Abstract
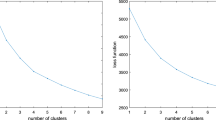
Objectives Domains of psychosocial health have been separately connected to pregnancy outcomes. This study explores the relationship between five domains of psychosocial health and their joint association with prenatal health and pregnancy outcomes. Methods Women from a prospective cohort study in Durham, North Carolina were clustered based on measures of paternal support, perceived stress, social support, depression, and self-efficacy. Clusters were constructed using the K-means algorithm. We examined associations between psychosocial health and maternal health correlates, pregnancy intention, and pregnancy outcomes using Chi square tests and multivariable models. Results Three psychosocial health profiles were identified, with the first (Resilient; n = 509) characterized by low depression and perceived stress and high interpersonal support, paternal support, and self-efficacy. The second profile (Vulnerable; n = 278) was marked by high depression and perceived stress, and low interpersonal support, paternal support, and self-efficacy. The third profile (Moderate, n = 526) fell between the other profiles on all domains. Health correlates, pregnancy intention, and pregnancy outcomes varied significantly across profiles. Women with the vulnerable profile were more likely to have risky health correlates, have an unintended pregnancy, and deliver preterm. Women with the resilient profile had better birth outcomes and fewer deleterious health correlates, preconception and prenatally. Conclusions We posit that vulnerable psychosocial health, deleterious health correlates, and the stress which often accompanies pregnancy may interact to magnify risk during pregnancy. Identifying and intervening with women experiencing vulnerable psychosocial health may improve outcomes for women and their children.

Similar content being viewed by others
References
Kramer, M. S., Seguin, L., Lydon, J., & Goulet, L. (2000). Socio-economic disparities in pregnancy outcome: Why do the poor fare so poorly? Paediatric and Perinatal Epidemiology, 14(3), 194–210.
Neggers, Y., Goldenberg, R., Cliver, S., & Hauth, J. (2006). The relationship between psychosocial profile, health practices, and pregnancy outcomes. Acta Obstetricia et Gynecologica Scandinavica, 85(3), 277–285.
Ritter, C., Hobfoll, S. E., Lavin, J., Cameron, R. P., & Hulsizer, M. R. (2000). Stress, psychosocial resources, and depressive symptomatology during pregnancy in low-income, inner-city women. Health Psychology, 19(6), 576–585.
Kurki, T., Hiilesmaa, V., Raitasalo, R., Mattila, H., & Ylikorkala, O. (2000). Depression and anxiety in early pregnancy and risk for preeclampsia. Obstetrics and Gynecology, 95(4), 487–490.
Leiferman, J. (2002). The effect of maternal depressive symptomatology on maternal behaviors associated with child health. Health Education & Behavior, 29(5), 596–607.
Maxson, P. J., Edwards, S. E., Ingram, A., & Miranda, M. L. (2012). Psychosocial differences between smokers and non-smokers during pregnancy. Addictive Behaviors, 37(2), 153–159.
Grote, N. K., Bridge, J. A., Gavin, A. R., Melville, J. L., Iyengar, S., & Katon, W. J. (2010). A meta-analysis of depression during pregnancy and the risk of preterm birth, low birth weight, and intrauterine growth restriction. Archives of General Psychiatry, 67(10), 1012–1024.
Dole, N., Savitz, D. A., Hertz-Picciotto, I., Siega-Riz, A. M., McMahon, M. J., & Buekens, P. (2003). Maternal stress and preterm birth. American Journal of Epidemiology, 157(1), 14–24.
Zuckerman, B., Amaro, H., Bauchner, H., & Cabral, H. (1989). Depressive symptoms during pregnancy: Relationship to poor health behaviors. American Journal of Obstetrics and Gynecology, 160(5 Pt 1), 1107–1111.
Beck, C. T. (2002). Revision of the postpartum depression predictors inventory. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 31(4), 394–402.
Feldman, P. J., Dunkel-Schetter, C., Sandman, C. A., & Wadhwa, P. D. (2000). Maternal social support predicts birth weight and fetal growth in human pregnancy. Psychosomatic Medicine, 62(5), 715–725.
Borders, A. E., Grobman, W. A., Amsden, L. B., & Holl, J. L. (2007). Chronic stress and low birth weight neonates in a low-income population of women. Obstetrics and Gynecology, 109(2 Pt 1), 331–338.
Copper, R. L., Goldenberg, R. L., Das, A., Elder, N., Swain, M., Norman, G., et al. (1996). The preterm prediction study: Maternal stress is associated with spontaneous preterm birth at less than thirty-five weeks’ gestation. National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. American Journal of Obstetrics and Gynecology, 175(5), 1286–1292.
