Abstract
Introduction
Every year many workers are excluded from work because of a work disability attributable to a musculoskeletal disorder (MSD). Factors associated with the development and persistence of the work disability can be related to the worker, work environment, compensation policies, healthcare system and insurance system. Workers’ understanding/representations of their disability are associated with coping behaviors aimed at helping them adapt to or solve their health problem. A representation is a complex, organized entity incorporating thoughts, beliefs, and attitudes regarding a particular subject. Representations have been studied in anthropology, sociology and psychology since the 1960s, but often in a compartmentalized way. These representations provide an important key to understanding what motivates workers during rehabilitation and the return-to-work process. To build upon disciplinary knowledge and better understand workers’ efforts to cope with their persistent disability, this article therefore aims to pool the different knowledge available on the illness representation concept, from the fields of anthropology, sociology and psychology in order to gain a better understanding of its application in the MSD context.
Methods
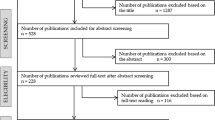
An electronic literature search (French, English) from 1960 on was conducted in medical, paramedical and social science databases (MedLINE, PsychINFO, CINAHL, etc.) using predetermined key words. After screening abstracts based on a set of criteria, content analysis was performed on the 131 articles retained. Results: The theoretical models and approaches can be divided into three categories: (1) personal experience; (2) interactionist; and (3) sociocultural. The models found in sociology and anthropology are mainly descriptive and developed in a medical context, and only rarely in an occupational health context. However, these models could add elements to psychosocial models that are more dynamic and oriented toward understanding the reasons behind specific behaviors.
Conclusion
Bridging the gap between these disciplines will help us achieve a new level of knowledge that will, by taking social interactions into account, enhance understanding of workers’ representations, and the behaviors they adopt to manage their MSD-related disability.

Similar content being viewed by others
References
Baril, R., Martin, J. C., Lapointe, C., & Massicotte, P. (1994). Etude exploratoire des processus de réinsertion sociale et professsionnelle des travailleurs en réadaptation. Montréal, Québec (Canada): Institut de recherche Robert-Sauvé en santé et en sécurité du travail.
Frank, J. W., Brooker, A., DeMaio, S. E., Kerr, M. S., Maetzel, A., Shannon, H. S. et al. (1996). Disability resulting from occupational low back pain. Part II: What do we know about secondary prevention? A review of the scientific evidence on prevention after disability begins. Spine, 21(24), 2918–2929.
Gallagher, R. M., Williams, R. A., Skelly, J., Haugh, L. D., Rauh, V., Milhous, R. et al (1995). Workers’ Compensation and return-to-work in low back pain. Pain, 61(2), 299–307.
Truchon, M., & Fillion, L. (2000). Biopsychosocial determinants of chronic disability and low-back pain: a review. Journal of Occupational Rehabilitation, 10(2), 117–142.
Turk, D. C., & Okifuji, A. (1996). Perception of traumatic onset, compensation status, and physical findings: impact on pain severity, emotional distress, and disability in chronic pain patients. Journal of Behavioral Medicine, 19(5), 435–453.
Michie, S. A., & Abraham, C. B. (2004). Interventions to change health behaviours: evidence-based or evidence-inspired? Psychology & Health, 19(1), 29–49.
Moss-Morris, R., Petrie, K. J., & Weinman, J. (1996). Functioning in chronic fatigue syndrome – do illness perceptions play a regulatory role. British Journal of Health Psychology, 1(Part 1), 15–25.
Smith, T. W., Christensen, A. J., Peck, J. R., & Ward, J. R. (1994). Cognitive distortion, helplessness, and depressed mood in rheumatoid arthritis: a four-year longitudinal analysis. Health Psychology, 13(3), 213–217.
van der Hulst, M., Vollenbroek-Hutten, M. M., & Ijzerman, M. J. (2005). A systematic review of sociodemographic, physical, and psychological predictors of multidisciplinary rehabilitation-or, back school treatment outcome in patients with chronic low back pain. Spine, 30(7), 813–825.
Kaplan, R. M., Sallis, J. F., & Patterson, T. L. (1993). Health and human behavior. New York: McGraw-Hill.
Jensen, M. P., & Karoly, P. (1991). Control beliefs, coping efforts, and adjustment to chronic pain. Journal of Consulting and Clinical Psychology, 59(3), 431–438.
