestard-Lorigados I, Song W (2022) The synapse as a treatment avenue for Alzheimer’s Disease. Mol Psychiatry 27:2940–2949. https://doi.org/10.1038/s41380-022-01565-z
Petzold A (2005) Neurofilament phosphoforms: surrogate markers for axonal injury, degeneration and loss. J Neurol Sci 233:183–198. https://doi.org/10.1016/j.jns.2005.03.015
Ramesh M, Gopinath P, Govindaraju T (2020) Role of post-translational modifications in Alzheimer’s Disease. ChemBioChem 21:1052–1079. https://doi.org/10.1002/cbic.201900573
Scheltens P, De Strooper B, Kivipelto M, Holstege H, Chételat G, Teunissen CE, Cummings J, van der Flier WM (2021) Alzheimer’s disease. Lancet 397:1577–1590. https://doi.org/10.1016/s0140-6736(20)32205-4
Sontag JM, Sontag E (2014) Protein phosphatase 2A dysfunction in Alzheimer’s disease. Front Mol Neurosci 7:16. https://doi.org/10.3389/fnmol.2014.00016
Tanaka H, Kondo K, Chen X, Homma H, Tagawa K, Kerever A, Aoki S, Saito T, Saido T, Muramatsu SI, Fujita K, Okazawa H (2018) The intellectual disability gene PQBP1 rescues Alzheimer’s disease pathology. Mol Psychiatry 23:2090–2110. https://doi.org/10.1038/s41380-018-0253-8
Tompa P, Davey NE, Gibson TJ, Babu MM (2014) A million peptide motifs for the molecular biologist. Mol Cell 55:161–169. https://doi.org/10.1016/j.molcel.2014.05.032
Volkert MR, Crowley DJ (2020) Preventing neurodegeneration by Controlling oxidative stress: the role of OXR1. Front Neurosci 14:611904. https://doi.org/10.3389/fnins.2020.611904
Wang J, Lv X, Wu Y, Xu T, Jiao M, Yang R, Li X, Chen M, Yan Y, Chen C, Dong W, Yang W, Zhuo M, Chen T, Luo J, Qiu S (2018) Postsynaptic RIM1 modulates synaptic function by facilitating membrane delivery of recycling NMDARs in hippocampal neurons. Nat Commun 9:2267. https://doi.org/10.1038/s41467-018-04672-0
Wang BB, Liang WD, Liang HZ, Liu B, Wang QY, Yan YH, Wang TT, Jiang YF, Jiang YL, Qiu HD, Lu LH, Cui W, Zhou Y, Zhao LL, Yu HB (2021) Phosphonate-functionalized ionic liquid: a new surface modifier contributing to the enhanced Enrichment of phosphorylated peptides. ACS Sustain Chem Eng 9:7930–7940. https://doi.org/10.1021/acssuschemeng.1c02119
Wang T, Zhang X, Wang Y, Liu W, Wang L, Hao L, Ju M, Xiao R (2022) High cholesterol and 27-hydroxycholesterol contribute to phosphorylation of tau protein by impairing autophagy causing learning and memory impairment in C57BL/6J mice. J Nutr Biochem 106:109016. https://doi.org/10.1016/j.jnutbio.2022.109016
Wegmann S, Biernat J, Mandelkow E (2021) A current view on tau protein phosphorylation in Alzheimer’s disease. Curr Opin Neurobiol 69:131–138. https://doi.org/10.1016/j.conb.2021.03.003
Xia CL, Wang QY, Liang WD, Wang BB, Feng QS, Zhou CY, Xie YS, Yan YH, Zhao LL, Jiang B, Cui W, Liang HZ (2022) Superhydrophilic nanocomposite adsorbents modified via nitrogen-rich phosphonate-functionalized ionic liquid linkers: enhanced phosphopeptide enrichment and phosphoproteome analysis of tau phosphorylation in the hippocampal lysate of Alzheimer’s transgenic mice. J Mater Chem B 10:7967–7978. https://doi.org/10.1039/d2tb01508k
Yazawa A, Hensley K, Ohshima T (2022) Effects of Lanthionine Ketimine-5-Ethyl Ester on the α-Synucleinopathy mouse model. Neurochem Res 47:2373–2382. https://doi.org/10.1007/s11064-022-03626-9
Yoshiyama Y, Higuchi M, Zhang B, Huang SM, Iwata N, Saido TC, Maeda J, Suhara T, Trojanowski JQ, Lee VM (2007) Synapse loss and microglial activation precede tangles in a P301S tauopathy mouse model. Neuron 53:337–351. https://doi.org/10.1016/j.neuron.2007.01.010
Yu H, Wu J (2021) Amyloid-β: a double agent in Alzheimer’s disease? Biomed Pharmacother 139:111575. https://doi.org/10.1016/j.biopha.2021.111575
Zhang H, Wei W, Zhao M, Ma L, Jiang X, Pei H, Cao Y, Li H (2021) Interaction between Aβ and tau in the pathogenesis of Alzheimer’s Disease. Int J Biol Sci 17:2181–2192. https://doi.org/10.7150/ijbs.57078
Zott B, Busche MA, Sperling RA, Konnerth A (2018) What happens with the circuit in Alzheimer’s Disease in mice and humans? Annu Rev Neurosci 41:277–297. https://doi.org/10.1146/annurev-neuro-080317-061725
Acknowledgements
We would like to express our gratitude to all members of the College Student Innovation Team in Dr. Cui Wei’s Lab. We sincerely appreciate the technical supports by Dr. Majie Wang in Ningbo Kangning hospital, and by the Core Facilities and Laboratory Animal Center of Ningbo University, School of Medicine.
Funding
This work was supported by Natural Science Foundation of Zhejiang Province (LY21H090002), the National Natural Science Foundation of China (81870853, 82271443), Applied Research Project on Nonprofit Technology of Ningbo (20211JCGY020160), Major program of Ningbo Science and Technology Innovation 2025 (2019B10067, 2020Z093, 2021Z046), and the K. C. Wong Magna Fund in Ningbo University.
Author information
Authors and Affiliations
Contributions
Qiyao Wang: Conceptualization, Methodology, Formal analysis, Investigation, Data curation, Writing - original draft, and Writing - review & editing. Chenglong Xia: Investigation, Data curation. An Zhu: Investigation. Yongjie Bao: Investigation. Jiani Lu: Investigation. Yuan Chen: Investigation. Jiayi Xu: Investigation. Binbin Wang, Investigation. C. Benjamin Naman: Investigation, and Writing - review & editing. Liping Li: Investigation. Qinwen Wang: Investigation. Hao Liu: Investigation. Hongze Liang: Conceptualization, Writing - original draft, Writing - review & editing, Supervision, Funding acquisition. Wei Cui: Conceptualization, Writing - original draft, Writing - review & editing, Supervision, Funding acquisition.
Corresponding authors
Ethics declarations
Competing interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethics approval
All procedures in our animal experiments were approved by the Animal Ethics and Welfare Committee of Ningbo University (SYXK-2019-0005).
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Q., Xia, C., Zhu, A. et al. Discrepancy of synaptic and microtubular protein phosphorylation in the hippocampus of APP/PS1 and MAPT×P301S transgenic mice at the early stage of Alzheimer’s disease. Metab Brain Dis 38, 1983–1997 (2023). https://doi.org/10.1007/s11011-023-01209-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-023-01209-3