Abstract
Introduction
Reducing the Length Of postpartum Stay (LOS) is associated with lower hospital costs, a major reason for initiating federal projects in Belgium. Disadvantages following the reduction of LOS are the risks of maternal and neonatal readmissions. This study compares readmissions with or without reduced LOS, by introducing the KOZI&Home program in the university hospital Brussels.
Methods
This is an observational study comparing the readmission rates of the length of postpartum hospital stay between two groups: the non-KOZI&Home group (> 2 days for vaginal birth and > 4 days for caesarean section) and KOZI&Home group (≤ 2 days for vaginal birth and ≤ 4 days for caesarean section). A follow-up period of 16 weeks was set up.
Results
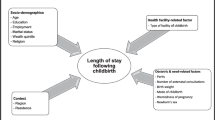
The maternal readmission rate was 4,8% for the non-KOZI&Home group (n = 332) and 3.3% for the KOZI&Home group (n = 253). Neonatal readmission rates were 7.2% and 15.9% respectively. After controlling influencing factors in a multivariate model for maternal and neonatal readmissions, there were no statistical significant differences. Factors negatively affecting neonatal readmissions are (1) dismissal period October-January (OR:3.22;95% CI 1.10–9.42) and (2) low education level (OR:3.44;95% CI 1.54–7.67), for maternal readmissions it concerns whether or not LOS is known (OR:3.26;95% CI 1.21–8.81).
Discussion
There is no effect of the KOZI&Home program on maternal nor neonatal readmission rates. Systematically informing about postpartum LOS antenatally will enforce preparation and is important to reduce maternal readmissions. Personalized information should be given to women discharged in the period October-January and to those with a lower education level, in order to reduce neonatal readmissions.
Significance
What is already known on this subject? Reducing the ‘length of stay’ after giving birth is known, for example, to reduce costs and for having a more family-centered approach. Above the known advantages, there is also some conflicting literature about the disadvantages. Some of the articles shown a higer readmission rate, and others no difference in readmission rates.
What this study adds? The influencing factors of maternal and neonatal readmissions are checked, in order to reduce the number of readmissions in the future. Systematically informing about postpartum LOS antenatally will enforce preparation and is important to reduce maternal readmissions. Personalized information should be given to women discharged in the period October-January and to those with a lower education level, in order to reduce neonatal readmissions.


Similar content being viewed by others
References
Askelsdottir, B., Lam-de Jonge, W., Edman, G., & Wiklund, I. (2013). Home care after early discharge: Impact on healthy mothers and newborns. Midwifery, 29(8), 927–934. https://doi.org/10.1016/j.midw.2012.11.001.
Bayoumi, Y. A., Bassiouny, Y. A., Hassan, A. A., Gouda, H. M., Zaki, S. S., & Abdelrazek, A. A. (2016). Is there a difference in the maternal and neonatal outcomes between patients discharged after 24 h versus 72 h following cesarean section? A prospective randomized observational study on 2998 patients. The Journal of Maternal-Fetal & Neonatal Medicine: The Official Journal of the European Association of Perinatal Medicine the Federation of Asia and Oceania Perinatal Societies the International Society of Perinatal Obstetricians, 29(8), 1339–1343. https://doi.org/10.3109/14767058.2015.1048678.
Benahmed, N. A. D. I. A., Devos, C., San Miguel, I., Vinck, R., Vankelst, L., Lauwerier, E., Verschueren, M., Obyn, C., Paulus, D., & Christiaens, W. (2014). De organisatie van de zorg na een bevalling Synthese. In Health services research (HSR): Vol. KCE 232As.
Benahmed, N., Miguel, S., Devos, L., Fairon, C., N., & Christiaens, W. (2017). Vaginal delivery: How does early hospital discharge affect mother and child outcomes? A systematic literature review. BMC Pregnancy and Childbirth, 17(289), 1–14. https://doi.org/10.1186/s12884-017-1465-7.
Bostanci Ergen, E., Ozkaya, E., Eser, A., Abide Yayla, C., & Yenidede, I. (2018). Comparison of readmission rates between groups with early versus late discharge after vaginal or cesarean delivery: A retrospective analyzes of 14,460 cases. The Journal of Maternal-Fetal & Neonatal Medicine, 31(10), 1318–1322.
Boubred, F., Herlenius, E., Andres, V., Robert, D., C., & Marchini, G. (2016). Hospital readmission after postpartum discharge of term newborns in two maternity wards in Stockholm and Marseille. Archives de Pédiatrie, 23, 234–240.
