Abstract
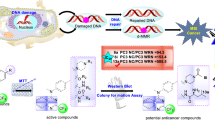
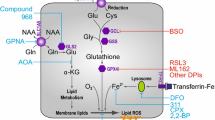
Novel derivatives of aminophenyl-1,4-naphthoquinones, in which a pyrrolidine group was added to the naphthoquinone ring, were synthesized and investigated for the mechanisms of leukemic cell killing. The novel compounds, TW-85 and TW-96, differ in the functional (methyl or hydroxyl) group at the para-position of the aminophenyl moiety. TW-85 and TW-96 were found to induce concentration- and time-dependent apoptotic and/or necrotic cell death in human U937 promonocytic leukemia cells but only TW-96 could also kill K562 chronic myeloid leukemia cells and CCRF-CEM lymphoblastic leukemia cells. Normal peripheral blood mononuclear cells were noticeably less responsive to both compounds than leukemia cells. At low micromolar concentrations used, TW-85 killed U937 cells mainly by inducing apoptosis. TW-96 was a weaker apoptotic agent in U937 cells but proved to be cytotoxic and a stronger inducer of necrosis in all three leukemic cell lines tested. Both compounds induced mitochondrial permeability transition pore opening, cytochrome c release, and caspase activation in U937 cells. Cytotoxicity induced by TW-96, but not by TW-85, was associated with the elevation of the cytosolic levels of reactive oxygen species (ROS). The latter was attenuated by diphenyleneiodonium, indicating that NADPH oxidase was likely to be the source of ROS generation. Activation of p38 MAPK by the two agents appeared to prevent necrosis but differentially affected apoptotic cell death in U937 cells. These results further expand our understanding of the structure–activity relationship of aminophenyl-1,4-naphthoquinones as potential anti-leukemic agents with distinct modes of action.








Similar content being viewed by others
Data availability
All data generated and analyzed in this study are included in this article.
Code availability
Not applicable.
Abbreviations
- AO/EtBr:
-
Acridine orange/ethidium bromide
- DCFH-DA:
-
2′,7′-Dichlorodihydrofluorescein diacetate
- DiOC6 :
-
Dihexylcarbocynaine iodide
- DMF:
-
Dimethyformamide
- DPI:
-
Diphenyleneiodonium
- NQs:
-
Naphthoquinones
- NAC:
-
N-Acetyl cysteine
- PBMC:
-
Peripheral blood mononuclear cells
- PT:
-
Permeability transition
- ROS:
-
Reactive oxygen species
- PTPases:
-
Phosphotyrosine phosphatases
- VDAC:
-
Voltage-dependent anion channe
- Ψ m :
-
Mitochondrial transmembrane potential
References
DiNardo C, Lachowiez C (2019) Acute myeloid leukemia: from mutation profiling to treatment decisions. Curr Hematol Malig Rep 14:386–394. https://doi.org/10.1007/s11899-019-00535-7
Liu H (2021) Emerging agents and regimens for AML. J Hematol Oncol 14:49
Saxena K, Konopleva M (2021) New treatment options for older patients with acute myeloid leukemia. Curr Treat Options Oncol 22:39. https://doi.org/10.1007/s11864-021-00841-4
Qiu HY, Wang PF, Lin HY, Tang CY, Zhu HL, Yang YH (2018) Naphthoquinones: a continuing source for discovery of therapeutic antineoplastic agents. Chem Biol Drug Des 91:681–690. https://doi.org/10.1111/cbdd.13141
Awasthi BP, Kathuria M, Pant G, Kumari N, Mitra K (2016) Plumbagin, a plant-derived naphthoquinone metabolite induces mitochondria mediated apoptosis-like cell death in Leishmania donovani: an ultrastructural and physiological study. Apoptosis 21:941–953. https://doi.org/10.1007/s10495-016-1259-9
