Abstract
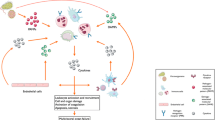
Significant strides have been made in our understanding of the immune system and its role in cardiac transplant rejection. Despite the growing knowledge of immune responses, the mortality rate following cardiac transplantation remains grim. Related to procedural and pathological complications, toll-like receptor (TLR) and damage-associated molecular pattern (DAMP) signaling is the most direct and earliest interface between tissue integration and the innate immune response. This in turn can activate an adaptive immune response that further damages myocardial tissue. Furthermore, relevant literature on the status of DAMPs in the context of heart-transplantation remains limited, warranting further attention in clinical and translational research. This review aims to critically appraise the perspectives, advances, and challenges on DAMP-mediated innate immune response in the immune-mediated rejection of cardiac transplantation. Detailed analysis of the influence of TLR and DAMP signaling in mounting the immune response against the transplanted heart holds promise for improving outcomes through early detection and prevention of varied forms of organ rejection.

Similar content being viewed by others
Data availability
Not applicable; all information is gathered from published articles.
Code availability
Not applicable.
References
World Health Organization. Cardiovascular diseases (CVDs). Fact sheet. https://www.who.int/en/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds). Accessed 11 June 2021
Virani SS, Alonso A, Aparicio HJ et al (2021) Heart disease and stroke statistics—2021 update: a report from the American Heart Association. Circulation. https://doi.org/10.1161/CIR.0000000000000950
Heidenreich PA, Trogdon JG, Khavjou OA et al (2011) Forecasting the future of cardiovascular disease in the United States. Circulation 123:933–944. https://doi.org/10.1161/CIR.0b013e31820a55f5
Taylor CJ, Ordóñez-Mena JM, Roalfe AK et al (2019) Trends in survival after a diagnosis of heart failure in the United Kingdom 2000–2017: population based cohort study. BMJ 364:223. https://doi.org/10.1136/bmj.l223
Alraies MC, Eckman P (2014) Adult heart transplant: indications and outcomes. J Thorac Dis 6:1120–1128. https://doi.org/10.3978/j.issn.2072-1439.2014.06.44
Li J, Li C, Zhuang Q et al (2019) The evolving roles of macrophages in organ transplantation. J Immunol Res 2019:1–11
Fuchs M, Schibilsky D, Zeh W et al (2019) Does the heart transplant have a future? Eur J Cardio-Thorac Surg 55:i38–i48. https://doi.org/10.1093/ejcts/ezz107
Colvin MM, Cook JL, Chang P et al (2015) Antibody-mediated rejection in cardiac transplantation: emerging knowledge in diagnosis and management. Circulation. https://doi.org/10.1161/CIR.0000000000000093
Garces JC, Giusti S, Staffeld-Coit C et al (2017) Antibody-mediated rejection: a review. Ochsner J 17:46–55
Schinstock CA, Mannon RB, Budde K et al (2020) Recommended treatment for antibody-mediated rejection after kidney transplantation: the 2019 expert consensus from the Transplantion Society Working Group. Transplantation 104:911–922. https://doi.org/10.1097/TP.0000000000003095
Patel S (2018) Danger-associated molecular patterns (DAMPs): the derivatives and triggers of inflammation. Curr Allergy Asthma Rep 18:63. https://doi.org/10.1007/s11882-018-0817-3
Todd JL, Palmer SM (2017) Danger signals in regulating the immune response to solid organ transplantation. J Clin Investig 127:2464–2472. https://doi.org/10.1172/JCI90594
Zindel J, Kubes P (2020) DAMPs, PAMPs, and LAMPs in immunity and sterile inflammation. Annu Rev Pathol 15:493–518. https://doi.org/10.1146/annurev-pathmechdis-012419-032847
