Abstract
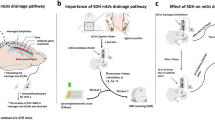
Subdural hematoma (SDH) drains into the extracranial lymphatic system through the meningeal lymphatic vessels (mLVs) but the formation of SDH impairs mLVs. Because vitamin D (Vit D) can protect the endothelial cells, we hypothesized that Vit D may enhance the SDH clearance. SDH was induced in Sprague–Dawley rats and treated with Vit D or vehicle. Hematoma volume in each group was measured by H&E staining and hemoglobin quantification. Evans blue (EB) quantification and red blood cells injection were used to evaluated the drainage of mLVs. Western blot analysis and immunofluorescence were conducted to assess the expression of lymphatic protein markers. We also examined the inflammatory factors levels in subdural space by ELISA. Vit D treatment significantly reduced SDH volume and improved the drainage of SDH to cervical lymph nodes. The structure of mLVs in SDH rats were protected by Vit D, and the expressions of LYVE1, PROX1, FOXC2, and VE-cadherin were increased after Vit D treatment. The TNF-α, IL-6, and IL-8 levels were reduced in Vit D group. In vitro, Vit D also increased the VE-cadherin expression levels under inflammation. Vit D protects the structure of mLVs and enhances the absorption of SDH, partly by the anti-inflammatory effect of Vit D.






Similar content being viewed by others
Data availability
The data are available from the corresponding author on reasonable request.
References
Nathan S, Goodarzi Z, Jette N et al (2017) Anticoagulant and antiplatelet use in seniors with chronic subdural hematoma: systematic review. Neurology 88:1889–1893. https://doi.org/10.1212/WNL.0000000000003918
Miranda LB, Braxton E, Hobbs J, Quigley MR (2011) Chronic subdural hematoma in the elderly: not a benign disease: clinical article. J Neurosurg 114:72–76. https://doi.org/10.3171/2010.8.JNS10298
Hohenstein A, Erber R, Schilling L, Weigel R (2005) Increased mRNA expression of VEGF within the hematoma and imbalance of angiopoietin-1 and -2 mRNA within the neomembranes of chronic subdural hematoma. J Neurotrauma 22:518–528. https://doi.org/10.1089/neu.2005.22.518
Heula A-L, Ohlmeier S, Sajanti J, Majamaa K (2013) Characterization of chronic subdural hematoma fluid proteome. Neurosurgery 73:317–331. https://doi.org/10.1227/01.neu.0000430323.24623.de
Edlmann E, Giorgi-Coll S, Whitfield PC et al (2017) Pathophysiology of chronic subdural haematoma: inflammation, angiogenesis and implications for pharmacotherapy. J Neuroinflammation 14:108. https://doi.org/10.1186/s12974-017-0881-y
Schwarz F, Loos F, Dünisch P et al (2015) Risk factors for reoperation after initial burr hole trephination in chronic subdural hematomas. Clin Neurol Neurosurg 138:66–71. https://doi.org/10.1016/j.clineuro.2015.08.002
Almenawer SA, Farrokhyar F, Hong C et al (2014) Chronic subdural hematoma management: a systematic review and meta-analysis of 34,829 patients. Ann Surg 259:449–457. https://doi.org/10.1097/SLA.0000000000000255
Oh H-J, Lee K-S, Shim J-J et al (2010) Postoperative course and recurrence of chronic subdural hematoma. J Korean Neurosurg Soc 48:518–523. https://doi.org/10.3340/jkns.2010.48.6.518
Jiang R-C, Feng H, Zhang J et al (2018) Safety and Efficacy of Atorvastatin for Chronic Subdural Hematoma in Chinese Patients: A Randomized ClinicalTrial. JAMA Neurol 75:1338–1346. https://doi.org/10.1001/jamaneurol.2018.2030
Louveau A, Smirnov I, Keyes TJ et al (2015) Structural and functional features of central nervous system lymphatic vessels. Nature 523:337–341. https://doi.org/10.1038/nature14432
Ahn JH, Cho H, Kim J-H et al (2019) Meningeal lymphatic vessels at the skull base drain cerebrospinal fluid. Nature 572:62–66. https://doi.org/10.1038/s41586-019-1419-5
Da Mesquita S, Louveau A, Vaccari A et al (2018) Functional aspects of meningeal lymphatics in ageing and Alzheimer’s disease. Nature 560:185–191. https://doi.org/10.1038/s41586-018-0368-8
