Abstract
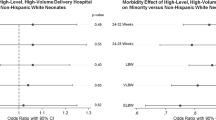
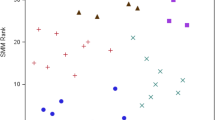
Objectives In the United States, significant ethnic and racial health and healthcare disparities exist among our most vulnerable populations, new mothers and newborns. We sought to determine disparities in socioeconomic status, perinatal health, and perinatal healthcare for black mothers and their newborns cared for in well-baby nurseries compared with white mother/baby pairs in Pennsylvania. Methods A retrospective analysis of a merged data set containing birth and clinical discharge records was conducted. Perinatal data from 44,105 black mothers and their singleton newborns, ≥35 weeks gestational age cared for in Pennsylvania well-baby nurseries from 1998–2002 were compared with 88,210 white mother/baby pairs. Results Black mothers were younger and were much more likely to receive Medicaid or be uninsured compared with white mothers. They were less likely to be college-educated, married, or have prenatal care beginning in the first trimester. Infants born to black mothers were less likely to be delivered via Cesarean section, but were more likely to be born between 35 and 38 weeks gestation and be of low birth weight. Conclusions Numerous significant disparities exist for black mothers and their newborns cared for in well-baby nurseries in Pennsylvania. Since most newborns are cared for in this setting as opposed to intensive care environments, recognition of the differences that exist for this group when compared to well newborns of white mothers can help to improve healthcare and its delivery to this population. Federal and local initiatives must continue efforts to eliminate racial disparities.
Similar content being viewed by others
Abbreviations
- AAP:
-
American Academy of Pediatrics
- PDOH:
-
Pennsylvania Department of Health
- PHC4:
-
Pennsylvania Health Care Cost Containment Council
- LOS:
-
Length of stay
References
US Department of Health and Human Services. (2000). Healthy people 2010. Washington, DC: US Department of Health and Human Services, Office on Women’s Health.
Smedley, B. D., Stith, A. Y., & Nelson, A. R., (Eds.) (2003). Institute of Medicine. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, D.C.: National Academies Press.
Groman, R., & Ginsburg, J. (2004). Racial and ethnic disparities in health care: A position paper of the American College of Physicians. Annals of Internal Medicine, 141(3), 226–232.
2005 National healthcare disparities report. Rockville, MD: U.S. Department of Health and Human Services, Agency for Healthcare Research and Quality; 2005.
Vintzileos, A. M., Ananth, C. V., Smulian, J. C., Scorza, W. E., & Knuppel, R. A. (2002). Prenatal care and black-white fetal death disparity in the United States: Heterogeneity by high-risk conditions. Obstetrics and Gynecology, 99(3), 483–489.
Racial/ethnic disparities in neonatal mortality—United States, 1989–2001. MMWR Morbidity and Mortality Weekly Report 2004;53(29), 655–658.
Hoyert, D. L., Mathews, T. J., Menacker, F., Strobino, D. M., & Guyer, B. (2006). Annual summary of vital statistics: 2004. Pediatrics, 117(1), 168–183.
Maternal mortality—United States, (1982–1996). MMWR. Morbidity and Mortality Weekly Report (1998) 47(34), 705–707.
Mathews, T. J., & MacDorman, M. F. (2007). Infant mortality statistics from the 2004 period linked birth/infant death data set. National Vital Statistics Reports, 55(14), 1–32.
Anachebe, N. F., & Sutton, M. Y. (2003). Racial disparities in reproductive health outcomes. American Journal of Obstetrics and Gynecology, 188(4), S37–S42.
Parham, G. P., & Hicks, M. L. (2005). Racial disparities affecting the reproductive health of African-American women. The Medical Clinics of North America, 89(5), 935–943, 41.
Alexander, G. R., Kogan, M. D., & Nabukera, S. (2002). Racial differences in prenatal care use in the United States: Are disparities decreasing? American Journal of Public Health, 92(12), 1970–1975.
Entry into prenatal care—United States, (1989–1997) MMWR. Morbidity and Mortality Weekly Report (2000)49, 393–398.
Frisbie, W. P., Echevarria, S., & Hummer, R. A. (2001). Prenatal care utilization among non-Hispanic Whites, African Americans, and Mexican Americans. Maternal and Child Health Journal, 5(1), 21–33.
Alexander, G. R., & Cornely, D. A. (1987). Racial disparities in pregnancy outcomes: The role of prenatal care utilization and maternal risk status. American Journal of Preventive Medicine, 3(5), 254–261.
