Abstract
Background
Adverse childhood experiences (ACEs) are common, often co-occur, and are associated with poor health outcomes across the life course. Emerging research has emphasized the lasting consequences of ACEs across generations, suggesting parental ACEs are associated with poor physical and mental health outcomes in children. However, the individual effects of fathers’ ACEs and pathways of transmission remain unclear. A scoping review was conducted to summarize the current knowledgebase of the intergenerational consequences of parental ACEs on offspring health, clarify pathways of transmission, understand how ACEs are operationalized in the intergenerational literature, and identify gaps in knowledge.
Methods
Six electronic databases were searched for articles published in English from 1995 to 2022 relating to the long-term consequences of parental ACEs on offspring physical and mental health. Articles underwent title, abstract, and full-text review by two investigators. Content analysis was performed to integrate findings across the included studies.
Results
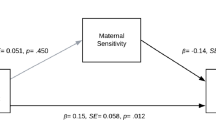
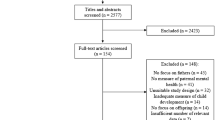
The search yielded 14,542 unique articles; 49 met the inclusion criteria. Thirty-six articles focused exclusively on mothers, one solely on fathers, and 12 included both mothers and fathers in their analyses. Six studies used an expanded definition of ACEs. Both direct and indirect associations between parental ACEs and poor offspring outcomes were identified, primarily through biological and psychosocial pathways.
Conclusions
Findings underscore the importance and oversight of fathers and the need to solidify a unified definition and measure of ACEs. This review identified modifiable protective factors (social support, father involvement) and pathways of transmission (parental mental health, parenting); both having important implications for intervention development.
Significance
What is known on this subject? Recently, research has highlighted the intergenerational consequences of parental ACEs on offspring physical and mental health outcomes with a primary focus on mothers. Maternal exposure to ACEs is associated with poor offspring behavioral, mental and physical health, and developmental outcomes.
What the study adds? This review extends prior literature by summarizing the nascent research on paternal ACEs, pathways of transmission, and suggesting the transmission of maternal ACEs to offspring outcomes is observed across a wide range of health outcomes and ACEs.

Similar content being viewed by others
Data Availability
Upon request.
Code Availability
Not applicable.
References
Adgent, M. A., Elsayed-Ali, O., Gebretsadik, T., Tylavsky, F. A., Kocak, M., Cormier, S. A., Wright, R. J., & Carroll, K. N. (2019). Maternal childhood and lifetime traumatic life events and infant bronchiolitis. Paediatric and Perinatal Epidemiology, 33(4), 262–270. https://doi.org/10.1111/ppe.12559
Adkins, T., Reisz, S., Doerge, K., & Nulu, S. (2020). Adverse childhood experience histories in foster parents: Connections to foster children’s emotional and behavioral difficulties. Child Abuse and Neglect, 104, 104475.
Ahmad, S. I., Rudd, K. L., LeWinn, K. Z., Mason, W. A., Murphy, L., Juarez, P. D., Karr, C. J., Sathyanarayana, S., Tylavsky, F. A., & Bush, N. R. (2021). Maternal childhood trauma and prenatal stressors are associated with child behavioral health. Journal of Developmental Origins of Health and Disease. https://doi.org/10.1017/s2040174421000581
Andersson, S. O., Annerbäck, E. M., Söndergaard, H. P., Hallqvist, J., & Kristiansson, P. (2021). Adverse childhood experiences are associated with choice of partner, both partners’ relationship and psychosocial health as reported one year after birth of a common child. A cross-sectional study. PLoS ONE, 16(1), e0244696. https://doi.org/10.1371/journal.pone.0244696
Appleton, A. A., Holdsworth, E., Ryan, M., & Tracy, M. (2017). Measuring childhood adversity in life course cardiovascular research: A systematic review. Psychosomatic Medicine, 79(4), 434–440. https://doi.org/10.1097/psy.0000000000000430
Arksey, H., & O’Malley, L. (2005). Scoping studies: Towards a methodological framework. International Journal of Social Research Methodology: Theory and Practice, 8(1), 19–32.