Louveau A, Plog BA, Antila S et al (2017) Understanding the functions and relationships of the glymphatic system and meningeal lymphatics. J Clin Invest 127:10
Aspelund A, Antila S, Proulx ST et al (2015) A dural lymphatic vascular system that drains brain interstitial fluid and macromolecules. J Exp Med 212:991–999. https://doi.org/10.1084/jem.20142290
Bolte AC, Dutta AB, Hurt ME et al (2020) Meningeal lymphatic dysfunction exacerbates traumatic brain injury pathogenesis. Nat Commun 11:4524. https://doi.org/10.1038/s41467-020-18113-4
Kanamori M, Kipnis J (2020) Meningeal lymphatics “drain” brain tumors. Cell Res 30:191–192. https://doi.org/10.1038/s41422-020-0286-9
Liu X, Gao C, Yuan J et al (2020) Subdural haematomas drain into the extracranial lymphatic systemthrough the meningeal lymphatic vessels. Acta Neuropathol Commun 8:16. https://doi.org/10.1186/s40478-020-0888-y
Jamali N, Sorenson CM, Sheibani N (2018) Vitamin D and regulation of vascular cell function. Am J Physiol Heart Circ Physiol 314:H753–H765. https://doi.org/10.1152/ajpheart.00319.2017
Colotta F, Jansson B, Bonelli F (2017) Modulation of inflammatory and immune responses by vitamin D. J Autoimmun 85:78–97. https://doi.org/10.1016/j.jaut.2017.07.007
Schröder-Heurich B, von Hardenberg S, Brodowski L et al (2019) Vitamin D improves endothelial barrier integrity and counteracts inflammatory effects on endothelial progenitor cells. FASEB J Off Publ Fed Am Soc Exp Biol 33:9142–9153. https://doi.org/10.1096/fj.201802750RR
Latic N, Erben RG (2020) Vitamin D and Cardiovascular Disease, with Emphasis on Hypertension, Atherosclerosis, and Heart Failure. Int J Mol Sci 21:6483. https://doi.org/10.3390/ijms21186483
Giulietti A, van Etten E, Overbergh L et al (2007) Monocytes from type 2 diabetic patients have a pro-inflammatory profile. 1,25-Dihydroxyvitamin D(3) works as anti-inflammatory. Diabetes Res Clin Pract 77:47–57. https://doi.org/10.1016/j.diabres.2006.10.007
Kassi E, Adamopoulos C, Basdra EK, Papavassiliou AG (2013) Role of vitamin D in atherosclerosis. Circulation 128:2517–2531. https://doi.org/10.1161/CIRCULATIONAHA.113.002654
Yazdani S, Poosti F, Toro L et al (2017) Vitamin D inhibits lymphangiogenesis through VDR-dependent mechanisms. Sci Rep 7:44403. https://doi.org/10.1038/srep44403
Quan W, Zhang Z, Li P et al (2019) Role of regulatory T cells in atorvastatin induced absorption of chronic subdural hematoma in rats. Aging Dis 10:992–1002. https://doi.org/10.14336/AD.2018.0926
Xu X, Wang D, Han Z et al (2021) A novel rat model of chronic subdural hematoma: induction of inflammation and angiogenesis in the subdural space mimicking human-like features of progressively expanding hematoma. Brain Res Bull 172:108–119. https://doi.org/10.1016/j.brainresbull.2021.04.024
Grundmann M, Haidar M, Placzko S et al (2012) Vitamin D improves the angiogenic properties of endothelial progenitor cells. Am J Physiol Cell Physiol 303:C954-962. https://doi.org/10.1152/ajpcell.00030.2012
Heaney RP (2004) Functional indices of vitamin D status and ramifications of vitamin D deficiency. Am J Clin Nutr 80:1706S-S1709. https://doi.org/10.1093/ajcn/80.6.1706S
Jurisic G, Detmar M (2009) Lymphatic endothelium in health and disease. Cell Tissue Res 335:97–108. https://doi.org/10.1007/s00441-008-0644-2
Dejana E, Orsenigo F, Lampugnani MG (2008) The role of adherens junctions and VE-cadherin in the control of vascular permeability. J Cell Sci 121:2115–2122. https://doi.org/10.1242/jcs.017897
Liao S, von der Weid PY (2014) Inflammation-induced lymphangiogenesis and lymphatic dysfunction. Angiogenesis. https://doi.org/10.1007/s10456-014-9416-7
Quan W, Zhang Z, Tian Q et al (2015) A rat model of chronic subdural hematoma: insight into mechanisms of revascularization and inflammation. Brain Res 1625:84–96. https://doi.org/10.1016/j.brainres.2015.08.017
