Abstract
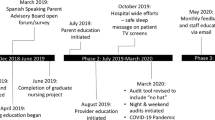
Sleep-related infant deaths continue to be a major, largely preventable cause of infant mortality, especially in Georgia. The Georgia Department of Public Health (DPH), as part of a multi-pronged safe infant sleep campaign, implemented a hospital initiative to (1) provide accurate safe infant sleep information to hospital personnel; (2) support hospitals in implementing and modeling safe sleep practices; and (3) provide guidance on addressing caregiver safe sleep concerns. A process evaluation was conducted to determine progress toward four goals set out by DPH: (1) all birthing hospitals have a safe infant sleep policy; (2) all safe infant sleep policies reference the AAP 2011 recommendations; (3) all safe infant sleep policies specify the type and/or content of patient safe sleep education; and (4) all hospitals require regular staff training on safe sleep recommendations. Data were collected via structured interviews and document review of crib audit data and safe sleep policies. All 79 birthing hospitals in the state participated in the statewide campaign. Prior to the initiative, 44.3% of hospitals had a safe sleep policy in place; currently, 87.3% have a policy in place. The majority (91.4%) of hospitals have provided safe sleep training to their staff at this time. Important lessons include: (1) Engagement is vital to success; (2) A comprehensive implementation guide is critical; (3) Piloting the program provides opportunities for refinement; (4) Ongoing support addresses barriers; and (5) Senior leadership facilitates success.
Similar content being viewed by others
References
Moon, R. Y. & American Academy of Pediatrics Taskforce on Sudden Infant Death Syndrome. (2016). SIDS and other sleep-related infant deaths: Updated 2016 recommendations for a safe infant sleeping environment. Pediatrics, 138(5), e20162938. https://doi.org/10.1542/peds.2016-2938.
Carlin, R. F., & Moon, R. Y. (2017). Risk factors, protective factors, and current recommendations to reduce sudden infant death syndrome: A review. JAMA Pediatrics, 171(2), 175–180. https://doi.org/10.1001/jamapediatrics.2016.3345.
National Institute of Child Health and Human Development. (2015). Safe to sleep® public education campaign. Retrieved from http://www.nichd.nih.gov/sts/.
Colvin, J. D., Collie-Akers, V., & Moon, R. Y. (2014). Sleep environment risks for younger and older infants. Pediatrics, 134(2), e406–e412. https://doi.org/10.1542/peds.2014-0401.
Kassa, H., Moon, R. Y., & Colvin, J. D. (2016). Risk factors for sleep-related infant deaths in in-home and out-of-home settings. Pediatrics, 138(5), e20161124. https://doi.org/10.1542/peds.2016-1124.
Shapiro-Mendoza, C. K., Colson, E. R., Willinger, M., Rybin, D. V., Camperlengo, L., & Corwin, M. J. (2015). Trends in infant bedding use: National infant sleep position study 1993–2010. Pediatrics, 135(1), 10–17. https://doi.org/10.1542/peds.2014-1793.
Georgia Child Fatality Review Panel. (2016). Georgia child fatality review panel 2014 annual report. Atlanta, GA: State of Georgia.
Georgia Department of Public Health. (2017). Pregnancy risk assessment monitoring system. Atlanta, GA: Georgia Department of Public Health. Retrieved from https://dph.georgia.gov/pregnancy-risk-assessment-monitoring-system-prams.
Moon, R. Y., Hauck, F. R., & Colson, E. R. (2016). Safe infant sleep interventions: What is the evidence for successful behavior change? Current Pediatric Reviews, 12, 67–75. https://doi.org/10.2174/1573396311666151026220906.
Salm Ward, T. C., & Balfour, G. (2016). Infant safe sleep interventions, 1990–2015: A review. Journal of Community Health, 41(1), 180–196. https://doi.org/10.1007/s10900-015-0060-y.
