Abstract
Objectives
In Virginia, Black women experience higher rates of adverse birth and labor outcomes that may not be explained solely by risky behaviors or social standing. Previous studies have found an association between racial discrimination and adverse birth outcomes; however, their findings may be underpowered due to small sample sizes. The purpose of this study was to examine the relationship between racial discrimination and poor birth outcomes.
Methods
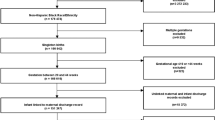
VA PRAMS (2016–2018) was used for this secondary data analysis of mothers age 15–44. The exposure was measured using two VA PRAMS questions on racial discrimination and information on the outcomes were extracted from birth certificate data. Simple logistic regression was used obtain an association between experiencing racial discrimination and adverse birth outcomes (i.e. preterm birth, low birth weight, and small for gestational age) and to identify risk factors for experiencing racial discrimination. Multivariate logistic regressions were performed after controlling for other covariates.
Results
Virginia women (N = 2634) who experienced racial discrimination had statistically significant increased odds of having a low birth weight infant (OR 2.27; 95% CI 1.18, 4.38); however, when stratified by race, only non-Hispanic Black (n = 540) women had statistically significant increased odds of preterm birth and low birth weight (PTB OR 7.18; 95% CI 2.28, 22.65; LBW OR 3.56; 95% CI 1.28, 9.91).
Conclusions
Non-Hispanic Black women in Virginia who experience racial discrimination are more likely to have low birth weight and preterm births. Efforts to effectively reduce adverse birth outcomes and eliminate racial inequities must consider upstream, holistic approaches beyond the biomedical model.
Similar content being viewed by others
Data Availability
Data is not publically available, but may be requested from the Virginia Department of Health Pending IRB approval.
Code Availability
The SAS-callable SUDAAN custom code is available upon request.
References
Alhusen, J. L., Bower, K. M., Epstein, E., & Sharps, P. (2016). Racial discrimination and adverse birth outcomes: An integrative review. Journal of Midwifery & Women’s Health, 61, 707–720. https://doi.org/10.1111/jmwh.12490
Braveman, P., Heck, K., Egerter, S., Dominguez, T. P., Rinki, C., et al. (2017). Worry about racial discrimination: A missing piece of the puzzle of Black-White disparities in preterm birth? PLoS ONE. https://doi.org/10.1371/journal.pone.0186151.
Carty, D. C., Kruger, D. J., Turner, T. M., Campbell, B., DeLoney, E. H., & Lewis, E. Y. (2011). Racism, health status, and birth outcomes: Results of a participatory community-based intervention and health survey. Journal of Urban Health: Bulletin of the New York Academy of Medicine, 88(1), 84–97. https://doi.org/10.1007/s11524-010-9530-9
Centers for Disease Control and Prevention. (2017). Key findings: Folate deficiency is common in women of reproductive age. Retrieved from https://www.cdc.gov/ncbddd/folicacid/features/kf-folate-deficiency-reproductive-women.html.
Centers for Disease Control and Prevention. (2020a). What is PRAMS? Retrieved from https://www.cdc.gov/prams/.
Centers for Disease Control and Prevention WONDER database. (2020b). Linked birth / infant death records. Retrieved from https://wonder.cdc.gov/lbd.html
Coy, P. (2018). For Black women, education is no protection against infant mortality. Bloomberg Businessweek. Retrieved from https://www.bloomberg.com/news/articles/2018-04-02/for-black-women-education-is-no-protection-against-infant-mortality
Earnshaw, V. A., Rosenthal, L., Lewis, J. B., Stasko, E. C., Tobin, J. N., Lewis, T. T., Reid, A. E., & Ickovics, J. R. (2013). Maternal experiences with everyday discrimination and infant birth weight: A test of mediators and moderators among young, urban women of color. Annals of Behavioral Medicine: A Publication of the Society of Behavioral Medicine, 45(1), 13–23. https://doi.org/10.1007/s12160-012-9404-3
Elina Hemminki Affilation. (1996). Births by younger and older mothers in a population with late and regulated childbearing: Finland 1991[Abstract]. Acta Obstetricia Et Gynecologica Scandinavica, 75(1), 19–27. https://doi.org/10.3109/00016349609033278
Fraser, A. M., Brockert, J. E., & Ward, R. H. (1995). Association of young maternal age with adverse reproductive outcomes. The New England Journal of Medicine, 332(17), 1113–1117. https://doi.org/10.1056/NEJM199504273321701
Giurgescu, C., Engeland, C. G., Zenk, S. N., & Kavanaugh, K. (2013). Stress, inflammation and preterm birth in African American women. Newborn and Infant Nursing Reviews, 13, 171–177. https://doi.org/10.1053/j.nainr.2013.09.004
Halanych, J. H., Safford, M. M., Shikany, J. M., Cuffee, Y., Person, S. D., Scarinci, I. C., Kiefe, C. I., & Allison, J. J. (2011). The association between income, education, and experiences of discrimination in older African American and European American patients. Ethnicity & Disease, 21(2), 223–229.
