Abstract
Objectives
Despite health risks for themselves and their children, urban underserved women smoke at high rates postpartum. The postpartum period is a stressful transition time that presents unique barriers to sustained cessation. There is limited extant evidence of efficacious psychosocial programs to maintain postpartum smoking cessation.
Methods
Guided by the Cognitive-Social Health Information Processing model, we explored the feasibility of TxT2Commit, a text-messaging intervention designed to prevent postpartum smoking relapse. Participants (n = 43) received supportive cessation-focused text messages for one month postpartum. Using a convergent mixed method design, surveys and interviews assessed changes in psychosocial factors and smoking status through a three month follow-up.
Results
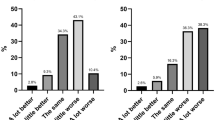
Participants reported satisfaction with TxT2Commit, rating text messages as helpful, understandable, supportive, and not bothersome. However, a majority of women (n = 28, 65.1%) relapsed by three months. Participants who stayed smoke free (i.e., non-relapsers) reported significantly less temptation to smoke at one and three months postpartum compared to relapsers (ps < .01). While relapsers had significantly less temptation at one month compared to baseline, temptation increased by three months (p < .01). Consistent with the quantitative results, qualitative interviews identified informational and coping needs, with continued temptation throughout the three months. Non-relapsers were able to manage temptation and reported greater support.
Conclusions for Practice
TxT2Commit demonstrates preliminary feasibility and acceptability among urban, underserved postpartum women. However, most participants relapsed by three months postpartum. Additional research is needed to identify targeted messaging to best help women avoid temptation and bolster support to stay smoke free in this uniquely stressful period.
Similar content being viewed by others
References
Allen, A. M., Jung, A. M., Lemieux, A. M., Alexander, A. C., Allen, S. S., Ward, K. D., et al. (2018). Stressful life events are associated with perinatal cigarette smoking. Preventive Medicine, 118, 264–271. https://doi.org/10.1016/j.ypmed.2018.11.012.
Anderson-Lewis, C., Darville, G., Mercado, R. E., Howell, S., & Di Maggio, S. (2018). mHealth Technology Use and implications in historically underserved and minority populations in the United States: Systematic literature review. JMIR Mhealth and Uhealth, 6(6), e128. https://doi.org/10.2196/mhealth.8383.
Banderali, G., Martelli, A., Landi, M., Moretti, F., Betti, F., Radaelli, G., et al. (2015). Short and long term health effects of parental tobacco smoking during pregnancy and lactation: A descriptive review. Journal of Translational Medicine, 13, 327–327. https://doi.org/10.1186/s12967-015-0690-y.
Bauld, L., Graham, H., Sinclair, L., Flemming, K., Naughton, F., Ford, A., et al. (2017). Barriers to and facilitators of smoking cessation in pregnancy and following childbirth: Literature review and qualitative study. Health Technology Assessment, 21(36), 1–158. https://doi.org/10.3310/hta21360.
Brandon, T. H., Simmons, V. N., Meade, C. D., Quinn, G. P., Lopez Khoury, E. N., Sutton, S. K., et al. (2012). Self-help booklets for precenting postpartum smoking relapse: A randomized trial. American Journal of Public Health, 102(11), 2109–2115.
Brugha, T., Bebbington, P., Tennant, C., & Hurry, J. (1985). The list of threatening experiences: A subset of 12 life event categories with considerable long-term contextual threat. Psychological Medicine, 15(1), 189–194.
Campbell, J. L., Quincy, C., Osserman, J., & Pedersen, O. K. (2013). Coding in-depth semistructured interviews: Problems of unitization and intercoder reliabilty and agreement. Sociological Methods & Research, 42(3), 294–320.
Chamberlain, C., O'Mara-Eves, A., Porter, J., Coleman, T., Perlen, S. M., Thomas, J., et al. (2017). Psychosocial interventions for supporting women to stop smoking in pregnancy. The Cochrane Database of Systematic Reviews, 2, Cd001055. https://doi.org/10.1002/14651858.CD001055.pub5.
Correa, J. B., Simmons, V. N., Sutton, S. K., Meltzer, L. R., & Brandon, T. H. (2015). A content analysis of attributions for resuming smoking or maintaining abstinence in the post-partum period. Maternal and Child Health Journal, 19(3), 664–674. https://doi.org/10.1007/s10995-014-1556-2.
Creswell, J. W., & Plano Clark, V. L. (2011). Designing and conducting mixed methods research (2nd ed.). Thousand Oaks, CA: Sage Publications Inc.
