Abstract
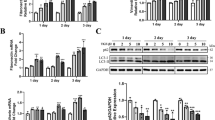
The epithelial–mesenchymal transition (EMT) plays a significant role in fibrosis and migration of lens epithelial cells (LECs), and eventually induces posterior capsule opacification (PCO). In the past, it was generally believed that the TGF-β/Smad pathway regulates lens EMT. A recent study found that attenuated glutathione level promotes LECs EMT via the Wnt/β-catenin pathway, which suggests a more complex pathogenesis of PCO. To test the hypothesis, we used the mouse cataract surgery PCO model and tested both canonical Wnt/β-catenin and TGF-β/Smad signaling pathways. The results showed that both TGF-β/Smad and Wnt/β-catenin pathways were activated during the lens capsule fibrosis. Compared with the freshly isolated posterior capsule, the expression level of phosphorylated Smad2 was highest at day3 and then slightly decreased, but the expression level of Wnt10a gradually increased from day0 to day7. It shows that these two pathways are involved in the lens epithelium’s fibrotic process and may play different roles in different periods. Subsequently, we established oxidative stress-induced EMT model in primary porcine lens epithelial cells and found that both the TGF-β/Smad and Wnt/β-catenin pathways were activated. Further study suggests that block Wnt/β-catenin pathway using XAV939 alone or block TGF-β/Smad pathway using LY2109761 could partially block pLECs fibrosis, but blocking Wnt/β-catenin and TGF-β/Smad pathway using combined XAV939 and LY2109761 could completely block pLECs fibrosis. In conclusion, this study demonstrates that both TGF-β/Smad and canonical Wnt/β-catenin pathways play a significant role in regulating epithelial–mesenchymal transformation of lens epithelial cells but might be in a different stage.





Similar content being viewed by others
Availability of data and material
The analyzed datasets generated during the study are available from the corresponding author on reasonable request.
Abbreviations
- EMT:
-
Epithelial–mesenchymal transition
- LECs:
-
Lens epithelial cells
- pLECs:
-
Porcine lens epithelial cells
- PCO:
-
Posterior capsule opacification
- IOL:
-
Intraocular lens
- H2O2 :
-
Hydrogen peroxide
- BSO:
-
Buthionine sulfoximine
- TGF-β:
-
Transforming growth factor β
- GSK-3β:
-
Glycogen synthase kinase 3β
- APC:
-
Adenomatous polyposis coli
- CK1:
-
Casein kinase 1
- LRP6:
-
Low-density lipoprotein receptor-related protein 6
- α-SMA:
-
α-smooth muscle actin
References
Menon GJ, Wong KK, Bundhun T, Ewings P, Twomey JM (2009) The effect of Nd:YAG laser posterior capsulotomy on stereoacuity. Eye (Lond) 23(1):186–189. https://doi.org/10.1038/sj.eye.6702932
Eldred JA, Dawes LJ, Wormstone IM (2011) The lens as a model for fibrotic disease. Philos Trans R Soc Lond Ser B Biol Sci 366(1568):1301–1319. https://doi.org/10.1098/rstb.2010.0341
Vasavada AR, Praveen MR, Tassignon MJ, Shah SK, Vasavada VA, Vasavada VA, Van Looveren J, De Veuster I, Trivedi RH (2011) Posterior capsule management in congenital cataract surgery. J Cataract Refract Surg 37(1):173–193. https://doi.org/10.1016/j.jcrs.2010.10.036
Von Tress M, Marotta JS, Lane SS, Sarangapani R (2018) A meta-analysis of Nd:YAG capsulotomy rates for two hydrophobic intraocular lens materials. Clin Ophthalmol 12:1125–1136. https://doi.org/10.2147/OPTH.S161380
Ursell PG, Dhariwal M, Majirska K, Ender F, Kalson-Ray S, Venerus A, Miglio C, Bouchet C (2018) Three-year incidence of Nd:YAG capsulotomy and posterior capsule opacification and its relationship to monofocal acrylic IOL biomaterial: a UK Real World Evidence study. Eye (Lond) 32(10):1579–1589. https://doi.org/10.1038/s41433-018-0131-2
