Abstract
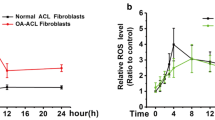
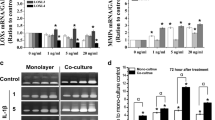
The adult human anterior cruciate ligament (ACL) has a poor functional healing response, whereas the medial collateral ligament (MCL) does not. The difference in intrinsic properties of these ligament cells can be due to their different response to their located microenvironment. Hypoxia is a key environmental regulator after ligament injury. In this study, we investigated the differential response of ACL and MCL fibroblasts to hypoxia on hypoxia-inducible factor-1α, vascular endothelial growth factor, and matrix metalloproteinase-2 (MMP-2) expression. Our results show that ACL cells responded to hypoxia by up-regulating the HIF-1α expression significantly as compared to MCL cells. We also observed that in MCL fibroblasts response to hypoxia resulted in increase in expression of VEGF as compared to ACL fibroblasts. After hypoxia treatment, mRNA and protein levels of MMP-2 increased in both ACL and MCL. Furthermore we found in ACL pro-MMP-2 was converted more into active form. However, hypoxia decreased the percentage of wound closure for both ligament cells and had a greater effect on ACL fibroblasts. These results demonstrate that ACL and MCL fibroblasts respond differently under the hypoxic conditions suggesting that these differences in intrinsic properties may contribute to their different healing responses and abilities.





Similar content being viewed by others
References
Woo SL, Chan SS, Yamaji T (1997) Biomechanics of knee ligament healing, repair and reconstruction. J Biomech 30:431–439
Louboutin H, Debarge R, Richou J et al (2009) Osteoarthritis in patients with anterior cruciate ligament rupture: a review of risk factors. Knee 16:239–244
Oiestad BE, Engebretsen L, Storheim K et al (2009) Knee osteoarthritis after anterior cruciate ligament injury a systematic review. Am J Sports Med 37:1434–1443
Yang L, Tsai CM, Hsieh AH et al (1999) Adhesion strength differential of human ligament fibroblasts to collagen types I and III. J Orthop Res 17:755–762
Witkowski J, Yang L, Wood DJ et al (1997) Migration and healing of ligament cells under inflammatory conditions. J Orthop Res 15:269–277
Sung KL, Yang L, Whittemore DE et al (1996) The differential adhesion forces of anterior cruciate and medial collateral ligament fibroblasts: effects of tropomodulin, talin, vinculin, and alpha-actinin. Proc Natl Acad Sci USA 93:9182–9187
Zhang J, Yang L, Tang Z et al (2009) Expression of MMPs and TIMPs family in human ACL and MCL Fibroblasts. Connect Tissue Res 50:7–13
Tang Z, Yang L, Wang Y et al (2009) Contributions of different intraarticular tissues to the acute phase elevation of synovial fluid MMP-2 following rat ACL rupture. J Orthop Res 27:243–248
Wang P, Yang L, You X et al (2009) Mechanical stretch regulates the expression of matrix metalloproteinase in rheumatoid arthritis fibroblast-like synoviocytes. Connect Tissue Res 50:98–109
Wang Y, Yang L, Zhang J et al (2010) Differential MMP-2 activity induced by mechanical compression and inflammatory factors in human synoviocytes. Mol Cell Biomech 7:105–114
Zhou D, Lee HS, Villarreal F et al (2005) Differential MMP-2 activity of ligament cells under mechanical stretch injury: an in vitro study on human ACL and MCL fibroblasts. J Orthop Res 23:949–957
Hsieh AH, Tsai CM, Ma QJ et al (2000) Time-dependent increases in type-III collagen gene expression in medical collateral ligament fibroblasts under cyclic strains. J Orthop Res 18:220–227
Tang Z, Yang L, Xue R et al (2009) Differential expression of matrix metalloproteinases and tissue inhibitors of metalloproteinases in anterior cruciate ligament and medial collateral ligament fibroblasts after a mechanical injury: involvement of the p65 subunit of NF-kappaB. Wound Repair Regen 17:709–716
Gaber T, Dziurla R, Tripmacher R et al (2005) Hypoxia inducible factor (HIF) in rheumatology: low O2! See what HIF can do! Ann Rheum Dis 64:971–980