Ghosh SK, Ganta A, Spanjaard RA (2018) Discovery and cellular stress pathway analysis of 1,4-naphthoquinone derivatives with novel, highly potent broad-spectrum anticancer activity. J Biomed Sci 25:12. https://doi.org/10.1186/s12929-018-0408-6
Roa-Linares VC, Miranda-Brand Y, Tangarife-Castano V, Ochoa R, Garcia PA, Castro MA, Betancur-Galvis L, San Feliciano A (2019) Anti-herpetic, anti-dengue and antineoplastic activities of simple and heterocycle-fused derivatives of terpenyl-1,4-naphthoquinone and 1,4-anthraquinone. Molecules. https://doi.org/10.3390/molecules24071279
Ren B, Li D, Si L, Ding Y, Han J, Chen X, Zheng Q (2018) Alteronol induces cell cycle arrest and apoptosis via increased reactive oxygen species production in human breast cancer T47D cells. J Pharm Pharmacol 70:516–524. https://doi.org/10.1111/jphp.12879
Liang W, Cai A, Chen G, Xi H, Wu X, Cui J, Zhang K, Zhao X, Yu J, Wei B, Chen L (2016) Shikonin induces mitochondria-mediated apoptosis and enhances chemotherapeutic sensitivity of gastric cancer through reactive oxygen species. Sci Rep 6:38267. https://doi.org/10.1038/srep38267
Wang KJ, Meng XY, Chen JF, Wang KY, Zhou C, Yu R, Ma Q (2021) Emodin induced necroptosis and inhibited glycolysis in the renal cancer cells by enhancing ROS. Oxid Med Cell Longev 2021:8840590. https://doi.org/10.1155/2021/8840590
Trombetti S, Cesaro E, Catapano R, Sessa R, Lo Bianco A, Izzo P, Grosso M (2021) Oxidative stress and ROS-mediated signaling in leukemia: novel promising perspectives to eradicate chemoresistant cells in myeloid leukemia. Int J Mol Sci. https://doi.org/10.3390/ijms22052470
Mattes K, Vellenga E, Schepers H (2019) Differential redox-regulation and mitochondrial dynamics in normal and leukemic hematopoietic stem cells: a potential window for leukemia therapy. Crit Rev Oncol Hematol 144:102814. https://doi.org/10.1016/j.critrevonc.2019.102814
Frydman B, Marton LJ, Sun JS, Neder K, Witiak DT, Liu AA, Wang HM, Mao Y, Wu HY, Sanders MM, Liu LF (1997) Induction of DNA topoisomerase II-mediated DNA cleavage by beta-lapachone and related naphthoquinones. Cancer Res 57:620–627
Collins JA, Osheroff N (2021) 1,2-Naphthoquinone as a poison of human type II topoisomerases. Chem Res Toxicol. https://doi.org/10.1021/acs.chemrestox.0c00492
Byrne FL, Olzomer EM, Marriott GR, Quek LE, Katen A, Su J, Nelson ME, Hart-Smith G, Larance M, Sebesfi VF, Cuff J, Martyn GE, Childress E, Alexopoulos SJ, Poon IK, Faux MC, Burgess AW, Reid G, McCarroll JA, Santos WL, Quinlan KG, Turner N, Fazakerley DJ, Kumar N, Hoehn KL (2020) Phenotypic screen for oxygen consumption rate identifies an anti-cancer naphthoquinone that induces mitochondrial oxidative stress. Redox Biol 28:101374. https://doi.org/10.1016/j.redox.2019.101374
Ma X, Du J, Nakashima I, Nagase F (2002) Menadione biphasically controls JNK-linked cell death in leukemia Jurkat T cells. Antioxid Redox Signal 4:371–378. https://doi.org/10.1089/15230860260196173
Marinho-Filho JD, Bezerra DP, Araujo AJ, Montenegro RC, Pessoa C, Diniz JC, Viana FA, Pessoa OD, Silveira ER, de Moraes MO, Costa-Lotufo LV (2010) Oxidative stress induction by (+)-cordiaquinone J triggers both mitochondria-dependent apoptosis and necrosis in leukemia cells. Chem Biol Interact 183:369–379. https://doi.org/10.1016/j.cbi.2009.11.030
