Abstract
Objectives
Children raised by depressed mothers perform lower on measures of cognitive, emotional, and behavioral skills, compared to children of non-depressed mothers. It is unclear how maternal depressive symptoms (MDS), which persist and accrue over time, impact child development. The purpose of this study was to determine whether cumulative MDS from pre-pregnancy to postpartum influences child development in children by age 2.5.
Methods
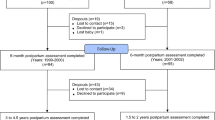
Using a longitudinal population-based study design, 2679 racially and ethnically diverse mothers completed the 2014 Los Angeles Mommy and Baby (LAMB) and 2016 Follow-Up surveys. A total MDS score was created based on responses to standardized questions, including the Patient Health Questionnaire-2 (PHQ-2). Data was collected for before pregnancy, during pregnancy, and 4 months postpartum in the 2014 survey, and at 2.5 years postpartum in the 2016 survey. Child development was measured using the CDC’s Learn the Signs. Act Early Milestones Checklist. Bivariate and multivariate logistic regressions were conducted.
Results
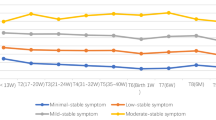
The prevalence of any cumulative MDS was 45.2%. Language, cognitive/adaptive, motor, and social-emotional delays for surveyed toddlers were 7.7%, 4.0%, 1.2%, and 14.2%. After adjusting for covariates, mothers reporting depressive symptoms at all four time points were significantly more likely to report a social-emotional delay in their child (aOR = 4.39, 95% CI − 1.72 to 11.18).
Conclusions for Practice
Mothers with cumulative depressive symptoms are at-risk of reporting social-emotional delays by age 2.5. Understanding these effects may help direct resources to target interventions that support mothers with depressive symptoms early-on and promote positive developmental outcomes among their children.

Similar content being viewed by others
References
Ahun, M. N., Geoffroy, M.-C., Herba, C. M., Brendgen, M., Séguin, J. R., Sutter-Dallay, A.-L., et al. (2017). Timing and chronicity of maternal depression symptoms and children’s verbal abilities. The Journal of Pediatrics, 190, 251–257. https://doi.org/10.1016/j.jpeds.2017.07.007.
Avalos, L. A., Flanagan, T., & Li, D.-K. (2019). Preventing perinatal depression to improve maternal and child health—A health care imperative. JAMA Pediatrics, 173(4), 313. https://doi.org/10.1001/jamapediatrics.2018.5491.
Azad, G., Blacher, J., & Marcoulides, G. A. (2013). Mothers of children with developmental disabilities: Stress in early and middle childhood. Research in Developmental Disabilities, 34(10), 3449–3459. https://doi.org/10.1016/j.ridd.2013.07.009.
Barkin, J. L., Wisner, K. L., Bromberger, J. T., Beach, S. R., & Wisniewski, S. R. (2016). Factors associated with postpartum maternal functioning in women with positive screens for depression. Journal of Womens Health, 25(7), 707–713. https://doi.org/10.1089/jwh.2015.5296.
Batra, P., Higgins, C., & Chao, S. M. (2016). Previous adverse infant outcomes as predictors of preconception care use: An analysis of the 2010 and 2012 Los Angeles Mommy and Baby (LAMB) Surveys. Maternal and Child Health Journal, 20(6), 1170–1177. https://doi.org/10.1007/s10995-015-1904-x.
Bernard-Bonnin, A.-C. (2004). Maternal depression and child development. Paediatrics & Child Health, 9(8), 575–583. https://doi.org/10.1093/pch/9.8.575a.
Brennan, P. A., Hammen, C., Andersen, M. J., Bor, W., Najman, J. M., & Williams, G. M. (2000). Chronicity, severity, and timing of maternal depressive symptoms: Relationships with child outcomes at age 5. Developmental Psychology, 36(6), 759–766. https://doi.org/10.1037/0012-1649.36.6.759.
