Abstract
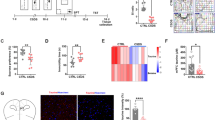
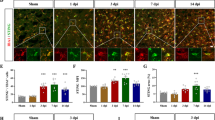
Some mechanisms of neuronal degeneration in endotoxinemia are already well described, but need to be detailed. In this study, we tested the effect of a single intraperitoneal injection of a LPS sub-septic dose (1 mg/kg of animal weight) on calpain activity in the striatum and hippocampus. We showed, that in the hippocampus the day after LPS administration an increase in production of IL-1β and TNF-α mRNA, followed by elevated mRNA expression and activity of µ- and m-calpains without signs of microglia activation is observed. In striatal cells, the day after LPS injection an increase in expression of IL-1β, TNF-α, IBA-1, m-calpain and calpastatin mRNA is revealed, which only intensifies over time. The elicited changes are accompanied by a decrease in motor behavior, which can be considered as a sign of sickness behavior. In the hippocampus, 180 days after LPS administration expression of TNF-α, content and activity of µ-calpain are increased. In the striatum, elevation in expression of TNF-α, IBA-1, µ- and m-calpain mRNA, with hyperactivation of only m-calpain, is observed. Significantly reduced motor activity can be a consequence of LPS-induced neuronal death. A long-lasting endotoxin activates microglia that damage neurons via proinflammation cytokines and calpain hyperactivation. The endotoxin hypothesis of neurodegeneration is unproven, but if correct, then neurodegeneration may be reduced by decreasing endotoxin-induced neuroinflammation and m-calpain hyperactivation. Therefore, the drugs, that decrease endotoxin-induced neuroinflammation and differently inhibit µ- or m-calpain, can be used to prevent or reduce the severity of neurodegeneration.







Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Abareshi A, Anaeigoudari A, Norouzi F, Marefati N, Beheshti F, Saeedjalali M, Hosseini M (2019) The effects of captopril on lipopolysaccharide-induced sickness behaviors in rats. Vet Res Forum 10(3):199–205. https://doi.org/10.30466/vrf.2018.90760.2198
Banks WA, Robinson SM (2010) Minimal penetration of lipopolysaccharide across the murine blood–brain barrier. Brain Behav Immun 24(1):102–109. https://doi.org/10.1016/j.bbi.2009.09.001
Batista CRA, Gomes GF, Candelario-Jalil E, Fiebich BL, Oliveira ACP (2019) Lipopolysaccharide-induced neuroinflammation as a bridge to understand neurodegeneration. Int J Mol Sci 20(9):2293. https://doi.org/10.3390/ijms20092293
Baudry M, Bi X (2016) Calpain-1 and calpain-2: the yin and yang of synaptic plasticity and neurodegeneration. Trends Neurosci 39(4):235–245. https://doi.org/10.1016/j.tins.2016.01.007
Biswas AK, Tandon S (2019) Casein zymography for analysis of calpain-1 and calpain-2 activity. Methods Mol Biol 1915:31–38. https://doi.org/10.1007/978-1-4939-8988-1_3
Bossù P, Cutuli D, Palladino I, Caporali P, Angelucci F, Laricchiuta D, Gelfo F, Bartolo P, Caltagirone C, Petrosini L (2012) A single intraperitoneal injection of endotoxin in rats induces long-lasting modifications in behavior and brain protein levels of TNF-α and IL-18. J Neuroinflammation 9:101. https://doi.org/10.1186/1742-2094-9-101
Brown GC (2019) The endotoxin hypothesis of neurodegeneration. J Neuroinflammation 16(1):180. https://doi.org/10.1186/s12974-019-1564-7
Buchanan JB, Sparkman NL, Johnson RW (2010) A neurotoxic regimen of methamphetamine exacerbates the febrile and neuroinflammatory response to a subsequent peripheral immune stimulus. J Neuroinflammation 7:82. https://doi.org/10.1186/1742-2094-7-82
Burton MD, Sparkman NL, Johnson RW (2011) Inhibition of interleukin-6 trans-signaling in the brain facilitates recovery from lipopolysaccharide-induced sickness behavior. J Neuroinflammation 8:54. https://doi.org/10.1186/1742-2094-8-54
