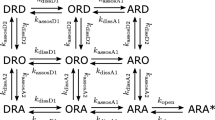
The time course of twitch depression following neuromuscular blocking agent (NMBA) administration is influenced by the duration of control neuromuscular monitoring (twitch stabilization). The physiological mechanism for this interaction is not known. During twitch stabilization twitch response often increases to a plateau, this is known as twitch potentiation or the staircase phenomenon. Since twitch potentiation contributes to the observed twitch response it may also influence the time course of twitch depression following NMBA administration. Our objective was to estimate the degree that twitch potentiation influences the time course of twitch depression following NMBA administration under conditions typical for muscle relaxation studies. We used previousy described pharmacokinetic-pharmacodynamic (PK-PD) and twitch potentiation models to simulate twitch data. Simulations consisted of twitch stabilization followed by a NMBA bolus dose and subsequent onset and recovery from muscle relaxation. Twitch data were analyzed for onset and recovery characteristics and the results compared to clinical muscle relaxation studies in existing literature. We found that twitch potentiation likely plays a minor role in shortened onset time and increased duration of twitch depression observed with long periods of twitch stabilization.
Similar content being viewed by others
References
Donati F. (1988). Onset of action of relaxants. Can. J. Anaesth. 35:S52–S58
Curran M.J., Donati F., Bevan D.R. (1987). Onset and recovery of atracurium and suxamethonium-induced neuromuscular blockade with simultaneous train-of-four and single twitch stimulation. Br. J. Anaesth. 59:989–994
McCoy E.P., Mirakhur R.K., Connolly F.M., Loan P.B. (1995). The influence of the duration of control stimulation on the onset and recovery of neuromuscular block. Anesth. Analg. 80:364–367
Kopman A.F., Kunmar S., Klewicka M.M., Neuman G.G. (2001). The staircase phenomenon. Anesthesiology 95:403–407
Krarup C. (1981). Enhancement and diminution of mechanical tension evoked by staircase and by tetanus in rat muscle. J. Physiol. 311:355–372
Ritchie J.M., Wilkie D.R. (1955). The effect of previous stimulation on the active state of muscle. J. Physiol. 130:488–496
Eleveld D.J., Proost J.H., De Haes A., Wierda J.M.K.H. (2005). Improving pharmacokinetic-pharmacodynamic models of muscle relaxants using potentiation modeling. J. Pharmacokinet. Pharmacodyn. 32:143–154
Eleveld D.J., Kopman A.F., Proost J.H., Wierda J.M.K.H. (2004). Model to describe the degree of twitch potentiation during neuromuscular monitoring. Br. J. Anaesth. 92:373–380
Sheiner L.B., Stanski D.R., Vozeh S., Miller R.D., Ham J. (1979). Simultaneous modeling of pharmacokinetics and pharmacodynamics: application to d-tubocurarine. Clin. Pharmacol. Ther. 25:358–371
Sweeney H.L., Bowman B.F., Stull J.T. (1993). Myosin light chain phosphorylation in vertebrate striated muscle: regulation and function. Am. J. Physiol. Cell. Physiol. 264:C1085–C1095
Klug G.A., Botterman B.R., Stull J.T. (1982). The effect of low frequency stimulation on myosin light chain phosphorylation in skeletal muscle. J. Biol. Chem. 257:4688–4690
S. Beal and L. Sheiner. NONMEM User’s Guide I: Users Basic Guide, Division of clinical Pharmacology, University of California, San Francisco (CA), (1989).
Sheiner L. (1984). The population approach to pharmacokinetic data analysis: rationale and standard data analysis methods. Drug. Metab. Rev. 15:153–171
Beal S. (1984). Population pharmacokinetic data and parameter estimation based on their first two statistical moments. Drug. Metab. Rev. 15:173–193
De Haes A., Proost J.H., Kuks J.B.M., Van den Tol D.C., Wierda J.M.K.H. (2002). Pharmacokinetic-pharmacodynamic modeling of rocuronium in myasthenic patients is improved by taking into account the number of unbound acetylcholine receptors. Anest. Analg. 95:588–596
Viby-Mogensen J., Engbaek J., Eriksson L.I., Gramstad L., Jensen E., Jensen F.S., Koscielniak-Nielsen Z., Skovgaard L.T., Ostergaard D. (1996). Good clinical research practice (GCRP) in pharmacodynamic studies of neuromuscular blocking agents. Acta. Anaesth. Scand. 40:59–74
Girling K.J., Mahajan R.P. (1996). The effect of stabilization on the onset of neuromuscular block when assessed using accelerometry. Anesth. Analg. 82:1257–1260
Rédai I., England A.J., Feldman S.A. (1995). Time taken for stabilization of muscle twitch does not necessarily affect onset and offset times of atracurium. Br. J. Anaesth. 74: 474P
Lee G.C., Iyengar S., Szenohradszky J., Caldwell J.E., Wright P.M., Brown R., Lau M., Luks A., Fisher D.M. (1997). Improving the design of muscle relaxant studies. Stabilization period and tetanic recruitment. Anesthesiology 86:48–54
van Santen G., Fidler V., Wierda J.M.K.H. (1998). Stabilization and stability of twitch force during mechanomyography of the adductor pollicis muscle. J. Clin. Monit. Comput. 14:457–463
Mentre F., Gomeni R. (1995). A two-step iterative algorithm for estimation in nonlinear mixed-effect models with an evaluation in population pharmacokinetics. J. Biopharm. Stat. 5:141–158
Bennett J.E., Wakefield J.C. (1996). A comparison of Bayesian population method with two methods as implemented in commercially available software. J. Pharmacokinet. 24:403–432
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Eleveld, D.J., Proost, J.H. & Wierda, J.M.K.H. Twitch Potentiation Influences the Time Course of Twitch Depression in Muscle Relaxant Studies: A Pharmacokinetic-Pharmacodynamic Explanation. J Pharmacokinet Pharmacodyn 33, 795–806 (2006). https://doi.org/10.1007/s10928-006-9034-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10928-006-9034-0