Bowers, J., & Cheyne, H. (2016). Reducing the length of postnatal hospital stay: Implications for cost and quality of care. BMC Health Services Research, 16, 16. https://doi.org/10.1186/s12913-015-1214-4.
Burgos, A. E., Schmitt, S. K., Stevenson, D. K., Phibbs, C. S., Alto, P., This, W., & Adds, S. (2018). Readmission for Neonatal Jaundice in California, 1991–2000: Trends and implications. Pediatrics. https://doi.org/10.1542/peds.2007-1214
Cangiano, G., Nenna, R., Frassanito, A., Evangelisti, M., Nicolai, A., Scagnolari, C., Pierangeli, A., Antonelli, G., Papoff, P., Petrarca, L., Capocaccia, P., Moretti, C., & Midulla, F. (2016). Bronchiolitis: Analysis of 10 consecutive epidemic seasons. Pediatric Pulmonology, 51(12), 1330–1335. https://doi.org/10.1002/ppul.23476.
Clapp, A., Little, M. E., Zheng, S., J., & Robinson, J. N. (2016). A multi-state analysis of postpartum readmissions in the United States. The American Journal of Obstetrics & Gynecology, 215(1), 113e1. 113.e10.
Cunha, B. A. (2017). Viral influenza-like illnesses: Dynamic interrelationships during the 2015–2016 influenza season in hospitalized patients. The Journal of Hospital Infection, 95(3), 275–279. https://doi.org/10.1016/j.jhin.2016.12.015.
Datar, A., & Sood, N. (2006). Impact of postpartum hospital-stay legislation on newborn length of stay, readmission, and mortality in California. Pediatrics, 118(1), 63–72. https://doi.org/10.1542/peds.2005-3044.
Edmonson, M. B., Stoddard, J. J., & Owens, L. M. (1997). Hospital Readmission with feeding-related problems after early postpartum discharge of normal newborns. Journal Of The American Medical Association, 278(4), 299–303. https://doi.org/10.1001/jama.1997.03550040055037
Ellberg, L., Högberg, U., Lundman, B., Källén, K., Håkansson, S., & Lindh, V. (2008). Maternity care options influence readmission of newborns. Acta Paediatrica (Oslo Norway: 1992), 97(5), 579–583. https://doi.org/10.1111/j.1651-2227.2008.00714.x.
Farbu, J., Haugen, M., Meltzer, H. M., & Brantsæter, A. L. (2014). Impact of singlehood during pregnancy on dietary intake and birth outcomes- a study in the norwegian mother and child cohort study. BMC Pregnancy and Childbirth, 14, 396. https://doi.org/10.1186/s12884-014-0396-9.
Ford, J. B., Algert, C. S., Morris, J. M., & Roberts, C. L. (2012). Decreasing length of maternal hospital stay is not associated with increased readmission rates. Aust NZ J Public Health, 36, 430–434. https://doi.org/10.1111/j.1753-6405.2012.00882.x.
Goodwin, L., Taylor, B., Kokab, F., & Kenyon, S. (2018). Postnatal care in the context of decreasing length of stay in hospital after birth: The perspectives of community midwives. Midwifery, 60, 36–40. https://doi.org/10.1016/j.midw.2018.02.006.
Gupta, P., Malhotra, S., Singh, D. K., & Tarun, D. (2006). Length of postnatal stay in healthy newborns and re-hospitalization following their early discharge. Indian Journal of Pediatrics, 73(10), 897–900.
Gyselaers, W., Jonckheer, P., Ahmadzal, N., Ansari, M., Carville, S., Dworzynski, K., Gaudet, L., Glen, J., Jones, K., Miller, P., Tetzlaff, J., Alexander, S., Allegaert, K., Beeckman, K., Ceysens, G., Christiane, Y., De Ronne, N., De Thysebaert, B., Dekker, N., & Stordeur, S. (2015). Welke onderzoeken zijn aanbevolen bij een zwangerschap? – Synthese. Good Clinical Practice (GCP) Brussel: Federaal Kenniscentrum Voor de Gezondheidszorg (KCE), KCE reports 248As, D/2015/10.273/55.
Ha, J., & Kim, Y. (2013). Factors influencing self-confidence in the maternal role among early Postpartum mothers. Korean Journal of Women Health Nursing, 19(1), 48–56. https://doi.org/10.4069/kjwhn.2013.19.1.48.
Habib, H. S. (2013). Impact of discharge timings of healthy newborns on the rates and etiology of neonatal hospital readmissions. Journal of the College of Physicians and Surgeons–Pakistan: JCPSP, 23(10), 715–719. https://doi.org/10.2013/JCPSP.715719.