Mester U, Sauer T, Kaymak H (2009) Decentration and tilt of a single-piece aspheric intraocular lens compared with the lens position in young phakic eyes. J Cataract Refract Surg 35(3):485–490. https://doi.org/10.1016/j.jcrs.2008.09.028
Cinar E, Yuce B, Aslan F, Erbakan G, Kucukerdonmez C (2019) Intraocular lens tilt and decentration after Nd:YAG laser posterior capsulotomy: femtosecond laser capsulorhexis versus manual capsulorhexis. J Cataract Refract Surg 45(11):1637–1644. https://doi.org/10.1016/j.jcrs.2019.07.017
Whitson JA, Sell DR, Goodman MC, Monnier VM, Fan X (2016) Evidence of dual mechanisms of glutathione uptake in the rodent lens: a novel role for vitreous humor in lens glutathione homeostasis. Invest Ophthalmol Vis Sci 57(8):3914–3925. https://doi.org/10.1167/iovs.16-19592
Ma B, Yang L, Jing R, Liu J, Quan Y, Hui Q, Li J, Qin L, Pei C (2018) Effects of Interleukin-6 on posterior capsular opacification. Exp Eye Res 172:94–103. https://doi.org/10.1016/j.exer.2018.03.013
Wormstone IM (2019) The human capsular bag model of posterior capsule opacification. Eye 34(2):225–231. https://doi.org/10.1038/s41433-019-0680-z
Liu J, Yan XL, Zheng XL, Mei L, Wang S, Han J, Yan H (2017) Electric field exposure promotes epithelial-mesenchymal transition in human lens epithelial cells via integrin β1-FAK signaling. Mol Med Rep 16(4):4008–4014. https://doi.org/10.3892/mmr.2017.7086
Mei L, Yan H, Wang S, Guo C, Zheng X, Yan B, Zhao J, Yang A (2020) Upregulation of miR-630 induced by oxidative damage resists cell migration through targeting ALCAM in human Lens epithelium cells. Curr Eye Res 45(2):153–161. https://doi.org/10.1080/02713683.2019.1656748
Saika S, Okada Y, Miyamoto T, Ohnishi Y, Ooshima A, McAvoy JW (2001) Smad translocation and growth suppression in lens epithelial cells by endogenous TGFbeta2 during wound repair. Exp Eye Res 72(6):679–686. https://doi.org/10.1006/exer.2001.1002
Kubo E, Shibata T, Singh DP, Sasaki H (2018) Roles of TGF beta and FGF signals in the lens: tropomyosin regulation for posterior capsule opacity. Int J Mol Sci 19(10):3093. https://doi.org/10.3390/ijms19103093
Lovicu FJ, Shin EH, McAvoy JW (2016) Fibrosis in the lens. Sprouty regulation of TGFbeta-signaling prevents lens EMT leading to cataract. Exp Eye Res 142:92–101. https://doi.org/10.1016/j.exer.2015.02.004
Marcantonio JM, Syam PP, Liu CSC, Duncan G (2003) Epithelial transdifferentiation and cataract in the human lens. Exp Eye Res 77(3):339–346. https://doi.org/10.1016/s0014-4835(03)00125-8
Raghavan CT, Smuda M, Smith AJ, Howell S, Smith DG, Singh A, Gupta P, Glomb MA, Wormstone IM, Nagaraj RH (2016) AGEs in human lens capsule promote the TGFbeta2-mediated EMT of lens epithelial cells: implications for age-associated fibrosis. Aging Cell 15(3):465–476. https://doi.org/10.1111/acel.12450
Ishibashi T, Hatae T, Inomata H (1994) Collagen types in human posterior capsule opacification. J Cataract Refract Surg 20(6):643–646. https://doi.org/10.1016/s0886-3350(13)80655-4
Linnola RJ, Werner L, Pandey SJ, Escobar-Gomez M, Znoiko SL, Apple DJ (2000) Adhesion of fibronectin, vitronectin, laminin, and collagen type IV to intraocular lens materials in pseudophakic human autopsy eyes. Part 2: Explanted intraocular lenses. J Cataract Refract Surg 26(12):1807–1818. https://doi.org/10.1016/s0886-3350(00)00747-1