Johnson, L. M., Zautra, A. J., & Davis, M. C. (2006). The role of illness uncertainty on coping with fibromyalgia symptoms. Health Psychology, 25(6), 696–703.
Abric, J.-C. (2003). La recherche du noyau central et de la zone muette des représentations sociales. In J.-C. Abric (Eds.), Méthodes d’étude des représentations sociales (pp. 59–80). Ramonville Saint-Agne: Eres.
Jodelet, D. (1989). Les représentations sociales. Paris (France): Presses universitaires de France.
Massé, R. (1995). Culture et santé publique. Boucherville, Québec (Canada): Gaëtan Morin.
Larousse (Ed.). (1999). Grand dictionnaire de la psychologie (p. 1062). Paris (France).
Toombs, S. K. (1987). The meaning of illness: A phenomenological approach to the patient-physician relationship. Journal of Medicine and Philosophy, 12(3), 219–240.
Turk, D. C., & Okifuji, A. (2002). Psychological factors in chronic pain: evolution and revolution. Journal of Consulting & Clinical Psychology, 70(3), 678–690.
Landry, R. (1997). L’analyse de contenu. In B. Gauthier (Ed.), Recherche sociale de la problématique à la collecte de données (pp. 329–356). Québec, Québec (Canada): Presses de l’Université du Québec.
Vlaeyen, J. W. S., Kole-Snijders, A. M., Boeren, R. G., & van Eek, H. (1995). Fear of movement/(re)injury in chronic low back pain and its relation to behavioral performance. Pain, 62(3Using Smart Source Parsing Sep), 363–372.
Prochaska, J. O., Norcross, J. C., & Di Clemente, C. C. (1994). Changing for good: a revolutionary six-stage program for overcoming bad habits and moving your life positively forward. New York: L. W. Morrow and Company Inc.
Leventhal, H., Brissette, I., & Leventhal, E. A. (2003). The common-sense model of self-regulation of health and illness. In L. D. Cameron & H. Leventhal (Eds.), The self-regulation of health and illness behaviour (pp. 42–65). London(England): Routledge.
Leventhal, H., Meyer, D., Nerenz, D., & Rachman, S. (1980). The common sense representation of illness danger. In Anonymous, editor. Contributions to Medical Psychology (pp. 7–30). Oxford (England): Pergamon Press.
Kelly, G. A. (1955). The psychology of personal constructs, 2 volumes. New York: Norton.
Bury, M. (1982). Chronic illness as biographical disruption. Sociology of Health and Illness, 4, 167–182.
Corbin, J. M., & Strauss, A. (1992). A nursing model for chronic illness management based upon the trajectory framework. In P. Woog (Ed.), The chronic illness trajectory framework (pp. 9–28). New York: Springer.
Kori, S. H., Miller, R. P., & Todd, D. D. (1990). Kinesiophobia: A new view of chronic pain behavior. Pain Manage, 3, 35–43.
Lethem, J., Slade, P. D., Troup, J. D., & Bentley, G. (1983). Outline of a Fear-Avoidance Model of exaggerated pain perception–I. Behaviour Research & Therapy, 21(4), 401–408.
Vlaeyen, J. W., & Linton, S. J. (2000). Fear-avoidance and its consequences in chronic musculoskeletal pain: a state of the art. Pain, 85(3), 317–332.
Waddell, G., & Burton, A. K. (2005). Concepts of rehabilitation for the management of low back pain. Best Practice & Research in Clinical Rheumatology, 19(4), 655–670.
Sullivan, M. J. L., Bishop, S. R., & Pivik, J. (1995). The Pain Catastrophizing Scale-Development and Validation. Psychological Assessment, 7(4), 524–532.
Goubert, L., Crombez, G., & De Bourdeaudhuij, I. (2004). Low back pain, disability and back pain myths in a community sample: Prevalence and interrelationships. European Journal of Pain, 8(4), 385–394.
Vowles, K. E., & Gross, R. T. (2003). Work-related beliefs about injury and physical capability for work in individuals with chronic pain. Pain, 101(3), 291–298.
Walsh, D. A., & Radcliffe, J. C. (2002). Pain beliefs and perceived physical disability of patients with chronic low back pain. Pain, 97(1–2), 23–31.
Fritz, J. M., George, S. Z., & Delitto, A. (2001). The role of fear-avoidance beliefs in acute low back pain: Relationships with current and future disability and work status. Pain, 94(1), 7–15.
