Abstract
Women with diffuse large B-cell lymphoma (DLBCL) are at an increased risk of mortality from breast cancer and osteoporosis. However, the impact of DLBCL on rates of mammography and bone density testing (BDT) is unknown. We compared female DLBCL and non-cancer patients utilizing the Surveillance, Epidemiology, and End Results-Medicare dataset to analyze the predictors of mammography and BDT. Guided by the Social Ecological Model (SEM), we used multivariable logistic regressions with inverse probability treatment weighting to examine the association of intrapersonal, interpersonal, healthcare system, and community factors with mammography and BDT. The rates of mammography (59.8%) and BDT (18.5%) in women with DLBCL were similar to those without cancer (60.2% and 19.6%, respectively). After adjusting for the SEM factors, DLBCL patients were less likely to get mammography and BDT than non-cancer patients. The treatments of radiotherapy and stem cell transplant were not associated with either mammography or BDT. DLBCL diagnosis was associated with lower rates of mammography and BDT rates among women with DLBCL, as compared to non-cancer patients. To reduce the morbidity and mortality from breast cancer and fractures in women with DLBCL, providers should increase their recommendations for mammography in those receiving radiotherapy and BDT in stem cell transplant patients.
Similar content being viewed by others
References
American Cancer Society. (2019). Second cancers after Non-Hodgkin lymphoma. Retrieved Nov 24, 2020 from https://www.cancer.org/cancer/non-hodgkin-lymphoma/after-treatment/second-cancers.html.
Austin, P. C., & Stuart, E. A. (2015). Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies. Statistics in Medicine, 34(28), 3661–3679.
Block, L. D., Jarlenski, M. P., Wu, A. W., & Bennett, W. L. (2013). Mammography use among women ages 40–49 after the 2009 US preventive services task force recommendation. Journal of General Internal Medicine, 28(11), 1447–1453.
Chun, K. J. (2011). Bone densitometry. Seminars in Nuclear Medicine, 41(3), 220–228.
Curry, S. J., Krist, A. H., Owens, D. K., Barry, M. J., Caughey, A. B., Davidson, K. W., & Kubik, M. (2018). Screening for osteoporosis to prevent fractures: US preventive services task force recommendation statement. JAMA, 319(24), 2521–2531.
DeSantis, C. E., Lin, C. C., Mariotto, A. B., Siegel, R. L., Stein, K. D., Kramer, J. L., & Jemal, A. (2014). Cancer treatment and survivorship statistics, 2014. CA: A Cancer Journal for Clinicians, 64(4), 252–271.
Doubeni, C. A., Field, T. S., Ulcickas Yood, M., Rolnick, S. J., Quessenberry, C. P., Fouayzi, H., & Wei, F. (2006). Patterns and predictors of mammography utilization among breast cancer survivors. Cancer, 106(11), 2482–2488.
Earle, C. C., Burstein, H. J., Winer, E. P., & Weeks, J. C. (2003). Quality of non-breast cancer health maintenance among elderly breast cancer survivors. Journal of Clinical Oncology: Official Journal of the American Society of Clinical Oncology, 21(8), 1447–1451. https://doi.org/10.1200/JCO.2003.03.060.
Earle, C. C., & Neville, B. A. (2004). Under use of necessary care among cancer survivors. Cancer, 101(8), 1712–1719.
Finkelstein, M. M. (2002). Preventive screening. What factors influence testing? Canadian Family Physician Medecin De Famille Canadien, 48, 1494–1501.
Giordano, S. H., Kuo, Y. F., Duan, Z., Hortobagyi, G. N., Freeman, J., & Goodwin, J. S. (2008). Limits of observational data in determining outcomes from cancer therapy. Cancer: Interdisciplinary International Journal of the American Cancer Society, 112(11), 2456–2466.
Gourlay, M. L., Fine, J. P., Preisser, J. S., May, R. C., Li, C., Lui, L., & Ensrud, K. E. (2012). Bone-density testing interval and transition to osteoporosis in older women. New England Journal of Medicine, 366(3), 225–233.
Healthy People 2030. (2020). Retrieved Nov 24, 2020 from https://health.gov/healthypeople/objectives-and-data/browse-objectives
Hillier, T. A., Stone, K. L., Bauer, D. C., Rizzo, J. H., Pedula, K. L., Cauley, J. A., & Cummings, S. R. (2007). Evaluating the value of repeat bone mineral density measurement and prediction of fractures in older women: The study of osteoporotic fractures. Archives of Internal Medicine, 167(2), 155–160.
Lafata, J. E., Salloum, R. G., Fishman, P. A., Ritzwoller, D. P., O’Keeffe-Rosetti, M. C., & Hornbrook, M. C. (2015). Preventive care receipt and office visit use among breast and colorectal cancer survivors relative to age-and gender-matched cancer-free controls. Journal of Cancer Survivorship, 9(2), 201–207.
Leslie, W. D., Tsang, J. F., Caetano, P. A., & Lix, L. M. (2007). Effectiveness of bone density measurement for predicting osteoporotic fractures in clinical practice. The Journal of Clinical Endocrinology and Metabolism, 92(1), 77–81.
Li, S., Young, K. H., & Medeiros, L. J. (2018). Diffuse large B-cell lymphoma. Pathology, 50(1), 74–87.
Majhail, N. S., Mau, L., Denzen, E. M., & Arneson, T. J. (2013). Costs of autologous and allogeneic hematopoietic cell transplantation in the united states: A study using a large national private claims database. Bone Marrow Transplantation, 48(2), 294–300.