Dwyer GK, Turnquist HR (2021) Untangling local pro-inflammatory, reparative, and regulatory damage-associated molecular-patterns (DAMPs) pathways to improve transplant outcomes. Front Immunol 12:49. https://doi.org/10.3389/fimmu.2021.611910
Tsilimingas NB (2003) Modification of bicaval anastomosis: an alternative technique for orthotopic cardiac transplantation. Ann Thorac Surg 75:1333–1334. https://doi.org/10.1016/S0003-4975(02)04550-2
Calderwood SK, Gong J, Murshid A (2016) Extracellular HSPs: the complicated roles of extracellular HSPs in immunity. Front Immunol 7:159. https://doi.org/10.3389/fimmu.2016.00159
Calderwood SK, Murshid A, Gong J (2012) Heat shock proteins: conditional mediators of inflammation in tumor immunity. Front Immunol. https://doi.org/10.3389/fimmu.2012.00075
Millington TM, Madsen JC (2009) Innate immunity in heart transplantation. Curr Opin Organ Transplant 14:571–576. https://doi.org/10.1097/MOT.0b013e32832e7158
Murao A, Aziz M, Wang H et al (2021) Release mechanisms of major DAMPs. Apoptosis 26:152–162. https://doi.org/10.1007/s10495-021-01663-3
Yuan S, Liu Z, Xu Z et al (2020) High mobility group box 1 (HMGB1): a pivotal regulator of hematopoietic malignancies. J Hematol Oncol 13:91. https://doi.org/10.1186/s13045-020-00920-3
Parisi L, Toffoli A, Ghezzi B et al (2020) A glance on the role of fibronectin in controlling cell response at biomaterial interface. Jpn Dent Sci Rev 56:50–55. https://doi.org/10.1016/j.jdsr.2019.11.002
Gupta RC, Lall R, Srivastava A, Sinha A (2019) Hyaluronic acid: molecular mechanisms and therapeutic trajectory. Front Vet Sci 6:192. https://doi.org/10.3389/fvets.2019.00192
Simon Davis DA, Parish CR (2013) Heparan sulfate: a ubiquitous glycosaminoglycan with multiple roles in immunity. Front Immunol. https://doi.org/10.3389/fimmu.2013.00470
Jang HS, Shin WJ, Lee JE, Do JT (2017) CpG and non-CpG methylation in epigenetic gene regulation and brain function. Genes 8:148. https://doi.org/10.3390/genes8060148
Kim I-C, Youn J-C, Kobashigawa JA (2018) The past, present and future of heart transplantation. Korean Circ J 48:565–590. https://doi.org/10.4070/kcj.2018.0189
Sarris GE, Moore KA, Schroeder JS et al (1994) Cardiac transplantation: the Stanford experience in the cyclosporine era. J Thorac Cardiovasc Surg 108:240–252. https://doi.org/10.1016/S0022-5223(94)70006-0
Söderlund C, Rådegran G (2015) Immunosuppressive therapies after heart transplantation—the balance between under- and over-immunosuppression. Transplant Rev 29:181–189. https://doi.org/10.1016/j.trre.2015.02.005
Tonsho M, Michel S, Ahmed Z et al (2014) Heart transplantation: challenges facing the field. Cold Spring Harb Perspect Med. https://doi.org/10.1101/cshperspect.a015636
Westerdahl DE, Kobashigawa JA (2019) Heart transplantation for advanced heart failure. Cardiac Intensive Care. https://doi.org/10.1016/B978-0-323-52993-8.00048-5
Gupta T, Krim SR (2019) Cardiac transplantation: update on a road less traveled. Ochsner J 19:369–377. https://doi.org/10.31486/toj.19.0022
Bresnick AR (2018) S100 proteins as therapeutic targets. Biophys Rev 10:1617–1629. https://doi.org/10.1007/s12551-018-0471-y
Rosenberg JH, Rai V, Dilisio MF, Agrawal DK (2017) Damage associated molecular patterns in the pathogenesis of osteoarthritis: potentially novel therapeutic targets. Mol Cell Biochem 434:171–179. https://doi.org/10.1007/s11010-017-3047-4
Andersson U, Yang H, Harris H (2018) Extracellular HMGB1 as a therapeutic target in inflammatory diseases. Expert Opin Ther Targets 22:263–277. https://doi.org/10.1080/14728222.2018.1439924
