Abstract
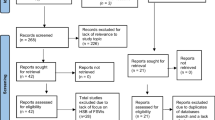
South Asian communities comprise one of the fastest growing populations in Western countries. However, the sexual health of immigrant men in particular remains vastly understudied and little is known about how and if men access these services. Four multi-disciplinary electronic databases were searched to between 1998 and 2018. The search yielded 586 articles; 407 duplicate articles were removed, and 376 did not meet the inclusion criteria. A total of 10 articles were included in this review. Herein we report the factors shaping sexual health service access and use, namely: (1) cultural and psychological factors; (2) sexual health service accessibility; (3) personal beliefs and patterns in service use; (4) social perspectives and conflicting values on sexual health. We identify the gaps in research needed for policymakers, formal healthcare providers, and South Asian community stakeholders to develop effective and inclusive sexual health programs for South Asian men in Western countries.

Similar content being viewed by others
References
Nilaweera I, Doran F, Fisher J. Prevalence, nature and determinants of postpartum mental health problems among women who have migrated from South Asian to high-income countries: a systematic review of the evidence. J Affect Disord. 2014;166:213–26. https://doi.org/10.1016/j.jad.2014.05.021.
Islam F, Khanlou N, Tamim H. South Asian populations in Canada: Migration and mental health. BMC Psychiatry. 2014;14(1):1–13. https://doi.org/10.1186/1471-244X-14-154.
United Nations Population Fund. Migration. 2015. https://www.unfpa.org/migration. Accessed 10 Apr 2018.
Statistics Canada. Immigration and ethnocultural diversity in Canada. National Household Survey, 2011. National Household Survey, 2011 (vol. 99-10-X20). 2013.
Statistics Canada. Canada Yearbook. Ottawa: Statistics Canada; 2011. p. 438–447.
SAALT Demographic Snapshot. (citing United States Census data on Bangladeshi, Indian, Pakistani, and Sri Lankan groups (2000, 2010)). (2012). https://saalt.org/resources/reports-and-publications/#factsheets.
Lebrun LA, Dubay LC. Access to primary and preventive care among foreign-born adults in Canada and the United States. Health Serv Res. 2010;45(6 PART 1):1693–719. https://doi.org/10.1111/j.1475-6773.2010.01163.x.
ABS. Australian Bureau of Statistics web site. 2011. https://www.abs.gov.au/. Accessed 10 Apr 2018.
Vasileva K. 6.5% of the EU population are foreigners and 9.4% are born abroad. Eurostat Stat Focus. 2011;34:1–8. Accessed 8 June 2018.
Davies A, Blake C, Dhavan P. Social determinants and risk factors for non-communicable diseases (NCDs) in south asian migrant populations in Europe. Asia Eur J. 2011;8(4):461–73. https://doi.org/10.1007/s10308-011-0291-1.
Degni F, Suominen S, Essén B, El Ansari W, Vehviläinen-Julkunen K. Communication and cultural issues in providing reproductive health care to immigrant women: Health care providers’ experiences in meeting Somali women living in Finland. J Immigr Minor Health. 2012;14(2):330–43. https://doi.org/10.1007/s10903-011-9465-6.
Doll LS, Beeker C. Male bisexual behavior and HIV risk in the united states: Synthesis of research with implications for behavioral interventions. AIDS Educ Prev. 1996;8(3):205–25.
Leininger MM. Transcultural nursing: concepts, theories, research and practice. Columbus: WCB McGraw-Hill; 1995.
Courtenay WH. Behavioral factors associated with disease, injury, and death among men: evidence and implications for prevention. J Men’s Stud. 2000;9(1):81–142. https://doi.org/10.3149/jms.0901.81.
Courtenay WH. Engendering health: a social constructionist examination of men’s health beliefs and behaviors. Psychol Men Masc. 2000;1(1):4–15. https://doi.org/10.1037//1524-9220.1.1.4.
Weston HJ. Public honour, private shame and HIV: Issues affecting sexual health service delivery in London's south asian communities. Health and Place. 2003;9(2):109–17. https://doi.org/10.1016/S1353-8292(03)00002-9.
Buzi RS, Smith PB. Access to sexual and reproductive health care services: young men's perspectives. J Sex Marital Ther. 2014;40(2):149–57. https://doi.org/10.1080/0092623X.2012.736923.
Hahm HC, Song IH, Ozonoff A, Sassani JC. HIV testing among sexually experienced Asian and pacific islander young women. Association with routine gynecologic care. Women’s Health Issues. 2009;19(4):279–88. https://doi.org/10.1016/j.whi.2009.05.001.