Jensen, M. P., & Karoly, P. (1992). Pain-specific beliefs, perceived symptom severity, and adjustement to chronic pain. Clinical Journal of Pain, 8(2), 123–130.
Jensen, M. P., Romano, J. M., Turner, J. A., Good, A. B., & Wald, L. H. (1999). Patient beliefs predict patient functioning: Further support for a cognitive-behavioural model of chronic pain. Pain, 81(1–2), 95–104.
Keen, S., Dowell, A. C., Hurst, K., Klaber Moffett, J. A., Tovey, P., & Williams, R. (1999). Individuals with low back pain: how do they view physical activity? Family practice, 16(1), 39–45.
Knish, S., & Calder, P. (1999). Beliefs of chronic low back pain sufferers: A concept map. Canadian Journal of Rehabilitation, 12(3), 167–179.
Werner, E. L., Ihlebaek, C., Skouen, J. S., & Laerum, E. (2005). Beliefs about low back pain in the norwegian general population: are they related to pain experiences and health professionals. Spine, 30(15), 1770–1776.
Woby, S. R., Watson, P. J., Roach, N. K., & Urmston, M. (2004). Adjustment to chronic low back pain: the relative influence of fear-avoidance beliefs, catastrophizing, and appraisals of control. Behaviour research and therapy, 42(7), 761–774.
Cleary, L., Thombs, D. L., Daniel, E. L., & Zimmerli, W. H. (1995). Occupational low back disability: effective strategies for reducing lost work time. AAOHN Journal, 43(2), 87–94.
van der Giezen, A. M., Bouter, L. M., & Nijhuis, F. J. (2000). Prediction of return-to-work of low back pain patients sicklisted for 3–4 months. Pain, 87(3), 285–294.
Crook, J., Moldofsky, H., & Shannon, H. (1998). Determinants of disability after a work related musculetal injury. Journal of Rheumatology, 25(8), 1570–1577.
Hazard, R. G. (1996). Chronic low back pain and disability: the efficacy of functional restoration. Bulletin Hospital for Joint Diseases, 55(4), 213–216.
van der Weide, W. E., Verbeek, J. H., Salle, H. J., & van Dijk, F. J. (1999). Prognostic factors for chronic disability from acute low-back pain in occupational health care. Scandinavian Journal of Work, Environment & Health, 25(1), 50–56.
Prochaska, J. O., DiClemente, C. C., & Norcross, J. C. (1992). In Search of How People Change. American Psychologist, 47(9), 1102–1114.
Prochaska, J. O., & Norcross, J. C. (2001). Stages of Change. Psychotherapy, 38(4), 443–448.
Coutu, M. F., Dupuis, G., Marchand, A., O’Connor K, Trudel, G., & Bouthillier D (2000). Adoption et maintien des habitudes comportementales saines: recension des modèles explicatifs. Revue Francophone de Clinique Comportementale Cognitive, 5(2), 23–35.
Gibertini, M., DiClemente, C. C., Prochaska, J. O. (1985). Self-efficacy and the stages of self-change of smoking.
Bandura, A. (1977). Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review, 84, 191–215.
Bandura, A. (1997). Self-efficacy: the exercise of control. New York: W. H. Freeman.
Kaplan, R. M., & Simon, H. J. (1990). Compliance in medical care: reconsideration of self-prediction. Annals of Behavioral Medicine, 12, 66–71.
Dionne, C., Bourbonnais, R., Fémont P, Rossignol, M., & Stock, S. (2004). Le pronostic occupationnel des travailleurs aux prises avec des affections vertébrales. Montréal (Québec, Canada): Institut de recherche Robert-Sauvé en santé et sécurité au travail (IRSST).
Dijkstra, A. (2005). The validity of the stages of change model in the adoption of the self-management approach in chronic pain. Clinical Journal of Pain, 21(1), 27–37.
Jensen, M. P., Nielson, W. R., & Kerns, R. D. (2003). Toward the development of a motivational model of pain self-management. Journal of Pain, 4(9), 477–492.
Jensen, M. P., Nielson, W. R., Turner, J. A., Romano, J. M., & Hill, M. L. (2004). Changes in readiness to self-manage pain are associated with improvement in multidisciplinary pain treatment and pain coping. Pain, 111(1–2), 84–95.
