Abstract
Objectives
During the perinatal period, 10–20% of women experience anxiety and/or depression. Untreated perinatal depression has the potential for adverse effects on the family and infant resulting in long-term deleterious consequences. This study measured the association between self-reported depression using the Edinburgh Postnatal Depression Scale scores, self-reported anxiety and neonatal birth outcomes.
Methods
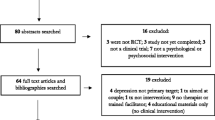
A retrospective design was used with ObstetriX™ data retrieved from 16 metropolitan and rural hospitals in NSW, Australia during 2009–2014. Data were available for 53,646 singleton births. The Edinburgh Postnatal Depression Scale was used to identify self-reported depression while women self-reported pregnancy related anxiety. Regression modelling measured the effects of self-reported depression and self-reported pregnancy related anxiety on neonatal birth outcomes. Linear regression and logistic regression were used to model the effect on birth weight, gestational age, admission to NICU or the SCN, outcome (stillborn vs livebirth), and Apgar scores. Cox proportional hazards regression was used to estimate the effect on neonatal length of stay.
Results
Babies born to women self-reporting anxiety were more likely to have birth complications, be admitted to the nursery, had lower Apgar scores and longer hospital stays. Babies born to women self-identifying as experiencing a level of depression were more likely to have a lower birth weight, shorter gestational age, and, lower Apgar score. These babies were more likely to be admitted to the nursery with an increased length of stay.
Conclusions
Perinatal anxiety and depression contribute to poor birth outcomes. Early detection of maternal perinatal anxiety and depression is an important step towards treatment interventions. More research is needed to identify models of care that are effective in identifying and managing perinatal depression and anxiety to improve birth outcomes for women and their babies.
Similar content being viewed by others
References
American College of Obstetricians and Gynecologists (ACOG) Committee Opinion. (2018). Screening for perinatal depression. Obstetrics and Gynecology,132(5), e208–e212.
Austin, M., Colton, J., Priest, S., Reilly, N., & Hadzi-Pavlovic, D. (2013). The antenatal risk questionnaire (ANRQ): Acceptability and use for psychosocial risk assessment in the maternity setting. Women and Birth,26(1), 17–25. https://doi.org/10.1016/j.wombi.2011.06.002.
Austin, M., Highet, N., & The Expert Working Group. (2017). Mental health care in the perinatal period: Australian clinical practice guideline. Retrieved from http://cope.org.au/about/review-of-new-perinatal-mental-health-guidelines/.
Austin, M., Tully, L., & Parker, G. (2007). Examining the relationship between antenatal anxiety and postnatal depression. Journal of Affective Disorders. https://doi.org/10.1016/j.jad.2006.11.015.
Australian Institute of Health and Welfare (AIHW). (2005). Metadata online registry METeOR. Retrieved February 14, 2020, from https://meteor.aihw.gov.au/content/index.phtml/itemId/327314.
Australian Institute of Health and Welfare (AIHW). (2016). Enhancing maternity data collection and reporting in Australia: National Maternity Data Development Project Stage 2. Cat. no. PER 73. Canberra: AIHW. Retrieved from February 14, 2020, https://www.aihw.gov.au/reports/mothers-babies/enhancing-maternity-data-collection-reporting/contents/table-of-contents.
Bauer, A., Knapp, M., & Parsonage, M. (2016). Lifetime costs of perinatal anxiety and depression. Journal of Affective Disorders,192, 83–90. https://doi.org/10.1016/j.jad.2015.12.005.
Buultjens, M., Murphy, G., Robinson, P., & Milgrom, J. (2013). The perinatal period: A literature review from the biopsychosocial perspective. Clinical Nursing Studies. https://doi.org/10.5430/cns.v1n3p19.
Centre of Perinatal Excellence (COPE). (2014). Postnatal anxiety. Retrieved from http://cope.org.au/first-year/postnatal-mental-health-conditions/postnatal-anxiety/.
