Abstract
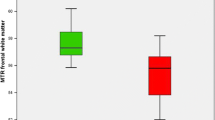
Hepatic encephalopathy (HE) is a frequent and debilitating complication of cirrhosis and its pathogenesis is not definitively clarified. Recent hypotheses focus on the possible existence of low-grade cerebral edema due to accumulation of osmolytes secondary to hyperammonemia. In the present study we investigated increases in cerebral water content by a novel magnetic resonance impedance (MRI) technique in cirrhosis patients with and without clinically manifest HE. We used a 3 T MRI technique for quantitative cerebral water content mapping in nine cirrhosis patients with an episode of overt HE, ten cirrhosis patients who never suffered from HE, and ten healthy aged-matched controls. We tested for differences between groups by statistical non-parametric mapping (SnPM) for a voxel-based spatial evaluation. The patients with HE had significantly higher water content in white matter than the cirrhosis patients (0.6%), who in turn, had significantly higher content than the controls (1.7%). Although the global gray matter water content did not differ between the groups, the patients with HE had markedly higher thalamic water content than patients who never experienced HE (6.0% higher). We found increased white matter water content in cirrhosis patients, predominantly in those with manifest HE. This confirms the presence of increasing degrees of low-grade edema with exacerbation of pathology. The thalamic edema in manifest HE may lead to compromised basal ganglia-thalamo-cortical circuits, in accordance with the major clinical symptoms of HE. The identification of the thalamus as particularly inflicted in manifest HE is potentially relevant to the pathophysiology of HE.


Similar content being viewed by others
Abbreviations
- HE:
-
Hepatic encephalopathy
- CRT:
-
continuous reaction time
- CSF:
-
ventricular cerebrospinal fluid
References
Abbas Z, Gras V, Mollenhoff K, Oros-Peusquens AM, Shah NJ (2015) Quantitative water content mapping at clinically relevant field strengths: a comparative study at 1.5 T and 3 T. Neuroimage. 106:404–413. https://doi.org/10.1016/j.neuroimage.2014.11.017
Ahl B, Weissenborn K, van den Hoff J et al (2004) Regional differences in cerebral blood flow and cerebral ammonia metabolism in patients with cirrhosis. Hepatology. 40(1):73–79. https://doi.org/10.1002/hep.20290
Bernal W, Hall C, Karvellas CJ, Auzinger G, Sizer E, Wendon J (2007) Arterial ammonia and clinical risk factors for encephalopathy and intracranial hypertension in acute liver failure. Hepatology. 46(6):1844–1852. https://doi.org/10.1002/hep.21838
Chen HJ, Zhu XQ, Shu H et al (2012) Structural and functional cerebral impairments in cirrhotic patients with a history of overt hepatic encephalopathy. Eur J Radiol 81(10):2463–2469. https://doi.org/10.1016/j.ejrad.2011.10.008
Chen HJ, Chen R, Yang M, Teng GJ, Herskovits EH (2015) Identification of minimal hepatic encephalopathy in patients with cirrhosis based on white matter imaging and bayesian data mining. AJNR Am J Neuroradiol 36(3):481–487. https://doi.org/10.3174/ajnr.A4146
Clemmesen JO, Larsen FS, Kondrup J, Hansen BA, Ott P (1999) Cerebral herniation in patients with acute liver failure is correlated with arterial ammonia concentration. Hepatology. 29(3):648–653
Córdoba J, Alonso J, Rovira A, Jacas C, Sanpedro F, Castells L, Vargas V, Margarit C, Kulisewsky J, Esteban R et al (2001) The development of low-grade cerebral edema in cirrhosis is supported by the evolution of (1)H-magnetic resonance abnormalities after liver transplantation. J Hepatol 35:598–604
Elsass P, Hartelius H (1985) Reaction time and brain disease: relations to location, etiology and progression of cerebral dysfunction. Acta Neurol Scand 71(1):11–19
Filley CM (2002) The neuroanatomy of attention. Semin Speech Lang 23(2):89–98. https://doi.org/10.1055/s-2002-24985
Gosseries O, Schnakers C, Ledoux D et al (2011a) Automated EEG entropy measurements in coma, vegetative state/unresponsive wakefulness syndrome and minimally conscious state. Funct Neurol 26(1):25–30
Gosseries O, Bruno MA, Chatelle C et al (2011b) Disorders of consciousness: What's in a name? NeuroRehabilitation. 28(1):3–14. https://doi.org/10.3233/NRE-2011-0625