Keller, S., Herda, C., Ridder, K., & Basler, H. D. (2001). Readiness to adopt adequate postural habits: an application of the Transtheoretical Model in the context of back pain prevention. Patient Education & Counseling, 42(2), 175–184.
Franche, R. L., & Krause, N. (2002). Readiness for return to work following injury or illness: conceptualizing the interpersonal impact of health care, workplace, and insurance factors. Journal of Occupational Rehabilitation, 12(4), 233–256.
Krause, N., & Ragland, D. R. (1994). Occupational disability due to low back pain: a new interdisciplinary classification based on a phase model of disability. Spine, 19(9), 1011–1020.
de Ridder, D. T. D., de Wit, J. B. F., de Ridder, D. T. D., & de Wit J. B. F. (2006). Self-regulation in health behavior: Concepts, theories, and central issues. In Anonymous (Ed.), Self-regulation in Health Behavior (pp. 1–23). New York: John Wiley and Sons Ltd.
Flick, U. (1993). La perception quotidienne de la santé et de la maladie. Aperçu général et introduction. In U. Flick (Ed.), La perception quotidienne de la santé et de la maladie Théories subjectives et représentations sociales (pp. 11–71). Paris (France): L’Harmattan.
Furnham, A. (1994). Explaining health and illness: lay beliefs on the nature of health. Personality and individual differences, 17(4), 455–466.
Lawton, J. (2003). Lay experiences of health and illness: past research and future agendas. Sociology of Health and Illness, 25(NS), 23–40.
Leventhal, H., Benyamini, Y., Brownlee, S., Diefenbach, M., Leventhal, E. A., Patrick-Miller, L., et al. (1997). Illness Representations: Theoretical Foundations. In K. Petrie & J. A. Weinman (Eds.), Perception of health and illness (pp. 19–45). Amsterdam (Netherland): Harewood Academic Publishers.
Murray, M., Bennett, P., & Weinman, J. (1990). Lay representations of illness. In Anonymous (Ed.), Current developments in health psychology (pp. 63–92). London: Harwood academic publishers.
Lackner, J. M., Carosella, A. M., & Feuerstein, M. (1996). Pain expectacies, pain, and functional self-efficacy expectancies as determinants of disability in patients with chronic low back disorders. Journal of Consulting and Clinical Psychology, 64(1), 212–220.
Charmaz, K. (1983). Loss of self : a fundamental form of suffering in the chronically ill. Sociology of Health and Illness, 5, 168–195.
Good, M. J., Brodwin, P., Good, B., & Kleinman, A. (1992). Pain as Human experience: An anthropological perspective. Berkeley, California: University of California Press.
Kleinman, A. (1988). The illness narratives: Suffering, healing and the human condition. New York: Basic Books.
Williams, G. (1984). The genesis of chronic illness : narrative reconstruction. Sociology of Health and Illness, 6, 175–200.
Horne, R., Weinman, J., Myers, L. B., & Midence, K. (1998). Predicting treatment adherence: An overview of theoretical models. In Anonymous (Ed.), Adherence to treatment in medical conditions (pp. 25–50). Amsterdam (Netherland): Harwood Academic.
Young, J. T. (2004). Illness behaviour: a selective review and synthesis. Sociology of Health & Illness, 26(1), 1–31.
Schiaffino K. M., Shawaryn M. A., & Blum, D. (1998). Examining the Impact of Illness Representations on Psychological Adjustment to Chronic Illness. Health Psychology, 17(3), 262–268.
Leventhal, H., Zimmerman, R., & Gutmann, M. (1984). Compliance: A self-regulation perspective. In W. D. Gentry (Ed.), Handbook of behavioral medicine (pp. 369–436). New York: Guilford Press.
Croyle, R. T., & Jemmott I. J. B. (1991). Psychological reaction to risk factor testing. In J. A. Skelton & R. T. Croyle (Eds.), Mental representation in health and illness (pp. 85–107). New York: Spring-Verlag.
Leventhal, H., Diefenbach, M., & Leventhal, E. A. (1992). Illness cognition: Using common sense to understand treatment adherence and affect cognition interactions. Therapy and Research, 16, 143–163.
Bandura, A. (1977). A social learning theory. Englewood Cliffs, New Jersey: Prentice-Hall.