Chua, S. C., Treadwell, E. L., Gidaszewski, B., Gibbs, E., Kirby, A., & Khajehei, M. (2018). Validation of the accuracy of postpartum haemorrhage data in the ObstetriX database: A retrospective cohort study. International Journal of Medical Informatics,120, 42–49. https://doi.org/10.1016/j.ijmedinf.2018.09.020.
Connell, T., Barnett, B., & Waters, D. (2018). Barriers to antenatal psychosocial assessment and depression screening in private hospital settings. Women and Birth,31, 292–298. https://doi.org/10.1016/j.wombi.2017.09.021.
Cox, J., & Holden, J. (2003). Perinatal mental health (A guide to the Edinburgh Postnatal Depression Scale). London, UK: Gaskell.
Cox, J., Holden, J., & Sagovsky, R. (1987). Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. British Journal of Psychiatry. https://doi.org/10.1192/bjp.150.6.782.
Deave, T., Johnson, D., & Ingram, J. (2008). Transition to parenthood: The needs of parents in pregnancy and early parenthood. BMC Pregnancy and Childbirth,8(1), 30. https://doi.org/10.1186/1471-2393-8-30.
Dickens, M. J., & Pawluski, J. L. (2018). The HPA axis during the perinatal period: Implications for perinatal depression. Endocrinology,159(11), 3737–3746. https://doi.org/10.1210/en.2018-00677.
Ding, X.-X., Wu, Y.-L., Xu, S.-J., Zhu, R.-P., Jia, X.-M., Zhang, S.-F., et al. (2014). Maternal anxiety during pregnancy and adverse birth outcomes: A systematic review and meta-analysis of prospective cohort studies. Journal of Affective Disorders,159, 103–110. https://doi.org/10.1016/j.jad.2014.02.027.
Fisher, J., Cabral de Mello, M., Patel, V., Rahman, R., Tran, T., Holton, S., et al. (2011). Prevalence and determinants of common perinatal mental disorders in women in low- and lower-middle-income countries: A systematic review. World Health Organization,90(2), 77–156.
He, H., Zhu, L., Chan, S., Chong, Y., Jiao, N., Chan, Y., et al. (2018). The effectiveness and cost-effectiveness of web-based and home-based postnatal psychoeducational interventions for first-time mothers: Randomized controlled trial protocol. JMIR Research Protocols,7(1), e35–e35. https://doi.org/10.2196/resprot.9042.
Highet, N., & Purtell, C. (2012). The national perinatal depression initiative: A synopsis of progress to date and recommendations for beyond 2013. Retrieved from http://cope.org.au/wp-content/uploads/2013/12/Final-Synopsis-Report_PDF.pdf.
Highet, N., Stevenson, A., Purtell, C., & Coo, S. (2014). Qualitative insights into women’s personal experiences of perinatal depression and anxiety. Women and Birth,27, 179–184. https://doi.org/10.1016/j.wombi.2014.05.003.
Martin, C. R. (2012). Perinatal mental health: A clinical guide. Keswick, United Kingdom: M&K Update Ltd.
Meridan Health Informatics. (2017). Obstetrix. Retrieved February 14, 2020, from http://www.meridianhi.com/obstetrix/.
National Health Service England (NHS). (2018). The Perinatal Mental Health Care Pathways. NHS Improvement and National Collaborating Centre for Mental Health. Retrieved from https://www.england.nhs.uk/publication/the-perinatal-mental-health-care-pathways/.
National Institute for Health and Care Excellence (NICE). (2018). Antenatal and postnatal mental health: Clinical management and service guidance (CG192). Retrieved from https://www.nice.org.uk/guidance/cg192/resources/antenatal-and-postnatal-mental-health-clinical-management-and-service-guidance-pdf-35109869806789.
NSW Department of Health. (2010a). NSW health/families NSW supporting families early package—SAFE START Strategic Policy PD2010_016. North Sydney Retrieved from http://www0.health.nsw.gov.au/policies/pd/2010/pdf/PD2010_016.pdf.
NSW Department of Health. (2010b). NSW health/families NSW supporting families early package—SAFE START Guidelines: Improving mental health outcomes for parents and infants GL2010_004. North Sydney: NSW Department of Health. Retrieved from http://www0.health.nsw.gov.au/policies/gl/2010/pdf/GL2010_004.pdf.