Beveridge, J. K., Yeates, K. O., Madigan, S., Stone, A. L., Wilson, A. C., Sumpton, J. E., & Noel, M. (2021). Examining parent adverse childhood experiences as a distal risk factor in pediatric chronic pain. The Clinical Journal of Pain, 38(2), 95–107. https://doi.org/10.1097/ajp.0000000000001002
Blaire, K., Topitzes, J., & Merskey, J. (2019). Do parents’ adverse childhood experiences influence treatment responses to parent-child interaction therapy? An exploratory study with a child welfare sample. Child & Family Behavior Therapy, 41(2), 78–83.
Bremner, J. D., Bolus, R., & Mayer, E. A. (2007). Psychometric properties of the Early Trauma Inventory-Self Report. The Journal of Nervous and Mental Disease, 195(3), 211–218.
Brittain, K., Zerbe, A., Phillips, T. K., Gomba, Y., Mellins, C. A., Myer, L., & Abrams, E. J. (2021). Impact of adverse childhood experiences on women’s psychosocial and HIV-related outcomes and early child development in their offspring. Global Public Health. https://doi.org/10.1080/17441692.2021.1986735
Center for the Developing Child. (2022). Toxic stress. Retrieved 2022, from https://developingchild.harvard.edu/science/key-concepts/toxic-stress/
Centers for Disease Control and Prevention (2021a). Preventing adverse childhood experiences Retrieved 2021, from https://www.cdc.gov/violenceprevention/aces/fastfact.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fviolenceprevention%2Facestudy%2Ffastfact.html
Centers for Disease Control and Prevention (2021b). About the CDC-Kaiser ACE study. Retrieved 2021, from https://www.cdc.gov/violenceprevention/aces/about.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fviolenceprevention%2Facestudy%2Fabout.html.
Centers for Disease Control and Prevention (2021c). Impact of racism on our nation’s health. Retrieved 2021, from https://www.cdc.gov/healthequity/racism-disparities/impact-of-racism.html.
Chang, Y. T., Feng, J. Y., Chang, H. Y., Chang, Y. C., & Lee, C. K. (2021). The impacts of maternal childhood adversity, stress, and mental health on child development at 6 months in Taiwan: A follow-up study. Development and Psychopathology, 33(3), 970–979. https://doi.org/10.1017/s0954579420000267
Christensen, J., Beveridge, J. K., Wang, M., Orr, S. L., Noel, M., & Mychasiuk, R. (2021). A pilot study investigating the role of gender in the intergenerational relationships between gene expression, chronic pain, and adverse childhood experiences in a clinical sample of youth with chronic pain. Epigenomes. https://doi.org/10.3390/epigenomes5020009
Coe, J. L., Huffhines, L., Contente, C. A., Seifer, R., & Parade, S. H. (2020). Intergenerational effects of maternal childhood experiences on maternal parenting and infant developmental progress. Journal of Developmental and Behavioral Pediatrics, 41(8), 619–627. https://doi.org/10.1097/dbp.0000000000000835
Cooke, J. E., Racine, N., Pador, P., & Madigan, S. (2021). Maternal adverse childhood experiences and child behavior problems: A systematic review. Pediatrics. https://doi.org/10.1542/peds.2020-044131
Cooke, J. E., Racine, N., Plamondon, A., Tough, S., & Madigan, S. (2019). Maternal adverse childhood experiences, attachment style, and mental health: Pathways of transmission to child behavior problems. Child Abuse and Neglect, 93, 27–37. https://doi.org/10.1016/j.chiabu.2019.04.011
Cronholm, P. F., Forke, C. M., Wade, R., Bair-Merritt, M. H., Davis, M., Harkins-Schwarz, M., & Fein, J. A. (2015). Adverse childhood experiences: Expanding the concept of adversity. American Journal of Preventive Medicine, 49(3), 354–361. https://doi.org/10.1016/j.amepre.2015.02.001
Dennis, C. H., Clohessy, D. S., Stone, A. L., Darnall, B. D., & Wilson, A. C. (2019). Adverse childhood experiences in mothers with chronic pain and intergenerational impact on children. The Journal of Pain, 20(10), 1209–1217. https://doi.org/10.1016/j.jpain.2019.04.004