Leventhal, H., & Diefenbach, M. (1991). The active side of illness cognition. In J. A. Skelton & R. T. Croyle (Eds.), Mental representation in health and illness (pp. 247–272). New York: Springer-Verlag.
Kleinman, A. (1980). Patients and healers in the context of culture: An exploration of the borderland between anthropology, medicine, and psychiatry. Berkeley (California): University of California Press.
Kleinman, A., & Seeman, D. (2000). Personal experience of illness. In G. L. Albrecht, Fitzpatrick R & S. C. Scrimshaw (Eds.), The handbook of social studies in health and medicine (pp. 230–42). London (England): Sage.
Leventhal, H., Nerenz, D., Straus, A., & Mechanic, D. (1982). Self-regulation and the mechanisms for symptom appraisal. In Anonymous (Ed.), Symptoms, illness behavior, and the help-seeking monographs in psychosocial epidemiology (pp. 55–86). New York: Neal Watson Academic.
Buick, D. L., Petrie, K. J., & Weinman, J. A. (1997). Illness representations and breast cancer: Coping with radiation and chemotherapy. In Anonymous (Ed.), Perceptions of health and illness: Current research and applications (pp. 379–409). Amsterdam (Netherland): Harwood Academic Publishers.
Heijmans, M. (1999). The role of patients’ illness representations in coping and functioning with Addison’s disease. British Journal of Health Psychology, 4(2), 137–49.
Petrie, K., Moss-Morris, R., & Weinman, J. (1995). The impact of catastrophic beliefs on functioning in chronic fatigue syndrome. Journal of Psychosomatic Research, 39(1), 31–37.
Petrie, K. J., Weinman, J., Sharpe, N., & Buckley, J. (1996) Role of patients’ view of their illness in predicting return to work and functioning after myocardial infarction: longitudinal study. British Medical Journal, 312, 1191–1194.
Scharloo, M., & Kaptein, A. (1997). Measurement of illness perceptions in patients with chronic somatic illness: A review. In K. J. Petrie & J. A. Weinman (Eds.), Perceptions of health and illness (pp. 103–54). Amsterdam: Harwood Academic.
Blowers, G. H., & O’Connor, K. P. (1996). Les construits personnels. De la théorie à l’application clinique. Montréal, Québec (Canada): Presses de l’Université de Montréal.
O’Connor, K. P., Gareau, D., & Blowers, G. H. (1994). Personal constructs associated with tics. British Journal of Clinical Psychology, 33, 151–158.
Berger, P. L., & Berger, B. (1972). Sociology: a biographical approach. New York: Basic Books.
Goffman, E. (1974). Frame analysis: an essay on the organization of experience. New York: Harper & Row.
Strauss, A. L., & Glaser, B. G. (1970). Anguish; a case history of a dying trajectory. Mill Valley, California: Sociology Press.
Berger, P. L., & Luckmann, T. (1966). The social construction of reality : a treatise in the sociology of knowledge. Garden City, NY: Doubleday.
Schütz, A. (1967). The phenomenology of the social world Alfred Schutz. Evanston, IL: North-western University Press.
Twaddle, A. (1980). Sickness and the sickness career: Some implications. In L. Eisenberg & A. Kleinman (Eds.), The Relevance of social science for medicine (pp. 111–33). Dordrecht (Netherland): D. Reidel Pub.
Herzlich, C. (1984). Médecine moderne et quête de sens: la maladie signifiant social. In M. Augé & C. Herzlich (Eds.), Le sens du mal Anthropologie, histoire, sociologie de la maladie (pp. 189–215). Paris (France): Éditions des archives contemporaines.
Charmaz, K. (1994). Discoveries of self in illness. In M. L. Dietz, R. Prus & W. Shaffir (Eds.), Doing everyday life Ethnography as human lived experience (pp. 226–42). Mississauga, Ontario (Canada): Copp Clark Longman.
Bury, M. (2001). Illness narratives: fact or fiction? Sociology of health & illness, 23(3), 263–285.
Beaton, D. E., Tarasuk, J. N., Katz, J. N., Wright, J. G., & Bombardier, C. (2001). “Are You Better?” A Qualitative Study of the Meaning of Recovery. Arthritis Care and Research, 45, 270–279.
Garro, L. C. (1994). Narrative representations of chronic illness experience: Cultural models of illness, mind, and body in stories concerning the temporomandibular joint (TMJ). Social Science & Medicine, 38(6), 775–788.
