Abstract
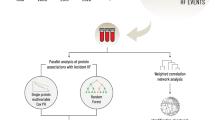
Stroke is a common disorder with significant morbidity and mortality, and complex aetiology involving both environmental and genetic risk factors. Although some of the major risk factors for stoke, such as smoking and hypertension, are well-documented, the underlying genetic and detailed molecular mechanisms remain elusive. Exploring the relevant biochemical pathways may contribute to the clinical diagnosis of stroke and shed light on its aetiology. A comparative proteomic analysis of blood serum of a pair of monozygotic (MZ) twins discordant for ischaemic stroke (IS) was performed using a label-free quantitative proteomics approach. To overcome the limit of reproducibility in the serum preparation, two separate runs were performed, each consisting of three technical replicates per sample. Biological processes associated with proteins differentially expressed between the twins were explored with gene ontology (GO) classification using the functional analysis tool g:Profiler. ANOVA test performed in Progenesis LC-MS identified 179 (run 1) and 209 (run 2) proteins as differentially expressed between the affected and unaffected twin (p < 0.05). Furthermore, the level of serum fibulin 1, an extracellular matrix protein associated with arterial stiffness, was on average 13.37-fold higher in the affected twin. Each dataset was then analysed independently, and the proteins were classified according to GO terms. The categories overrepresented in the affected twin predominantly corresponded to stroke-relevant processes, including wound healing, blood coagulation and haemostasis, with a high proportion of the proteins overexpressed in the affected twin associated with these terms. By contrast, in the unaffected twin diagnosed with atopic dermatitis, there were increased levels of keratin proteins and GO terms associated with skin development. The identification of cellular pathways enriched in IS as well as the upregulation of fibulin 1 sheds new light on the underlying disease-causing mechanisms at the molecular level. Our findings of distinct proteomic signatures associated with IS and atopic dermatitis suggest proteomic profiling could be used as a general approach for improved diagnostic, prognostic and therapeutic strategies.

Similar content being viewed by others
References
Raffeld MR, Debette S, Woo D (2016) International stroke genetics consortium update. Stroke 47:1144–1145. https://doi.org/10.1161/STROKEAHA.116.012682
Goodwin S, McPherson JD, McCombie WR (2016) Coming of age: ten years of next-generation sequencing technologies. Nat Rev Genet 17:333–351. https://doi.org/10.1038/nrg.2016.49
Lever NM, Nyström KV, Schindler JL et al (2013) Missed opportunities for recognition of ischemic stroke in the emergency department. J Emerg Nurs 39:434–439. https://doi.org/10.1016/j.jen.2012.02.011
Makris K, Haliassos A, Chondrogianni M, Tsivgoulis G (2018) Blood biomarkers in ischemic stroke: potential role and challenges in clinical practice and research. Crit Rev Clin Lab Sci 55:294–328. https://doi.org/10.1080/10408363.2018.1461190
Jickling GC, Sharp FR (2015) Biomarker panels in ischemic stroke. Stroke 46:915–920. https://doi.org/10.1161/STROKEAHA.114.005604
Zwijnenburg PJG, Meijers-Heijboer H, Boomsma DI (2010) Identical but not the same: the value of discordant monozygotic twins in genetic research. Am J Med Genet Part B. https://doi.org/10.1002/ajmg.b.31091
Vadgama N, Gaze D, Ranson J et al (2015) Elevated γ-glutamyltransferase and erythrocyte sedimentation rate in ischemic stroke in discordant monozygotic twin study. Int J Stroke 10:. https://doi.org/10.1111/ijs.12440
Reimand J, Kull M, Peterson H et al (2007) g:Profiler–a web-based toolset for functional profiling of gene lists from large-scale experiments. Nucleic Acids Res 35:W193–W200. https://doi.org/10.1093/nar/gkm226
Smoot ME, Ono K, Ruscheinski J et al (2011) Cytoscape 2.8: new features for data integration and network visualization. Bioinformatics 27:431–432. https://doi.org/10.1093/bioinformatics/btq675
Walker HK, Hall WD, Hurst JW (1990) Clinical Methods. Butterworths
Connor DE, Chaitanya GV, Chittiboina P et al (2017) Variations in the cerebrospinal fluid proteome following traumatic brain injury and subarachnoid hemorrhage. Pathophysiology 24:169–183. https://doi.org/10.1016/j.pathophys.2017.04.003
Huang P, Lo L-H, Chen Y-C et al (2009) Serum free hemoglobin as a novel potential biomarker for acute ischemic stroke. J Neurol 256:625–631. https://doi.org/10.1007/s00415-009-0133-x
Nezu T, Hosomi N, Aoki S et al (2013) Alpha2-macroglobulin as a promising biomarker for cerebral small vessel disease in acute ischemic stroke patients. J Neurol 260:2642–2649. https://doi.org/10.1007/s00415-013-7040-x