Doi, S., Fujiwara, T., & Isumi, A. (2020). Association between maternal adverse childhood experiences and mental health problems in offspring: An intergenerational study. Development and Psychopathology. https://doi.org/10.1017/S0954579420000334
Esteves, K. C., Jones, C. W., Wade, M., Callerame, K., Smith, A. K., Theall, K. P., & Drury, S. S. (2020). Adverse childhood experiences: Implications for offspring telomere length and psychopathology. American Journal of Psychiatry, 177(1), 47–57. https://doi.org/10.1176/appi.ajp.2019.18030335
Felitti, V. J., Anda, R. F., Nordenberg, D., Williamson, D. F., Spitz, A. M., Edwards, V., Koss, M. P., & Marks, J. S. (1998). Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults. The Adverse Childhood Experiences (ACE) Study. American Journal of Preventive Medicine, 14(4), 245–258. https://doi.org/10.1016/s0749-3797(98)00017-8
Fenerci, R. L. B., & DePrince, A. P. (2018). Intergenerational transmission of trauma: Maternal trauma-related cognitions and toddler symptoms. Child Maltreatment, 23(2), 126–136. https://doi.org/10.1177/1077559517737376
Finkelhor, D., Shattuck, A., Turner, H., & Hamby, S. (2015). A revised inventory of adverse childhood experiences. Child Abuse and Neglect, 48, 13–21. https://doi.org/10.1016/j.chiabu.2015.07.011
Folger, A. T., Eismann, E. A., Stephenson, N. B., Shapiro, R. A., Macaluso, M., Brownrigg, M. E., & Gillespie, R. J. (2018). Parental adverse childhood experiences and offspring development at 2 years of age. Pediatrics. https://doi.org/10.1542/peds.2017-2826
Folger, A. T., Putnam, K. T., Putnam, F. W., Peugh, J. L., Eismann, E. A., Sa, T., Shapiro, R. A., Van Ginkel, J. B., & Ammerman, R. T. (2017). Maternal interpersonal trauma and child social-emotional development: An intergenerational effect. Paediatric and Perinatal Epidemiology, 31(2), 99–107. https://doi.org/10.1111/ppe.12341
Fredland, N., McFarlane, J., Symes, L., & Maddoux, J. (2018). Exploring the association of maternal adverse childhood experiences with maternal health and child behavior following intimate partner violence. Journal of Women’s Health (2002), 27(1), 64–71. https://doi.org/10.1089/jwh.2016.5969
Giunta, H., Romanowicz, M., Baker, A., O’Toole-Martin, P., & Lynch, B. A. (2021). Positive impact of education class for parents with adverse childhood experiences on child behavior. Progress in Community Health Partnerships, 15(4), 431–438. https://doi.org/10.1353/cpr.2021.0056
Hatch, V., Swerbenski, H., & Gray, S. A. O. (2020). Family social support buffers the intergenerational association of maternal adverse childhood experiences and preschoolers’ externalizing behavior. American Journal of Orthopsychiatry, 90(4), 489–501. https://doi.org/10.1037/ort0000451
Haynes, E., Crouch, E., Probst, J., Radcliff, E., Bennett, K., & Glover, S. (2020a). Exploring the association between a parent’s exposure to adverse childhood experiences (ACEs) and outcomes of depression and anxiety among their children. Children and Youth Services Review. https://doi.org/10.1016/j.childyouth.2020.105013
Haynes, E., Crouch, E., Probst, J., Radcliff, E., Bennett, K., & Glover, S. (2020b). Exploring the association between a parent’s exposure to adverse childhood experiences (ACEs) and outcomes of depression and anxiety among their children. Children and Youth Services Review, 113, 7. https://doi.org/10.1016/j.childyouth.2020.105013
Hetherington, E., Racine, N., Madigan, S., McDonald, S., & Tough, S. (2020). Relative contribution of maternal adverse childhood experiences to understanding children’s externalizing and internalizing behaviours at age 5: Findings from the all our families cohort. CMAJ Open, 8(2), E352-e359. https://doi.org/10.9778/cmajo.20190149