Mandelblatt, J., Saha, S., Teutsch, S., Hoerger, T., Siu, A. L., Atkins, D., & Helfand, M. (2003). The cost-effectiveness of screening mammography beyond age 65 years: A systematic review for the US preventive services task force. Annals of Internal Medicine, 139(10), 835–842.
Mobley, L. R., Driscoll, D., Clayton, L., & Anselin, L. (2008). Heterogeneity in mammography use across the nation: Separating evidence of disparities from the disproportionate effects of geography. International Journal of Health Geographics, 7(1), 1.
Mobley, L., Kuo, T. M., Urato, M., Boos, J., Lozano-Gracia, N., & Anselin, L. (2010). Predictors of endoscopic colorectal cancer screening over time in 11 states. Cancer Causes and Control, 21(3), 445–461.
Moore, A. R., Buchanan, N. D., Fairley, T. L., & Smith, J. L. (2015). Public health action model for cancer survivorship. American Journal of Preventive Medicine, 49(6), S470–S476.
Morton, L. M., Curtis, R. E., Linet, M. S., Bluhm, E. C., Tucker, M. A., Caporaso, N., & Fraumeni, J. F., Jr. (2010). Second malignancy risks after non-hodgkin’s lymphoma and chronic lymphocytic leukemia: Differences by lymphoma subtype. Journal of Clinical Oncology : Official Journal of the American Society of Clinical Oncology, 28(33), 4935–4944. https://doi.org/10.1200/JCO.2010.29.1112.
National Cancer Institute. (2020). Division of cancer control & population sciences. SEER-Medicare linked database. Retrieved Nov 24, 2020 from https://healthcaredelivery.cancer.gov/seermedicare/.
Nutting, P. A., Baier, M., Werner, J. J., Cutter, G., Conry, C., & Stewart, L. (2001). Competing demands in the office visit: What influences mammography recommendations? The Journal of the American Board of Family Practice, 14(5), 352–361.
Paccou, J., Merlusca, L., Henry-Desailly, I., Parcelier, A., Gruson, B., Royer, B., & Damaj, G. (2014). Alterations in bone mineral density and bone turnover markers in newly diagnosed adults with lymphoma receiving chemotherapy: A 1-year prospective pilot study. Annals of Oncology: Official Journal of the European Society for Medical Oncology, 25(2), 481–486. https://doi.org/10.1093/annonc/mdt560.
Sanna, G., Lorizzo, K., Rotmensz, N., Bagnardi, V., Cinieri, S., Colleoni, M., & Goldhirsch, A. (2007). Breast cancer in hodgkin’s disease and non-hodgkin’s lymphoma survivors. Annals of Oncology: Official Journal of the European Society for Medical Oncology, 18(2), 288–292.
SEER. (2020a). Cancer Stat Facts: Non-Hodgkin’s Lymphoma. National Cancer Institute. Bethesda, MD, Retrieved Nov 24, 2020 from https://seer.cancer.gov/statfacts/html/nhl.html
SEER. (2020b). Cancer Stat Facts: Diffuse large B-cell lymphoma. National Cancer Institute. Bethesda, MD, Retrieved Nov 24, 2020 from https://seer.cancer.gov/statfacts/html/dlbcl.html
SEER. (2020c). Cancer Stat Facts: Breast cancer. National Cancer Institute. Bethesda, MD, Retrieved Nov 24, 2020 fromhttps://seer.cancer.gov/statfacts/html/breast.html
Smith, R. A., Andrews, K. S., Brooks, D., Fedewa, S. A., Manassaram-Baptiste, D., Saslow, D., & Wender, R. C. (2018). Cancer screening in the United States, 2018: A review of current American cancer society guidelines and current issues in cancer screening. CA: A Cancer Journal for Clinicians, 68(4), 297–316.
Svendsen, P., Shekhrajka, N., Nielsen, K. L., Vestergaard, P., Poulsen, M. Ø., Vistisen, A. K., & Jakobsen, L. H. (2017). R-CHOP (-like) treatment of diffuse large B-cell lymphoma significantly reduces CT-assessed vertebral bone density: A single center study of 111 patients. Leukemia and Lymphoma, 58(5), 1105–1113.
US Department of Health and Human Services. (2019). Area health resource file (AHRF). Rockville, MD: Health Resources and Services Administration, Retrieved Nov 24, 2020 from http://ahrf.hrsa.gov/ALLVARs_search.asp
US Preventive Services Task Force. (2009). Screening for breast cancer: U.S. preventive services task force recommendation statement. Annals of Internal Medicine, 151(10), 716–26. https://doi.org/10.7326/0003-4819-151-10-200911170-00008.
Yu, X., McBean, A. M., & Virnig, B. A. (2007). Physician visits, patient comorbidities, and mammography use among elderly colorectal cancer survivors. Journal of Cancer Survivorship, 1(4), 275–282.
Yusuf, A. A., Hu, Y., Chandler, D., Crittenden, D. B., & Barron, R. L. (2020). Predictors of imminent risk of fracture in Medicare-enrolled men and women. Archives of osteoporosis, 15(1), 1–9.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
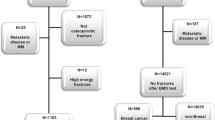
Appendix 1: Flowchart of Sample Selection for Female Medicare Beneficiaries With Diffuse Large B-Cell Lymphoma

Appendix 2: Flowchart of Sample Selection for Female Medicare Beneficiaries With No Cancer

Rights and permissions
About this article
Cite this article
Garg, R., Sambamoorthi, U., Tan, X. et al. Impact of Diffuse Large B-Cell Lymphoma on Mammography and Bone Density Testing in Women. J Primary Prevent 42, 143–162 (2021). https://doi.org/10.1007/s10935-021-00621-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10935-021-00621-8