Bright Futures. (2020). Retrieved May 5, 2020 from https://brightfutures.aap.org/Pages/default.aspx
California Department of Public Health. (2018). Symptoms of depression during and after pregnancy. MIHA data brief. Retrieved May 5, 2020 from https://www.cdph.ca.gov/Programs/CFH/DMCAH/CDPH%2520Document%2520Library/Communications/Data-Brief-MIHA-2018–01.pdf
CDC's Developmental Milestones. (2019, December 5). Retrieved May 5, 2020 from https://www.cdc.gov/ncbddd/actearly/milestones/index.html
Center on the Developing Child. (2009). Maternal depression can undermine the development of young children: Working Paper No. 8. Retrieved May 5, 2020 from https://www.developingchild.harvard.edu/
Centers for Disease Control and Prevention. (CDC). (2019, December 9). PRAMS methodology. Retrieved May 5, 2020 from https://www.cdc.gov/prams/methodology.htm
Chao, S. M., Wakeel, F., Herman, D., Higgins, C., Shi, L., Chow, J., et al. (2014). The 2007 Los Angeles Mommy and Baby Study: A multilevel, population-based study of maternal and infant health in Los Angeles County. Advances in Preventive Medicine, 2014, 1–9. https://doi.org/10.1155/2014/293648.
Chao, S. M., Wakeel, F., Nazinyan, Y., & Sun, S. (2016). Does preconception health differ by nativity?: Findings from the Los Angeles Mommy and Baby (LAMB) Study. Maternal and Child Health Journal, 20(4), 769–777. https://doi.org/10.1007/s10995-015-1907-7.
Comaskey, B., Roos, N. P., Brownell, M., Enns, M. W., Chateau, D., Ruth, C. A., et al. (2017). Maternal depression and anxiety disorders (MDAD) and child development: A Manitoba population-based study. PLoS ONE. https://doi.org/10.1371/journal.pone.0177065.
Committee on Children with Disabilities. (2001). Developmental Surveillance and Screening of Infants and Young Children. Pediatrics, 108(1), 192–195. https://doi.org/10.1542/peds.108.1.192.
Deave, T., Heron, J., Evans, J., & Emond, A. (2008). The impact of maternal depression in pregnancy on early child development. International Journal of Obstetrics & Gynaecology, 115(8), 1043–1051. https://doi.org/10.1111/j.1471-0528.2008.01752.x.
Felder, J. N. (2019). Implementing the USPSTF recommendations on prevention of perinatal depression—Opportunities and challenges. JAMA Internal Medicine, 179(4), 467. https://doi.org/10.1001/jamainternmed.2018.7729.
Field, T. (2010). Postpartum depression effects on early interactions, parenting, and safety practices: A review. Infant Behavior and Development, 33(1), 1–6. https://doi.org/10.1016/j.infbeh.2009.10.005.
Gartstein, M. A., Bridgett, D. J., Dishion, T. J., & Kaufman, N. K. (2009). Depressed mood and maternal report of child behavior problems: Another look at the depression–distortion hypothesis. Journal of Applied Developmental Psychology, 30(2), 149–160. https://doi.org/10.1016/j.appdev.2008.12.001.
Glascoe, F. (1999). The value of parents concerns to detect and address developmental and behavioural problems. Journal of Paediatrics and Child Health, 35(1), 1–8. https://doi.org/10.1046/j.1440-1754.1999.00342.x.
Goodman, S. H., Rouse, M. H., Connell, A. M., Broth, M. R., Hall, C. M., & Heyward, D. (2011). Maternal depression and child psychopathology: A meta-analytic review. Clinical Child and Family Psychology Review, 14(1), 1–27. https://doi.org/10.1007/s10567-010-0080-1.
Hanley, G. E., Brain, U., & Oberlander, T. F. (2013). Infant developmental outcomes following prenatal exposure to antidepressants, and maternal depressed mood and positive affect. Early Human Development, 89(8), 519–524. https://doi.org/10.1016/j.earlhumdev.2012.12.012.