Hayashi K, Nikolos F, Lee YC et al (2020) Tipping the immunostimulatory and inhibitory DAMP balance to harness immunogenic cell death. Nat Commun 11:6299. https://doi.org/10.1038/s41467-020-19970-9
Yin P, Wang X, Wang S et al (2019) Maresin 1 improves cognitive decline and ameliorates inflammation in a mouse model of Alzheimer’s disease. Front Cell Neurosci 13:466. https://doi.org/10.3389/fncel.2019.00466
Land WG (2020) Use of DAMPs and SAMPs as therapeutic targets or therapeutics: a note of caution. Mol Diagn Ther 24:251–262. https://doi.org/10.1007/s40291-020-00460-z
Varki A (2011) Letter to the Glyco-Forum: since there are PAMPs and DAMPs, there must be SAMPs? Glycan “self-associated molecular patterns” dampen innate immunity, but pathogens can mimic them. Glycobiology 21:1121–1124. https://doi.org/10.1093/glycob/cwr087
Coady A, Nizet V (2016) SAMP-ening down sepsis. Ann Transl Med 4:31–31. https://doi.org/10.21037/atm.2016.11.31
Relja B, Land WG (2020) Damage-associated molecular patterns in trauma. Eur J Trauma Emerg Surg 46:751–775. https://doi.org/10.1007/s00068-019-01235-w
Land WG, Agostinis P, Gasser S et al (2016) Transplantation and damage-associated molecular patterns (DAMPs). Am J Transplant 16:3338–3361. https://doi.org/10.1111/ajt.13963
Sosa RA, Rossetti M, Naini BV et al (2018) Pattern recognition receptor–reactivity screening of liver transplant patients: potential for personalized and precise organ matching to reduce risks of ischemia–reperfusion injury. Ann Surg. https://doi.org/10.1097/SLA.0000000000003085.10.1097/SLA.0000000000003085
Frye CC, Bery AI, Kreisel D, Kulkarni HS (2021) Sterile inflammation in thoracic transplantation. Cell Mol Life Sci 78:581–601. https://doi.org/10.1007/s00018-020-03615-7
Chen GY, Nuñez G (2010) Sterile inflammation: sensing and reacting to damage. Nat Rev Immunol 10:826–837. https://doi.org/10.1038/nri2873
Bhogal RH, Weston CJ, Velduis S et al (2018) The reactive oxygen species-mitophagy signaling pathway regulates liver endothelial cell survival during ischemia/reperfusion injury. Liver Transpl 24:1437–1452. https://doi.org/10.1002/lt.25313
Braza F, Brouard S, Chadban S, Goldstein DR (2016) Role of TLRs and DAMPs in allograft inflammation and transplant outcomes. Nat Rev Nephrol. https://doi.org/10.1038/nrneph.2016.41
Hausenloy DJ, Yellon DM (2013) Myocardial ischemia–reperfusion injury: a neglected therapeutic target. J Clin Investig 123:92–100. https://doi.org/10.1172/JCI62874
Granger DN, Kvietys PR (2015) Reperfusion injury and reactive oxygen species: the evolution of a concept. Redox Biol 6:524–551. https://doi.org/10.1016/j.redox.2015.08.020
Sosa RA, Zarrinpar A, Rossetti M et al (2016) Early cytokine signatures of ischemia/reperfusion injury in human orthotopic liver transplantation. JCI Insight 1(20):e89679. https://doi.org/10.1172/jci.insight.89679
Chen W, Li D (2020) Reactive oxygen species (ROS)-responsive nanomedicine for solving ischemia–reperfusion injury. Front Chem 8:732. https://doi.org/10.3389/fchem.2020.00732
Bulluck H, Rosmini S, Abdel-Gadir A et al (2016) Residual myocardial iron following intramyocardial hemorrhage during the convalescent phase of reperfused ST-segment–elevation myocardial infarction and adverse left ventricular remodeling. Circulation. https://doi.org/10.1161/CIRCIMAGING.116.004940
Yan H-F, Tuo Q-Z, Yin Q-Z, Lei P (2020) The pathological role of ferroptosis in ischemia/reperfusion-related injury. Zool Res 41:220–230. https://doi.org/10.24272/j.issn.2095-8137.2020.042