Shaw, L., Segal, R., Polatajko, H., & Harburn, K. (2002). Understanding return to work behaviours: promoting the importance of individual perceptions in the study of return to work. Disability & Rehabilitation, 24(4), 185–195.
Söderberg S, Jumisko, E., & Gard, G. (2004). Clients’ experiences of a work rehabilitation process. Disability & Rehabilitation, 26(7), 419–424.
Walker, J., Holloway, I., & Sofaer, B. (1999). In the system: The lived experience of chronic back pain from the perspectives of those seeking help from pain clinics. Pain, 80(3), 621–628.
Brown, C. A. (2004). The beliefs of people with chronic pain in relation to “important” treatment components. European Journal of Pain, 8(4), 325–333.
Cameron, L. D., Booth, R. J., Schlatter, M., Ziginskas, D., Harman, J. E., & Benson, S. R. (2005). Cognitive and affective determinants of decisions to attend a group psychosocial support program for women with breast cancer. Psychosomatic Medicine, 67(4), 584–589.
Fortune, G., Barrowclough, C., & Lobban, F. (2004). Illness representations in depression. British Journal of Clinical Psychology, 43(4), 347–364.
Leventhal, P. A. M., Robitaille, C., Leventhal, H., Swigar, M., Leventhal, E. A. (2002). Trait negative affect relates to prior-week symptoms, but not to reports of illness episodes, illness symptoms, and care seeking among older persons. Psychosomatic Medicine, 436–449.
van Mens-Verhulst, J., van Dijkum, C., van Kuijk, E., & Lam, N. (2003). The self-regulation of fatigue and associated complaints: An exploratory simulation. Patient Education and Counseling, 49(1), 53–57.
Walsh, J. C., Lynch, M., Murphy, A. W., & Daly, K. (2004). Factors influencing the decision to seek treatment for symptoms of acute myocardial infarction: An evaluation of the Self-Regulatory Model of illness behaviour. Journal of Psychosomatic Research, 56(1), 67–73.
Coulon, A. (2002). L’ethnométhodologie. Paris (France): Presses Universitaires de France.
Le Breton, D. (2004). L’interactionnisme symbolique. 1re éd. ed. Paris (France): Presses universitaires de France.
Parsons, T. (1951). The social systems. Glencoe, Illinois: Free Press.
Mucchielli, A. (1999). La théorie systémique des communications. Paris (France): Armand Colin.
Glenton, C. (2003). Chronic back pain sufferers–striving for the sick role. Social science & medicine, 57(11), 2243–2252.
Bourdieu, P. (1994). Raisons pratiques. Sur la théorie de l’action. Paris (France): Seuil.
Ewan, C., Lowy, E., & Reid, J. (1991). ‘Falling out of culture’: The effects of repetition strain injury on sufferers’roles and identity. Sociology of health & illness, 13(2), 168–192.
Goffman, E. (1963). Stigma; notes on the management of spoiled identity. Englewood Cliffs, New Jersey: Prentice-Hall.
Blumer, H. (1969). Symbolic interactionism. Perspective and method. Englewood Cliffs, New Jersey: Prentice-Hall.
Bendelow, G. A., & Williams, S. J. (1996). The end of the road? Lay views on a pain-relief clinic. Social Science & Medicine, 43(7), 1127–1136.
Hilbert, R. A. (1984). The acultural dimensions of chronic pain: flawed reality construction and the problem of meaning. Social Problems, 31(4), 365–378.
Osborn, M., & Smith, J. A. (1998). The personal experience of chronic lower back pain: an interpretative phenomenological analysis. British Journal of Health Psychology, 3(1), 65–83.
Edwards, P. W., O’Neill, G. W., & Zeichner, A. (1985). Effects of familial pain models on pain complaints and coping strategies. Perceptual and Motor Skills, 61, 1053–1054.
Reid, J., Ewan, C., & Lowy, E. (1991). Pilgrimage of pain: The illness experiences of women with repetition strain injury and the search for credibility. Social Science & Medicine, 32(5), 601–612.
Szasz, T. S., & Hollender, M. (1956). A Contribution to the Philosophy of Medicine: the Basic Models of the Doctor-Patient Relationship. Journal of the Amercian Medical Association, 97, 585–588.
Veatch, R. M. (1972). Models for ethical medicine in a revolutionary age. What physician-patient roles foster the most ethical realtionship? Hastings Center Report, 2(3), 5–7.
