Abstract
Objective
In-hospital formula supplementation places infants at risk for early breastfeeding cessation. The study’s aim was to identify predictive and protective factors for in-hospital formula supplementation in individuals documented as wanting to exclusively breastfeed and residing in a geographic region with adverse social determinants of health and low breastfeeding rates. Additionally, we wished to determine if lactation consultation served as a protective factor against supplementation.
Methods
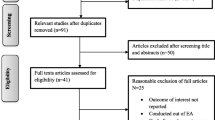
In this cross-sectional study, we retrospectively reviewed 500 randomly selected charts of newborns born in a 12 month period at a regional tertiary care hospital. We included healthy, full-term neonates having a recorded maternal decision to exclusively breastfeed. Maternal-newborn dyad characteristics were compared between those exclusively breastfeeding and those with in-hospital formula supplementation.
Results
Of the 500 charts, 70% of individuals desired to exclusively breastfeed. Overall, 41% of breastfed newborns were supplemented with formula before discharge, and 32% of women met with lactation consultants prior to supplementation. No statistically significant association was present between exclusive breastfeeding at discharge and meeting with a hospital lactation consultant (p = 0.55). When controlling for the confounders of maternal demographics and lactation consultation, significant associations with formula supplementation included Cesarean delivery (odd ratio: 2.08, 95% confidence interval: 1.04–4.16), primiparity (2.48, 1.27–4.87), and high school level of education (2.78, 1.33–5.78).
Conclusions
Maternal characteristics of high school level educational, primiparity, and Caesarean delivery place individuals at risk for in-hospital formula supplementation in individuals wishing to exclusively breastfeed. Addressing barriers to exclusive breastfeeding is essential to enhance maternal and newborn health equity.
Significance
What is already known on this subject? Exclusive breastfeeding is recognized as the ideal feeding method for infants. Newborns receiving formula in-hospital are at higher risk for early breastfeeding cessation. Rural residence and/or in the Appalachian region negatively impact breastfeeding rates.
What this study adds? Predictors for in-hospital formula supplementation in women desiring to exclusively breastfeed included high school level educational, primiparity, and C-section delivery. Lactation consultation did not associate with decreased initiation of formula supplementation.



Similar content being viewed by others
Data Availability
The data underlying this study are not publicly available due to patient privacy issues. The data are available from the corresponding author upon reasonable request and appropriate data use agreements.
Code Availability
Not applicable.
References
Census Bureau, U. S. (2022). 2016–2020 American Community Survey 5-Year Estimates. Retrieved August 1, 2022, from https://data.census.gov/cedsci/table?q=median%20income&tid=ACSST5Y2020.S1901.
Centers for Disease Control and Prevention (2021). ) Data to Action Success Story: West Virginia: Launching the Tobacco-Free Pregnancy Initiative of West Virginia. Retrieved August 1, 2022 from https://www.cdc.gov/prams/state-success-stories/West-Virginia.html
Centers for Disease Control and Prevention (2022). Breastfeeding report card United States, 2022. Retrieved August 1, 2022 from https://www.cdc.gov/breastfeeding/data/reportcard.htm.