Hughes, K., Bellis, M. A., Hardcastle, K. A., Sethi, D., Butchart, A., Mikton, C., Jones, L., & Dunne, M. P. (2017). The effect of multiple adverse childhood experiences on health: a systematic review and meta-analysis. Lancet Public Health, 2(8), e356–e366. https://doi.org/10.1016/s2468-2667(17)30118-4
Jones, C. W., Esteves, K. C., Gray, S. A. O., Clarke, T. N., Callerame, K., Theall, K. P., & Drury, S. S. (2019). The transgenerational transmission of maternal adverse childhood experiences (ACEs): Insights from placental aging and infant autonomic nervous system reactivity. Psychoneuroendocrinology, 106, 20–27. https://doi.org/10.1016/j.psyneuen.2019.03.022
Kang, N. R., Kwack, Y. S., Song, J. K., Kim, M. D., Park, J. H., Kim, B. N., & Moon, D. S. (2021). The impact of maternal adverse childhood experiences on offspring’s internalizing and externalizing problems. Psychiatry Investigation, 18(11), 1050–1057. https://doi.org/10.30773/pi.2021.0343
Karatekin, C., Mason, S. M., Riegelman, A., Bakker, C., Hunt, S., Gresham, B., Corcoran, F., & Barnes, A. (2022). Adverse childhood experiences: A scoping review of measures and methods. Children and Youth Services Review. https://doi.org/10.1016/j.childyouth.2022.106425
Khalifian, C. E., Boch, J., Knopp, K., Delay, C., Sohn, M., & Morland, L. (2022). Adverse childhood experiences, mental health & relationship satisfaction in military couples. Journal of Family Psychology. https://doi.org/10.1037/fam0000952
Khan, M., & Renk, K. (2019). Mothers’ adverse childhood experiences, depressive symptoms, parenting, and attachment as predictors of young children’s problems. Journal of Child Custody, 16(3), 268–290. https://doi.org/10.1080/15379418.2019.1575318
Kubany, E. S., Haynes, S. N., Leisen, M. B., Owens, J. A., Kaplan, A. S., Watson, S. B., & Burns, K. (2000). Development and preliminary validation of a brief broad-spectrum measure of trauma exposure: The Traumatic Life Events Questionnaire. Psychological Assessment, 12(2), 210–224. https://doi.org/10.1037//1040-3590.12.2.210
Kumar, M., Amugune, B., Madeghe, B., Wambua, G. N., Osok, J., Polkonikova-Wamoto, A., Bukusi, D., Were, F., & Huang, K.-Y. (2018). Mechanisms associated with maternal adverse childhood experiences on offspring’s mental health in Nairobi informal settlements: a mediational model testing approach. BMC Psychiatry, 18(1), 381. https://doi.org/10.1186/s12888-018-1953-y
Lafavor, T., Boer, D., & Poole, M. (2020). Intergenerational effects of early parental adversity on child developmental outcomes among families living in emergency homeless shelters. Journal of Health Care for the Poor and Underserved, 31(3), 1264–1280. https://doi.org/10.1353/hpu.2020.0093
Leeners, B., Rath, W., Block, E., Görres, G., & Tschudin, S. (2014). Risk factors for unfavorable pregnancy outcome in women with adverse childhood experiences. Journal of Perinatal Medicine, 42(2), 171–178. https://doi.org/10.1515/jpm-2013-0003
Lê-Scherban, F., Wang, X., Boyle-Steed, K. H., & Pachter, L. M. (2018). Intergenerational associations of parent adverse childhood experiences and child health outcomes. Pediatrics. https://doi.org/10.1542/peds.2017-4274
Letourneau, N., Dewey, D., Kaplan, B. J., Ntanda, H., Novick, J., Thomas, J. C., Deane, A. J., Leung, B., Pon, K., & Giesbrecht, G. F. (2019). Intergenerational transmission of adverse childhood experiences via maternal depression and anxiety and moderation by child sex. Journal of Developmental Origins of Health and Disease, 10(1), 88–99. https://doi.org/10.1017/s2040174418000648
Liu, S. Y., Pabayo, R., & Muennig, P. (2021). Perceived discrimination and increased odds of unmet medical needs among US children. International Journal of Health Services, 51(3), 364–370.
