Abstract
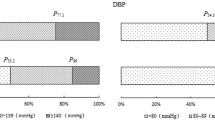
Taiwan’s indigenous population exhibits a higher mortality of cardiovascular disease, but current research has not reported any associations among ethnicities on the blood pressure (BP). We randomly selected representative samples in this population-based study. We measured height, weight, hip and waist circumferences, and blood pressure in a screening survey. Systolic BP and diastolic BP were significantly higher in the indigenous population. Among women, prevalence rates of DBP > 90 mmHg among indigenes (32.9 %) were significantly high than those in Han Chinese (17.4 %). Based on multivariate analysis adjusted for covariates, the results showed gender and ethnicity to be significantly correlated with systolic and diastolic BP. Gender was a modifier between ethnicity and BP. Furthermore, we found an additive effect between ethnicity and age on systolic and diastolic BP by gender. Our study showed independent additive effects on systolic BP and diastolic BP between ethnicity and age by gender.
Similar content being viewed by others
References
Chow RA, Caeiro JL, Chen SJ, et al. Genetic characterization of four Austronesian-speaking populations. J Hum Genet. 2005;50:550–9.
Council of Indigenous Peoples. Annual report of population and health statistics in. Council of Indigenous Peoples. Taiwan: Executive Yuan; 2010.
Australian Bureau of Statistics. National Aboriginal and Torres Strait Islander social survey, 2008. http://www.abs.gov.au/ausstats/abs@.nsf/mf/4714.0?OpenDocument, 2009.
Wang XL, Poole JC, Treiber FA, et al. Ethnic and gender differences in ambulatory blood pressure trajectories: results from a 15-year longitudinal study in youth and young adults. Circulation. 2006;114:2780–7.
Criado JR, Gilder DA, Kalafut MA, et al. Obesity in American Indian and Mexican American men and women: associations with blood pressure and cardiovascular autonomic control. Cardiovasc Psychiatry Neurol. 2013;. doi:10.1155/2013/680687.
Lazarou C, Panagiotakos DB, Matalas AL. Lifestyle factors are determinants of children’s blood pressure levels: the CYKIDS study. J Hum Hypertens. 2009;23:456–63.
Tseng CH. Higher risk of hypertension in indigenous type 2 diabetic patients in Taiwan. J Hypertens. 2006;24:1817–21.
Brown DE, Sievert LL, Aki SL, et al. Effects of age, ethnicity and menopause on ambulatory blood pressure: Japanese-American and Caucasian school teachers in Hawaii. Am J Hum Biol. 2001;13:486–93.
Hsu, Mutsu. Culture, self and adaptation: the psychological anthropology of two Malayo-Polynesian groups in Taiwan. Taipei, Taiwan: Institute of Ethnology, Academia Sinica. ISBN 957-9046-78-6, 1991.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, et al. Seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure. Hypertension 2003;42(6):1206–52.
Burt VL, Whelton P, Roccella EJ, et al. Prevalence of hypertension in the US adult population. Results from the Third National Health and Nutrition Examination Survey, 1988–1991. Hypertension. 1995;25(3):305–13.
Tsai AC, Lin YR. Sex and ethnic disparities in weight and height among children of transnational couples, aborigines, and Han Chinese in Taiwan. Nutr Res. 2008;28:664–70.
Jones DW, Hall JE. Racial and ethnic differences in blood pressure: biology and sociology. Circulation. 2006;114:2757–9.
Freedman DS, Khan LK, Serdula MK, et al. Racial differences in the tracking of childhood BMI to adulthood. Obesity Res. 2005;13:928–35.
Profant J, Dimsdale JE. Race and diurnal blood pressure patterns. A Rev Meta-analysis Hypertens. 1999;33:1099–104.
Staessen J, Bulpitt CJ, Fagard R, et al. The influence of menopause on blood pressure. J Hum Hypertens. 1989;3:427–33.
Reckelhoff JF. Gender differences in the regulation of blood pressure. Hypertension. 2001;37:1199–208.
Rosano GM, Vitale C, Marazzi G, et al. Menopause and cardiovascular disease: the evidence. Climacteric. 2007;10(Suppl 1):19–24.
Tseng CH. Betel nut chewing is associated with hypertension in Taiwanese type 2 diabetic patients. Hypertens Res. 2008;31:417–23.
Yen CF, Hsu CC, Liu SC, et al. Psychopathology of aboriginal and non-aboriginal adolescents living in the mountainous region of southern Taiwan. Kaohsiung J Med Sci. 2006;22:560–9.
Hsiao YC, Wang K, Bair MJ. Prevalence of obesity and metabolic syndrome in aboriginals in southeastern Taiwan—a hospital-based study. J Int Med (Taiwan). 2011;22:48–56.
Ho CS, Tsai AC. Prevalence of overweight and obesity and its associated factors in aboriginal Taiwanese: findings from the 2001 National Health Interview Survey in Taiwan. Asia Pac J Clin Nutr. 2007;16:572–9.
Chen HD, Shaw CK, Tseng WP, et al. Prevalence of diabetes mellitus and impaired glucose tolerance in aborigines and Chinese in eastern Taiwan. Diabetes Res Clin Pract. 1997;38:199–205.
Lee MS, Lin SC, Chang HY, et al. High prevalence of hyperuricemia in elderly Taiwanese. Asia Pac J Clin Nutr. 2005;14:285–92.
Pan WH, Yeh WT, Chang HY, et al. Prevalence and awareness of diabetes and mean fasting glucose by age, sex, and region: results from the Nutrition and Health Survey in Taiwan, 1993–1996. Diabetic Med. 2003;20:182–5.
Su TC, Hwang LC, You SL, et al. Ethnic variation in hypertension prevalence of women in Taiwan. J Hum Hypertens. 2009;23:160–7.
Wang TN, Huang MC, Lin HL, et al. UCP2 A55 V variant is associated with obesity and related phenotypes in an aboriginal community in Taiwan. Int J Obes. 2007;31:1746–52.
Cheng ATA. Risk factors for alcoholism among Taiwanese Aborigines. Arch Gen Psychiatry. 2004;61:184–91.
Pérez-Miranda AM, Alfonso-Sánchez MA, Herrera RJ. Microsatellite polymorphisms in two Taiwanese aboriginal groups. Int Congress Series. 2006;1288:394–6.
WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet. 2004;363:157–63.
Hsieh SD, Yoshinaga H, Muto T, et al. Health risks among Japanese men with moderate body mass index. Int J Obes Relat Metab Disord. 2000;24:358–62.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Chen, S.C., Lo, T.C., Chang, J.H. et al. Ethnic Disparities in Blood Pressure: A Population-based Study. J Immigrant Minority Health 19, 1427–1433 (2017). https://doi.org/10.1007/s10903-016-0434-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10903-016-0434-y