Salm Ward, T. C., & Doering, J. J. (2014). Application of a socio-ecological model to mother-infant bed-sharing. Health Education and Behavior, 41(6), 577–589. https://doi.org/10.1177/1090198114543010.
Colson, E. R., Rybin, D., Smith, L. A., Colton, T., Lister, G., & Corwin, M. J. (2009). Trends and factors associated with infant sleeping position: The national infant sleep position study. Archives of Pediatrics & Adolescent Medicine, 163(12), 1122–1128. https://doi.org/10.1001/archpediatrics.2009.234.
Colson, E. R., & Joslin, S. C. (2002). Changing nursery practice gets inner-city infants in the supine position for sleep. Archives of Pediatrics and Adolescent Medicine, 156(7), 717–720. https://doi.org/10.1001/archpedi.156.7.717.
Gelfer, P., Cameron, R., Masters, K., & Kennedy, K. A. (2013). Integrating “back to sleep” recommendations into neonatal ICU practice. Pediatrics, 131(4), e1264–e1270. https://doi.org/10.1542/peds.2012-1857.
Goodstein, M. H., Bell, T., & Krugman, S. D. (2015). Improving infant sleep safety through a comprehensive hospital-based program. Clinical Pediatrics, 54(3), 212–221. https://doi.org/10.1177/0009922814566928.
Mason, B., Ahlers-Schmidt, C. R., & Schunn, C. (2013). Improving safe sleep environments for well newborns in the hospital setting. Clinical Pediatrics, 52(10), 969–975. https://doi.org/10.1177/0009922813495954.
Moon, R. Y., Oden, R. P., Joyner, B. L., & Ajao, T. I. (2010). Qualitative analysis of beliefs and perceptions about sudden infant death syndrome in African-American mothers: Implications for safe sleep recommendations. The Journal of Pediatrics, 157, 92–97. https://doi.org/10.1016/j.jpeds.2010.01.027.
Stastny, P. F., Ichinose, T. Y., Thayer, S. D., Olson, R. J., & Keens, T. G. (2004). Infant sleep positioning by nursery staff and mothers in newborn hospital nurseries. Nursing Research, 53, 122–129.
Vernacchio, L., Corwin, M. J., Lesko, S. M., Vezina, R. M., Hunt, C. E., Hoffman, H. J., … Mitchell, A. A. (2003). Sleep position of low birth weight infants. Pediatrics, 111(3), 633–640. https://doi.org/10.1542/peds.111.3.633.
Macklin, J. R., Gittelman, M. A., Denny, S. A., Southworth, H., & Arnold, M. W. (2016). The EASE quality improvement project: Improving safe sleep practices in ohio’s children’s hospitals. Pediatrics, 138(4), e20154267. https://doi.org/10.1542/peds.2015-4267.
Kuhlmann, S., Ahlers-Schmidt, C. R., Lukasiewicz, T., & Truong, T. M. (2016). Interventions to improve safe sleep among hospitalized infants at eight children’s hospitals. Hospital Pediatrics, 6(2), 88–94. https://doi.org/10.1542/hpeds.2015-0121.
Georgia Department of Public Health. (2015). Safe to sleep. Retrieved from https://dph.georgia.gov/safetosleep.
Moon, R. Y. & American Academy of Pediatrics Taskforce on Sudden Infant Death Syndrome. (2011). SIDS and other sleep-related infant deaths: Expansion of recommendations for a safe infant sleeping environment. Pediatrics, 128(5), 1030–1039. https://doi.org/10.1542/peds.2011-2284.
Barnes-Josiah, D. L., Eurek, P., Huffman, S., Heusinkvelt, J., Severe-Oforah, J., & Schwalberg, R. (2007). Effect of “this side up” T-shirts on infant sleep position. Maternal and Child Health Journal, 11(1), 45–48. https://doi.org/10.1007/s10995-006-0124-9.