Nylen, K. J., O’Hara, M. W., & Engeldinger, J. (2013). Perceived social support interacts with prenatal depression to predict birth outcomes. Journal of Behavioral Medicine,36, 427. https://doi.org/10.1007/s10865-012-9436-y.
O’Hara, M., & Wisner, K. (2014). Perinatal mental illness: Definition, description and aetiology. Best Practice & Research Clinical Obstetrics & Gynaecology,28(1), 3–12. https://doi.org/10.1016/j.bpobgyn.2013.09.002.
Paulson, J. F., Bazemore, S. D., Goodman, J. H., & Leiferman, J. A. (2016). The course and interrelationship of maternal and paternal perinatal depression. Archives of Womens Mental Health,19, 655–663. https://doi.org/10.1007/s00737-016-0598-4.
Perinatal Anxiety & Depression Australia (PANDA) (2019). Submission to the productivity commission mental health inquiry: The social and economic benefits of improving perinatal mental health April 2019. Retrieved February 14, 2020, from https://www.pc.gov.au/__data/assets/pdf_file/0005/240908/sub344-mental-health.pdf.
Petrillo, L. F., Nonacs, R. M., Viguera, A. C., & Chen, L. S. (2005). Course of psychiatric illness during pregnancy and the postpartum. In L. S. Cohen & R. M. Nonacs (Eds.), Mood and Anxiety Disorders during pregnancy and postpartum. Washington, DC: American Psychiatric Publishing.
Reilly, N., Harris, S., Loxton, D., Chojenta, C., Forder, P., Milgrom, J., et al. (2013). Disparities in reported psychosocial assessment across public and private maternity settings: A national survey of women in Australia. BMC Public Health,13(1), 632. https://doi.org/10.1186/1471-2458-13-632.
Reilly, N., Kingston, D., Loxton, D., Talcevska, K., & Austin, M.-P. (2020). A narrative review of studies addressing the clinical effectiveness of perinatal depression screening programs. Women and Birth,33(1), 51–59. https://doi.org/10.1016/j.wombi.2019.03.004.
Somerville, S., Dedman, K., Hagan, R., Oxnam, E., Wettinger, M., Byrne, S., et al. (2014). The Perinatal Anxiety Screening Scale: Development and preliminary validation. Archives of Women’s Mental Health,17(5), 443–454. https://doi.org/10.1007/s00737-014-0425-8.
The Royal Australian and New Zealand College of Obstetricians and Gynaecologists [RANZCOG]. (2018). Mental Health Care in the Perinatal Period. Retrieved February 14, 2020, from https://ranzcog.edu.au/RANZCOG_SITE/media/RANZCOG-MEDIA/Women%27s%20Health/Statement%20and%20guidelines/Clinical-Obstetrics/Mental-health-care-in-the-perinatal-period-(C-Obs-48).pdf?ext=.pdf.
Waqas, A., Raza, N., Lodhi, H. W., Muhammad, Z., Jamal, M., & Rehman, A. (2015). Psychosocial factors of antenatal anxiety and depression in Pakistan: Is social support a mediator? PLoS ONE,10(1), e0116510. https://doi.org/10.1371/journal.pone.0116510.
Yelland, J., & Brown, S. (2014). Asking women about mental health and social adversity in pregnancy: Results of an Australian population-based survey. Birth,41(1), 79–87. https://doi.org/10.1111/birt.12083.
Yelland, J., Sutherland, G., Wiebe, J., & Brown, S. (2009). A national approach to perinatal mental health in Australia: Exercising caution in the roll-out of a public health initiative. Medical Journal of Australia,191(5), 276–279.
Acknowledgements
1. Pilot Grant, Priority Research Centre for Brain & Mental Health, University of Newcastle, Australia.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dowse, E., Chan, S., Ebert, L. et al. Impact of Perinatal Depression and Anxiety on Birth Outcomes: A Retrospective Data Analysis. Matern Child Health J 24, 718–726 (2020). https://doi.org/10.1007/s10995-020-02906-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-020-02906-6