Li W, Feng G, Gauthier JM et al (2019) Ferroptotic cell death and TLR4/Trif signaling initiate neutrophil recruitment after heart transplantation. J Clin Investig 129(6):2293–2304. https://doi.org/10.1172/JCI126428
Tang D, Kepp O, Kroemer G (2021) Ferroptosis becomes immunogenic: implications for anticancer treatments. Oncoimmunology. https://doi.org/10.1080/2162402X.2020.1862949
Schaefer L (2014) Complexity of danger: the diverse nature of damage-associated molecular patterns. J Biol Chem 289:35237–35245. https://doi.org/10.1074/jbc.R114.619304
Huang Y, Yin H, Han J et al (2007) Extracellular Hmgb1 functions as an innate immune-mediator implicated in murine cardiac allograft acute rejection. Am J Transplant 7:799–808. https://doi.org/10.1111/j.1600-6143.2007.01734.x
Bertheloot D, Latz E (2017) HMGB1, IL-1α, IL-33 and S100 proteins: dual-function alarmins. Cell Mol Immunol 14:43–64. https://doi.org/10.1038/cmi.2016.34
Zhu H, Li J, Wang S, Liu K et al (2013) Hmgb1-TLR4-IL-23-IL-17A axis promote ischemia–reperfusion injury in a cardiac transplantation model. Transplantation 95:1448–1454. https://doi.org/10.1097/TP.0b013e318293b7e1
Zhang A, Mao X, Li L et al (2014) Necrostatin-1 inhibits Hmgb1-IL-23/IL-17 pathway and attenuates cardiac ischemia reperfusion injury. Transpl Int 27:1077–1085. https://doi.org/10.1111/tri.12349
Vergani A, Tezza S, Fotino C et al (2014) The purinergic system in allotransplantation. Am J Transplant 14:507–514. https://doi.org/10.1111/ajt.12567
Vergani A, Tezza S, D’Addio F et al (2013) Long-term heart transplant survival by targeting the ionotropic purinergic receptor P2X7. Circulation 127:463–475. https://doi.org/10.1161/CIRCULATIONAHA.112.123653
Zeiser R, Robson SC, Vaikunthanathan T et al (2016) Unlocking the potential of purinergic signaling in transplantation. Am J Transplant 16:2781–2794. https://doi.org/10.1111/ajt.13801
Silvis MJM, Kaffka Genaamd Dengler SE, Odille CA et al (2020) Damage-associated molecular patterns in myocardial infarction and heart transplantation: the road to translational success. Front Immunol 11:599511. https://doi.org/10.3389/fimmu.2020.599511
Chorawala MR, Prakash P, Doddapattar P et al (2018) Deletion of extra domain A of fibronectin reduces acute myocardial ischemia/reperfusion injury in hyperlipidemic mice by limiting thrombo-inflammation. Thromb Haemost 118:1450–1460. https://doi.org/10.1055/s-0038-1661353
Qin C-Y, Zhang H-W, Gu J et al (2017) Mitochondrial DNA-induced inflammatory damage contributes to myocardial ischemia reperfusion injury in rats: cardioprotective role of epigallocatechin. Mol Med Rep 16:7569–7576. https://doi.org/10.3892/mmr.2017.7515
Chen C, Feng Y, Zou L et al (2014) Role of extracellular RNA and TLR3-Trif signaling in myocardial ischemia–reperfusion injury. J Am Heart Assoc 3:e000683. https://doi.org/10.1161/JAHA.113.000683
Chen HH, Yuan H, Cho H et al (2017) Theranostic nucleic acid binding nanoprobe exerts anti-inflammatory and cytoprotective effects in ischemic injury. Theranostics 7:814–825. https://doi.org/10.7150/thno.17366
Tu G, Zou L, Liu S et al (2016) Long noncoding NONRATT021972 siRNA normalized abnormal sympathetic activity mediated by the upregulation of P2X7 receptor in superior cervical ganglia after myocardial ischemia. Purinergic Signal 12:521–535. https://doi.org/10.1007/s11302-016-9518-3
Gu M, Zheng A-B, Jin J et al (2016) Cardioprotective effects of genistin in rat myocardial ischemia–reperfusion injury studies by regulation of P2X7/NF-κB pathway. Evid Based Complement Altern Med 2016:5381290. https://doi.org/10.1155/2016/5381290
Hackert K, Homann S, Mir S et al (2021) 4-Methylumbelliferone attenuates macrophage invasion and myocardial remodeling in pressure-overloaded mouse hearts. Hypertension 77:1918–1927. https://doi.org/10.1161/HYPERTENSIONAHA.120.15247