Rini, C. K., Dunkel-Schetter, C., Wadhwa, P. D., & Sandman, C. A. (1999). Psychological adaptation and birth outcomes: The role of personal resources, stress, and sociocultural context in pregnancy. Health Psychology, 18(4), 333–345.
Lu, M. C., Kotelchuck, M., Hogan, V., Jones, L., Wright, K., & Halfon, N. (2010). Closing the black–white gap in birth outcomes: A life-course approach. Ethnicity and Disease, 20(1 Suppl 2), S2–S76.
Lancaster, C. A., Gold, K. J., Flynn, H. A., Yoo, H., Marcus, S. M., & Davis, M. M. (2010). Risk factors for depressive symptoms during pregnancy: A systematic review. American Journal of Obstetrics and Gynecology, 202(1), 5–14.
Dole, N., Savitz, D. A., Siega-Riz, A. M., Hertz-Picciotto, I., McMahon, M. J., & Buekens, P. (2004). Psychosocial factors and preterm birth among African American and White women in central North Carolina. American Journal of Public Health, 94(8), 1358–1365.
Hogue, C. J., & Bremner, J. D. (2005). Stress model for research into preterm delivery among black women. American Journal of Obstetrics and Gynecology, 192(5 Suppl), S47–S55.
Maciejewski, P. K., Prigerson, H. G., & Mazure, C. M. (2000). Self-efficacy as a mediator between stressful life events and depressive symptoms. Differences based on history of prior depression. British Journal of Psychiatry, 176, 373–378.
Cobb, S. (1976). Social support as a moderator of life stress. Psychosomatic Medicine, 38(5), 300.
Ghosh, J. K., Wilhelm, M. H., Dunkel-Schetter, C., Lombardi, C. A., & Ritz, B. R. (2010). Paternal support and preterm birth, and the moderation of effects of chronic stress: A study in Los Angeles county mothers. Archives of Women’s Mental Health, 13(4), 327–338.
Carlson, M., McLanahan, S., & England, P. (2004). Union formation in fragile families. Demography, 41(2), 237–261.
Cohen, S., & Williamson, G. (1988). Perceived stress in a probability sample of the United States. In S. Spacapam (Ed.), The social psychology of health (pp. 31–67). Thousand Oaks, CA: Sage Publications, Inc.
Cohen, S., & Wills, T. A. (1985). Stress, social support, and the buffering hypothesis. Psychological Bulletin, 98(2), 310–357.
Radloff, L. S. (1977). The CES-D Scale. Applied Psychological Measurement, 1(3), 385.
Jerusalem, M., & Schwarzer, R. (1992). Self-efficacy as a resource factor in stress appraisal processes. Self-efficacy: Thought control of action (pp. 195–213). Washington, DC: Hemisphere Publishing Corp.
Centers for Disease Control and Prevention. Pregnancy Risk Assessment Monitoring System. (2014). Divison of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion. Ref Type: Online Source.
Elo, I. T., Culhane, J. F., Kohler, I. V., O’Campo, P., Burke, J. G., Messer, L. C., et al. (2009). Neighbourhood deprivation and small-for-gestational-age term births in the United States. Paediatric and Perinatal Epidemiology, 23(1), 87–96.
Asendorpf, J. B., Borkenau, P., Ostendorf, F., & Van Aken, M. A. (2001). Carving personality description at its joints: Confirmation of three replicable personality prototypes for both children and adults. European Journal of Personality, 15(3), 169–198.
Hobel, C. J., Goldstein, A., & Barrett, E. S. (2008). Psychosocial stress and pregnancy outcome. Clinical Obstetrics and Gynecology, 51(2), 333–348.
Knackstedt, M. K., Hamelmann, E., & Arck, P. C. (2005). Mothers in stress: Consequences for the offspring. American Journal of Reproductive Immunology, 54(2), 63–69.
Kramer, M. R., & Hogue, C. R. (2009). What causes racial disparities in very preterm birth? A biosocial perspective. Epidemiologic Reviews, 31, 84–98.
Lu, M. C., & Halfon, N. (2003). Racial and ethnic disparities in birth outcomes: A life-course perspective. Maternal and Child Health Journal, 7(1), 13–30.
Savitz, D. A., Kaufman, J. S., Dole, N., Siega-Riz, A. M., Thorp, J. M, Jr, & Kaczor, D. T. (2004). Poverty, education, race, and pregnancy outcome. Ethnicity and Disease, 14(3), 322–329.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maxson, P.J., Edwards, S.E., Valentiner, E.M. et al. A Multidimensional Approach to Characterizing Psychosocial Health During Pregnancy. Matern Child Health J 20, 1103–1113 (2016). https://doi.org/10.1007/s10995-015-1872-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-015-1872-1