Abstract
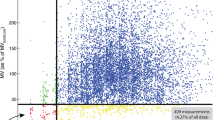
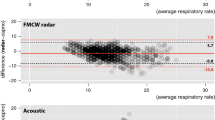
During moderate sedation for gastrointestinal endoscopic submucosal dissection (ESD), monitoring of ventilatory function is recommended. We compared the following techniques of respiratory rate (RR) measurement with respiratory sound (RRa): capnography (RRc), thoracic impedance (RRi), and plethysmograph (RRp). This study enrolled patients aged ≥ 20 years who underwent esophageal (n = 19) and colorectal (n = 5) ESDs. RRc, RRi, RRp, and RRa were measured by Capnostream™ 20P, BSM-2300, Nellcor™ PM1000N, and Radical-7®, respectively. In total, 413 RR data were collected from the esophageal ESD group and 114 RR data were collected from the colorectal ESD group. Compared with RRa during colorectal ESD, that during esophageal ESD had larger bias [95% limit of agreement (LOA)] with RRc [1.9 (− 11.0–14.8) vs. − 0.4 (− 2.9–2.2)], RRi [9.4 (− 16.8–9.4) vs. − 1.5 (− 12.0–8.9)], and RRp [0.3 (− 5.7–6.4) vs. 0.2 (− 3.2–3.6)]. Of the correct RR values displayed during esophageal ESD, > 90% were measured as RRa and RRp. Moreover, RRc was a useful parameter during colorectal ESD. To maximize patient safety during ESD under sedation, endoscopists and medical staff should know the feature and principle of the devices used for RR measurement. During esophageal ESD, RRa and RRp may be a good parameter to detect bradypnea or apnea. RRc, RRa and RRp are useful for reliable during colorectal ESD.
Trial registration UMIN-CTR (UMIN000025421).



Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author, [TF].
Code availability
Not applicable.
References
American Society of Anesthesiologists, American Association of Oral and Maxillofacial Surgeons, American College of Radiology, American Dental Association, American Society of Dentist Anesthesiologists, Society of Interventional Radiology. Practice guidelines for moderate procedural sedation and analgesia 2018: a report by the American Society of Anesthesiologists Task Force on moderate procedural sedation and analgesia, the American Association of Oral and Maxillofacial Surgeons, American College of Radiology, American Dental Association, American Society of Dentist Anesthesiologists, and Society of Interventional Radiology. Anesthesiology. 2018;128(3):437–79. https://doi.org/10.1097/ALN.0000000000002043.
Burton JH, Harrah JD, Germann CA, Dillon DC. Does end-tidal carbon dioxide monitoring detect respiratory events prior to current sedation monitoring practices? Acad Emerg Med. 2006;13:500–4. https://doi.org/10.1197/j.aem.2005.12.017.
Takamaru H, Kawaguchi Y, Oda I, Sekiguchi M, Yamada M, Abe S, Nonaka S, Suzuki H, Yoshinaga S, Saito Y. A new reliable acoustic respiratory monitoring technology during upper gastrointestinal tract therapeutic endoscopy with CO2 insufflation. J Clin Monit Comput Epub ahead print. 2020. https://doi.org/10.1007/s10877-020-00547-2.
Suzuki T, Tsuda S, Nakae H, Imai J, Sawamoto K, Kijima M, Tsukune Y, Uchida T, Igarashi M, Koike J, Matsushima M, Suzuki T, Mine T. Usefulness of acoustic monitoring of respiratory rate in patients undergoing endoscopic submucosal dissection. Gastroenterol Res Pract. 2016. https://doi.org/10.1155/2016/2964581.
Fukada T, Iwakiri H, Nomura M, Ozaki M. Clinical evaluation of acoustic respiration rate monitoring compared with conventional systems in the postanaesthesia care unit. Eur J Anaesthesiol. 2015;32:58–68. https://doi.org/10.1097/EJA.0000000000000193.
Ramsay MAE, Usman M, Lagow E, Mendoza M, Untalan E, De Vol E. The accuracy, precision and reliability of measuring ventilatory rate and detecting ventilatory pause by rainbow acoustic monitoring and capnometry. Anesth Analg. 2013;117:69–75. https://doi.org/10.1213/ANE.0b013e318290c798.
Nonaka S, Saito Y, Takisawa H, Kim Y, Kikuchi T, Oda I. Safety of carbon dioxide insufflation for upper gastrointestinal tract endoscopic treatment of patients under deep sedation. Surg Endose. 2010;24:1638–45. https://doi.org/10.1007/s00464-009-0824-5.
Takada J, Araki H, Onogi F, Nakanishi T, Kubota M, Ibuka T, Shimizu M, Moriwaki H. Safety and efficacy of carbon dioxide insufflation during gastric endoscopic submucosal dissection. World J Gastroenterol. 2015;21:8195–02. https://doi.org/10.3748/wjg.v21.i26.8195.
Kusunoki R, Amano Y, Yuki T, Oka A, Okada N, Tada Y, Uno G, Moriyama I, Ishimura N, Ishihara S, Kinoshita Y. Capnographic monitoring for carbon dioxide insufflation during endoscopic mucosal dissection: comparison of transcutaneous and end-tidal capnometers. Surg Endose. 2012;26:501–6. https://doi.org/10.1007/s00464-011-1908-6.
Soto RG, Fu ES, Vila H Jr, Miguel RV. Capnography accurately detects apnea during monitored anesthesia care. Anesth Analg. 2004;99:379–82. https://doi.org/10.1213/01.ANE.0000131964.67524.E7.
Wilkinson JN, Thanawala VU. Thoracic impedance monitoring of respiratory rate during sedation – is it safe? Anaeshtesia. 2009;64:447–58. https://doi.org/10.1111/j.1365-2044.2009.05908.x.
Addison PS, Watson JN, Mestek ML, Ochs JP, Uribe AA, Bergese SD. Pulse oximetry-derived respiratory rate in general care patients. J Clin Monit Comput. 2015;29:113–20. https://doi.org/10.1007/s10877-014-9575-5.
Acknowledgements
The authors would like to thank Akiko Zaitsu, Department of Anesthesiology, Tokyo Women's Medical University, for preparing the four devices to measure RR, and Enago (www.enago.jp) for the English language review.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
TF, YT, and HI participated in the study design, data collection, data analysis, scientific input, and manuscript writing and reviewing. MO and MN participated in the design of the study and manuscript review. SF reviewed the manuscript. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
Approval for this study was obtained from the institutional review board of Tokyo Women's Medical University (No. 3886; approval date April 18, 2016).
Consent to participate
Written informed consent was obtained from all patients.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fukada, T., Tsuchiya, Y., Iwakiri, H. et al. Comparisons of the efficiency of respiratory rate monitoring devices and acoustic respiratory sound during endoscopic submucosal dissection. J Clin Monit Comput 36, 1013–1019 (2022). https://doi.org/10.1007/s10877-021-00727-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-021-00727-8