Junge, C., Garthus-Niegel, S., Slinning, K., Polte, C., Simonsen, T. B., & Eberhard-Gran, M. (2016). The Impact of perinatal depression on children’s social-emotional development: A longitudinal study. Maternal and Child Health Journal, 21(3), 607–615. https://doi.org/10.1007/s10995-016-2146-2.
Ko, J. Y., Farr, S. L., Dietz, P. M., & Robbins, C. L. (2012). Depression and treatment among US pregnant and nonpregnant women of reproductive age, 2005–2009. Journal of Womens Health, 21(8), 830–836. https://doi.org/10.1089/jwh.2011.3466.
Ko, J. Y., Rockhill, K. M., Tong, V. T., Morrow, B., & Farr, S. L. (2017). Trends in postpartum depressive symptoms—27 States, 2004, 2008, and 2012 MMWR. Morbidity and Mortality Weekly Report, 66(6), 153–158. https://doi.org/10.15585/mmwr.mm6606a1.
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2003). The patient health questionnaire-2. Medical Care, 41(11), 1284–1292. https://doi.org/10.1097/01.mlr.0000093487.78664.3c.
Los Angeles Mommy and Baby Project (LAMB). (2020). Retrieved May 5, 2020 from https://publichealth.lacounty.gov/mch/LAMB/LAMB.html
National Institute of Mental Health. (2017). Major depression. Retrieved May 5, 2020, from https://www.nimh.nih.gov/health/statistics/major-depression.shtml.
Netsi, E., Pearson, R. M., Murray, L., Cooper, P., Craske, M. G., & Stein, A. (2018). Association of persistent and severe postnatal depression with child outcomes. JAMA Psychiatry, 75(3), 247. https://doi.org/10.1001/jamapsychiatry.2017.4363.
Ordway, M. R. (2011). Depressed mothers as informants on child behavior: Methodological issues. Research in Nursing & Health, 34(6), 520–532. https://doi.org/10.1002/nur.20463.
Pascoe, J. M., Stolfi, A., & Ormond, M. B. (2006). Correlates of mothers’ persistent depressive symptoms: A national study. Journal of Pediatric Health Care, 20(4), 261–269. https://doi.org/10.1016/j.pedhc.2006.01.006.
Patient Health Questionnaire (PHQ) Screeners. (2020). Retrieved May 5, 2020 from https://www.phqscreeners.com/select-screener
Rubin, D. B. (1996). Multiple imputation after 18 Years. Journal of the American Statistical Association, 91(434), 473–489. https://doi.org/10.1080/01621459.1996.10476908.
Shonkoff, J. P., Garner, A. S., Siegel, B. S., Dobbins, M. I., Earls, M. F., Garner, A. S., et al. (2011). The lifelong effects of early childhood adversity and toxic stress. Pediatrics, 129(1), e232–e246. https://doi.org/10.1542/peds.2011-2663.
Weinberg, M. K., & Tronick, E. Z. (1998). Emotional characteristics of infants associated with maternal depression and anxiety. Pediatrics, 102(5 Suppl E), 1298–1304.
Acknowledgements
Diana Liu, MPH, Epidemiologist, LAMB Follow-Up Project Coordinator. Paul Simon, MD, MPH, Chief Science Officer Los Angeles County Public Health Department. David Schonfeld, MD. Sheree Schrager, PhD
Funding
T77MC25732, Maternal Child Health Bureau, Division MCH Workforce Development Developmental Behavioral Pediatrics (DBP) Training Program. The 2014 LAMB and 2016 Follow-Up Surveys were made possible by funding from First Five Los Angeles, LA Care, and Maternal, Child, and Adolescent Health (MCAH) General Funds.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chorbadjian, T.N., Deavenport-Saman, A., Higgins, C. et al. Maternal Depressive Symptoms and Developmental Delay at Age 2: A Diverse Population-Based Longitudinal Study. Matern Child Health J 24, 1267–1277 (2020). https://doi.org/10.1007/s10995-020-02990-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-020-02990-8