Liu, K. P., Chan, C. C., & Chan, F. (2005). Would discussion on patients’needs add value to the rehabilitation process? International Journal of Rehabilitation Research, 28(1), 1–7.
Golin, C. E., DiMatteo, M. R., & Gelberg, L. (1996). The role of patient participation in the doctor visit. Implications for adherence to diabetes care. Diabetes care, 19(10), 1153–1164.
Heisler, M., Vijan, S., Anderson, R. M., Ubel, P. A., Bernstein, S. J., & Hofer, T. P. (2003). When do patients and their physicians agree on diabetes treatment goals and strategies, and what difference does it make? Journal of General Internal Medicine November, 18(11), 893–902.
Brown, C. A. (2003). Service users’ and occupational therapists’ beliefs about effective treatments for chronic pain: A meeting of the minds or the great divide? Disability & Rehabilitation: An International Multidisciplinary Journal, 25(19), 1115–1125.
Cook, F. M., & Hassenkamp, A. M. (2000). Active rehabilitation for chronic low back pain. Physiotherapy, 86, 61–68.
Dean, S. G., Smith, J. A., Payne, S., & Weinman, J. (2005). Managing time: An interpretative phenomenological analysis of patients’ and physiotherapists’ perception of adherence to therapeutic exercise for low back pain. Disability & Rehabilitation, 27(11), 625–636.
Gustafsson, M., Ekholm, J., & Ohman, A. (2004). From Shame to Respect: Musculoskeletal Pain Patients’ Experience of a Rehabilitation Programme. A Qualitative Study. Journal of Rehabilitation Medicine, 36, 97–103.
Ong, B. N., Hooper, H., & Dunn, K. (2004). Establishing self and meaning in low back pain narratives. The Sociological Review, 52(4), 532–549.
Perreault, K., & Dionne, C. (2005). Patient-Physiotherapist Agreement in Low Back Pain. The Journal of Pain, 6(12), 817–828.
Skelton, A. M., Murphy, E. A., Murphy, R. J., & O’Dowd, T. C. (1995). General practitioner perceptions of low back pain patients. Family practice, 12(1), 44–48.
Skelton, A. M., Murphy, E. A., Murphy, R. J., & O’Dowd, T. C. (1996). Patients’ views of low back pain and its management in general practice. British Journal of General Practice, 46(404), 153–156.
Thunberg, K. A., Carlsson, S. G., & Hallberg, L. R. M. (2001). Health care professionals’ understanding of chronic pain: A grounded theory study. Scandinavian Journal of Caring Sciences, 15(1), 99–105.
Dekkers, W. (1998). Hermeneutics and experiences of the body. The case of low back pain. Theoretical Medicine and Bioethics, 19, 277–293.
Leder, D. (1990). Clinical interpretation: the hermeneutics of medicine. Theoretical Medicine, 11(1), 9–24.
Hamberg, K., Johansson, E., Lingren, G., & Westman, G. (1997). The impact of marital relationship on the rehabilitation process in a group of women with long-term musculoskeletal disorders. Scandinavian Journal of Social Medicine, 25(1), 17–25.
Johansson, E. E., Hamberg, K., Westman, G., & Lindgren, G. (1999).The meanings of pain: an exploration of women’s description of symptoms. Social science & medicine, 48, 1791–1802.
Ostlund, G., Cedersund, E., Hensing, G., & Alexanderson, K. (2004). Domestic strain: a hindrance in rehabilitation? Scandinavian Journal of Caring Sciences, 18(1), 49–56.
McElroy, A., Jezewski, M. A., Albrecht, G. L. Ed., Fitzpatrick R. Cultural variation in the experience of health and illness. In Anonymous (Ed.), The handbook of social studies in health and medicine (pp. 191–209). London (England): Sage.
IRSC. Analyse des différences de genre et des différences de sexe dans les recherches en santé – Guide pour les comités d’examen par les pairs des IRSC. 2007 [cited 20-04-2007]; Available from:
Pierret, J. (2003). The illness experience: state of knowledge and perspectives for research. Sociology of Health and Illness, 25, 4–22.
Zborowski, M. (1952). Cultural component in responses to pain. Journal of Social Issues, 8, 16–30.
Zborowski, M. (1969). People in pain. San Francisco, California: Jossey-Bass.