Bernstein, H. H., Spino, C., Finch, S., et al. (2007). Decision-making for postpartum discharge of 4300 mothers and their healthy infants: The life around newborn discharge study. Pediatrics, 120, e391–e400.
http://www.mediqual.com/
Grupp-Phelan, J., Taylor, J. A., Liu, L. L., & Davis, R. L. (1999). Early newborn hospital discharge and readmission for mild and severe jaundice. Archives of Pediatrics & Adolescent Medicine, 153(12), 1283–1288.
Mandl, K. D., Brennan, T. A., Wise, P. H., Tronick, E. Z., & Homer, C. J. (1997). Maternal and infant health: Effects of moderate reductions in postpartum length of stay. Archives of Pediatrics & Adolescent Medicine, 151(9), 915–921.
Mosen, D. M., Clark, S. L., Mundorff, M. B., Tracy, D. M., McKnight, E. C., & Zollo, M. B. (2002). The medical and economic impact of the newborns’ and Mothers’ Health Protection Act. Obstetrics and Gynecology, 99(1), 116–124.
Liu, L. L., Clemens, C. J., Shay, D. K., Davis, R. L., & Novack, A. H. (1997). The safety of newborn early discharge. The Washington state experience. JAMA: The Journal of the American Medical Association, 278(4), 293–298.
Edmonson, M. B., Stoddard, J. J., & Owens, L. M. (1997). Hospital readmission with feeding-related problems after early postpartum discharge of normal newborns. JAMA: The Journal of the American Medical Association, 278(4), 299–303.
Galbraith, A. A., Egerter, S. A., Marchi, K. S., Chavez, G., & Braveman, P. A. (2003). Newborn early discharge revisited: Are California newborns receiving recommended postnatal services? Pediatrics, 111(2), 364–371.
Paul, I. M., Lehman, E. B., Hollenbeak, C. S., & Maisels, M. J. (2006). Preventable newborn readmissions since passage of the Newborns’ and Mothers’ Health Protection Act. Pediatrics, 118(6), 2349–2358.
Frisbie, W. P., Biegler, M., de Turk, P., Forbes, D., & Pullum, S. G. (1997). Racial and ethnic differences in determinants of intrauterine growth retardation and other compromised birth outcomes. American Journal of Public Health, 87(12), 1977–1983.
Fraser, A. M., Brockert, J. E., & Ward, R. H. (1995). Association of young maternal age with adverse reproductive outcomes. The New England Journal of Medicine, 332(17), 1113–1117.
Manning, W. D. (2001). Childbearing in cohabiting unions: Racial and ethnic differences. Family Planning Perspectives, 33(5), 217–223.
Brown, S. L. (2000). The effect of union type on psychological well-being: Depression among cohabitors versus marrieds. Journal of Health and Social Behaviour, 41(3), 241–255.
Luo, Z. C., Wilkins, R., & Kramer, M. S. (2004). Disparities in pregnancy outcomes according to marital and cohabitation status. Obstetrics and Gynecology, 103(6), 1300–1307.
Kenney, C. T., & McLanahan, S. S. (2006). Why are cohabiting relationships more violent than marriages? Demography, 43(1), 127–140.
Manning, W. D., & Smock, P. J. (1995). Why marry? Race and the transition to marriage among cohabitors. Demography, 32(4), 509–520.
Moffitt, R. A., Reville, R., & Winkler, A. E. (1998). Beyond single mothers: cohabitation and marriage in the AFDC program. Demography, 35(3), 259–278.
Lichter, D. T., Qian, Z., & Mellott, L. M. (2006). Marriage or dissolution? Union transitions among poor cohabiting women. Demography, 43(2), 223–240.
Santorum, R. (2005). It takes a family: Conservatism, the common good. Wilmington, DE: ISI Books.
Tossounian, S. A., Schoendorf, K. C., & Kiely, J. L. (1997). Racial differences in perceived barriers to prenatal care. Maternal Child Health Journal, 1(4), 229–236.
Mikhail, B. I. (1999). Perceived impediments to prenatal care among low-income women. West Journal of Nursing Research, 21(3), 335–350; discussion 51–55.
Johnson, A. A., El-Khorazaty, M. N., Hatcher, B. J., et al. (2003). Determinants of late prenatal care initiation by African American women in Washington, DC. Maternal Child Health Journal, 7(2), 103–114.
Orstead, C., Arrington, D., Kamath, S. K., Olson, R., & Kohrs, M. B. (1985). Efficacy of prenatal nutrition counseling: Weight gain, infant birth weight, and cost-effectiveness. Journal of American Dietetic Association, 85(1), 40–45.
Racine, A., Joyce, T., & Anderson, R. (1993). The association between prenatal care and birth weight among women exposed to cocaine in New York City. JAMA: The Journal of the American Medical Association, 270(13), 1581–1586.
Sable, M. R., & Herman, A. A. (1997). The relationship between prenatal health behavior advice and low birth weight. Public Health Report, 112(4), 332–339.