Livingston, G., & Parker, K. (2019). 8 facts about American dads. Retrieved from https://www.pewresearch.org/fact-tank/2019/06/12/fathers-day-facts/
Lyons-Ruth, K., & Block, D. (1996). The disturbed caregiving system: Relations among childhood trauma, maternal caregiving, and infant affect and attachment. Infant Mental Health Journal, 17(3), 257–275.
Madigan, S., Wade, M., Plamondon, A., Maguire, J. L., & Jenkins, J. M. (2017). Maternal adverse childhood experience and infant health: Biomedical and psychosocial risks as intermediary mechanisms. Journal of Pediatrics, 187, 282-289.e281. https://doi.org/10.1016/j.jpeds.2017.04.052
Maguire-Jack, K., Lanier, P., & Lombardi, B. (2020). Investigating racial differences in clusters of adverse childhood experiences. American Journal of Orthopsychiatry, 90(1), 106–114. https://doi.org/10.1037/ort0000405
McDonald, S. W., Madigan, S., Racine, N., Benzies, K., Tomfohr, L., & Tough, S. (2019). Maternal adverse childhood experiences, mental health, and child behaviour at age 3: The all our families community cohort study. Preventive Medicine, 118, 286–294. https://doi.org/10.1016/j.ypmed.2018.11.013
McDonnell, C. G., & Valentino, K. (2016). Intergenerational effects of childhood trauma: Evaluating pathways among maternal ACEs, perinatal depressive symptoms, and infant outcomes. Child Maltreatment, 21(4), 317–326. https://doi.org/10.1177/1077559516659556
Mersky, J. P., Janczewski, C. E., & Topitzes, J. (2017). Rethinking the measurement of adversity: Moving toward second-generation research on adverse childhood experiences. Child Maltreatment, 22(1), 58–68. https://doi.org/10.1177/1077559516679513
Mersky, J. P., & Lee, C. P. (2019). Adverse childhood experiences and poor birth outcomes in a diverse, low-income sample. BMC Pregnancy and Childbirth, 19(1), 387. https://doi.org/10.1186/s12884-019-2560-8
Moon, D. S., Bong, S. J., Kim, B. N., & Kang, N. R. (2021). Association between maternal adverse childhood experiences and attention-deficit/hyperactivity disorder in the offspring: The mediating role of antepartum health risks. Soa Chongsonyon Chongsin Uihak, 32(1), 28–34. https://doi.org/10.5765/jkacap.200041
Munn, Z., Peters, M. D. J., Stern, C., Tufanaru, C., McArthur, A., & Aromataris, E. (2018). Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Medical Research Methodology, 18(1), 143. https://doi.org/10.1186/s12874-018-0611-x
Na, M. C., Kim, M. D., Park, J. H., Jung, Y. E., Moon, D. S., Yang, H. J., Kim, B. N., & Kang, N. R. (2021). Association between maternal adverse childhood experiences and risk of post-traumatic stress disorder in the offspring. Soa Chongsonyon Chongsin Uihak, 32(2), 63–70. https://doi.org/10.5765/jkacap.200045
Parker K, Morin, R, Horowitz, J. (2022). Pew Research Center. Views of demographic changes. Retrieved 2022, from https://www.pewresearch.org/social-trends/2019/03/21/views-of-demographic-changes-in-america/
Petruccelli, K., Davis, J., & Berman, T. (2019). Adverse childhood experiences and associated health outcomes: A systematic review and meta-analysis. Child Abuse and Neglect, 97, 104127. https://doi.org/10.1016/j.chiabu.2019.104127
Racine, N., Byles, H., Killam, T., Ereyi-Osas, W., & Madigan, S. (2022). Asking about childhood adversity in the prenatal care setting: Cross-sectional associations with maternal health and mental health outcomes. Maternal and Child Health Journal, 26(5), 994–1004. https://doi.org/10.1007/s10995-021-03301-5
Racine, N., Plamondon, A., Madigan, S., McDonald, S., & Tough, S. (2018). Maternal adverse childhood experiences and infant development. Pediatrics. https://doi.org/10.1542/peds.2017-2495