Yang H, Wang L, Zhao J, Chen Y, Lei Z, Liu X, Xia W, Guo L, Zhang HT (2015) TGF-beta-activated SMAD3/4 complex transcriptionally upregulates N-cadherin expression in non-small cell lung cancer. Lung Cancer 87(3):249–257. https://doi.org/10.1016/j.lungcan.2014.12.015
Tanaka T, Goto K, Iino M (2017) Sec8 modulates TGF-beta induced EMT by controlling N-cadherin via regulation of Smad3/4. Cell Signal 29:115–126. https://doi.org/10.1016/j.cellsig.2016.10.007
Yao J, Yang W, Liu Y, Sun YX, Jiang Q (2012) Dexamethasone inhibits TGF-beta2-induced migration of human lens epithelial cells: implications for posterior capsule opacification prevention. Mol Med Rep 5(6):1509–1513. https://doi.org/10.3892/mmr.2012.827
Dawes LJ, Sleeman MA, Anderson IK, Reddan JR, Wormstone IM (2009) TGFbeta/Smad4-dependent and -independent regulation of human lens epithelial cells. Invest Ophthalmol Vis Sci 50(11):5318–5327. https://doi.org/10.1167/iovs.08-3223
Taiyab A, Holms J, West-Mays JA (2019) β-catenin/Smad3 interaction regulates transforming growth factor-β-induced epithelial to mesenchymal transition in the lens. Int J Mol Sci 20(9):2078. https://doi.org/10.3390/ijms20092078
Lois N, Taylor J, McKinnon AD, Smith GC, van't Hof R, Forrester JV (2005) Effect of TGF-beta2 and anti-TGF-beta2 antibody in a new in vivo rodent model of posterior capsule opacification. Invest Ophthalmol Vis Sci 46(11):4260–4266. https://doi.org/10.1167/iovs.05-0168
Jiang J, Shihan MH, Wang Y, Duncan MK (2018) Lens epithelial cells initiate an inflammatory response following cataract surgery. Invest Ophthalmol Vis Sci 59(12):4986–4997. https://doi.org/10.1167/iovs.18-25067
Buehl W, Findl O, Neumayer T, Georgopoulos M, Sacu S (2005) Short-term changes in the morphology of posterior capsule opacification. J Cataract Refract Surg 31(5):962–968. https://doi.org/10.1016/j.jcrs.2004.08.051
Neumayer T, Findl O, Buehl W, Sacu S, Menapace R, Georgopoulos M (2005) Long-term changes in the morphology of posterior capsule opacification. J Cataract Refract Surg 31(11):2120–2128. https://doi.org/10.1016/j.jcrs.2005.04.038
Wei Z, Caty J, Whitson J, Zhang AD, Srinivasagan R, Kavanagh TJ, Yan H, Fan X (2017) Reduced glutathione level promotes epithelial-mesenchymal transition in Lens epithelial cells via a Wnt/beta-catenin-mediated pathway: Relevance for cataract therapy. Am J Pathol 187(11):2399–2412. https://doi.org/10.1016/j.ajpath.2017.07.018
Clevers H, Nusse R (2012) Wnt/beta-catenin signaling and disease. Cell 149(6):1192–1205. https://doi.org/10.1016/j.cell.2012.05.012
Guo Y, Xiao L, Sun L, Liu F (2012) Wnt/beta-catenin signaling: a promising new target for fibrosis diseases. Physiol Res 61(4):337–346. https://doi.org/10.33549/physiolres.932289
Chen W, ten Berge D, Brown J, Ahn S, Hu LA, Miller WE, Caron MG, Barak LS, Nusse R, Lefkowitz RJ (2003) Dishevelled 2 recruits beta-arrestin 2 to mediate Wnt5A-stimulated endocytosis of Frizzled 4. Science 301(5638):1391–1394. https://doi.org/10.1126/science.1082808
Arend RC, Londono-Joshi AI, Straughn JM Jr, Buchsbaum DJ (2013) The Wnt/beta-catenin pathway in ovarian cancer: a review. Gynecol Oncol 131(3):772–779. https://doi.org/10.1016/j.ygyno.2013.09.034
Macdonald BT, Semenov MV, He X (2007) SnapShot: Wnt/beta-catenin signaling. Cell 131(6):1204. https://doi.org/10.1016/j.cell.2007.11.036
Craene BD, Berx G (2013) Regulatory networks defining EMT during cancer initiation and progression. Nat Rev Cancer 13(2):97–110. https://doi.org/10.1038/nrc3447
Anastas JN, Moon RT (2013) WNT signalling pathways as therapeutic targets in cancer. Nat Rev Cancer 13(1):11–26. https://doi.org/10.1038/nrc3419