Kogan, M. D., Alexander, G. R., Kotelchuck, M., & Nagey, D. A. (1994). Relation of the content of prenatal care to the risk of low birth weight. Maternal reports of health behavior advice and initial prenatal care procedures. JAMA: The Journal of the American Medical Association, 271(17), 1340–1345.
Kotelchuck, M. (1994). The adequacy of prenatal care utilization index: Its US distribution and association with low birthweight. American Journal of Public Health, 84(9), 1486–1489.
Murray, J. L., & Bernfield, M. (1988). The differential effect of prenatal care on the incidence of low birth weight among blacks and whites in a prepaid health care plan. The New England Journal of Medicine, 319(21), 1385–1391.
Kogan, M. D., Alexander, G. R., Jack, B. W., & Allen, M. C. (1998). The association between adequacy of prenatal care utilization and subsequent pediatric care utilization in the United States. Pediatrics, 102(1 Pt 1), 25–30.
York, R., Tulman, L., & Brown, K. (2000). Postnatal care in low-income urban African American women: Relationship to level of prenatal care sought. Journal of Perinatology, 20(1), 34–40.
Gemperline, P., Brockert, J., & Osborn, L. M. (1989). Preventive health care utilization. Prenatal and the first 3 years in a Utah population. Clinical Pediatrics (Phila), 28(1), 34–37.
Butz, A. M., Funkhouser, A., Caleb, L., & Rosenstein, B. J. (1993). Infant health care utilization predicted by pattern of prenatal care. Pediatrics, 92(1), 50–54.
Wiecha, J. M., & Gann, P. (1994). Does maternal prenatal care use predict infant immunization delay? Family Medicine, 26(3), 172–178.
Gould, J. B., Davey, B., & Stafford, R. S. (1989). Socioeconomic differences in rates of cesarean section. The New England Journal of Medicine, 321(4), 233–239.
Kabir, A. A., Pridjian, G., Steinmann, W. C., Herrera, E. A., & Khan, M. M. (2005). Racial differences in cesareans: An analysis of U.S. 2001 national inpatient sample data. Obstetrics and Gynecology, 105(4), 710–718.
Papiernik, E., Cohen, H., Richard, A., de Oca, M. M., & Feingold, J. (1986). Ethnic difference in duration of pregnancy. Annals of Human Biology, 13(3), 259–265.
Shiono, P. H., Klebanoff, M. A., Graubard, B. I., Berendes, H. W., & Rhoads, G. G. (1986). Birth weight among women of different ethnic groups. JAMA: The Journal of the American Medical Association, 255(1), 48–52.
Blendon, R. J., Scheck, A. C., Donelan, K., et al. (1995). How white and African Americans view their health and social problems. Different experiences, different expectations. JAMA: The Journal of the American Medical Association, 273(4), 341–346.
Rust, G., Fryer, G. E. Jr., Phillips, R. L. Jr., Daniels, E., Strothers, H., & Satcher, D. (2004). Modifiable determinants of healthcare utilization within the African-American population. Journal of National Medical Association, 96(9), 1169–1177.
Beal, A. C. (2004). Policies to reduce racial and ethnic disparities in child health and health care. Health Affairs (Millwood), 23(5), 171–179.
Acknowledgements
Dr. Paul is supported by grant R40 MC 06630 from the Maternal Child Health Bureau (Title V, Social Security Act), Health Resources and Services Administration, Department of Health and Human Services. A Penn State College of Medicine Dean’s Feasibility Grant as well as a grant from the Children’s Miracle Network awarded to Dr. Paul also supported this work. Co-author, Erik Lehman, MS, had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. The authors thank Maxine Vance and Rosalind German for their review and editorial comments, and Edward Hain from the Pennsylvania Healthcare Cost Containment Council (PHC4) for his extensive technical assistance. Additional assistance was provided by Craig Edelman from the Pennsylvania Department of Health. PHC4, who provided the clinical discharge records, is an independent state agency responsible for addressing the problem of escalating health costs, ensuring the quality of healthcare, and increasing access to health care for all citizens regardless of ability to pay. PHC4 provided their data in an effort to further PHC4’s mission of educating the public and containing health care costs in Pennsylvania. PHC4, its agents, and staff, have made no representation, guarantee, or warranty, express or implied, that the data: financial, patient, payor, and physician specific information provided to this entity, are error-free, or that the use of the data will avoid differences of opinion or interpretation. The authors of this manuscript conducted this analysis without the assistance of PHC4, which bears no responsibility or liability for the results of the analysis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Paul, I.M., Lehman, E.B., Suliman, A.K. et al. Perinatal Disparities for Black Mothers and Their Newborns. Matern Child Health J 12, 452–460 (2008). https://doi.org/10.1007/s10995-007-0280-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-007-0280-6