Schiopu A, Cotoi OS (2013) S100A8 and S100A9: DAMPs at the crossroads between innate immunity, traditional risk factors, and cardiovascular disease. Med Inflamm 2013:1–10
Moser B, Szabolcs MJ, Ankersmit HJ et al (2007) Blockade of RAGE suppresses alloimmune reactions in vitro and delays allograft rejection in murine heart transplantation. Am J Transplant 7:293–302. https://doi.org/10.1111/j.1600-6143.2006.01617.x
Volz HC, Laohachewin D, Seidel C et al (2012) S100A8/A9 aggravates post-ischemic heart failure through activation of RAGE-dependent NF-κB signaling. Basic Res Cardiol 107:250. https://doi.org/10.1007/s00395-012-0250-z
Wang S, Song R, Wang Z et al (2018) S100A8/A9 in inflammation. Front Immunol. https://doi.org/10.3389/fimmu.2018.01298
Brennan TV, Lunsford KE, Kuo PC (2010) Innate pathways of immune activation in transplantation. J Transplant. https://doi.org/10.1155/2010/826240
Matta BM, Reichenbach DK, Blazar BR, Turnquist HR (2017) Alarmins and their receptors as modulators and indicators of alloimmune responses. Am J Transplant 17:320. https://doi.org/10.1111/ajt.13887
Pankov R, Yamada KM (2002) Fibronectin at a glance. J Cell Sci 115:3861–3863. https://doi.org/10.1242/jcs.00059
Kostrzewa-Nowak D, Ciechanowicz A, Clark JSC, Nowak R (2020) Damage-associated molecular patterns and Th-cell-related cytokines released after progressive effort. J Clin Med 9:876. https://doi.org/10.3390/jcm9030876
Collins SL, Black KE, Chan-Li Y et al (2011) Hyaluronan fragments promote inflammation by down-regulating the anti-inflammatory A2a receptor. Am J Respir Cell Mol Biol 45:675–683. https://doi.org/10.1165/rcmb.2010-0387OC
Hällgren R, Gerdin B, Tengblad A, Tufveson G (1990) Accumulation of hyaluronan (hyaluronic acid) in myocardial interstitial tissue parallels development of transplantation edema in heart allografts in rats. J Clin Investig 85:668–673. https://doi.org/10.1172/JCI114490
Petrey A, de la Motte C (2014) Hyaluronan, a crucial regulator of inflammation. Front Immunol 5:101. https://doi.org/10.3389/fimmu.2014.00101
Ruppert SM, Hawn TR, Arrigoni A et al (2014) Tissue integrity signals communicated by high-molecular weight hyaluronan and the resolution of inflammation. Immunol Res 58:186–192. https://doi.org/10.1007/s12026-014-8495-2
Liu X, Cao H, Li J et al (2017) Autophagy induced by DAMPs facilitates the inflammation response in lungs undergoing ischemia–reperfusion injury through promoting TRAF6 ubiquitination. Cell Death Differ. https://doi.org/10.1038/cdd.2017.1
LaRosa DF, Rahman AH, Turka LA (2007) The innate immune system in allograft rejection and tolerance. J Immunol. https://doi.org/10.4049/jimmunol.178.12.7503
Goldstein DR, Tesar BM, Akira S, Lakkis FG (2003) Critical role of the toll-like receptor signal adaptor protein MyD88 in acute allograft rejection. J Clin Investig. https://doi.org/10.1172/JCI17573
Georgel P (2016) Innate immune receptors in solid organ transplantation. Hum Immunol 77:1071–1075. https://doi.org/10.1016/j.humimm.2016.04.004
Arslan F, Smeets MB, O’Neill LAJ et al (2010) Myocardial ischemia/reperfusion injury is mediated by leukocytic toll-like receptor-2 and reduced by systemic administration of a novel anti-toll-like receptor-2 antibody. Circulation 121:80–90. https://doi.org/10.1161/CIRCULATIONAHA.109.880187
Hennessy EJ, Parker AE, O’Neill LAJ (2010) Targeting toll-like receptors: emerging therapeutics? Nat Rev Drug Discov 9:293–307. https://doi.org/10.1038/nrd3203