Nishikawa K, Osawa Y, Kimura K (2018) Wnt/beta-catenin signaling as a potential target for the treatment of liver cirrhosis using antifibrotic drugs. Int J Mol Sci 19(10):3103. https://doi.org/10.3390/ijms19103103
Feng Y, Ren J, Gui Y, Wei W, Shu B, Lu Q, Xue X, Sun X, He W, Yang J, Dai C (2018) Wnt/beta-catenin-promoted macrophage alternative activation contributes to kidney fibrosis. J Am Soc Nephrol 29(1):182–193. https://doi.org/10.1681/ASN.2017040391
Xu L, Cui WH, Zhou WC, Li DL, Li LC, Zhao P, Mo XT, Zhang Z, Gao J (2017) Activation of Wnt/beta-catenin signalling is required for TGF-beta/Smad2/3 signalling during myofibroblast proliferation. J Cell Mol Med 21(8):1545–1554. https://doi.org/10.1111/jcmm.13085
Huang SM, Mishina YM, Liu S, Cheung A, Stegmeier F, Michaud GA, Charlat O, Wiellette E, Zhang Y, Wiessner S, Hild M, Shi X, Wilson CJ, Mickanin C, Myer V, Fazal A, Tomlinson R, Serluca F, Shao W, Cheng H, Shultz M, Rau C, Schirle M, Schlegl J, Ghidelli S, Fawell S, Lu C, Curtis D, Kirschner MW, Lengauer C, Finan PM, Tallarico JA, Bouwmeester T, Porter JA, Bauer A, Cong F (2009) Tankyrase inhibition stabilizes axin and antagonizes Wnt signalling. Nature 461(7264):614–620. https://doi.org/10.1038/nature08356
Wang Y, Mahesh P, Wang Y, Novo SG, Shihan MH, Hayward-Piatkovskyi B, Duncan MK (2018) Spatiotemporal dynamics of canonical Wnt signaling during embryonic eye development and posterior capsular opacification (PCO). Exp Eye Res 175:148–158. https://doi.org/10.1016/j.exer.2018.06.020
Saika S, Miyamoto T, Ishida I, Shirai K, Ohnishi Y, Ooshima A, McAvoy JW (2002) TGFbeta-Smad signalling in postoperative human lens epithelial cells. Br J Ophthalmol 86(12):1428–1433. https://doi.org/10.1136/bjo.86.12.1428
Tiwari A, Ram J, Luthra-Guptasarma M (2014) Targeting the fibronectin type III repeats in tenascin-C inhibits epithelial-mesenchymal transition in the context of posterior capsular opacification. Invest Ophthalmol Vis Sci 56(1):272–283. https://doi.org/10.1167/iovs.14-14934
Ma B, Jing R, Liu J, Qi T, Pei C (2019) Gremlin is a potential target for posterior capsular opacification. Cell Cycle 18(15):1714–1726. https://doi.org/10.1080/15384101.2019.1632125
Wernecke L, Keckeis S, Reichhart N, Strauss O, Salchow DJ (2018) Epithelial-mesenchymal transdifferentiation in pediatric lens epithelial cells. Invest Ophthalmol Vis Sci 59(15):5785–5794. https://doi.org/10.1167/iovs.18-23789
Piersma B, Bank RA, Boersema M (2015) Signaling in fibrosis: TGF-β, WNT, and YAP/TAZ converge. Front Med (Lausanne) 2:59. https://doi.org/10.3389/fmed.2015.00059
Liu T, Zhang L, Wang Y, Zhang H, Li L, Bao X (2017) Dickkopf-1 inhibits Wnt3a-induced migration and epithelial-mesenchymal transition of human lens epithelial cells. Exp Eye Res 161:43–51. https://doi.org/10.1016/j.exer.2017.06.001
Petersen A, Zetterberg M (2016) The immunoproteasome in human lens epithelial cells during oxidative stress. Invest Ophthalmol Vis Sci 57(11):5038–5045. https://doi.org/10.1167/iovs.16-19536
Cheresh P, Kim SJ, Tulasiram S, Kamp DW (2013) Oxidative stress and pulmonary fibrosis. Biochim Biophys Acta 1832(7):1028–1040. https://doi.org/10.1016/j.bbadis.2012.11.021
Cipak Gasparovic A, Milkovic L, Dandachi N, Stanzer S, Pezdirc I, Vrancic J, Sitic S, Suppan C, Balic M (2019) Chronic oxidative stress promotes molecular changes associated with epithelial mesenchymal transition, nrf2, and breast cancer stem cell phenotype. Antioxidants (Basel) 8(12):633. https://doi.org/10.3390/antiox8120633