First Candle/SIDS Alliance. (2006). Model behavior: The most important modelling job of your life. Retrieved from http://www.firstcandle.org/professionals/program-highlights/model-behavior-nurses-ce-program/.
National Institute of Child Health and Human Development. (2007). Curriculum for nurses: Continuing education program on SIDS risk reduction. (No. 06–6005). Washington, DC: U.S. Government Printing Office.
Cribs for Kids. (2016). Cribs for kids(R) hospital certification. Retrieved from http://www.cribsforkids.org/hospitalinitiative/.
Hutton, J. (2013). Sleep baby safe and snug. Cincinnati, OH: Blue Manatee Press.
ASTM International. (2016). ASTM F2194-16e1, Standard consumer safety specification for bassinets and cradles. West Conshohocken, PA: ASTM International. https://doi.org/10.1520/F2194-16E01.
Barsman, S. G., Dowling, D. A., Damato, E. G., & Czeck, P. (2015). Neonatal nurses’ beliefs, knowledge, and practices in relation to sudden infant death syndrome risk-reduction recommendations. Advances in Neonatal Care, 15(3), 209–219. https://doi.org/10.1097/ANC.0000000000000160.
Bartlow, K. L., Cartwright, S. B., & Shefferly, E. K. (2016). Nurses’ knowledge and adherence to sudden infant death syndrome prevention guidelines. Pediatric Nursing, 42(1), 7–13.
Hwang, S. S., O’Sullivan, A., Fitzgerald, E., Melvin, P., Gorman, T., & Fiascone, J. M. (2015). Implementation of safe sleep practices in the neonatal intensive care unit. Journal of Perinatology, 35(10), 862–866. https://doi.org/10.1038/jp.2015.79.
McMullen, S. L., Fioravanti, I. D., Brown, K., & Carey, M. G. (2016). Safe sleep for hospitalized infants. The American Journal of Maternal/Child Nursing, 41(1), 43–50. https://doi.org/10.1097/NMC.0000000000000205.
Rowe, A. D., Sisterhen, L. L., Mallard, E., Borecky, B., Schmid, B., Rettiganti, M., & Luo, C. (2016). Integrating safe sleep practices into a pediatric hospital: Outcomes of a quality improvement project. Journal of Pediatric Nursing, 31(2), e141–e147. https://doi.org/10.1016/j.pedn.2015.10.015.
HALO. (2017). HALO(R) in-hospital sleep sack(R) program. Retrieved from http://www.halosleep.com/in-hospital-sleepsack-program.
American Academy of Pediatrics. (2005). The changing concept of sudden infant death syndrome (SIDS): Diagnostic coding shifts, controversies regarding the sleeping environment, and new variables to consider in reducing risk. Pediatrics, 116(5), 1245–1255. https://doi.org/10.1542/peds.2005-1499.
Georgia Department of Public Health. (2016). Georgia 5-STAR. Retrieved from https://dph.georgia.gov/georgia-5-star.
World Health Organization & UNICEF. (2012). Baby friendly hospital initiative. Retrieved from http://www.unicef.org/nutrition/files/BFHI_section_2_2009_eng.pdf.
Funding
Funding for the educational support tools was provided by the Georgia Children’s Cabinet, led by First Lady Sandra Deal. The initiative is supported by the Georgia Chapter of the American Academy of Pediatrics; the Georgia Bureau of Investigation; the Georgia Hospital Association; and the Georgia Obstetrical and Gynecological Society. A special thanks goes to the Georgia Commissioner of Public Health, Brenda Fitzgerald, M.D. We thank the many hospital staff members for taking on this voluntary program and for sharing their experiences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Miller, T.J., Salm Ward, T.C., McClellan, M.M. et al. Implementing a Statewide Safe to Sleep Hospital Initiative: Lessons Learned. J Community Health 43, 768–774 (2018). https://doi.org/10.1007/s10900-018-0483-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-018-0483-3