Catorce MN, Gevorkian G (2016) LPS-induced Murine Neuroinflammation Model: Main Features and Suitability for Pre-clinical Assessment of Nutraceuticals. Curr Neuropharmacol 14(2):155–164. https://doi.org/10.2174/1570159x14666151204122017
Goll DE, Thompson V, Li H, Wei W, Cong J (2003) The calpain system. Physiol Rev 83(3):731–801. https://doi.org/10.1152/physrev.00029.2002
He Q, Yu W, Wu J, Chen C, Lou Z, Zhang Q, Zhao J, Wang J, Xiao B (2013) Intranasal LPS-mediated Parkinson’s model challenges the pathogenesis of nasal cavity and environmental toxins. PLoS ONE 8(11):e78418. https://doi.org/10.1371/journal.pone.0078418
Huang J, Zhao L, Yang J, Zhang B, Xu X, Chen K, Huang M (2019) The effect of µ/m-calpain on protein degradation of chicken breast meat. J Food Sci 84(5):1054–1059. https://doi.org/10.1111/1750-3841.14596
Iturria SJ (2011) A method for obtaining randomized block designs in preclinical studies with multiple quantitative blocking variables. Pharm Stat 10(2):169–174. https://doi.org/10.1002/pst.445
Kagan JC (2017) Lipopolysaccharide detection across the kingdoms of life. Trends Immunol 38(10):696–704. https://doi.org/10.1016/j.it.2017.05.001
Kenessey A, Banay-Schwartz M, DeGuzman T, Lajtha A. (1989) Regional distribution of brain calpastatin and of calpain II. Activity with casein and with endogenous brain protein substrates. Neurochem Int. 15(3): 307–314. https://doi.org/10.1016/0197-0186(89)90137-x
Liu M, Bing G (2011) Lipopolysaccharide animal models for Parkinson’s disease. Parkinsons Dis 2011:327089. https://doi.org/10.4061/2011/327089
Neumar RW, Meng FH, Mills AM, Xu YA, Zhang C, Welsh FA, Siman R (2001) Calpain activity in the rat brain after transient forebrain ischemia. Exp Neurol 170(1):27–35. https://doi.org/10.1006/exnr.2001.7708
Paul CA, Beltz B, Berger-Sweeney J. (2008) Dissection of rat brains, CSH Protoc. 2008:pdb.prot4803. https://doi.org/10.1101/pdb.prot4803
Paxinos G, Watson C (2013) The Rat Brain in Stereotaxic Coordinates, 7th edn. Academic Press
Perry VH (2004) The influence of systemic inflammation on inflammation in the brain: implications for chronic neurodegenerative disease. Brain Behav Immun 18(5):407–413. https://doi.org/10.1016/j.bbi.2004.01.004
Qin L, Wu X, Block ML, Liu Y, Breese GR, Hong J, Knapp DJ, Crews FT (2007) Systemic LPS causes chronic neuroinflammation and progressive neurodegeneration. Glia 55(5):453–462. https://doi.org/10.1002/glia.20467
Rolls A, Shechter R, London A, Ziv Y, Ronen A, Levy R, Schwartz M (2007) Toll-like receptors modulate adult hippocampal neurogenesis. Nat Cell Biol 9(9):1081–1088. https://doi.org/10.1038/ncb1629
Ruetten H, Thiemermann C (1997) Effect of calpain inhibitor I, an inhibitor of the proteolysis of I kappa B, on the circulatory failure and multiple organ dysfunction caused by endotoxin in the rat. Br J Pharmacol 121(4):695–704. https://doi.org/10.1038/sj.bjp.0701180
Sadraie S, Kiasalari Z, Razavian M, Azimi S, Sedighnejad L, Afshin-Majd S, Baluchnejadmojarad T, Roghani M (2019) Berberine ameliorates lipopolysaccharide-induced learning and memory deficit in the rat: insights into underlying molecular mechanisms. Metab Brain Dis 34(1):245–255. https://doi.org/10.1007/s11011-018-0349-5
Seinfeld J, Baudry N, Xu X, Bi X, Baudry M. (2016) Differential Activation of Calpain-1 and Calpain-2 following Kainate-Induced Seizure Activity in Rats and Mice, eNeuro 3(4): ENEURO.0088–15.2016. https://doi.org/10.1523/ENEURO.0088-15.2016
Shang K, Zhang J, Amna T, Yang J, Cheng X, Zhang C, Hwang I (2015) Attenuation of cellular toxicity by calpain inhibitor induced by bacterial endotoxin: a mechanistic study using muscle precursor cells as a model system. Mol Biol Rep 42(8):1281–1288. https://doi.org/10.1007/s11033-015-3869-7
Swarnkar S, Tyagi E, Agrawal R, Singh MP, Nath C (2009) A comparative study on oxidative stress induced by LPS and rotenone in homogenates of rat brain regions. Environ Toxicol Pharmacol 27(2):219–224. https://doi.org/10.1016/j.etap.2008.10.003