Willcox A, Gleeson J. Boys, young men and teenage pregnancies: Adrienne willcox and judy gleeson explore the issues around educating boys on teenage pregnancy. Prim Health Care. 2003;13:27.
Ottawa Public Health. Sexually transmitted infections and sexual health in Ottawa. Ottawa (ON): Ottawa Public Health; 2011. Accessed 8 June 2018.
Smith AL. Health policy and the coloring of an American male crisis: a perspective on community-based health services. [Reprint in Am J Public Health. 2008 Sep;98(9 Suppl):S158–61; PMID: 18687603]. Am J Public Health. 2003; 93:749–52. https://doi.org/10.2105/AJPH.93.5.749
Jayaraman G, Totten S, Perrin M, Fang L, Remes O. Report on Sexually Transmitted Infections in Canada: 2008. Centre for Communicable Diseases and Infection Control. 2008. https://www.phac-aspc.gc.ca. Accessed 6 June 2018.
Hancock J. Can mainstream services learn from male only sexual health pilot projects? Sex Transm Infect. 2004;80(6):484–7. https://doi.org/10.1136/sti.2004.011304.
Manderson L, Allotey P. Storytelling, marginality, and community in Australia: how immigrants position their difference in health care settings. Med Anthropol. 2003;22(1):1–21. https://doi.org/10.1080/01459740306767.
Aggleton P, Campbell C. Working with young people—towards an agenda for sexual health. Sex Relatsh Ther. 2010;15(3):283–96. https://doi.org/10.1080/14681990050109863.
Zhou YR. ‘Race’ and HIV vulnerability in a transnational context: The case of chinese immigrants to canada. Cult Health Sex. 2017;19(6):695–708. https://doi.org/10.1080/13691058.2016.1192221.
Grewal S, Bottorff J, Hilton B. The influence of family on immigrant south Asian women’s health. J Fam Nurs. 2005;11(3):242–63. https://doi.org/10.1177/1074840705278622.
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32. https://doi.org/10.1080/1364557032000119616.
Levac D, Colquhoun H, O’Brien KK. Scoping studies: advancing the methodology. Implement Sci. 2010;5(1):1–9. https://doi.org/10.1186/1748-5908-5-69.
Al-Taiar A, Clark A, Longenecker JC, Whitty CJM. Physical accessibility and utilization of health services in Yemen. Int J Health Geogr. 2010;9:1–8. https://doi.org/10.1186/1476-072X-9-38.
Goddard M, Smith P. Equity of access to health care services : theory and evidence from the UK. Soc Sci Med. 2001;53(9):1149–62. https://doi.org/10.1016/S0277-9536(00)00415-9.
Cook BL, Doksum T, Chen C, Carle A, Alegría M. The role of provider supply and organization in reducing racial/ethnic disparities in mental health care in the U.S. Soc Sci Med. 2013;84:102–9. https://doi.org/10.1016/j.socscimed.2013.02.006.
Hibbard J. Using systematic measurement to target consumer activation strategies. Med Care Res Rev. 2009;66(1):9S–27S. https://doi.org/10.1177/1077558708326969.
Davidson PL, et al. A framework for evaluating safety-net and other community-level factors on access for low-income populations. Inquiry. 2004;41(1):21–38.
Vlassoff C, Ali F. HIV-related stigma among South Asians in Toronto. Ethn Health. 2011;16(1):25–422. https://doi.org/10.1080/13557858.2010.523456.
Zhou YR, Majumdar B, Vattikonda N. Culture, but more than culture: an exploratory study of the HIV vulnerability of Indian immigrants in Canada. Cult Health Sex. 2016;18(9):1067–80. https://doi.org/10.1080/13691058.2016.1162328.
Donnelly LR, Bailey L, Jessani A, Postnikoff J, Kerston P, Brondani M. Stigma experiences in marginalized people living with hiv seeking health services and resources in Canada. J Assoc Nurses AIDS Care. 2016;27(6):768–83. https://doi.org/10.1016/j.jana.2016.07.003.
Kang E, Rapkin BD, Springer C, Kim JH. The “Demon Plague” and access to care among Asian undocumented immigrants living with HIV disease in New York City. J Immigr Health. 2003;5(2):49–58.
Neville S, Adams J. Views about HIV / STI and health promotion among gay and bisexual Chinese and South Asian men living in Auckland New Zealand. Int J Qual Stud Health Well-being. 2016;11(1):30764. https://doi.org/10.3402/qhw.v11.30764.