Jackson, F. M., Phillips, M. T., Rowland Hogue, C. J., & Curry-Owens, T. Y. (2001). Examining the burdens of gendered racism: Implications for pregnancy outcomes among college-educated African American women. Maternal and Child Health Journal, 5(2), 95–107. https://doi.org/10.1023/a:1011349115711
Lewis, T. T., Cogburn, C. D., & Williams, D. R. (2015). Self-reported experiences of discrimination and health: Scientific advances, ongoing controversies, and emerging issues. Annual Review of Clinical Psychology, 11, 407–440. https://doi.org/10.1146/annurev-clinpsy-032814-112728
Maldonado, G., & Greenland, S. (1993). Simulation study of confounder-selection strategies. American Journal of Epidemiology, 138(11), 923–936. https://doi.org/10.1093/oxfordjournals.aje.a116813
March of Dimes. (2019). 2019 March of Dimes report card. Retrieved from https://www.marchofdimes.org/materials/US_REPORTCARD_FINAL.pdf
March of Dimes. (2020). Preterm birth rate report card for Virginia. Retrieved from https://www.marchofdimes.org/peristats/tools/reportcard.aspx?frmodrc=1®=51
Office of Disease Prevention and Health Promotion. (2020). Social determinants of health. Retrieved from https://health.gov/healthypeople/objectives-and-data/social-determinants-health
Rowland Hogue, C. J., & Hargraves, M. A. (1993). Class, race, and infant mortality in the United States. American Journal of Public Health, 83(1), 9–12. https://doi.org/10.2105/ajph.83.1.9
Shulman, H. B., D’Angelo, D. V., Harrison, L., Smith, R. A., & Warner, L. (2018). The Pregnancy Risk Assessment Monitoring System (PRAMS): Overview of design and methodology. American Journal of Public Health, 108(10), 1305–1313. https://doi.org/10.2105/AJPH.2018.304563
Tenkku, L. E., Morris, D. S., Salas, J., & Xaverius, P. K. (2009). Racial disparities in pregnancy-related drinking reduction. Maternal and Child Health Journal, 13(5), 604–613. https://doi.org/10.1007/s10995-008-0409-2
U.S. Department of Health and Human Services Office of Disease Prevention and Promotion. (2020). Healthy People 2020 reproductive and sexual health. Retrieved from https://www.healthypeople.gov/2020/leading-health-indicators/2020-lhi-topics/Reproductive-and-Sexual-Health/data.
United Health Foundation. (2020). America’s health rankings: Health of women and children. Retrieved from https://www.americashealthrankings.org/explore/health-of-women-and-children/measure/overall_hwc_2020/state/VA.
Virginia Division of Population Health Data. (2020). Virginia Pregnancy Risk Assessment Monitoring System [Unpublished raw data]. Virginia Department of Health.
Virginia Vital Records and Health Statistics. (2020). Electronic birth certificates and electronic death certificates [Unpublished raw data]. Virginia Department of Health.
Wallace, M. E., Green, C., Richardson, L., Theall, K., & Crear-Perry, J. (2017). “Look at the whole me”: A mixed-methods examination of Black infant mortality in the US through women’s lived experiences and community context. International Journal of Environmental Research and Public Health, 14(7), 727. https://doi.org/10.3390/ijerph14070727
Wallace, M. E., Mendola, P., Liu, D., & Grantz, K. L. (2015). Joint effects of structural racism and income inequality on small-for-gestational-age birth. American Journal of Public Health, 105, 1681–1688. https://doi.org/10.2105/AJPH.2015.302613
Acknowledgements
The authors would like to acknowledge the women who responded to the 2016–2018 Virginia PRAMS questionnaire.
Funding
The VA PRAMS project is supported by funding from the Centers for Disease Control & Prevention (U01DP006250) and the Maternal and Child Health Bureau (H18MC00052).
Author information
Authors and Affiliations
Contributions
Drs. MDR and KFSB conceived of the presented idea. Dr. KFSB developed the theory and performed the computations. Dr. MDR verified the analytical methods. Dr. MDR encouraged Dr. KFSB to investigate the findings by separating and then combining the exposure variables, and to investigate the findings by race. All authors discussed the results and contributed to the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
The study protocol was approved by the Virginia Department of Health’s (VDH) Institutional Review Board (IRB).
Consent to Participate
Participants provided either written or verbal consent to participate in the VA PRAMS study.
Consent for Publication
Participants provided either written or verbal consent to the following: Answers will be grouped with those from other women. Names will not be on any reports from PRAMS. Survey responses may be combined with information the health department has from other sources. Answers will be kept private and will be used only to answer questions related to the purpose of this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Barber, K.F.S., Robinson, M.D. Examining the Influence of Racial Discrimination on Adverse Birth Outcomes: An Analysis of the Virginia Pregnancy Risk Assessment Monitoring System (PRAMS), 2016–2018. Matern Child Health J 26, 691–699 (2022). https://doi.org/10.1007/s10995-021-03223-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-021-03223-2