Kofoed H (1986) Synovitis causes hypoxia and acidity in synovial fluid and subchondral bone. Injury 17:391–394
Cha HS, Ahn KS, Jeon CH et al (2003) Influence of hypoxia on the expression of matrix metalloproteinase-1,-3 and tissue inhibitor of metalloproteinase-1 in rheumatoid synovial fibroblasts. Clin Exp Rheumatol 21:593–598
Semenza GL (2003) Targeting HIF-1 for cancer therapy. Nat Rev Cancer 3:721–732
Petersen W, Tillmann B (1999) Structure and vascularization of the cruciate ligaments of the human knee joint. Anat Embryol (Berl) 200:325–334
Warner TD, Mitchell JA (2003) HIF, stretching to get control of VEGF. Clin Sci (Lond) 105:393–394
Hong KH, Yoo SA, Kang SS et al (2006) Hypoxia induces expression of connective tissue growth factor in scleroderma skin fibroblasts. Clin Exp Immunol 146:362–370
Petersen W, Varoga D, Zantop T et al (2004) Cyclic strain influences the expression of the vascular endothelial growth factor (VEGF) and the hypoxia inducible factor 1 alpha (HIF-1 alpha) in tendon fibroblasts. J Orthop Res 22:847–853
Wang Y, Tang Z, Xue R et al (2011) TGF-beta1 promoted MMP-2 mediated wound healing of anterior cruciate ligament fibroblasts through NF-kappaB. Connect Tissue Res 52:218–225
Wang Y, Tang Z, Xue R et al (2011) Combined effects of TNF-alpha, IL-1beta, and HIF-1alpha on MMP-2 production in ACL fibroblasts under mechanical stretch: an in vitro study. J Orthop Res 29:1008–1014
Johnstone CC, Farley A (2005) The physiological basics of wound healing. Nurs Stand 19: 59-65; quiz 66
Tandara AA, Mustoe TA (2004) Oxygen in wound healing—more than a nutrient. World J Surg 28:294–300
Ardyanto TD, Osaki M, Tokuyasu N et al (2006) CoCl2-induced HIF-1alpha expression correlates with proliferation and apoptosis in MKN-1 cells: a possible role for the PI3K/Akt pathway. Int J Oncol 29:549–555
Semenza GL (2001) Hypoxia-inducible factor 1: oxygen homeostasis and disease pathophysiology. Trends Mol Med 7:345–350
Finger EC, Giaccia AJ (2010) Hypoxia, inflammation, and the tumor microenvironment in metastatic disease. Cancer Metastasis Rev 29:285–293
Petersen W, Pufe T, Zantop T et al (2003) Hypoxia and PDGF have a synergistic effect that increases the expression of the angiogenetic peptide vascular endothelial growth factor in Achilles tendon fibroblasts. Arch Orthop Trauma Surg 123:485–488
Kondo S, Kubota S, Shimo T et al (2002) Connective tissue growth factor increased by hypoxia may initiate angiogenesis in collaboration with matrix metalloproteinases. Carcinogenesis 23:769–776
Yoshikawa T, Tohyama H, Katsura T et al (2006) Effects of local administration of vascular endothelial growth factor on mechanical characteristics of the semitendinosus tendon graft after anterior cruciate ligament reconstruction in sheep. Am J Sports Med 34:1918–1925
Eltzschig HK, Carmeliet P (2011) Hypoxia and inflammation. N Engl J Med 364:656–665
Murata M, Yudoh K, Nakamura H et al (2006) Distinct signaling pathways are involved in hypoxia- and IL-1-induced VEGF expression in human articular chondrocytes. J Orthop Res 24:1544–1554
Olszewska-Pazdrak B, Hein TW, Olszewska P et al (2009) Chronic hypoxia attenuates VEGF signaling and angiogenic responses by downregulation of KDR in human endothelial cells. Am J Physiol Cell Physiol 296:C1162–C1170
Acknowledgments
This study was supported by the Innovation and Attracting Talents Program for College and University (‘111’ Project) (B06023), The Fundamental Research Funds for the Central Universities (CDJXS11231176), National Natural Science Foundation of China (11032012), and Key Science and Technology Program of CQ CSTC (2009AA5045).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, Y., Tang, Z., Xue, R. et al. Differential response to CoCl2-stimulated hypoxia on HIF-1α, VEGF, and MMP-2 expression in ligament cells. Mol Cell Biochem 360, 235–242 (2012). https://doi.org/10.1007/s11010-011-1061-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-011-1061-5