Hallak M, Win T, Shpilberg O, Bittner S, Granot Y, Levy I, Nathan I (2009) The anti-leukaemic activity of novel synthetic naphthoquinones against acute myeloid leukaemia: induction of cell death via the triggering of multiple signalling pathways. Br J Haematol 147:459–470. https://doi.org/10.1111/j.1365-2141.2009.07867.x
Kleih M, Bopple K, Dong M, Gaissler A, Heine S, Olayioye MA, Aulitzky WE, Essmann F (2019) Direct impact of cisplatin on mitochondria induces ROS production that dictates cell fate of ovarian cancer cells. Cell Death Dis 10:851. https://doi.org/10.1038/s41419-019-2081-4
Zou Z, Chang H, Li H, Wang S (2017) Induction of reactive oxygen species: an emerging approach for cancer therapy. Apoptosis 22:1321–1335. https://doi.org/10.1007/s10495-017-1424-9
Kallio A, Zheng A, Dahllund J, Heiskanen KM, Harkonen P (2005) Role of mitochondria in tamoxifen-induced rapid death of MCF-7 breast cancer cells. Apoptosis 10:1395–1410. https://doi.org/10.1007/s10495-005-2137-z
Han XJ, Shi SL, Wei YF, Jiang LP, Guo MY, Wu HL, Wan YY (2017) Involvement of mitochondrial dynamics in the antineoplastic activity of cisplatin in murine leukemia L1210 cells. Oncol Rep 38:985–992. https://doi.org/10.3892/or.2017.5765
Teixeira J, Amorim R, Santos K, Soares P, Datta S, Cortopassi GA, Serafim TL, Sardao VA, Garrido J, Borges F, Oliveira PJ (2018) Disruption of mitochondrial function as mechanism for anti-cancer activity of a novel mitochondriotropic menadione derivative. Toxicology 393:123–139. https://doi.org/10.1016/j.tox.2017.11.014
Cheng G, Hardy M, Topchyan P, Zander R, Volberding P, Cui W, Kalyanaraman B (2020) Potent inhibition of tumour cell proliferation and immunoregulatory function by mitochondria-targeted atovaquone. Sci Rep 10:17872. https://doi.org/10.1038/s41598-020-74808-0
Goleva TN, Lyamzaev KG, Rogov AG, Khailova LS, Epremyan KK, Shumakovich GP, Domnina LV, Ivanova OY, Marmiy NV, Zinevich TV, Esipov DS, Zvyagilskaya RA, Skulachev VP, Chernyak BV (2020) Mitochondria-targeted 1,4-naphthoquinone (SkQN) is a powerful prooxidant and cytotoxic agent. Biochim Biophys Acta Bioenerg 1861:148210. https://doi.org/10.1016/j.bbabio.2020.148210
Wu HL, Fu XY, Cao WQ, Xiang WZ, Hou YJ, Ma JK, Wang Y, Fan CD (2019) Induction of apoptosis in human glioma cells by fucoxanthin via triggering of ROS-mediated oxidative damage and regulation of MAPKs and PI3K-AKT pathways. J Agric Food Chem 67:2212–2219. https://doi.org/10.1021/acs.jafc.8b07126
Li H, Liu Y, Gu Z, Li L, Liu Y, Wang L, Su L (2018) p38 MAPK-MK2 pathway regulates the heat-stress-induced accumulation of reactive oxygen species that mediates apoptotic cell death in glial cells. Oncol Lett 15:775–782. https://doi.org/10.3892/ol.2017.7360
Wang X, Gong Q, Song C, Fang J, Yang Y, Liang X, Huang X, Liu J (2021) Berberine-photodynamic therapy sensitizes melanoma cells to cisplatin-induced apoptosis through ROS-mediated P38 MAPK pathways. Toxicol Appl Pharmacol 418:115484. https://doi.org/10.1016/j.taap.2021.115484
Takata T, Araki S, Tsuchiya Y, Watanabe Y (2020) Oxidative stress orchestrates MAPK and nitric-oxide synthase signal. Int J Mol Sci. https://doi.org/10.3390/ijms21228750
Lee S, Rauch J, Kolch W (2020) Targeting MAPK signaling in cancer: mechanisms of drug resistance and sensitivity. Int J Mol Sci. https://doi.org/10.3390/ijms21031102