Chantry, C. J., Dewey, K. G., Peerson, J. M., Wagner, E. A., & Nommsen-Rivers, L. A. (2014). In-hospital formula use increases early breastfeeding cessation among first-time mothers intending to exclusively breastfeed. Journal of Pediatrics,164(6), 1339-1345.e1335. https://doi.org/10.1016/j.jpeds.2013.12.035
Chertok, I. R., Luo, J., Culp, S., & Mullett, M. (2011). Intent to breastfeed: A population-based perspective. Breastfeeding Medicine: The Official Journal of the Academy of Breastfeeding Medicine,6(3), 125–129. https://doi.org/10.1089/bfm.2010.0013
Chiang, K. V., Li, R., Anstey, E. H., & Perrine, C. G. (2021). Racial and ethnic disparities in breastfeeding initiation—United States, 2019. MMWR Morbidity and Mortality Weekly Report,70(21), 769–774. https://doi.org/10.15585/mmwr.mm7021a1
Chowdhury, R., Sinha, B., Sankar, M. J., Taneja, S., Bhandari, N., Rollins, N., & Martines, J. (2015). Breastfeeding and maternal health outcomes: A systematic review and meta-analysis. Acta Paediatrica,104(467), 96–113. https://doi.org/10.1111/apa.13102
Cohen, S. S., Alexander, D. D., Krebs, N. F., Young, B. E., Cabana, M. D., Erdmann, P., & Saavedra, J. M. (2018). Factors associated with breastfeeding initiation and continuation: A meta-analysis. Journal of Pediatrics,203, 190–196. https://doi.org/10.1016/j.jpeds.2018.08.008
Forbes, J. D., Azad, M. B., Vehling, L., Tun, H. M., Konya, T. B., Guttman, D. S., & Investigators, C. H. I. L. D. C. S. (2018). Association of exposure to formula in the hospital and subsequent infant feeding practices with gut microbiota and risk of overweight in the first year of life. JAMA Pediatrics,172(7), e181161. https://doi.org/10.1001/jamapediatrics.2018.1161
Gagnon, A. J., Leduc, G., Waghorn, K., Yang, H., & Platt, R. W. (2005). In-hospital formula supplementation of healthy breastfeeding newborns. Journal of Human Lactation : Official Journal of International Lactation Consultant Association,21(4), 397–405. https://doi.org/10.1177/0890334405280835
Grassley, J. S., Schleis, J., Bennett, S., Chapman, S., & Lind, B. (2014). Reasons for initial formula supplementation of healthy breastfeeding newborns. Nursing for Women’s Health,18(3), 196–203. https://doi.org/10.1111/1751-486X.12120
Harris, P. A., Taylor, R., Thielke, R., Payne, J., Gonzalez, N., & Conde, J. G. (2009). Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. Journal of Biomedical Informatics,42(2), 377–381. https://doi.org/10.1016/j.jbi.2008.08.010
Health Resources & Services Administration (2022). Federal Office of Rural Health Policy (FORHP) Data Files. Eligible ZIP Codes. Retrieved July 1, 2022 from https://www.hrsa.gov/rural-health/about-us/what-is-rural/data-files.
Jones, K. M., Power, M. L., Queenan, J. T., & Schulkin, J. (2015). Racial and ethnic disparities in breastfeeding. Breastfeeding Medicine : The Official Journal of the Academy of Breastfeeding Medicine,10(4), 186–196. https://doi.org/10.1089/bfm.2014.0152
Kogan, M. D., Singh, G. K., Dee, D. L., Belanoff, C., & Grummer-Strawn, L. M. (2008). Multivariate analysis of state variation in breastfeeding rates in the United States. American Journal of Public Health,98(10), 1872–1880. https://doi.org/10.2105/AJPH.2007.127118
Marshall, J. L., Thomas, L., Lane, N. G., Holmes, G. M., Arcury, T. A., Randolph, R., Silberman, P., Holding, W., Villamil, L., Thomas, S., Lane, M., Latus, J., Rodgers, J., & Ivey, K. (2017). Health Disparities in Appalachia [Appalachian Regional Commission]. Retrieved August 1, 2022, from https://www.arc.gov/report/health-disparities-inappalachia/.