Chang YW, Singh KP (2019) Nicotine-induced oxidative stress contributes to EMT and stemness during neoplastic transformation through epigenetic modifications in human kidney epithelial cells. Toxicol Appl Pharmacol 374:65–76. https://doi.org/10.1016/j.taap.2019.04.023
Huang W, Yu D, Wang M, Han Y, Lin J, Wei D, Cai J, Li B, Chen P, Zhang X (2020) ITGBL1 promotes cell migration and invasion through stimulating the TGF-beta signalling pathway in hepatocellular carcinoma. Cell Prolif 53(7):e12836. https://doi.org/10.1111/cpr.12836
Shetti D, Zhang B, Fan C, Mo C, Lee BH, Wei K (2019) Low dose of paclitaxel combined with XAV939 attenuates metastasis, angiogenesis and growth in breast cancer by suppressing Wnt signaling. Cells 8(8):892. https://doi.org/10.3390/cells8080892
Kim S, Lee J, Jeon M, Nam SJ, Lee JE (2015) Elevated TGF-beta1 and -beta2 expression accelerates the epithelial to mesenchymal transition in triple-negative breast cancer cells. Cytokine 75(1):151–158. https://doi.org/10.1016/j.cyto.2015.05.020
Zhang J, Tian XJ, Xing J (2016) Signal transduction pathways of EMT induced by TGF-beta, SHH, and WNT and their crosstalks. J Clin Med 5(4):41. https://doi.org/10.3390/jcm5040041
Dzialo E, Tkacz K, Blyszczuk P (2018) Crosstalk between the TGF-beta and WNT signalling pathways during cardiac fibrogenesis. Acta Biochim Pol 65(3):341–349. https://doi.org/10.18388/abp.2018_2635
Taiyab A, Korol A, Deschamps PA, West-Mays JA (2016) β-catenin/CBP-dependent signaling regulates TGF-β-induced epithelial to mesenchymal transition of lens epithelial cells. Invest Ophthalmol Vis Sci 57(13):5736–5747. https://doi.org/10.1167/iovs.16-20162
Falk S, Wurdak H, Ittner LM, Ille F, Sumara G, Schmid MT, Draganova K, Lang KS, Paratore C, Leveen P, Suter U, Karlsson S, Born W, Ricci R, Gotz M, Sommer L (2008) Brain area-specific effect of TGF-beta signaling on Wnt-dependent neural stem cell expansion. Cell Stem Cell 2(5):472–483. https://doi.org/10.1016/j.stem.2008.03.006
Wang H, Rajan S, Liu G, Chakrabarty S (2008) Transforming growth factor beta suppresses beta-catenin/Wnt signaling and stimulates an adhesion response in human colon carcinoma cells in a Smad4/DPC4 independent manner. Cancer Lett 264(2):281–287. https://doi.org/10.1016/j.canlet.2008.01.039
Acknowledgements
Special thanks to Professor Xinjun Fan of Department of Cellular and Anatomy, James and Jean Culver Vision Discovery Institute, Medical College of Georgia, Augusta University, GA, USA, for his assistance with the experiments and valuable discussion. Thanks to the Chongqing Key Laboratory of Ophthalmology (Chongqing, China) for providing the experiment platform.
Funding
This work was supported by National Natural Science Foundation of China (NO: 81873674).
Author information
Authors and Affiliations
Contributions
HY conceived the research; XC acquired the data and wrote the manuscript; YC, GL, and YB analyzed the data; XZ supervised the research.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest/competing interests.
Ethical approval
All animal experiments performed in this study were approved by the Ethics Committee for Animal Experimentation of Chongqing Medical University.
Consent to participate
Not applicable.
Consent for publication
All authors approved to submit this version to this publication.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, X., Yan, H., Chen, Y. et al. Moderate oxidative stress promotes epithelial–mesenchymal transition in the lens epithelial cells via the TGF-β/Smad and Wnt/β-catenin pathways. Mol Cell Biochem 476, 1631–1642 (2021). https://doi.org/10.1007/s11010-020-04034-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-020-04034-9