Ramanathan V, Sitharthan G, Pepper K, Wylie K. Sexual health of Indian immigrant men in Australia: an exploratory research on help-seeking attitudes. Sex Health. 2013;10(4):380–1. https://doi.org/10.1071/SH12199.
Sawleshwarkar S, Kakar SR, Jones R, Lagios K, Mindel A, Hillman RJ. Indian-born patients attending a sexual health clinic in Australia have differing characteristics to their Australian-born counterparts. Intern Med J. 2013;43(12):1327–30. https://doi.org/10.1111/imj.12299.
Sudhinaraset M, Ling I, To TM, Melo J, Quach T. Dreams deferred: contextualizing the health and psychosocial needs of undocumented Asian and Pacific Islander young adults in Northern California. Soc Sci Med. 2017;184:144–52. https://doi.org/10.1016/j.socscimed.2017.05.024.
Manzardo C, Treviño B, Gómez i Prat J, Cabezos J, Monguí E, Clavería I, Navarro R. Communicable diseases in the immigrant population attended to in a tropical medicine unit: Epidemiological aspects and public health issues. Travel Med Infect Dis. 2008;6(1–2):4–11. https://doi.org/10.1016/j.tmaid.2007.11.002.
Ramanathan V. Values, behaviour and identity: acculturation of Indian immigrant men in Australia. J Int Migr Integr. 2015;16(3):625–38. https://doi.org/10.1007/s12134-014-0364-2.
Brindis C, Barenbaum M, Sanchez-Flores H, McCarter V, Chand R. Let’s hear it for the guys: California’s male involvement program. Int J Men’s Health. 2005;4(1):29–53. https://doi.org/10.3149/jmh.0401.29.
Armstrong B. The young men’s clinic : addressing men’s reproductive health responsibilities. Perspect Sex Reprod Health. 2003;35(5):220–5.
Federal Register “Minority Health and Health Disparities Research and Education Act of 2000,” (S-1880). 2000. https://www.congress.gov/106/plaws/publ525/PLAW-106publ525.pdf.
Brach C, Fraserirector I. Can cultural competency reduce racial and ethnic health disparities? A review and conceptual model. Med Care Res Rev. 2000;57(1_suppl):181–217. https://doi.org/10.1177/1077558700057001S09.
Komaromy M, Grumbach K, Drake M, Vranizan K, Lurie N, Keane D, Bindman AB. The role of black and hispanic physicians in providing health care for underserved populations. N Engl J Med. 1996;334(20):1305–10. https://doi.org/10.1056/NEJM199605163342006.
Phillips KA, Mayer ML, Aday LA. Barriers to care among racial/ethnic groups under managed care. Health Aff. 2000;19(4):65–75.
Marcell AV, Bell DL, Lindberg LD, Takruri A. Prevalence of sexually transmitted infection/human immunodeficiency virus counseling services received by Teen Males, 1995–2002. J Adolesc Health. 2010;46(6):553–9. https://doi.org/10.1016/j.jadohealth.2009.12.002.
Smith JA, Braunack-Mayer A, Wittert G. What do we know about men’s help-seeking and health service use? Med J Aust. 2006;184:81–3.
Addis ME, Mahalik JR. Men, masculinity, and the contexts of help seeking. Am Psychol. 2003. https://doi.org/10.1037/0003-066X.58.1.5.
Raine T, Marcell AV, Rocca CH, Harper CC. The other half of the equation: Serving young men in a young women’s reproductive health clinic. Perspect Sex Reprod Health. 2008;35(5):208–14. https://doi.org/10.1363/psrh.35.208.03.
Wright AL, Morgan WJ. On the creation of “problem” patients. Soc Sci Med. 1990;30(9):951–9. https://doi.org/10.1016/0277-9536(90)90142-F.
Nyblade L, Stangl A, Weiss E, Ashburn K. Combating HIV stigma in health care settings: what works? J Int AIDS Soc. 2009;12(1):15. https://doi.org/10.1186/1758-2652-12-15.
Halcomb E, Fernandez R. Systematic reviews. Nurs Stand. 2015;29(33):45–51. https://doi.org/10.7748/ns.29.33.45.e8868.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jahangir, Y.T., Meyer, S.B. Understanding Access to and Utilisation of Sexual Health Services by South Asian Immigrant Men in Western Countries: A Scoping Review. J Immigrant Minority Health 22, 621–633 (2020). https://doi.org/10.1007/s10903-020-00981-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10903-020-00981-z