McCoy, M. B., & Heggie, P. (2020). In-hospital formula feeding and breastfeeding duration. Pediatrics,146(1), e20192946. https://doi.org/10.1542/peds.2019-2946
Meedya, S., Fahy, K., & Kable, A. (2010). Factors that positively influence breastfeeding duration to 6 months: A literature review. Women and Birth,23(4), 135–145. https://doi.org/10.1016/j.wombi.2010.02.002
Meek, J. Y., Noble, L., & Section on Breastfeeding (2022). Policy statement: Breastfeeding and the use of human milk. Pediatrics, 150(1), e2022057988. https://doi.org/10.1542/peds.2022-057988
Nguyen, T., Dennison, B. A., Fan, W., Xu, C., & Birkhead, G. S. (2017). Variation in formula supplementation of breastfed newborn infants in New York hospitals. Pediatrics,140(1), e20170142. https://doi.org/10.1542/peds.2017-0142
Odar Stough, C., Khalsa, A. S., Nabors, L. A., Merianos, A. L., & Peugh, J. (2019). Predictors of exclusive breastfeeding for 6 months in a national sample of US children. American Journal of Health Promotion: AJHP,33(1), 48–56. https://doi.org/10.1177/0890117118774208
Parry, J. E., Ip, D. K., Chau, P. Y., Wu, K. M., & Tarrant, M. (2013). Predictors and consequences of in-hospital formula supplementation for healthy breastfeeding newborns. Journal of Human Lactation: Official Journal of International Lactation Consultant Association,29(4), 527–536. https://doi.org/10.1177/0890334412474719
Patel, S. (2016). The effectiveness of lactation consultants and lactation counselors on breastfeeding outcomes. Journal of Human Lactation : Official Journal of International Lactation Consultant Association,32(3), 530–541. https://doi.org/10.1177/0890334415618668
Ryan, A. S., Zhou, W., & Gaston, M. H. (2004). Regional and sociodemographic variation of breastfeeding in the United States, 2002. Clinical Pediatrics (Phila),43(9), 815–824. https://doi.org/10.1177/000992280404300905
Sankar, M. J., Sinha, B., Chowdhury, R., Bhandari, N., Taneja, S., Martines, J., & Bahl, R. (2015). Optimal breastfeeding practices and infant and child mortality: A systematic review and meta-analysis. Acta Paediatrica,104(467), 3–13. https://doi.org/10.1111/apa.13147
Standish, K. R., & Parker, M. G. (2022). Social determinants of breastfeeding in the United States. Clinical Therapeutics,44(2), 186–192. https://doi.org/10.1016/j.clinthera.2021.11.010
Temple Newhook, J., Newhook, L. A., Midodzi, W. K., Murphy Goodridge, J., Burrage, L., Gill, N., & Twells, L. (2017). Determinants of nonmedically indicated in-hospital supplementation of infants whose birthing parents intended to exclusively breastfeed. Journal of Human Lactation,33(2), 278–284. https://doi.org/10.1177/0890334417695204
Urashima, M., Mezawa, H., Okuyama, M., Urashima, T., Hirano, D., Gocho, N., & Tachimoto, H. (2019). Primary prevention of cow’s milk sensitization and food allergy by avoiding supplementation with cow’s milk formula at birth: A randomized clinical trial. JAMA Pediatrics,173(12), 1137–1145. https://doi.org/10.1001/jamapediatrics.2019.3544
U. S. Department of Agriculture and U.S. Department of Health and Human Services. (2020). Dietary guidelines for americans, 2020–2025 (9th Edition). DietaryGuidelines.gov.
Wiener, R. C., & Wiener, M. A. (2011). Breastfeeding prevalence and distribution in the USA and Appalachia by rural and urban setting. Rural and Remote Health,11(2), 1713.
World Health Organization (2022). Breastfeeding recommendations. Retrieved August 1, 2022, from https://www.who.int/health-topics/breastfeeding#tab=tab_2
Acknowledgements
The project described was supported by Award Number UL1RR025755 from the National Center for Research Resources. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center for Research Resources or the National Institutes of Health.
Funding
No funding was secured for this study.
Author information
Authors and Affiliations
Contributions
EA collected data, interpreted results, drafted the initial manuscript, and reviewed the manuscript for important intellectual content. SB and KW collected data, interpreted results, and reviewed the manuscript for important intellectual content. ST assisted in study design, performed data analyses, and revised and reviewed the manuscript for important intellectual content. CE, KC and AD conceptualized and designed the study, interpreted results, and critically reviewed the manuscript for important intellectual content. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest relevant to this article to disclose.
Ethical Approval
All aspects of the study were approved by the Charleston Area Medical Center/West Virginia University-Charleston Institutional Review Board.
Consent to Participate
Waiver of consent was approved by by the Charleston Area Medical Center/West Virginia University-Charleston Institutional Review Board.
Consent to Publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alqudah, E., Davis, A., Berzingi, S. et al. In-Hospital Formula Supplementation in Appalachian Women Intending to Exclusively Breastfeed. Matern Child Health J 28, 324–332 (2024). https://doi.org/10.1007/s10995-023-03830-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-023-03830-1