Mistry P, Laird MHW, Schwarz RS et al (2015) Inhibition of TLR2 signaling by small molecule inhibitors targeting a pocket within the TLR2 TIR domain. Proc Natl Acad Sci USA 112:5455–5460. https://doi.org/10.1073/pnas.1422576112
Gao H-K, Yin Z, Zhang R-Q et al (2009) GSK-3β inhibitor modulates TLR2/NF-κB signaling following myocardial ischemia–reperfusion. Inflamm Res 58:377–383. https://doi.org/10.1007/s00011-009-0002-1
Shimamoto A, Chong AJ, Yada M et al (2006) Inhibition of toll-like receptor 4 with eritoran attenuates myocardial ischemia–reperfusion injury. Circulation 114:1–270. https://doi.org/10.1161/CIRCULATIONAHA.105.000901
Li C, Ha T, Kelley J et al (2004) Modulating toll-like receptor mediated signaling by (1→3)-β-d-glucan rapidly induces cardioprotection. Cardiovasc Res 61:538–547. https://doi.org/10.1016/j.cardiores.2003.09.007
Bai Y, Li Z, Liu W et al (2019) Biochanin a attenuates myocardial ischemia/reperfusion injury through the TLR4/NF-κB/NLRP3 signaling pathway. Acta Cir Bras. https://doi.org/10.1590/s0102-865020190110000004
Wang Y-H, Chen K-M, Chiu P-S et al (2016) Lumbrokinase attenuates myocardial ischemia–reperfusion injury by inhibiting TLR4 signaling. J Mol Cell Cardiol 99:113–122. https://doi.org/10.1016/j.yjmcc.2016.08.004
Liu C, Chen J, Liu B et al (2018) Role of IL-18 in transplant biology. Eur Cytokine Netw 29:48–51. https://doi.org/10.1684/ecn.2018.0410
He W-T, Zhang L-M, Li C et al (2016) Short-term MyD88 inhibition ameliorates cardiac graft rejection and promotes donor-specific hyporesponsiveness of skin grafts in mice. Transpl Int 29:941–952. https://doi.org/10.1111/tri.12789
Hsieh J-L, Shen P-C, Wu P-T et al (2017) Knockdown of toll-like receptor 4 signaling pathways ameliorate bone graft rejection in a mouse model of allograft transplantation. Sci Rep 7:46050. https://doi.org/10.1038/srep46050
Li W, Hsiao H-M, Higashikubo R et al (2016) CCR2+ macrophages promote neutrophil extravasation through TLR9/MyD88/CXCL5 signaling. JCI Insight 1(12):e87315. https://doi.org/10.1172/jci.insight.87315
Shah KB, Mauro AG, Flattery M et al (2015) Formation of the inflammasome during cardiac allograft rejection. Int J Cardiol 201:328–330. https://doi.org/10.1016/j.ijcard.2015.08.070
Cheung KP, Kasimsetty SG, McKay DB (2013) Innate immunity in donor procurement. Curr Opin Organ Transplant 18:154–160. https://doi.org/10.1097/MOT.0b013e32835e2b0d
Ochando J, Fayad ZA, Madsen JC et al (2020) Trained immunity in organ transplantation. Am J Transplant 20:10–18. https://doi.org/10.1111/ajt.15620
Rose ML (2004) De novo production of antibodies after heart or lung transplantation should be regarded as an early warning system. J Heart Lung Transplant 23:385–395. https://doi.org/10.1016/j.healun.2003.08.028
Acknowledgements
The figure was created using BioRender.com
Funding
The research work of DK Agrawal is supported by NIH-NHLBI Grants R01HL147662 and R01HL144125. The content of this original review article is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Contributions
Conception and design: FGT; Literature search, collection of the scientific information, analysis, and interpretation of the data: AK, DKA, FGT; Drafting of the article: AK, FGT; Critical revision and editing of the article for important intellectual content: FGT, DKA; Final approval of the submitted article: AK, DKA, FGT.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kesler, A., Agrawal, D.K. & Thankam, F.G. Toll-like receptors and damage-associated molecular patterns in the pathogenesis of heart transplant rejection. Mol Cell Biochem 477, 2841–2850 (2022). https://doi.org/10.1007/s11010-022-04491-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-022-04491-4