Tishkina A, Rukhlenko A, Stepanichev M, Levshina I, Pasikova N, Onufriev M, Moiseeva Y, Piskunov A, Gulyaeva N (2012) Region-specific changes in activities of cell death-related proteases and nitric oxide metabolism in rat brain in a chronic unpredictable stress model. Metab Brain Dis 27(4):431–441. https://doi.org/10.1007/s11011-012-9328-4
Torvell M, Hampton DW, Connick P, MacLullich A, Cunningham C, Chandran S (2019) A single systemic inflammatory insult causes acute motor deficits and accelerates disease progression in a mouse model of human tauopathy. Alzheimers Dement (n Y) 5:579–591. https://doi.org/10.1016/j.trci.2019.09.001
Tufekci KU, Genc S, Genc K (2011) The endotoxin-induced neuroinflammation model of Parkinson’s disease. Parkinsons Dis 2011:487450. https://doi.org/10.4061/2011/487450
Vasconcelos AR, Yshii LM, Viel TA, Buck HS, Mattson MP, Scavone C, Kawamoto EM (2014) Intermittent fasting attenuates lipopolysaccharide-induced neuroinflammation and memory impairment. J Neuroinflammation 11:85. https://doi.org/10.1186/1742-2094-11-85
Wang Y, Bi X, Baudry M (2018) Calpain-2 as a therapeutic target for acute neuronal injury. Expert Opin Ther Targets 22(1):19–29. https://doi.org/10.1080/14728222.2018.1409723
Young JJ, Bruno D, Pomara N (2014) A review of the relationship between proinflammatory cytokines and major depressive disorder. J Affect Disord 169:15–20. https://doi.org/10.1016/j.jad.2014.07.032
Zhao J, Bi W, Xiao S, Lan X, Cheng X, Zhang J, Lu D, Wei W, Wang Y, Li H, Fu Y, Zhu L (2019) Neuroinflammation induced by lipopolysaccharide causes cognitive impairment in mice. Sci Rep 9(1):5790. https://doi.org/10.1038/s41598-019-42286-8
Zhao Y, Lukiw WJ (2018) Bacteroidetes neurotoxins and inflammatory neurodegeneration. Mol Neurobiol 55(12):9100–9107. https://doi.org/10.1007/s12035-018-1015-y
Zhao Z, Wang Y, Zhou R, Li Y, Gao Y, Tu D, Wilson B, Song S, Feng J, Hong J, Yakel JL (2020) A novel role of NLRP3-generated IL-1β in the acute-chronic transition of peripheral lipopolysaccharide-elicited neuroinflammation: implications for sepsis-associated neurodegeneration. J Neuroinflammation 17(1):64. https://doi.org/10.1186/s12974-020-1728-5
Author information
Authors and Affiliations
Contributions
Maystrenko V.A.: significant input on experimental design, performed animal dosing and sacrifice, tissue processing, PCR, behavior analysis;
Ivleva I.S.: significant input on experimental design, PCR, behavior analysis;
Krytskaya D.U.: significant input on experimental design, calpain activity analysis;
Zubov A.S.: significant input involved in writing revisions and interpretation experimental results;
Ivlev A.P.: significant input involved in writing revisions and generating figures for the manuscript, developed methods for data analysis;
Karpenko M.N.: significant input on experiment design, significant input as an author, interpretation experimental results and editing of manuscript.
Corresponding author
Ethics declarations
Ethical approval
All study protocols were in accordance with the Local Ethics Committee of the Institute of Experimental Medicine, which follows the NIH guidelines for care and use of animals (ethical number № 8/17, 2017).
Research involving human and animal participants
This article does not contain any studies with human participants performed by any of the authors.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maystrenko, V., Ivleva, I., Krytskaya, D. et al. Changes in activity of µ- and m-calpains and signs of neuroinflammation in the hippocampus and striatum of rats after single intraperitoneal injection of subseptic dose of endotoxin. Metab Brain Dis 36, 1917–1928 (2021). https://doi.org/10.1007/s11011-021-00755-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-021-00755-y