Rayyan. (2022). Intelligent systematic review. Retrieved 2022, from https://www.rayyan.ai/
Rieder, A. D., Roth, S. L., Musyimi, C., Ndetei, D., Sassi, R. B., Mutiso, V., Hall, G. B., & Gonzalez, A. (2019). Impact of maternal adverse childhood experiences on child socioemotional function in rural Kenya: Mediating role of maternal mental health. Developmental Science, 22(5), e12833. https://doi.org/10.1111/desc.12833
Riggs, J. L., Rosenblum, K. L., Muzik, M., Jester, J., Freeman, S., Huth-Bocks, A., Waddell, R., Alfafara, E., Miller, A., Lawler, J., & Erickson, N. (2021). Infant mental health home visiting mitigates impact of maternal adverse childhood experiences on toddler language competence: A randomized controlled trial. Journal of Developmental & Behavioral Pediatrics. https://doi.org/10.1097/dbp.0000000000001020
Saldana, J. (2021). The coding manual for qualitative researchers. SAGE.
Schickedanz, A., Halfon, N., Sastry, N., & Chung, P. J. (2018). Parents’ adverse childhood experiences and their children’s behavioral health problems. Pediatrics. https://doi.org/10.1542/peds.2018-0023
Seteanu, S. L., & Giosan, C. (2021). Adverse childhood experiences in fathers and the consequences in their children. Professional Psychology: Research and Practice, 52(1), 80–89.
Smith, M. V., Gotman, N., & Yonkers, K. A. (2016). Early childhood adversity and pregnancy outcomes. Maternal and Child Health Journal, 20(4), 790–798. https://doi.org/10.1007/s10995-015-1909-5
Stepleton, K., Bosk, E. A., Duron, J. F., Greenfield, B., Ocasio, K., & MacKenzie, M. J. (2018). Exploring associations between maternal adverse childhood experiences and child behavior. Children and Youth Services Review, 95, 80–87. https://doi.org/10.1016/j.childyouth.2018.10.027
Suglia, S. F., Crookes, D. M., Kaplan, R., Sotres-Alvarez, D., Llabre, M. M., Van Horn, L., Carnethon, M. R., & Isasi, C. R. (2020). Intergenerational transmission of childhood adversity in parents and their children’s BMI in the Hispanic Community Children’s Health Study/Study of Latino Youth (HCHS/SOL Youth). Journal of Psychosomatic Research, 131, 109956. https://doi.org/10.1016/j.jpsychores.2020.109956
Suglia, S. F., Duarte, C. S., Chambers, E. C., & Boynton-Jarrett, R. (2013). Social and behavioral risk factors for obesity in early childhood. Journal of Developmental and Behavioral Pediatrics, 34(8), 549–556. https://doi.org/10.1097/DBP.0b013e3182a509c0
Sun, J., Patel, F., Rose-Jacobs, R., Frank, D. A., Black, M. M., & Chilton, M. (2017). Mothers’ adverse childhood experiences and their young children’s development. American Journal of Preventive Medicine, 53(6), 882–891. https://doi.org/10.1016/j.amepre.2017.07.015
Sun, W., Ren, Z., Zhu, S., Cheng, S., Liu, W., Li, H. C. W., Xia, W., Yuan, Adeloye, D., Rudan, I., Canoy, D., & Song, P. (2023). Spousal concordance in advese childhood experiences and the association with depressive symptoms in middle-aged and older adults: Findings accross China, the US, and Europe. Frontiers in Public Health. https://doi.org/10.3389/fpubh.2023.1158590
Testa, A., & Jackson, D. B. (2021). Maternal adverse childhood experiences, paternal involvement, and infant health. Journal of Pediatrics, 236, 157-163.e151. https://doi.org/10.1016/j.jpeds.2021.04.031
Thomas, J. C., Letourneau, N., Campbell, T. S., & Giesbrecht, G. F. (2018). Social buffering of the maternal and infant HPA axes: Mediation and moderation in the intergenerational transmission of adverse childhood experiences. Development and Psychopathology, 30(3), 921–939. https://doi.org/10.1017/s0954579418000512