Zola, I. K. (1966). Culture and symptoms: An analysis of patients’ presenting complaints. American Sociological Review, 31(5), 615–630.
Twaddle, A. C. (1969). Health decisions and sick role variations: an exploration. Journal of Health & Social Behavior, 10(2), 105–115.
Bates, M. S., & Edwards, W. T. (1992). Ethnic variations in the chronic pain experience. Ethnicity & Disease, 2(1), 63–83.
Bates, M. S., Rankin-Hill, L., & Sanchez-Ayendez, M. (1997). The effects of the cultural context of health care on treatment of and response to chronic pain and illness. Social science & medicine, 45(9), 1433–1447.
Sargent, C. (1984). Between death and shame: dimensions of pain in Bariba culture. Social science & medicine, 19(12), 1299–304.
Bibeau, G., & Pelletier, L. (1985). Le discours sur la santé et la maladie dans deux populations de la ville de Québec. Ottawa: Musées nationaux du Canada.
Corin, E., Bibeau, G., Martin, J. C., & Laplante, R. (1990). Comprendre pour agir autrement: repères pour régionaliser les services de santé mentale. Montréal, Québec (Canada): Presses de l’Université de Montréal.
Hansson, M., Bostrom, C., & Harms-Ringdahl, K. (2001). Living with spine-related pain in a changing society–a qualitative study. Disability & Rehabilitation, 23(7), 286–295.
Sommer, H. M. (1998). The patient in Jeopardy: How the low back pain patient becomes disabled. Occupational Medicine: State of the Art Reviews, 13(1), 23–31.
Cheng, Y. H. (1997). Explaining disablement in modern times: hand-injured workers’ accounts of their injuries in Hong Kong. Social Science & Medicine, 45(5), 739–750.
Lippell, K. (1999). Therapeutic and anti-therapeutic consequences of workers’ compensation. International journal of law and psychiatry, 22(5–6), 521–546.
Watson, P. J., Booker, C. K., Moores, L., & Main, C. J. (2004). Returning the chronically unemployed with low back pain to employment. European Journal of Pain, 8(4), 359–369.
Baril, R., Berthelette, D., & Massicotte, P. (2003). Early return to work of injured workers: Multidimensional patterns of individual and organizational factors. Safety Science, 41, 277–300.
Baril, R., Berthelette, D., Ross, C., Gourde, D., Massicotte, P., & Pajot, A. (2000). Les composantes et les déterminants organisationnels des interventions de maintien du lien d’emploi. Montréal: Institut de recherche Robert-Sauvé en santé et en sécurité du travail.
Frank, J., Sinclair, S., Hoggjohnson, S., Shannon, H., Bombardier, C., Beaton, D. et al. (1998). Preventing disability from work-related low-back pain – new evidence gives new hope – if we can just get all the players onside. Canadian Medical Association Journal, 158(12), 1625–1631.
Loisel, P., Abenhaim, L., Durand, P., Esdaile, J. M., Suissa, S., Gosselin, L. et al. (1997). A population-based, randomized clinical trial on back pain management. Spine, 22(24), 2911–2918.
Loisel, P., Durand M-J, Berthelette, D., Vézina N, Baril, R., Gagnon, D. et al (2001). Disability prevention: the new paradigm of management of occupational back pain. Disease Management & Health Outcomes, 9(7), 351–360.
Daykin, A. R. P. M., & Richardson, B. P. M. (2004). Physiotherapists’ pain beliefs and their influence on the management of patients with chronic low back pain. Spine April 1, 29(7), 783–795.
Kleinman, A., Brodwin, P. E., Good, B. J., & DelVecchio-Good, M. J., (Eds.). (1992). Pain as Human Experience. An Introduction. Berkeley, California: University of California Press.
Acknowledgements
This study was supported by a grant from the Institut de recherche Robert-Sauvé en santé et en sécurité au travail (IRSST). We also wish to thank the IRSST for providing support for the bibliographical literature search. In addition, we are grateful to Mr. Jacques Blain, who provided us with his expertise in bibliographical databases.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Coutu, MF., Baril, R., Durand, MJ. et al. Representations: An Important Key to Understanding Workers’ Coping Behaviors During Rehabilitation and the Return-to-Work Process. J Occup Rehabil 17, 522–544 (2007). https://doi.org/10.1007/s10926-007-9089-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10926-007-9089-9