Barbosa R, Acevedo LA, Marmorstein R (2021) The MEK/ERK network as a therapeutic target in human cancer. Mol Cancer Res 19:361–374. https://doi.org/10.1158/1541-7786.MCR-20-0687
Kyriakis JM, Avruch J (2012) Mammalian MAPK signal transduction pathways activated by stress and inflammation: a 10-year update. Physiol Rev 92:689–737. https://doi.org/10.1152/physrev.00028.2011
Yue J, Lopez JM (2020) Understanding MAPK signaling pathways in apoptosis. Int J Mol Sci. https://doi.org/10.3390/ijms21072346
Hallak M, Thakur BK, Winn T, Shpilberg O, Bittner S, Granot Y, Levy I, Nathan I (2013) Induction of death of leukemia cells by TW-74, a novel derivative of chloro-naphthoquinone. Anticancer Res 33:183–190
Mahalapbutr P, Leechaisit R, Thongnum A, Todsaporn D, Prachayasittikul V, Rungrotmongkol T, Prachayasittikul S, Ruchirawat S, Prachayasittikul V, Pingaew R (2022) Discovery of anilino-1,4-naphthoquinones as potent EGFR tyrosine kinase inhibitors: synthesis, biological evaluation, and comprehensive molecular modeling. ACS Omega. https://doi.org/10.1021/acsomega.2c01188
Ravichandiran P, Subramaniyan SA, Kim SY, Kim JS, Park BH, Shim KS, Yoo DJ (2019) Synthesis and anticancer evaluation of 1,4-naphthoquinone derivatives containing a phenylaminosulfanyl moiety. ChemMedChem 14:532–544. https://doi.org/10.1002/cmdc.201800749
Li Petri G, Raimondi MV, Spano V, Holl R, Barraja P, Montalbano A (2021) Pyrrolidine in drug discovery: a versatile scaffold for novel biologically active compounds. Top Curr Chem (Cham) 379:34. https://doi.org/10.1007/s41061-021-00347-5
Fostea RM, Arkenau HT (2022) Trifluridine/tipiracil in the treatment of gastric cancer. Future Oncol 18:1511–1517. https://doi.org/10.2217/fon-2021-0754
Aviv Y, Etzion S, Win T, Bittner S, Granot Y (2009) TW96, a synthetic 1,4-naphthoquinone, differentially regulates vascular and endothelial cells survival. Vasc Pharmacol 51:225–235. https://doi.org/10.1016/j.vph.2009.06.007
Muduli S, Golan-Goldhirsh A, Gopas J, Danilenko M (2022) Cytotoxicity of thioalkaloid-enriched nuphar lutea extract and purified 6,6′-dihydroxythiobinupharidine in acute myeloid leukemia cells: the role of oxidative stress and intracellular calcium. Pharmaceuticals (Basel). https://doi.org/10.3390/ph15040410
Zalk R, Israelson A, Garty ES, Azoulay-Zohar H, Shoshan-Barmatz V (2005) Oligomeric states of the voltage-dependent anion channel and cytochrome c release from mitochondria. Biochem J 386:73–83. https://doi.org/10.1042/BJ20041356
Hallak M, Vazana L, Shpilberg O, Levy I, Mazar J, Nathan I (2008) A molecular mechanism for mimosine-induced apoptosis involving oxidative stress and mitochondrial activation. Apoptosis 13:147–155. https://doi.org/10.1007/s10495-007-0156-7
Briehl MM, Tome ME, Wilkinson ST, Jaramillo MC, Lee K (2014) Mitochondria and redox homoeostasis as chemotherapeutic targets. Biochem Soc Trans 42:939–944. https://doi.org/10.1042/BST20140087
Binoy A, Nedungadi D, Katiyar N, Bose C, Shankarappa SA, Nair BG, Mishra N (2019) Plumbagin induces paraptosis in cancer cells by disrupting the sulfhydryl homeostasis and proteasomal function. Chem Biol Interact 310:108733. https://doi.org/10.1016/j.cbi.2019.108733
Vasudevarao MD, Mizar P, Kumari S, Mandal S, Siddhanta S, Swamy MM, Kaypee S, Kodihalli RC, Banerjee A, Naryana C, Dasgupta D, Kundu TK (2014) Naphthoquinone-mediated inhibition of lysine acetyltransferase KAT3B/p300, basis for non-toxic inhibitor synthesis. J Biol Chem 289:7702–7717. https://doi.org/10.1074/jbc.M113.486522