Thomas-Argyriou, J. C., Letourneau, N., Dewey, D., Campbell, T. S., & Giesbrecht, G. F. (2021). The role of HPA-axis function during pregnancy in the intergenerational transmission of maternal adverse childhood experiences to child behavior problems. Development and Psychopathology, 33(1), 284–300. https://doi.org/10.1017/s0954579419001767
Thomas-Giyer, J., & Keesler, J. M. (2021). Exploring maternal adversity and childhood outcomes among low-income rural families. Child Abuse and Neglect, 111, 104817. https://doi.org/10.1016/j.chiabu.2020.104817
Vandenburg, S. G. (1972). Assortative mating, or who marries whom? Behavior Genetics, 2(2), 127–157. https://doi.org/10.1007/bf01065686
Wade, R., Cronholm, P. F., Fein, J. A., Forke, C. M., Davis, M. B., Harkins-Schwarz, M., Pachter, L. M., & Bair-Merritt, M. H. (2016). Household and community-level adverse childhood experiences and adult health outcomes in a diverse urban population. Child Abuse & Neglect, 52, 135–145. https://doi.org/10.1016/j.chiabu.2015.11.021
Wessler, M. (2022). Prison policy initiative: Updated charts provided insights on racial disparities, correctional control, jail suidices, and more. Retrieved 2022, from https://www.prisonpolicy.org/blog/2022/05/19/updated_charts/
World Health Organization. (2020). Adverse Childhood Experiences International Questionnaire (ACE-IQ). Retrieved 2020, from https://www.who.int/publications/m/item/adverse-childhood-experiences-international-questionnaire-(ace-iq)
Wurster, H. E., Sarche, M., Trucksess, C., Morse, B., & Biringen, Z. (2020). Parents’ adverse childhood experiences and parent-child emotional availability in an American Indian community: Relations with young children’s social-emotional development. Development and Psychopathology, 32(2), 425–436. https://doi.org/10.1017/s095457941900018x
Xin, H. (2017). Editorial: Health disparities-an important public health policy concern. Frontiers in Public Health, 5, 99.
Yehuda, R., & Lehrner, A. (2018). Intergenerational transmission of trauma effects: Putative role of epigenetic mechanisms. World Psychiatry, 17(3), 243–257. https://doi.org/10.1002/wps.20568
Yogman, M., & Garfield, C. F. (2016). Fathers’ roles in the care and development of their children: The role of pediatricians. Pediatrics. https://doi.org/10.1542/peds.2016-1128
Ziv, Y., Sofri, I., Capps Umphlet, K. L., Olarte, S., & Venza, J. (2018). Children and caregivers’ exposure to Adverse Childhood Experiences (ACES): Association with children’s and caregivers’ psychological outcomes in a therapeutic preschool program. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph15040646
Acknowledgements
The research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
The research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Grafft conceptualized the study, participated in all 5 stages of the scoping review, drafted the initial manuscript, and reviewed and revised the manuscript. Lo participated in the abstract and full text review and reviewed and revised the manuscript. Easton and Pineros-Leano conceptualized the study and reviewed and revised the manuscript. Davison conceptualized the study, restructured portions of the manuscript, and reviewed and revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
Not applicable.
Consent to Participate
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Grafft, N., Lo, B., Easton, S.D. et al. Maternal and Paternal Adverse Childhood Experiences (ACEs) and Offspring Health and Wellbeing: A Scoping Review. Matern Child Health J 28, 52–66 (2024). https://doi.org/10.1007/s10995-023-03825-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-023-03825-y