Hanson E, Kanse SM, Joshi A et al (2012) Plasma factor VII-activating protease antigen levels and activity are increased in ischemic stroke. J Thromb Haemost 10:848–856. https://doi.org/10.1111/j.1538-7836.2012.04692.x
Ziegler G, Harhausen D, Schepers C et al (2007) TLR2 has a detrimental role in mouse transient focal cerebral ischemia. Biochem Biophys Res Commun 359:574–579. https://doi.org/10.1016/j.bbrc.2007.05.157
Füst G, Munthe-Fog L, Illes Z et al (2011) Low ficolin-3 levels in early follow-up serum samples are associated with the severity and unfavorable outcome of acute ischemic stroke. J Neuroinflammation 8:185. https://doi.org/10.1186/1742-2094-8-185
Carcaillon L, Alhenc-Gelas M, Bejot Y et al (2011) Increased thrombin generation is associated with acute ischemic stroke but not with coronary heart disease in the elderly. Arterioscler Thromb Vasc Biol 31:1445–1451. https://doi.org/10.1161/ATVBAHA.111.223453
Cangemi C, Skov V, Poulsen MK et al (2011) Fibulin-1 is a marker for arterial extracellular matrix alterations in type 2 diabetes. Clin Chem 57:1556–1565. https://doi.org/10.1373/clinchem.2011.162966
López-Farré AJ, Zamorano-León JJ, Segura A et al (2012) Plasma desmoplakin I biomarker of vascular recurrence after ischemic stroke. J Neurochem 121:314–325. https://doi.org/10.1111/j.1471-4159.2012.07683.x
Chao J, Bledsoe G, Yin H, Chao L (2006) The tissue kallikrein-kinin system protects against cardiovascular and renal diseases and ischemic stroke independently of blood pressure reduction. Biol Chem 387:665–675. https://doi.org/10.1515/BC.2006.085
Garrod D, Chidgey M (2008) Desmosome structure, composition and function. Biochim Biophys Acta 1778:572–587. https://doi.org/10.1016/j.bbamem.2007.07.014
Gori AM, Giusti B, Piccardi B et al (2017) Inflammatory and metalloproteinases profiles predict three-month poor outcomes in ischemic stroke treated with thrombolysis. J Cereb Blood Flow Metab 37:3253–3261. https://doi.org/10.1177/0271678X17695572
Kannemeier C, Al-Fakhri N, Preissner KT, Kanse SM (2004) Factor VII-activating protease (FSAP) inhibits growth factor-mediated cell proliferation and migration of vascular smooth muscle cells. FASEB J 18:728–730. https://doi.org/10.1096/fj.03-0898fje
Willeit J, Kiechl S, Weimer T et al (2003) Marburg I polymorphism of factor VII—activating protease: a prominent risk predictor of carotid stenosis. Circulation 107:667–670
Wang L, Luo H, Chen X et al (2014) Functional characterization of S100A8 and S100A9 in altering monolayer permeability of human umbilical endothelial cells. PLoS ONE 9:e90472. https://doi.org/10.1371/journal.pone.0090472
Schiopu A, Cotoi OS (2013) S100A8 and S100A9: DAMPs at the crossroads between innate immunity, traditional risk factors, and cardiovascular disease. Mediators Inflamm 2013:828354. https://doi.org/10.1155/2013/828354
Chao J, Bledsoe G, Chao L (2016) Protective role of Kallistatin in vascular and organ injury. Hypertens (Dallas, Tex 1979) 68:533–541. https://doi.org/10.1161/HYPERTENSIONAHA.116.07861
Stokes DL (2007) Desmosomes from a structural perspective. Curr Opin Cell Biol 19:565–571. https://doi.org/10.1016/j.ceb.2007.09.003
Yang Z, Bowles NE, Scherer SE et al (2006) Desmosomal Dysfunction due to Mutations in Desmoplakin Causes Arrhythmogenic Right Ventricular Dysplasia/Cardiomyopathy. Circ Res 99:646–655. https://doi.org/10.1161/01.RES.0000241482.19382.c6
Argraves WS, Tran H, Burgess WH, Dickerson K (1990) Fibulin is an extracellular matrix and plasma glycoprotein with repeated domain structure. J Cell Biol 111:3155–3164
Liu G, Cooley MA, Jarnicki AG et al (2016) Fibulin-1 regulates the pathogenesis of tissue remodeling in respiratory diseases. JCI Insight. https://doi.org/10.1172/jci.insight.86380
Godyna S, Diaz-Ricart M, Argraves WS (1996) Fibulin-1 mediates platelet adhesion via a bridge of fibrinogen. Blood 88:2569–2577
Al Maskari R, McEniery CM et al (2018) The matrix proteins aggrecan and fibulin-1 play a key role in determining aortic stiffness. Sci Rep 8:8550. https://doi.org/10.1038/s41598-018-25851-5
Lee Y-B, Park J-H, Kim E et al (2014) Arterial stiffness and functional outcome in acute ischemic stroke. J Cerebrovasc Endovasc Neurosurg 16:11–19. https://doi.org/10.7461/jcen.2014.16.1.11
Acknowledgements
We would like to thank the FingerPrints Proteomics Facility, School of Life Sciences, University of Dundee for the proteomic and mass spectrometry analysis, and The Leverhulme Trade Charities Trust for a bursary to NV.
Funding
RCL: Parkinson’s UK Grant G-1307, British Heart Foundation (RG/13/5/30112), the National Institute for Health Research University College London Hospitals Biomedical Research Centre.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Vadgama, N., Lamont, D., Hardy, J. et al. Distinct proteomic profiles in monozygotic twins discordant for ischaemic stroke. Mol Cell Biochem 456, 157–165 (2019). https://doi.org/10.1007/s11010-019-03501-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-019-03501-2