Grover VP, Dresner MA, Forton DM et al (2006) Current and future applications of magnetic resonance imaging and spectroscopy of the brain in hepatic encephalopathy. World J Gastroenterol 12(19):2969–2978
Guevara M, Baccaro ME, Gomez-Anson B et al (2011) Cerebral magnetic resonance imaging reveals marked abnormalities of brain tissue density in patients with cirrhosis without overt hepatic encephalopathy. J Hepatol 55(3):564–573. https://doi.org/10.1016/j.jhep.2010.12.008
Haussinger D, Kircheis G, Fischer R, Schliess F, vom Dahl S (2000) Hepatic encephalopathy in chronic liver disease: a clinical manifestation of astrocyte swelling and low-grade cerebral edema? J Hepatol 32(6):1035–1038
Lauridsen MM, Mikkelsen S, Svensson T et al (2017) The continuous reaction time test for minimal hepatic encephalopathy validated by a randomized controlled multi-modal intervention-a pilot study. PLoS One 12(10):e0185412. https://doi.org/10.1371/journal.pone.0185412
Miese FR, Wittsack HJ, Kircheis G et al (2009) Voxel-based analyses of magnetization transfer imaging of the brain in hepatic encephalopathy. World J Gastroenterol 15(41):5157–5164
Neeb H, Zilles K, Shah NJ (2006) Fully-automated detection of cerebral water content changes: study of age- and gender-related H2O patterns with quantitative MRI. Neuroimage. 29(3):910–922
Rai R, Ahuja CK, Agrawal S et al (2015) Reversal of low-grade cerebral edema after lactulose/rifaximin therapy in patients with cirrhosis and minimal hepatic encephalopathy. Clin Transl Gastroenterol 6:e111. https://doi.org/10.1038/ctg.2015.38
Rangroo Thrane V, Thrane AS, Wang F et al (2013) Ammonia triggers neuronal disinhibition and seizures by impairing astrocyte potassium buffering. Nat Med 19(12):1643–1648. https://doi.org/10.1038/nm.3400
Reetz K, Abbas Z, Costa AS et al (2015) Increased cerebral water content in hemodialysis patients. PLoS One 10(3):e0122188. https://doi.org/10.1371/journal.pone.0122188
Rovira A, Mínguez B, Aymerich FX, Jacas C, Huerga E, Alonso CJ (2007) Decreased white matter lesion volume and improved cognitive function after liver transplantation. J. Hepatology. 46(5):1485–1490
Rovira A, Alonso J, Córdoba J (2008) MR imaging findings in hepatic encephalopathy. AJNR Am J Neuroradiol 29:1612–1621
Shah NJ, Neeb H, Kircheis G, Engels P, Haussinger D, Zilles K (2008) Quantitative cerebral water content mapping in hepatic encephalopathy. Neuroimage. 41(3):706–717. https://doi.org/10.1016/j.neuroimage.2008.02.057
Tao R, Zhang J, You Z et al (2013) The thalamus in cirrhotic patients with and without hepatic encephalopathy: a volumetric MRI study. Eur J Radiol 82(11):e715–e720. https://doi.org/10.1016/j.ejrad.2013.07.029
Weissenborn K, Giewekemeyer K, Heidenreich S, Bokemeyer M, Berding G, Ahl B (2005) Attention, memory, and cognitive function in hepatic encephalopathy. Metab Brain Dis 20(4):359–367. https://doi.org/10.1007/s11011-005-7919-z
Zeneroli ML, Cioni G, Crisi G, Vezzelli C, Ventura E (1991) Globus pallidus alterations and brain atrophy in liver cirrhosis patients with encephalopathy: an MR imaging study. Magn Reson Imaging 9(3):295–302
Zhang LJ, Qi R, Zhong J, Xu Q, Zheng G, Lu GM (2012) The effect of hepatic encephalopathy, hepatic failure, and portosystemic shunt on brain volume of cirrhotic patients: a voxel-based morphometry study. PLoS One 7(8):e42824. https://doi.org/10.1371/journal.pone.0042824
Acknowledgements
The authors wish to thank Ryan Sangill from Center of Functionally Integrative Neuroscience (CFIN), Aarhus University. CFIN and the Aase og Ejnar Danielsens Foundation financially supported the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial conflicts of interest related to publication of the data in this manuscript.
Financial support
Center of Functionally Integrative Neuroscience (CFIN), Aarhus University and the Aase & Ejnar Danielsens Foundation financially supported the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Winterdahl, M., Abbas, Z., Noer, O. et al. Cerebral water content mapping in cirrhosis patients with and without manifest HE. Metab Brain Dis 34, 1071–1076 (2019). https://doi.org/10.1007/s11011-019-00427-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-019-00427-y