Health care use—Length of hospital stay—OECD Data. (2018). OECD Retrieved April 12, 2019, from https://doi.org/10.1787/8dda6b7a-en
Hirsch, A. W., Monuteaux, M. C., Fruchtman, G., Bachur, R. G., & Neuman, M. I. (2016). Characteristics of children hospitalized with aspiration pneumonia. Hospital Pediatrics, 6(11), 659–666. https://doi.org/10.1542/hpeds.2016-0064.
Jones, E., Taylor, B., MacArthur, C., Pritchett, R., & Cummins, C. (2016). The effect of early postnatal discharge from hospital for women and infants: A systematic review protocol. Systematic Reviews, 5(24), 1–7. https://doi.org/10.1186/s13643-016-0193-9.
Joseph, J., & Doyle, D. A. (2011). After midnight: A regression discontinuity design in length of Postpartum Hospital stays. AMERICAN ECONOMIC JOURNAL: ECONOMIC POLICY, 3(3), 1–34.
Kehila, M., Magdoud, K., Touhami, O., Abouda, H. S., Jeridi, S., Marzouk, S. B., Mahjoub, S., Hmid, R. B., & Chanoufi, M. B. (2016). Sortie précoce en post-partum: Résultats et facteurs de risque de ré hospitalisation. Pan African Medical Journal. https://doi.org/10.11604/pamj.2016.24.189.9371
Kim, J. E., Lee, J. Y., & Lee, S. H. (2018). Single mothers’ experiences with pregnancy and child rearing in Korea: Discrepancy between Social Services/Policies and single mothers’ needs. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph15050955
McLachlan, H. L., Gold, L., Forster, D. A., Yelland, J., Rayner, J., & Rayner, S. (2009). Women’s views of postnatal care in the context of the increasing pressure on postnatal beds in Australia. Women and Birth: Journal of the Australian College of Midwives, 22(4), 128–133. https://doi.org/10.1016/j.wombi.2009.04.003.
Mosen, D. M., Clark, S. L., Mundorff, M. B., Hsa, M. B. A., Tracy, D. M., Mcknight, E. C., & Zollo, M. B. (2002). The medical and economic impact of the newborns ’ and mothers ’ health protection act. Obstetrics and Gynecology, 99(1), 116–124.
Ramírez-Villalobos, D., Hernández-Garduño, A., Salinas, A., González, D., Walker, D., Rojo-Herrera, G., & Hernández-Prado, B. (2009). Early hospital discharge and early puerperal complications. Salud Publica De Mexico, 51(3), 212–218.
Sainz Bueno, J. A., Fernandez Palacin, A., Almeida Gonzalez, C., & Manzano, M. C. (2005). Early discharge from obstetrics-pediatrics at the Hospital de Valme, with domiciliary follow-up. American Journal of Obstetrics & Gynecology, 193(29), 714–726. https://doi.org/10.1016/j.ajog.2005.01.015.
Shakib, J., Buchi, K., Smith, E., Korgenski, K., & Young, P. C. (2015). Timing of initial well-child visit and readmissions of newborns. Pediatrics, 135(3), 469–474. https://doi.org/10.1542/peds.2014-2329.
Sievertsen, H. H., & Wüst, M. (2017). Discharge on the day of birth, parental response and health and schooling outcomes. Journal of Health Economics, 55, 121–138. https://doi.org/10.1016/j.jhealeco.2017.06.012.
Smets, K. (2016). AANDACHTSPUNTEN BIJ VROEGTIJDIG ONTSLAG UIT MATERNITEIT. http://www.neonatologie.ugent.be/Vroegtijdig_ontslag_uit_materniteit.pdf
Zadoroznyj, M. (2007). Postnatal care in the community: Report of an evaluation of birthing women’s assessments of a postnatal home-care programme. Health & Social Care in the Community, 15(1), 35–44. https://doi.org/10.1111/j.1365-2524.2006.00664.x.
Acknowledgements
First of all, we would like to thank all women that participated this study. Without them, this study could not have taken place. Furthermore, we would like to thank Mrs An Vanspringel and Mrs Peggy Uyttersprot for extracting specific data from women’s medical records. We also gratefully acknowledge Leander Scheir, for checking this work for spelling, grammar and clarity.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Stas, A., Breugelmans, M., Geerinck, L. et al. Implications of a Reduced Length of Postpartum Hospital Stay on Maternal and Neonatal Readmissions, an Observational Study. Matern Child Health J 27, 1949–1960 (2023). https://doi.org/10.1007/s10995-023-03667-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-023-03667-8