Boulos JC, Rahama M, Hegazy MF, Efferth T (2019) Shikonin derivatives for cancer prevention and therapy. Cancer Lett 459:248–267. https://doi.org/10.1016/j.canlet.2019.04.033
Aminin D, Polonik S (2020) 1,4-Naphthoquinones: some biological properties and application. Chem Pharm Bull (Tokyo) 68:46–57. https://doi.org/10.1248/cpb.c19-00911
Wigdal SS, Kirkland RA, Franklin JL, Haak-Frendscho M (2002) Cytochrome c release precedes mitochondrial membrane potential loss in cerebellar granule neuron apoptosis: lack of mitochondrial swelling. J Neurochem 82:1029–1038. https://doi.org/10.1046/j.1471-4159.2002.01049.x
Roberg K, Johansson U, Ollinger K (1999) Lysosomal release of cathepsin D precedes relocation of cytochrome c and loss of mitochondrial transmembrane potential during apoptosis induced by oxidative stress. Free Radic Biol Med 27:1228–1237. https://doi.org/10.1016/s0891-5849(99)00146-x
Ye YC, Wang HJ, Yu L, Tashiro S, Onodera S, Ikejima T (2012) RIP1-mediated mitochondrial dysfunction and ROS production contributed to tumor necrosis factor alpha-induced L929 cell necroptosis and autophagy. Int Immunopharmacol 14:674–682. https://doi.org/10.1016/j.intimp.2012.08.003
Abdelmohsen K, Gerber PA, von Montfort C, Sies H, Klotz LO (2003) Epidermal growth factor receptor is a common mediator of quinone-induced signaling leading to phosphorylation of connexin-43: role of glutathione and tyrosine phosphatases. J Biol Chem 278:38360–38367. https://doi.org/10.1074/jbc.M306785200
Yoshikawa K, Nigorikawa K, Tsukamoto M, Tamura N, Hazeki K, Hazeki O (2007) Inhibition of PTEN and activation of Akt by menadione. Biochim Biophys Acta 1770:687–693. https://doi.org/10.1016/j.bbagen.2006.12.009
Cuadrado A, Nebreda AR (2010) Mechanisms and functions of p38 MAPK signalling. Biochem J 429:403–417. https://doi.org/10.1042/BJ20100323
Martinez-Limon A, Joaquin M, Caballero M, Posas F, de Nadal E (2020) The p38 pathway: from biology to cancer therapy. Int J Mol Sci. https://doi.org/10.3390/ijms21061913
Kantarjian HM, Short NJ, Fathi AT, Marcucci G, Ravandi F, Tallman M, Wang ES, Wei AH (2021) Acute myeloid leukemia: historical perspective and progress in research and therapy over 5 decades. Clin Lymphoma Myeloma Leuk 21:580–597. https://doi.org/10.1016/j.clml.2021.05.016
Konopleva MY (2021) Mechanisms for resistance in AML insights into molecular pathways mediating resistance to venetoclax. Best Pract Res Clin Haematol 34:101251. https://doi.org/10.1016/j.beha.2021.101251
Kropp EM, Li Q (2022) Mechanisms of resistance to targeted therapies for relapsed or refractory acute myeloid leukemia. Exp Hematol. https://doi.org/10.1016/j.exphem.2022.04.001
Segura-Aguilar J, Jonsson K, Tidefelt U, Paul C (1992) The cytotoxic effects of 5-OH-1,4-naphthoquinone and 5,8-diOH-1,4-naphthoquinone on doxorubicin-resistant human leukemia cells (HL-60). Leuk Res 16:631–637. https://doi.org/10.1016/0145-2126(92)90013-w
Li K, Yang K, Zheng L, Li Y, Wang Q, Lin R, He D (2018) Anti-acute myeloid leukemia activity of 2-chloro-3-alkyl-1,4-naphthoquinone derivatives through inducing mtDNA damage and GSH depletion. Bioorg Med Chem 26:4191–4200. https://doi.org/10.1016/j.bmc.2018.07.010