Diclemente, C. C. (2016). Failure to change or failure to sustain: Pregnancy smoking and postpartum abstinence. Addiction, 111(6), 992–993. https://doi.org/10.1111/add.13393.
Duggan, M. (2013). Cell phone activities 2013. Retrieved from Washington, D.C.: https://www.pewinternet.org/wp-content/uploads/sites/9/media/Files/Reports/2013/PIP_Cell-Phone-Activities-May-2013.pdf.
Fahy. (2001). Addressing some common problems in transcript analysis. The International Review of Research in Open and Distance Learning, 1. https://www.irrodl.org/index/php/irrodl/article/view/321.
Feeney, A., & Britton, G. (2016). Counseling women on smoking relapse prevention during postpartum. MCN: The American Journal of Maternal/Child Nursing, 41(5), 287–292. https://doi.org/10.1097/nmc.0000000000000262.
Ferketich, A. K., Otterson, G. A., King, M., Hall, N., Browning, K. K., & Wewers, M. E. (2012). A pilot test of a combined tobacco dependence treatment and lung cancer screening program. Lung Cancer, 76(2), 211–215.
Goyal, D., Gay, C., & Lee, K. A. (2010). How much does low socioeconomic status increase the risk of prenatal and postpartum depressive symptoms in first-time mothers? Womens Health Issues, 20(2), 96–104. https://doi.org/10.1016/j.whi.2009.11.003.
Hauge, L. J., Torgersen, L., & Vollrath, M. (2012). Associations between maternal stress and smoking: Findings from a population-based prospective cohort study. Addiction, 107(6), 1168–1173. https://doi.org/10.1111/j.1360-0443.2011.03775.x.
Hayes, C. B., Collins, C., O'Carroll, H., Wyse, E., Gunning, M., Geary, M., et al. (2013). Effectiveness of motivational interviewing in influencing smoking cessation in pregnant and postpartum disadvantaged women. Nicotine and Tobbaco Research, 15(5), 969–977. https://doi.org/10.1093/ntr/nts225.
Hiscock, R., Bauld, L., Amos, A., Fidler, J. A., & Munafò, M. (2012). Socioeconomic status and smoking: A review. Annals of the New York Academy of Sciences, 1248(1), 107–123. https://doi.org/10.1111/j.1749-6632.2011.06202.x.
Jones, M., Lewis, S., Parrott, S., & Coleman, T. (2015). Systematic critical review of previous economic evaluations of smoking cessation during pregnancy. British Medical Journal Open, 5(11), e008998. https://doi.org/10.1136/bmjopen-2015-008998.
Jones, M., Lewis, S., Parrott, S., Wormall, S., & Coleman, T. (2016). Re-starting smoking in the postpartum period after receiving a smoking cessation intervention: A systematic review. Addiction, 111(6), 981–990. https://doi.org/10.1111/add.13309.
Kia, F., Tosun, N., Carlson, S., & Allen, S. (2018). Examining characteristics associated with quitting smoking during pregnancy and relapse postpartum. Addictive Behaviors, 78, 114–119. https://doi.org/10.1016/j.addbeh.2017.11.011.
Lee, M., Miller, S. M., Wen, K. Y., Hui, S. A., Roussi, P., & Hernandez, E. (2015). Cognitive-behavioral intervention to promote smoking cessation for pregnant and postpartum inner city women. Journal of Behavioral Medicine, 38(6), 932–943.
Levitt, C., Shaw, E., Wong, S., & Kaczorowski, J. (2007). Systematic review of the literature on postpartum care: Effectiveness of interventions for smoking relapse prevention, cessation, and reduction in postpartum women. Birth, 34(4), 341–347. https://doi.org/10.1111/j.1523-536X.2007.00194.x.
Lindson-Hawley, N., Aveyard, P., & Hughes, J. R. (2012). Reduction versus abrupt cessation in smokers who want to quit. The Cochrane Database of Systematic Reviews, 11, CD008033. https://doi.org/10.1002/14651858.CD008033.pub3.
McLeod, D., Pullon, S., & Cookson, T. (2003). Factors that influence changes in smoking behaviour during pregnancy. New Zealand Medical Journal, 116(1173), U418.
Merzel, C., English, K., & Moon-Howard, J. (2010). Identifying women at-risk for smoking resumption after pregnancy. Maternal and Child Health Journal, 14(4), 600–611. https://doi.org/10.1007/s10995-009-0502-1.