Xiang T, Feng D, Zhang X et al (2022) Effects of increased intracranial pressure on cerebrospinal fluid influx, cerebral vascular hemodynamic indexes, and cerebrospinal fluid lymphatic efflux. J Cereb Blood Flow Metab 42:2287–2302. https://doi.org/10.1177/0271678X221119855
Tammela T, Alitalo K (2010) Lymphangiogenesis: molecular mechanisms and future promise. Cell 140:460–476. https://doi.org/10.1016/j.cell.2010.01.045
Norden PR, Sabine A, Wang Y et al (2020) Shear stimulation of FOXC1 and FOXC2 differentially regulates cytoskeletal activity during lymphatic valve maturation. Elife 9:e53814. https://doi.org/10.7554/eLife.53814
Sabine A, Agalarov Y, Maby-El Hajjami H et al (2012) Mechanotransduction, PROX1, and FOXC2 cooperate to control connexin37 and calcineurin during lymphatic-valve formation. Dev Cell 22:430–445. https://doi.org/10.1016/j.devcel.2011.12.020
Sabine A, Bovay E, Demir CS et al (2015) FOXC2 and fluid shear stress stabilize postnatal lymphatic vasculature. J Clin Invest 125:3861–3877. https://doi.org/10.1172/JCI80454
Oliver G (2004) Lymphatic vasculature development. Nat Rev Immunol 4:35–45. https://doi.org/10.1038/nri1258
Zoccali C, Curatola G, Panuccio V et al (2014) Paricalcitol and endothelial function in chronic kidney disease trial. Hypertens Dallas Tex 64:1005–1011. https://doi.org/10.1161/HYPERTENSIONAHA.114.03748
Battistini C, Ballan R, Herkenhoff ME et al (2020) Vitamin D modulates intestinal microbiota in inflammatory bowel diseases. Int J Mol Sci 22:362. https://doi.org/10.3390/ijms22010362
Jeon S-M, Shin E-A (2018) Exploring vitamin D metabolism and function in cancer. Exp Mol Med 50:1–14. https://doi.org/10.1038/s12276-018-0038-9
Chiang K-C, Chen TC (2013) The anti-cancer actions of vitamin D. Anticancer Agents Med Chem 13:126–139
Bollag WB, Ducote J, Harmon CS (1995) Biphasic effect of 1,25-dihydroxyvitamin D3 on primary mouse epidermal keratinocyte proliferation. J Cell Physiol 163:248–256. https://doi.org/10.1002/jcp.1041630205
Lin M-S (2023) Subdural lesions linking additional intracranial spaces and chronic subdural hematomas: a narrative review with mutual correlation and possible mechanisms behind high recurrence. Diagn Basel Switz 13:235. https://doi.org/10.3390/diagnostics13020235
Pittarella P, Squarzanti DF, Molinari C et al (2015) NO-dependent proliferation and migration induced by Vitamin D in HUVEC. J Steroid Biochem Mol Biol 149:35–42. https://doi.org/10.1016/j.jsbmb.2014.12.012
Cromer WE, Zawieja SD, Tharakan B et al (2014) The effects of inflammatory cytokines on lymphatic endothelial barrier function. Angiogenesis 17:395–406. https://doi.org/10.1007/s10456-013-9393-2
Moskała M, Gościński I, Kałuża J et al (2007) Morphological aspects of the traumatic chronic subdural hematoma capsule: SEM studies. Microsc Microanal 13:211–219. https://doi.org/10.1017/S1431927607070286
Kitazono M, Yokota H, Satoh H et al (2012) Measurement of inflammatory cytokines and thrombomodulin in chronic subdural hematoma. Neurol Med Chir (Tokyo) 52:810–815. https://doi.org/10.2176/nmc.52.810
Funding
This study was funded by the National Natural Science Foundation of China (No. 82271394, No.82071390, No. 81671221).
Author information
Authors and Affiliations
Contributions
Yupeng Chen, Xuanhui Liu and Jiangyuan Yuan contributed equally to this work. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
This research was conducted without any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, Y., Liu, X., Yuan, J. et al. Vitamin D accelerates the subdural hematoma clearance through improving the meningeal lymphatic vessel function. Mol Cell Biochem (2024). https://doi.org/10.1007/s11010-023-04918-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11010-023-04918-6