Coulidiati TH, Dantas BB, Faheina-Martins GV, de Morais Gomes ER, Goncalves JCR, de Araujo DAM (2020) Proapoptotic effects of triazol-1,4-naphthoquinones involve intracellular ROS production and MAPK/ERK pathway in human leukemia cells. Anticancer Agents Med Chem 20:2089–2098. https://doi.org/10.2174/1871520620666200721124221
Coulidiati TH, Dantas BB, Faheina-Martins GV, Goncalves JC, Do Nascimento WS, De Oliveira RN, Camara CA, Oliveira EJ, Lara A, Gomes ER, Araujo DA (2015) Distinct effects of novel naphtoquinone-based triazoles in human leukaemic cell lines. J Pharm Pharmacol 67:1682–1695. https://doi.org/10.1111/jphp.12474
Inagaki R, Ninomiya M, Tanaka K, Koketsu M (2015) Synthesis, characterization, and antileukemic properties of naphthoquinone derivatives of lawsone. ChemMedChem 10:1413–1423. https://doi.org/10.1002/cmdc.201500189
Wiench B, Eichhorn T, Paulsen M, Efferth T (2012) Shikonin directly targets mitochondria and causes mitochondrial dysfunction in cancer cells. Evid Based Complement Alternat Med 2012:726025. https://doi.org/10.1155/2012/726025
Hancio T, Mazzoccoli L, Guimaraes G, Robaina M, Mendonca BDS, Nestal De Moraes G, Monte-Mor B, Mayumi Gutiyama L, De Carvalho LO, Netto CD, Costa PRR, De Faria FCC, Maia RC (2021) The pterocarpanquinone LQB118 compound induces apoptosis of cytarabineresistant acute myeloid leukemia cells. Int J Oncol. https://doi.org/10.3892/ijo.2021.5204
Hamdoun S, Fleischer E, Klinger A, Efferth T (2017) Lawsone derivatives target the Wnt/beta-catenin signaling pathway in multidrug-resistant acute lymphoblastic leukemia cells. Biochem Pharmacol 146:63–73. https://doi.org/10.1016/j.bcp.2017.10.008
Lee MH, Lapidus RG, Ferraris D, Emadi A (2019) Analysis of the mechanisms of action of naphthoquinone-based anti-acute myeloid leukemia chemotherapeutics. Molecules. https://doi.org/10.3390/molecules24173121
Acknowledgements
We thank Suchismita Muduli and Haimantika Seel (Ben-Gurion University of the Negev) for their valuable assistance in performing western blot and flow cytometry assays. We also thank Gulfira Yestemirova (Al-Farabi Kazakh National University) for her help in editing figures included in this article. This work was supported by grants from the Lyonel Israels’ Chair Fund and BGN Technologies (the technology company of Ben-Gurion University of the Negev).
Funding
This work was supported by grants from the Lyonel Israels’ Chair Fund and BGN Technologies (the technology company of Ben-Gurion University of the Negev).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by SB, MH, and TW. The first draft of the manuscript was written by MH and MD. All authors commented on the manuscript and approved for the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interests.
Ethical approval
Samples of peripheral blood were collected from healthy adult volunteers under Approval No. 0328-16-SOR by the institutional Helsinki committee (Soroka University Medical Center, Beer Sheva, Israel).
Consent to participate
All volunteers gave informed consent to participate in this study.
Consent for publication
All authors have agreed to publish this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hallak, M., Danilenko, M., Win, T. et al. Novel pyrrolidine-aminophenyl-1,4-naphthoquinones: structure-related mechanisms of leukemia cell death. Mol Cell Biochem 478, 393–406 (2023). https://doi.org/10.1007/s11010-022-04514-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-022-04514-0