Miller, S. M., & Diefenbach, M. A. (1998). The Cognitive-Social Health Information-Processing (C-SHIP) model: A theoretical framework for research in behavioral oncology. In D. S. Krantz & A. Baum (Eds.), Technology and methods in behavioral medicine (pp. 219–244). Mahwah, NJ: Lawrence Erlbaum Associates Publishers.
Myers, M. G., MacPherson, L., Jones, L. R., & Aarons, G. A. (2007). Measuring adolescent smoking cessation strategies: Instrument development and initial validation. Nicotine and Tobacco Research, 9(11), 1131–1138. https://doi.org/10.1080/14622200701648466.
Nohlert, E., Ohrvik, J., & Helgason, A. R. (2018). Self-perceived ability to cope with stress and depressive mood without smoking predicts successful smoking cessation 12 months later in a quitline setting: A secondary analysis of a randomized trial. BMC Public Health, 18(1), 1066. https://doi.org/10.1186/s12889-018-5973-9.
Orton, S., Coleman, T., Coleman-Haynes, T., & Ussher, M. (2018). Predictors of postpartum return to smoking: A Systematic Review. Nicotine and Tobacco Research, 20(6), 665–673. https://doi.org/10.1093/ntr/ntx163.
Parker, D. R., Windsor, R. A., Roberts, M. B., Hecht, J., Hardy, N. V., Strolla, L. O., et al. (2007). Feasibility, cost, and cost-effectiveness of a telephone-based motivational intervention for underserved pregnant smokers. Nicotine and Tobacco Research, 9(10), 1043–1051. https://doi.org/10.1080/14622200701591617.
Pollak, K. I., Fish, L. J., Lyna, P., Peterson, B. L., Swamy, G. K., & Levine, M. D. (2015). Predictors of pregnant quitters' intention to return to smoking postpartum. Nicotine and Tobacco Research, 17(6), 742–745. https://doi.org/10.1093/ntr/ntu270.
Rai, M., Moniz, M. H., Blaszczak, J., Richardson, C. R., & Chang, T. (2017). Real-time data collection using text messaging in a primary care clinic. Telemedicne and e-Health, 23(12), 955–963.
Reitzel, L. R., Vidrine, J. I., Businelle, M. S., Kendzor, D. E., Costello, T. J., Li, Y., et al. (2010). Preventing postpartum smoking relapse among diverse low-income women: A randomized clinical trial. N Nicotine and Tobacco Research, 12(4), 326–335. https://doi.org/10.1093/ntr/ntq001.
Ripley-Moffitt, C. E., Goldstein, A. O., Fang, W. L., Butzen, A. Y., Walker, S., & Lohr, J. A. (2008). Safe babies: A qualitative analysis of the determinants of postpartum smoke-free and relapse states. Nicotine and Tobacco Research, 10(8), 1355–1364. https://doi.org/10.1080/14622200802238936.
Velicer, W. F., DiClemente, C. C., Prochaska, J. O., & Brandenburg, N. (1985). Decisional balance measure for assessing and predicting smoking status. Journal Personality and Social Psychology, 48(5), 1279–1289.
Velicer, W. F., Diclemente, C. C., Rossi, J. S., & Prochaska, J. O. (1990). Relapse situations and self-efficacy: An integrative model. Addictive Behaviors, 15(3), 271–283.
Wen, K. Y., Miller, S. M., Kilby, L., Fleisher, L., Belton, T. D., Roy, G., et al. (2014). Preventing postpartum smoking relapse among inner city women: Development of a theory-based and evidence-guided text messaging intervention. JMIR Research Protocols, 3(2), e20.
Whittaker, R., McRobbie, H., Bullen, C., Borland, R., Rodgers, A., & Gu, Y. (2012). Mobile phone-based interventions for smoking cessation. The Cochrane Database of Systematic Reviews, 11, Cd006611. https://doi.org/10.1002/14651858.CD006611.pub3.
Acknowledgements
The authors would like to thank Shelby Spohn and Ryan Williams for their technical assistance. This work was supported by the National Cancer Institute at the National Institutes of Health [Grant Numbers RC1CA145063, P30CA06927, T32CA009035].
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tagai, E.K., Miller, S.M., Belfiglio, A. et al. Persistent Barriers to Smoking Cessation Among Urban, Underserved Women: A Feasibility Study of Tailored Barriers Text Messages. Matern Child Health J 24, 1308–1317 (2020). https://doi.org/10.1007/s10995-020-02963-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-020-02963-x